Primary cutaneous aggressive epidermotropic CD8+ T cell lymphoma with a chronic and indolent course. Is different from the peripheral T cell lymphoma?
Published Web Location
https://doi.org/10.5070/D37xx161pqMain Content
Primary cutaneous aggressive epidermotropic CD8+ T cell lymphoma with a chronic and indolent course. Is this different from
peripheral T cell lymphoma?
Mercedes Gómez Vázquez MD PhD, Ramón Navarra Amayuelas MD PhD
Dermatology Online Journal 18 (3): 11
Department of Dermatology, Hospital Municipal de Badalona, Barcelona, SpainAbstract
Cutaneous T cell lymphomas most commonly have a CD4+ memory T cell phenotype and exhibit a relatively indolent course, but may in rare cases present with a CD8+ cytotoxic phenotype with a strikingly more aggressive clinical behavior. Primary cutaneous aggressive epidermotropic CD8+ T cell lymphoma is an extremely rare entity with distinct clinicopatological features. The clinical features and prognosis of the recently-described CD8+ peripheral lymphoma are very different from cytotoxic CD8+ epidermotropic lymphoma, but the histological and phenotypic characteristics are very similar. We report a new case of CD8+ epidermotropic lymphoma with a chronic course and suggest the possibility of an overlap between these two types of lymphoma.
Cutaneous T cell lymphomas (CTCL) are primary malignancies of the skin and exhibit completely different clinical behavior and prognosis from histologically similar systemic lymphomas [1]. “Primary cutaneous peripheral T cell lymphomas of unspecified type” represent a heterogeneous group in the EORTC (European Organization for Research and Treatment of Cancer) classification and include a provisional entity, primary cutaneous aggressive epidermotropic CD8 cytotoxic T cell lymphoma [1, 2, 3].
A 69-year-old woman with a history of plaque psoriasis and hypertension developed a rapidly-growing nodule in the lower eyelid. She never received immunosuppressive treatment of her psoriasis and only received topical corticosteroids for a short time. Examination revealed an erythematous tumor with an ulcerated surface (Figure 1a). There was no palpable lymphadenopathy or hepatosplenomegaly.
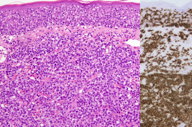
Skin biopsy revealed a monomorphous, dense dermal infiltrate of large pleomorphic lymphocytes with marked epidermotropism (Figure 1a). The tumor cells were positive for CD8, CD3, CD5, and CD30 and negative for CD4, CD2, CD7, and CD20 (Figures 1b and 1c). The percentage of Ki67-positive tumor cells was > 30 percent. Molecular genetic testing using polymerase chain reaction (PCR) showed a T cell clonal population in the skin and a matching clone in the peripheral blood.
A diagnosis of CD8+ epidermotropic cytotoxic primary cutaneous T cell lymphoma was made based on the histologic, immunophenotypic, and molecular biologic findings. Tests revealed medullary involvement without involvement of the internal organs or lymph nodes in the PET and MNR. Medullary involvement was consistent with stage IV medullary. Bone marrow and peripheral blood involvement occurred two months after the cutaneous diagnosis. Tests for human immunodeficiency viruses 1 and 2 and human T cell lymphotropic virus 1 were negative.
The patient was treated with combination local radiation therapy of the ocular lesion and chemotherapy with CHOP (cyclophosphamide, adriamycin, vincristine, prednisone) with complete remission of cutaneous lesions. Five years later, the patient presented a partial relapse with clonal T lymphocytosis in the bone marrow and peripheral blood. The bone marrow clonality does not differ from the initial picture and cannot bre attributed to chemotherapy. Because the patient is stable and there is no involvement of other organs, regular checkups are made, but therapy has not been reintroduced.
Four subtypes of CD8+ cutaneous T cell lymphoma have been identified, the first of which is well defined and is designated as primary cutaneous CD8+ epidermotropic cytotoxic T cell lymphoma by the EORTC [1, 2, 3].
The case reported here is similar to previous reports of aggressive CD8+ epidermotropic cytotoxic cutaneous T cell lymphoma, showing the distinctive clinical presentation, histology, and immunophenotypic features of this rare type of cutaneous T cell lymphoma [4], but with a more indolent course.
Clinically, this variant of cutaneous T cell lymphoma manifests as localized or disseminated papules, nodules, and larger tumors, often with ulceration, hemorrhage, and necrosis; superficial hyperkeratotic patches and plaques may also be seen [5]. Rapid progression with extracutaneous dissemination is typical, with metastasis to unusual sites including the lung, testes, and central nervous system, but generally sparing the lymph nodes [6, 7] Epidermotropism is seen in all stages of the disease, with tumor cells predominately confined to the epidermis [4].
