Pulmonary sarcoidosis in a patient with psoriatic arthritis during infliximab therapy
Published Web Location
https://doi.org/10.5070/D39jd8831cMain Content
Letter: Pulmonary sarcoidosis in a patient with psoriatic arthritis during infliximab therapy
S Izzi1,2, F Francesconi1, P Visca5, A Altieri3, C De Mutiis4, G Trevisan2, C Bonifati1
Dermatology Online Journal 16 (5): 16
1. Department of Dermatology, San Gallicano Dermatologic Institute-IRCCS, Rome, Italy. psoriasi@ifo.it2. Department of Clinical Dermatology, University of Trieste
3. Bronchopneumology and Tisiology Unit San Camillo-Forlanini Hospital, Rome, Italy
4. Radiodiagnostic Service, San Gallicano Dermatologic Institute-IRCCS, Rome, Italy
5. Department of Pathology, Regina Elena Cancer Institute, Rome, Italy
Abstract
The occurrence of sarcoidosis during anti-TNF-α therapy has occasionally been published. We report the case of a psoriasis patient who developed pulmonary sarcoidosis during a cycle of therapy with infliximab.
Case
The patient, a 34-year-old man, was admitted to our department in December 2006. He had a 12-year history of psoriasis with arthritis treated in the past with cycles of methotrexate with modest benefit. He reported that over the last two years he had only been taking homeopathic drugs.
Physical examination revealed scaly erythematous plaques involving 40 percent of the body surface and tenderness of the second, third, and fourth metacarpophalangeal joints of the left hand. Tenderness and swelling of the interphalangeal and metatarsophalangeal joints of the first ray of the right foot was also present. Chemical laboratory analyses detected an elevation of ESR (26 U.M.; normal range 1-18 U.M.), CRP (5 U.M.; normal range 0.0-0.8 U.M.), and ANA (1:320). The Rheumatoid factor was negative, as were the QuantiFERON TB Gold (QFT-TB) and the tuberculosis skin test (TST). The chest X-ray was normal without any evidence of hilar lymphadenopathy. Plain radiographs of the hands, wrists, feet, ankles, and sacro-iliac joints were also normal. A magnetic resonance image of the right foot revealed an effusion at the level of the metatarsophalangeal and interphalangeal joints of the first ray. At the same level edema of the tendons of the extensor and flexor muscles was also observed. On the basis of the clinical, biohumoral, and instrumental findings the diagnosis of psoriatic arthritis was confirmed.
A cycle of I.V. infusional therapy with infliximab (5 mg/kg) was started. The drug was initially administered at weeks 0, 2, 6, and then every 8 weeks. At the same time the clinical follow-up, including routine blood sample tests were performed.
After 6 weeks (before the 3th infusion) the patient showed a significant improvement of both skin and joint symptoms.
In November 2007, less than 2 months from the sixth infusion and 9 months after starting infliximab, the patient came to our department complaining of asthenia and right subdiaphragmatic pain during inspiration. He had neither dyspnea nor cough. The physical examination of the chest was unremarkable.
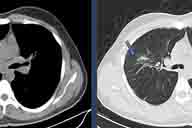 | 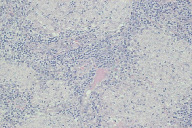 |
| Figure 1 | Figure 2 |
|---|
The skin and joint examination was negative. A chest X-ray revealed bilateral hilar adenopathies and subclavicular and middle right lung fibrotic infiltrates. Computed tomography (CT) confirmed the presence of several enlarged hilar and mediastinal lymph nodes (Figure 1A) and a diffuse reticulonodular interstitial infiltrate (Figure 1B). The histology of the hilar lymph nodes, collected through anterior mediastinotomy, showed noncaseating epithelioid cell granulomas (Figure 2).
Gallium 67 scintigraphy showed an increased uptake in the paratracheal and hilar lymph nodes and both lung fields.
QuantiFERON TB Gold (QFT-TB) and tuberculosis skin test (TST) were both negative.
Stains of the broncoalveolar lavage for acid-fast bacilli, fungi, and bacteria were negative, as were all subsequent cultures. In light of the pathologic findings, a diagnosis of sarcoidosis was made. Because of reported cases of sarcoidosis during anti-TNF-α therapy [1-13], infliximab administration was stopped.
In June 2008 (9 months after the last infliximab infusion) a new CT was performed that showed mild improvement as compared to the previous CT. At that time the patient no longer complained of fatigue, chest pain, dyspnea, or cough.
However, during this time both the skin and joint symptoms had worsened.
Treatment with prednisone (50 mg/daily) and leflunomide (20 mg/daily) was started. After 3 months a new CT showed a complete resolution of the reticulonodular infiltrates and a marked reduction of mediastinal hilar lymphadenopathy. Therefore, prednisone was slowly tapered off over the following months. Currently the patient is taking only leflunomide and continues to have no joint symptoms and only mild psoriatic skin activity.
Discussion
The case reported here confirms the possibility of the appearance of sarcoidosis during therapy with a TNF-α inhibitor. Because the sarcoidosis persisted after stopping infliximab a direct causality between the drug and the development of this granulomatous disease cannot be positively established.
The likelihood of a relationship between infliximab and the development of sarcoidosis was classified as possible (score: 4) using Naranjo’s algorithm [14].
At the present time 17 cases of sarcoidosis during anti-TNF-α treatment have been reported as follows: etanercept 9 cases, infliximab 6 cases, and adalimumab 2 cases [1-13]. The patients were affected with different rheumatic inflammatory diseases, such as rheumatoid arthritis, ankylosing spondylitis, juvenile idiopathic arthritis, and psoriatic arthritis. Hilar and mediastinal adenopathies were the most frequent findings, often associated with pulmonary infiltrates. However, parotid gland enlargement, cutaneous nodular lesions, and neuro-ocular manifestations have been reported.
