Occupational contact allergy to cephalosporins
Published Web Location
https://doi.org/10.5070/D389c0s3stMain Content
Letter: Occupational contact allergy to cephalosporins
Joana Antunes MD, Raquel Silva, David Pacheco, Rita Travassos, Paulo Filipe
Dermatology Online Journal 17 (5): 13
Hospital de Santa Maria, Lisboa, PortugalAbstract
Contact sensitivity to systemically administered drugs occurs mainly among healthcare workers and is frequently caused by antibiotics. A 32-year-old nurse presented with a 1½ year history of hand dermatitis and a 2 month history of palpebral eczema, which were clearly work related. Patch tests with standard and gloves series were negative. Testing of the products commonly handled by the patient were positive for cefradine and cefazolin. Testing of other cephalosporins the patient had not come in contact with were also positive for cefuroxime, ceftriaxone, and cefotaxime. This cross-reactivity may be explained by similar molecular structures. The patient stopped preparing cephalosporin solutions for systemic administration and the lesions cleared.
 |
| Figure 1 |
|---|
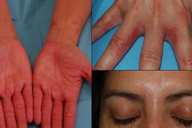
| Figure 1. (a) Eczema of the palms and forearms, (b) eczematous lesions on interdigital folds, (c) palpebral eczema |
Nurses are frequently affected by hand eczema, either due to irritant or allergic sensitization [1]. Occasionally, contact sensitization occurs in association of preparation of systemically administered drugs, mostly antibiotics [2].
A 32-year-old female nurse, working in the gynecology department, presented with a 1½ year history of hand eczema and a 2 month history of palpebral eczema (Figure 1). She reported that the lesions improved during the holidays and worsened when she returned to work. The patient had no personal history of atopy but had a mother with asthma and a brother with hay fever. Her work included performing patients’ hygiene and the preparation of intravenously administered drugs. She also admitted to extensive use of latex/rubber gloves and hand sanitizers.
 Table 1
Table 1
Patch tests were performed using the Portuguese standard series and rubber gloves series (Chemotechnique®). All tests from these two were negative. The daily used disinfectants and the drugs handled by the patient were then tested (both the active principles manufactured by Chemotechnique® and the patient’s own drugs, at full strength and in progressive dilutions), in IQ chambers®. The results are shown in the following table (Table 1).
The patient denied ever having taken these drugs or having a previous history of cutaneous drug eruption. A diagnosis of occupational contact dermatitis to cefradine and cefazolin was made.
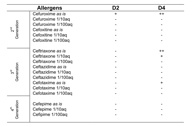 Table 2
Table 2
Both cefradin and cefazolin are first generation cephalosporins. To exclude possible cross-reactivity with other generation cephalosporins, 6 weeks later, the patient was retested with all other cephalosporins available at the hospital pharmacy. We obtained the following results shown in the second table (Table 2).
Occupational contact sensitization to 1st (cefradine, cefazolin), 2nd (cefuroxime) and 3rd (ceftriaxone, cefotaxime) generation cephalosporins was confirmed. The patient was advised to avoid preparation of cephalosporin solutions for systemic administration and also to refrain from taking these drugs in the future because of the risk of systemic contact dermatitis.
Cephalosporins are a class of β-lactam antibiotics that share the β-lactam ring structure and mode of action with penicillins, but are inherently resistant to β-lactamase [3]. They have a common cephem nucleus (Figure 2a), which can be modified by 2 side chains to gain different antimicrobial properties.
 |
| Figure 2 |
|---|
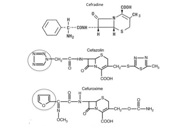
| Figure 2. (a) Cephalosporins’ common nucleus, (b) Structural formulas of the cephalosporins with positive patch tests with the tetrazolic group highlighted. |
Cross-reactivity between penicillins and cephalosporins is said to be 5 percent to 10 percent [3], mainly regarding first-generation cephalosporins. No reaction was elicited by the penicillins tested in our patient (ampicillin, amoxicillin, piperacillin/tazobactam, flucloxacillin). This is consistent with the idea that sensitization is not caused by the β-lactam ring, but rather by cephalosporin side chains [4].
Our patient also showed positive reactions when tested with other cephalosporins with which she had not previously come in contact (cefuroxime, ceftriaxone, cefotaxime). All these drugs share a common tetrazolic group with cefazolin, which may be responsible for the cross-sensitization (Figure 2b).
Healthcare workers are prone to allergic contact dermatitis caused by drugs, especially by coming in contact with the allergens during reconstitution of solutions. The fact that our patient also had periorbital lesions may be explained by needle gushing, hand contact, or airborne diffusion [5]. The dermatitis resolved after the patient stopped preparing cephalosporin solutions for systemic administration.
References
1. Schnuch A, Uter W, Geier J, Frosch PJ, Rustemeyer T. Contact allergies in healthcare workers. Results from the IVDK. Acta Derm Venereol 2008;78:358-363 [PubMed]2. Gielen K, Goossens A. Occupational allergic contact dermatitis from drugs in healthcare workers. Contact Dermatitis 2001;45:273-279 [PubMed]
3. Ashourian N, Cohen PR. Systemic antibacterial agents. In: Comprehensive dermatologic drug therapy, 2nd edition, Wolverton SE - Ed: Philadelphia, Saunders - Elsevier, 2007:39-74
4. Foti C, Bonamonte D, Trenti R, Veña GA, Angelini G. Occupational contact allergy to cephalosporins. Contact Dermatitis 1997;36:104-5 [PubMed]
5. Yesudian PD, King CM. Occupational allergic contact dermatitis from meropenem. Contact Dermatitis 2001;45:53 [PubMed]
© 2011 Dermatology Online Journal

