Eccrine angiomatous hamartoma
Published Web Location
https://doi.org/10.5070/D38zc8d63qMain Content
Eccrine angiomatous hamartoma
Chicky Dadlani MD1, Seth J Orlow MD PhD2
Dermatology Online Journal 12 (5): 9
1. University of California Davis Department of Dermatology 2. Department of Dermatology and Pediatrics, New York University School of Medicine, New York
Abstract
A 7-year-old girl presented with asymptomatic bruise-like hairy nodules on her right lower leg since 8 months of age. Histopathology demonstrated an increased number of blood vessels and eccrine glands, thicker collagen bundles, and a terminal hair follicle in catagen phase. The patient was diagnosed with multiple eccrine pilar angiomatous nevi, an unusual variant of eccrine angiomatous hamartomas. The natural course of eccrine angiomatous hamartomas is typically slow growth and benign behavior. Simple excision is usually curative and is reserved for painful or cosmetically disfiguring lesions. Our patient's nevus is large and multifocal, making excision more challenging.
Clinical synopsis
A 7-year-old girl presented for re-evaluation of bruise-like, hairy nodules noted on her right lower leg since 8 months of age. She was seen at 1 year of age for an initial consultation at the New York University pediatric dermatology clinic. Her nodules had spread over time and now involved most of the anterior right leg from above the knee down to her ankle. She had two additional lesions on her right posterior thigh and lower mid-back. The patient was adopted from China at 10 months of age and documentation from birth did not indicate the presence of any lesions. Her lesions have increased in number and grown proportionately with the patient. The parents describe sweating of the nodules when the patient is hot. The size of the lesions is described as somewhat variable from day-to-day. They have not been painful. She is otherwise developmentally normal and has no musculo-skeletal abnormalities. Her past medical history was significant for hay fever, atopic dermatitis, and hives.
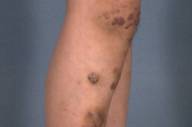
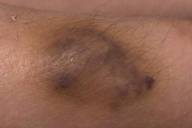
Physical examination revealed multiple irregular, 2-3 cm nodules with an overlying ecchymotic to maroon surface beginning above the right patella extending down to the ankle. They were located mainly along the pretibial surface but included the medial aspect of the knee. Similar lesions were present on the right posterior upper thigh and lower mid-back. Nodules were of varying firmness and had no pulsations or bruits. Several of the lesions had areas of increased, darker, and coarser terminal hairs. Stroking failed to elicit muscular contraction. Increased sweating was present on the lesions. No leg length discrepancy was present and the patient had full range of motion of both lower extremities. Examination of the hair, nails and mucous membranes were unremarkable.
Histopathological examination showed a thickened epidermis and an increased number of small and medium-sized blood vessels with thin muscular walls of uneven thickness. An increased number of eccrine glands with large coils composed of an increased number of tubules and ducts with a normal proportion of cells were noted in the dermis. There was abundant fibromyxomatous stroma in these coils. The dermis appeared to have increased thickness with mature fat cells. Collagen bundles were thicker and in haphazard array. Some collagen bundles were oriented perpendicular to the skin surface. There was a terminal hair follicle in the catagen phase. The clinical and histopathological findings supported a diagnosis of multiple eccrine pilar angiomatous nevi.
 |  |
| Figure 1 | Figure 2 |
|---|---|
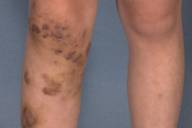
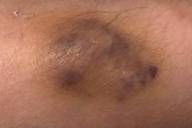
| Figure 1: Multiple irregular, nodules 2-3 cm in size with an overlying ecchymotic to maroon surface Figure 2: Increased sweating is present on the nodules. | |
The patient has been followed over several years with no intervention during this time. Most recently, surgical excision of these masses has been considered due to their increased size and bothersome sweating. An MRI with and without contrast was requested to further delineate the full extent of her nevi. Laser hair removal and depilatory creams were discussed as treatment options for the increased hair.
Comment
As described in Sanmartin et al., Beier in 1985 described a painful, sudoriferous skin nodule of angiomatous nature, which he called sudoriferous angioma [1]. Vilanova et al. [2], referred to this lesion as sweating angiomatous hamartoma in 1963. Then in 1968, Hyman described a similar lesion as eccrine angiomatous hamartoma [3].