The prognosis of sarcoidosis appearing during anti-TNF-α therapy would appear to be favorable. In several patients a complete resolution of the granulomatous disease was achieved simply by withdrawing the offending drug [2, 4, 10, 11, 12]. In other cases, as well as that reported here, a cycle of therapy with corticosteroids was necessary [1, 3, 4, 6-9, 12].
The development of a granulomatous disease such as sarcoidosis in patients taking anti-TNF-α drugs seems a paradoxical effect. In fact there is evidence that TNF-α plays a central role both in the formation and maintenance of granuloma [15]. Moreover, some cases of sarcoidosis, resistant to conventional therapies, have been successfully treated with TNF-α antagonists [16, 17]. The appeareance of sarcoidosis during the use of TNF-α inhibitors is reminiscent of another paradoxical effect sometimes seen with these drugs, such as the development of psoriatic lesions in patients with no previous disease or family history of psoriasis [18].
At the present time the mechanisms underlying the appearance of either sarcoidosis or psoriasis during anti-TNF-α therapy are completely unknown. Because the onset of sarcoidosis or psoriasis has been reported with all 3 anti-TNF-α agents it is likely that they represent a “class-dependent” effect rather than an immunoallergic reaction [12].
References
1. Hashkes PJ, Shajrawi I. Sarcoid-related uveitis occurring during etanercept therapy. Clin Exp Rheumatol 2003; 21: 645-646. [PubMed]2. González-López MA, Blanco R, González-Vela MC, Fernández-Llaca H, Rodríguez-Valverde V. Development of sarcoidosis during etanercept therapy. Arthritis Rheum 2006; 55: 817-820. [PubMed]
3. O’Shea FD, Marras TK, Inman RD. Pulmonary sarcoidosis developing during infliximab therapy. Arthritis Rheum 2006; 55: 978-981. [PubMed]
4. Verschueren K, Van Essche E, Verschueren P, Taelman V, Westhovens R. Development of sarcoidosis in etanercept-treated rheumatoid arthritis patients. Clin Rheumatol 2007; 26: 1969-1971. [PubMed]
5. Almodóvar R, Izquierdo M, Zarco P, Javier Quirós F, Mazzucchelli R, Steen B. Pulmonary sarcoidosis in a patient with ankylosingspondylitis treated with infliximab. Clin Exp Rheumatol 2007; 25: 99-101. [PubMed]
6. Farah RE, Shay MD. Pulmonary sarcoidosis associated with etanercept therapy. Pharmacotherapy 2007; 27: 1446-1448. [PubMed]
7. Kudrin A, Chilvers ER, Ginawi A, Hazleman BL, Griffiths MH, Thiru S, Ostor AJ. Sarcoid-like granulomatous disease following etanercept treatment for RA. J Rheumatol 2007; 34: 648-649. [PubMed]
8. Louie GH, Chitkara P, Ward MM. Relapse of sarcoidosis upon treatment with etanercept. Ann Rheum Dis 2008; 67: 896-868. [PubMed]
9. Sturfelt G, Christensson B, Bynke G, Saxne T. Neurosarcoidosis in a patient with rheumatoid arthritis during treatment with infliximab. J Rheumatol 2007; 34: 2313-2314. [PubMed]
10. Ishiguro T, Takayanagi N, Kurashima K, Matsushita A, Harasawa K, Yoneda K, Tsuchiya N, Miyahara Y, Yamaguchi S, Yano R, Tokunaga D, Saito H, Ubukata M, Yanagisawa T, Sugita Y, Kawabata Y. Development of sarcoidosis during etanercept therapy. Intern Med 2008; 47: 1021-1025. [PubMed]
11. Toussirot È, Pertuiset È, Kantelip B, Wendling D. Sarcoidosis occurring during anti-TNF-α treatment for inflammatory rheumatic diseases: report of two cases. Clin Exp Rheumatol 2008; 26: 471-475. [PubMed]
12. Massara A, Cavazzini L, La Corte R, Trotta F. Sarcoidosis appearing during anti-tumor necrosis factor alpha therapy: a new “class effect” paradoxical phenomenon. Two case reports and literature review. Semin Arthritis Rheum 2010; 39: 313-319. [PubMed]
13. Dhaille F, Viseux V, Caudron A, Dadban A, Tribout C, Boumier P, Clabaut A, Lok C. Cutaneous sarcoidosis occurring during anti-TNF-alpha treatment: report of two cases. Dermatology 2010 DOI:10.1159/000275676 [PubMed]
14. Naranjo CA, Busto U, Sellers EM, Sandor P, Ruiz I, Roberts EA, Janecek E, Domecq C, Greenblatt DJ. A method for estimating the probability of adverse drug reaction. Clin Pharmacol Ther 1981; 30: 239-245. [PubMed]
15. Ziegenhagen MW, Muller-Quernheim J. The cytokine network in sarcoidosis and its clinical relevance. J Intern Med 2003; 253: 18-30. [PubMed]
16. Doty JD, Mazur JE, Judson MA. Treatment of sarcoidosis with infliximab. Chest 2005; 127: 1064-1071. [PubMed]
17. Callejas-Rubio JL, Ortego-Centeno N, Lopez-Perez L, Benticuaga MN. Treatment of therapy-resistant sarcoidosis with adalimumab. Clin Rheumatol 2006; 25: 596-597. [PubMed]
18. Mouston AE, Matekovits A, Dessinioti C, Antoniou C, Sfikaki PP, Stratigos AJ. Cutaneous side effects of anti-tumor necrosis factor biologic therapy: a clinical review. J Am Acad Dermatol 2009; 61: 486-504. [PubMed]
© 2010 Dermatology Online Journal

