Longitudinal melanonychia induced by capecitabine
Published Web Location
https://doi.org/10.5070/D39207d9jrMain Content
Longitudinal melanonychia induced by capecitabine
Taraneh Paravar MD, Sharon R Hymes MD
Dermatology Online Journal 15 (10): 11
Department of Dermatology, University of Texas MD Anderson Cancer Center, Houston, Texas. Taraneh.paravar@uth.tmc.eduAbstract
Capecitabine is an oral prodrug of 5-fluorouracil (5-FU), used in the treatment of metastatic colon and breast cancers; it is also under investigation for use in gastric cancers. Multiple cutaneous adverse effects have been reported with the use of capecitabine including acral erythema, pyogenic granulomas, inflammation of actinic keratoses, cutaneous and mucosal hyperpigmentation, leopardlike vitiligo, radiation recall, onycholysis, onychomadesis, and subacute cutaneous lupus. To our knowledge, no cases of capecitabine-induced linear melanonychia have been reported to date in the literature.
Case report
A 41-year-old female presented with a three-month history of dark lines on her fingernails. A diagnosis of metastatic breast carcinoma had been made in October 2003 and soon thereafter she received seven treatments with paclitaxel with poor response and subsequently four cycles of fluorouracil, adriamycin, and cyclophosphamide without response. In March 2004 she underwent a left modified radial mastectomy with axillary node dissection and was given one month of tamoxifen. She was disease free until January 2006 when she was evaluated for visual disturbances and was found to have choroidal metastasis. Upon restaging she was found to have hilar adenopathy as well as pleural, adrenal, and vertebral metastases. In February 2006 she began goserelin treatment and during February and March of that year received radiation therapy to the bilateral orbits and spine. In March 2006 she began anastrozole. In July 2006 she received one month of endoxin therapy. She subsequently received radiation therapy for further vertebral metastases in August 2006.
In September 2006 she began treatment with capecitabine, 1500 mg in the morning and 1000 mg in the evening for two-week cycles with a one week break in between. Two years later she continued to be on capecitabine. Of note, when she began treatment with this agent, she reportedly developed an urticarial reaction and, therefore, was changed during the second cycle to 1000 mg twice a day for ten days of therapy with ten days of break. Within one month of therapy the patient noticed itching and peeling of her palms and soles. Six months after treatment she was found to have onycholysis of her right first toenail as well as diffuse hyperpigmentation of her skin. In March 2008 the patient noticed dark lines on her left thumbnail as well as the second and fourth fingernails of her right hand. In addition, on her 2nd, 3rd, and 4th fingernails bilaterally, clinicians noticed a single transverse white line, parallel to the lunula. The patient's medical history was otherwise positive only for cervical dysplasia. The patient's other medications included zoledronic acid, selenium supplements, vitamin E supplements, turmeric, and thymol application to her toenails.
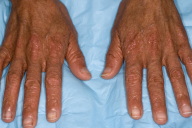 | 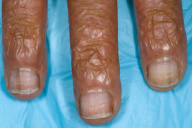 |
| Figure 1 | Figure 2 |
|---|
Clinical examination revealed generalized hyperpigmentation on the entire body. Examination of the extremities revealed linear "melanonychia" on the second and fourth fingernails of the right hand as well as first fingernail of the left hand (Figs. 1 & 2). Transverse depressions of the mid-portion of the bilateral fingernails were seen. In addition, she had dystrophy, onycholysis, and yellow discoloration of all of her toenails.
Discussion
Capecitabine is a carbamate derivative of 5'-deoxy-5-fluorouracil [1]. It is metabolized to 5-FU after oral absorption of this prodrug form through the intenstine via three enzymatic steps with final conversion to 5-FU by thymidine phosporylase. This enzyme is found at higher levels in tumor cells compared to healthy tissue, consequently accounting for the lower systemic toxicity of capecitabine compared to 5-FU.
Longitudinal melanonychia or melanonychia striata manifests as a brown or brown-black longitudinal band on the fingernails or toenails. It is seen secondary to the presence of melanin within the nail plate. It may be associated with an increased synthesis of melanin and/or an increased number of melanoncytes. The presence of a solitary broad longitudinal band of pigmentation with extension over the proximal nail fold (Hutchinson sign) raises concern for melanoma. A benign etiology can be suggested by the presence of multiple lesions and onset in childhood, especially in darker skin types including V or VI [2,3]. Medications associated with longitudinal "melanonychia" include minocycline [4], hydroxyurea [5], and AZT [6]. PUVA treatment has also been related to this condition [7]. Associated disorders include Laugier-Hunziker syndrome, Peutz-Jegher [3] syndrome, and Addison disease [8].