The prognosis for this type of lymphoma is very poor, with a median survival of only 22.5-33 months [4]. Some authors suggest that loss of CD2 and CD5 pan T cell markers may be indicative of rapidly progressive disease (our patient was CD5 positive), whereas CD7-/CD2+ phenotypes are more-commonly associated with chronic disease (our patient was CD7 negative) [4].
A recent report by Ryan et. al. described a case of CD8+ lymphoma, which they named CD8+ peripheral primary cutaneous lymphoma, with different clinical and prognostic features of primary cutaneous CD8+ epidermotropic cytotoxic T cell lymphoma, but with similar histological and phenotypic features, except for the absence of epidermotropism [8]. Petrela et al [9], described four cases of indolent CD8+ lymphoma. This type of lymphoma presents with characteristic facial lesions with no extracutaneous involvement and with a phenotype similar to our case but with a Ki67 proliferation index < 10 and without epidermotropism in most cases. Nearly all cases have a good response to local radiotherapy.
Comparison of the lymphoma presented by Ryan et al and the CD8+ cytotoxic lymphomas reported to date shows differences that suggest the possibility of a new subtype of CD8+ lymphoma which is more indolent, permitting a more-conservative therapy and better survival.
The case presented here, to our knowledge the only reported case with these characteristics, has features common to both primary cutaneous CD8+ epidermotropic cytotoxic T cell lymphoma and CD8+ peripheral primary cutaneous lymphoma, suggesting the possibility of an overlap (Table 1). Alternatively, it may be a unique presentation of cytotoxic CD8+ epidermotropic lymphoma.
This case report adds information to the existing data on primary cutaneous aggressive epidermotropic CD8+ cytotoxic T cell lymphoma, a rare clinicopathologic entity, which is a distinct disease characterized by specific histological and immunophenotypic features, with aggressive clinical behavior and no effective treatment at present.
References
1. Willence R, Jaffe ES, Brug G, Cerroni L, Berti E, Swerdolw SH et al. WHO-EORTC classification for cutaneous lymphomas. Blood 2005;105:3768-85. [PubMed]2. Gallardo F, Pujol RM. Diagnóstico y tratamiento de los linfomas cutáneos de células T primarios. Actas Dermosifiliogr 2004;95:473-90.
3. Willence R, Kerl H, Sterry W, Berti E, Cerroni L, Chimenti S, et al. EORTC classification for primary cutaneous lymphomas: a proposal from the cutaneous lymphoma study group of the European Organitation for Research and Treatment of Cancer. Blood 1997; 90:354-71. [PubMed]
4. Gormley RH, Hess SD, Anand D, Junkins-Hopkins J, Rook A, Kim EJ. Primary cutaneous aggressive epidermotropic CD8+ T-cell lymphoma. J Am Acad Dermatol 2010; 62:300-7. [PubMed]
5. Marzano AV, Ghislanzoni M, Gianelli U, Ruggero C, Alessi E, Berti E. Fatal CD8+ Epidermotropic Cytotoxic Primary Cutaneous T-cell Lymphoma with Multiorgan Involvement. Dermatology 2005;211:281-5. [PubMed]
6. Csomor J, Bognár A, Benedek S, Sinkó S, Krenács L, Matolcsy A, Reiniger L. Rare provisional entity: primary cutaneous aggressive epidermotropic CD8+ cytotoxic T-cell lymphoma in a young woman. J Clin Pathol 2008;61:770-72. [PubMed]
7. Intracaso CE, Kim EJ, Gardner J, Junkis-Hopkins JM, Vittorio CC, Rook AH. CD8+ epidermotropic cytotoxic T-cell lymphoma with peripheral blood and central system involvement. Arch Dermatol 2008;144:1027-9. [PubMed]
8. Ryan AJA, Robson A, Hayes BD, Sheehan, Collins P. Primary cutaneous peripheral T-cell lymphoma, unspecified with an indolent clinical course: a distinct peripheral T-cell lymphoma. Clin Experim Dermatol, 2010;25:892-896. [PubMed]
9. Petrella T, Maubec E, Cornillet-Lefebvre P et al. Indolent CD8-positive lymphoid proliferation of the ear: a distinct primary cutaneous T-cell lymphoma? Am J Surg Pathol 2007;31:1887-92. [PubMed]
© 2012 Dermatology Online Journal