Eccrine angiomatous hamartoma (EAH) is a rare, benign cutaneous tumor usually present at birth or during early infancy and childhood. Clinically, EAH presents as an angiomatous lesion, usually solitary, although several cases with multiple lesions have been described [1, 2, 4]. EAH, generally asymptomatic, occasionally presents with pain and focal hyperhidrosis (accounting for the designation of sudoriferous angioma adopted by some authors). The hyperhidrosis is presumably an expression of its eccrine component [1].
On histopathology, EAH is characterized by a dermal proliferation of well-differentiated eccrine secretory and ductal elements closely associated with thin-walled angiomatous channels [5]. In addition, unusual histopathologic variants have been reported and include the infiltration of adipose tissue [6, 7], increased dermal mucin [6], and the presence of apocrine glands [8] or pilar structures [6, 9, 10, 11] as was found in our case.
In 1971, Zeller and Goldman first described an eccrine pilar angiomatous nevus in a 37-year-old patient [9]. They hypothesized a heterotypic dependency during organogenesis to account for the embryonic origin of the three structures (eccrine, pilar, and vascular) in the nevus. According to Zeller and Goldman's theory, altered chemical interactions between the differentiating epithelium and mesenchyme result in the hamartomatous growth of these elements, creating an abnormal proliferation of vascular and eccrine structures [9].
The differential diagnosis of EAH may include an eccrine nevus, tufted angioma, macular telangiectatic mastocytosis, nevus flammeus, glomus tumor, and smooth muscle hamartoma. These entities can be readily differentiated by histopathology.
While definitive diagnosis is based upon histology, MRI and ultrasound are useful to delineate the extent of soft tissue and vascular masses. The natural history of EAH is benign and typically slow-growing. Although aggressive treatment is generally unwarranted, simple excision is usually curative and is reserved for painful or cosmetically disfiguring lesions [5]. Our patient's EAH is large and multifocal, making excision more challenging.
References
1. Sanmartin O, Botella R, Alegre V, Martinez A, Aliaga A. Congenital eccrine angiomatous hamartoma. Am J Dermatopathol, 1992 Apr;14(2):161-4. PubMed2. VILANOVA X, PINOL-AGUADE J, CASTELLS A. (Secreting sudoriferous angiomatous hamartoma.( Dermatologica. 1963;127:9-16. French. No abstract available. PubMed
3. Hyman AB, Harris H, Brownstein MH. Eccrine angiomatous hamartoma. NY State J Med. 1968 Nov;68(21):2803-6. No abstract available. PubMed
4. Domonkos AN, Suarez LS. Sudoriparous angioma. Arch Dermatol. 1967 Nov;96(5):552-3. No abstract available. PubMed
5. Martinelli PT, Tschen JA. Eccrine angiomatous hamartoma: a case report and review of the literature. Cutis. 2003 Jun;71(6):449-55. PubMed
6. Seraly MP, Magee K, Abell E, Bridenstine J, Jegasothy BV. Eccrine-angiomatous nevus, a new variant. J Am Acad Dermatol. 1993 Aug;29(2 Pt 1):274-5. No abstract available. PubMed
7. Smith C, Montesinos E, Revert A, Ramon D, Molina I, Jorda E. Eccrine angiomatous hamartoma: report of three patients. Pediatr Dermatol. 1996 Mar-Apr;13(2):139-42. PubMed
8. Sulica RL, Kao GF, Sulica VI, Penneys NS. Eccrine angiomatous hamartoma (nevus): immunohistochemical findings and review of the literature. J Cutan Pathol. 1994 Feb;21(1):71-5. PubMed
9. Zeller DJ, Goldman RL. Eccrine-pilar angiomatous hamartoma: a report of a unique case. Dermatologica. 1971;143(2):100-4. No abstract available. PubMed
10. Aloi F, Tomasini C, Pippione M. Eccrine angiomatous hamartoma: a multiple variant. Dermatology. 1992;184(3):219-22. PubMed
11. Velasco JA, Almeida V. Eccrine-pilar angiomatous nevus. Dermatologica. 1988;177(5):317-22. PubMed
© 2006 Dermatology Online Journal