Although multiple cutaneous adverse effects have been reported with the use of capecitabine [9], the specific association with capecitabine and longitudinal melanonychia has not been reported. There have been cases of longitudinal melanonychia associated with a combination of 5-FU, adriamycin, and cyclophosphamide [10], in addition to transverse leukonychia in these patients. If 5-FU is associated with linear melanonychia, it would not be surprising that the pro-drug, capecitabine, would have the same effect. In addition, given the presence of diffuse hyperpigmentation in this patient, as has been previously reported with capecitabine [11], we may also expect increased pigmentation of the nails as well. The pathogenesis of this is unknown. This pigmentation did not develop until over 1 year after start of capecitabine therapy, in contrast to development of acral erythema within one month of treatment, as has been previously reported [12]. Of note, the presence of multiple transverse depressions of her fingernails allows us to interpret them as Beau lines, a sign of nail matrix toxicity resulting in a temporary arrest in keratinization. This finding can be observed during chemotherapy [13] as well as systemic illnesses. Capecitabine may have been the causative agent in the development of the Beau lines, although the timing of this finding was unclear in this patient's history.
Awareness of the dermatologic side effects of capecitabine is crucial given the increased use in the treatment of various cancers. A biopsy was not performed because these lesions were multiple and felt to be benign in nature. She will be monitored for progression.
References
1. Walko, CM and Lindley, C. Capecitabine: a review. Clin.Ther. 2005 Jan;27(1):23-44. [PubMed]2. Goldberg, DJ. Melanonychia striata longitudinalis: multiple benign pigmented streaks in a Caucasian. J.Dermatol.Surg.Oncol. 1986 Feb;12(2):188-9. [PubMed]
3. Ronger, S, Touzet, S, Ligeron, C, Balme, B, Viallard, AM, Barrut, D, Colin, C, Thomas, L. Dermoscopic examination of nail pigmentation. Arch.Dermatol. 2002 Oct;138(10):1327-33. [PubMed]
4. Mallon, E and Dawber, RP. Longitudinal melanonychia induced by minocycline. Br.J.Dermatol. 1994 Jun;130(6):794-5. [PubMed]
5. Hernandez-Martin, A, Ros-Forteza, S, de Unamuno, P. Longitudinal, transverse, and diffuse nail hyperpigmentation induced by hydroxyurea. J.Am.Acad.Dermatol. 1999 Aug;41(2 Pt 2):333-4. [PubMed]
6. Tosti, A, Gaddoni, G, Fanti, PA, D'Antuono, A, Albertini, F. Longitudinal melanonychia induced by 3'-azidodeoxythymidine. Report of 9 cases. Dermatologica. 1990;180(4):217-20. [PubMed]
7. MacDonald, KJ, Hargreaves, GK, Ead, RD. Longitudinal melanonychia during photochemotherapy. Br.J.Dermatol. 1986 Mar;114(3):395-6. [PubMed]
8. Prat, C, Vinas, M, Marcoval, J, Jucgla, A. Longitudinal melanonychia as the first sign of Addison's disease. J.Am.Acad.Dermatol. 2008 Mar;58(3):522-4. [PubMed]
9. Heidary, N, Naik, H, Burgin, S. Chemotherapeutic agents and the skin: An update. J.Am.Acad.Dermatol. 2008 Apr;58(4):545-70. [PubMed]
10. Bianchi, L, Iraci, S, Tomassoli, M, Carrozzo, AM, Nini, G. Coexistence of apparent transverse leukonychia (Muehrcke's lines type) and longitudinal melanonychia after 5-fluorouracil/adriamycin/cyclophosphamide chemotherapy. Dermatology. 1992;185(3):216-7. [PubMed]
11. Tavares-Bello, R. Capecitabine-induced hand-foot syndrome and cutaneous hyperpigmentation in an elderly vitiligo patient. J.Eur.Acad.Dermatol.Venereol. 2007 Nov;21(10):1434-5. [PubMed]
12. Blum, JL, Jones, SE, Buzdar, AU, LoRusso, PM, Kuter, I, Vogel, C, Osterwalder, B, Burger, HU, Brown, CS, Griffin, T. Multicenter phase II study of capecitabine in paclitaxel-refractory metastatic breast cancer. J.Clin.Oncol. 1999 Feb;17(2):485-93. [PubMed]
13. Piraccini, BM, Iorizzo, M, Starace, M, Tosti, A. Drug-induced nail diseases. Dermatol.Clin. 2006 Jul;24(3):387-91. [PubMed]
© 2009 Dermatology Online Journal

