Fibroepithelioma of Pinkus
Published Web Location
https://doi.org/10.5070/D387v4t5rgMain Content
Fibroepithelioma of Pinkus
Michael W Su MD PhD, Eric Fromer MD, Maxwell A Fung MD
Dermatology Online Journal 12 (5): 2
University of California, Davis Department of DermatologyAbstract
An 88-year-old woman presented with an 8-year history of a slowly enlarging growth on the suprapubic area. A shave excision of this lesion demonstrated fibroepithelioma of Pinkus (FEP). Fibroepithelioma of Pinkus is an indolent growing tumor that traditionally has been classified as a variant of the basal cell carcinoma. More recent evidence favors the classification of FEP as a variant of trichoblastoma. In this case report, we identified a large FEP with benign histologic features suggestive of a follicular origin as demonstrated in part by CK 20 staining and the presence of scattered Merkel cells within the tumor. The pathogenesis of FEP remains enigmatic, and the genetic basis has yet to be fully elucidated. Complete surgical resection is considered curative.
Clinical synopsis
An 88-year-old woman with Alzheimer disease presented to the University of California Davis dermatology department in consultation for a slowly enlarging growth on the suprapubic area. Although this lesion had been present for 8 years, she was previously reassured that the lesion was a giant skin tag that did not warrant surgical removal. Given her baseline dementia, she did not seek further medical attention until the lesion became superficially eroded and bled. Otherwise, this lesion had been asymptomatic without other constitutional symptoms that could be attributed to the growth.
Examination of the suprapubic area revealed a 3 cm firm, polypoid, exophytic tumor that was superficially eroded (Figs. 1 and 2)
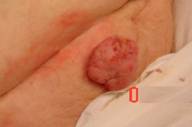 | 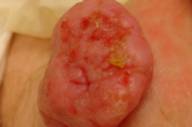 |
| Figure 1 | Figure 2 |
|---|---|
| Superficially eroded, polypoid, exophytic tumor in the suprapubic area. | |
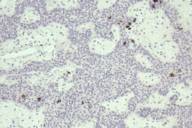 |
| Figure 5 |
|---|
| Cytokeratin 20 staining of Merkel Cells in fibroepithelioma of Pinkus (FEP) and basal cell carcinoma (insert) from the patient at the same office visit |
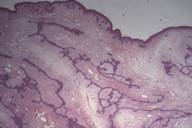
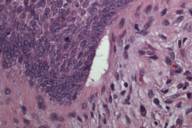
The lesion was excised; histopathological examination revealed narrow inter-anastamosing strands of basaloid cells with variable fibrotic and myxoid stroma in the dermis with peripheral palisading of basal cells and focal clefting between tumor and stroma (Fig. 3 and 4). A cytokeratin 20 (CK20) stain highlighted scattered Merkel cells within the lesion, whereas a conventional basal cell carcinoma (BCC) biopsied from the patient at the same office visit was negative for CK20 (Fig. 5). The clinical presentation and histopathological findings supported a diagnosis of FEP.
Comment
Fibroepithelioma of Pinkus was first described by Herman Pinkus in 1953 who termed it premalignant fibroepithelial tumor of the skin [1]. Although FEP traditionally is considered to be an unusual variant of basal cell carcinoma, its indolent nature and often asymptomatic clinical presentation suggest that it may be best classified as a benign counterpart of BCC, such as a trichoblastoma. This concept was supported by a recent study, representing the largest case series of FEP to date, whereby the features of FEP were compared with those of conventional BCC by immunohistochemical staining [2]. In particular, FEP expressed significantly less p53 oncogene and MIB-1 proliferative marker than the conventional BCC. Moreover, Merkel cells were found within the lesions of FEP similar to many benign follicular tumors, but were absent in the conventional BCC. Finally, FEP consistently displays no infiltration of the subcutis and has no known aggressive clinical course.
In this case report, we identified a large FEP that was initially misdiagnosed clinically as a giant acrochordon. On the same patient, the coincidental finding of conventional BCC at different sites allowed us to support the question of whether FEP is distinct from BCC based on CK20 immunohistochemical staining. The presence of CK20 positive Merkel cells has been used to reliably differentiate benign follicular tumors from BCC [3, 4]. Accordingly, we could readily identify scattered Merkel cells within the lesion of FEP, but not within the control BCC from the same patient (Fig. 5). It is worth noting that in the views of some investigators, the presence of BCC-like areas in FEP, such as illustrated in Fig. 4, may represent a neoplastic process that qualifies FEP as one of the variants of BCC [5]. Despite this histological similarity, the BCC-like areas within an FEP are evidently more closely related to trichoblastoma based on immunohistochemical stains, e.g. presence of Merkel cells and weak expression of p53 oncogene. Fibroepithelioma of Pinkus does not behave clinically as a conventional BCC, e.g., no invasion of the subcutis [2].
The clinical appearances of FEP ranges from a single or multiple, dome-shaped sessile papules to large pedunculated tumors. The color is variable to include shades of pink, yellow, brown, or skin colored. Several forms of FEP, including cystic, pleomorphic, eroded and giant variants, have been described. Therefore, it is not surprising that the clinical differential diagnosis is vast, including acrochordon, nevus lipomatosus, amelanotic melanoma, compound nevus, hemangioma, neurofibroma, nevus sebaceous, pyoderma gangrenosum, and seborrheic keratosis [6].
FEP has a predilection for females and is found mainly in individuals greater than 50 years of age, whereas BCCs are more common in males [7]. The sites of distribution for FEP are also distinct from those for BCC. Although 80 percent of BCCs are found on sun-exposed areas of the head and neck, FEPs are typically found on the lower trunk, and especially on the lumbar and sacral region. These differences suggest that UV exposure might be more important for the pathogenesis of BCC than it is for FEP.
The genetic basis of FEP is currently not completely understood but the work on the patched (ptch) transmembrane molecule may be relevant [8]. Genetic mutation of ptch eliminates the negative regulation on the Hedgehog pathway. The constitutive activation of the Hedgehog pathway is known to be the basis for 30-40 percent of sporadic BCC, as well as the basal cell nevus syndrome. In the ptch heterozygous knock-out mouse, exposure to ionizing radiation predisposes to development of BCC and trichoblastomas that resemble FEP on histology [2, 8]. Nevertheless, patients with basal cell nevus syndrome and ptch mutation have not been documented to develop FEP, and other genetic aberrations, either related or distinct from the Hedgehog pathway, appears obligatory.
Treatment options of FEP are similar to those for BCC [9]. Unlike BCC, FEP is not known to have an aggressive clinical course and has not been reported to result in death of patients. The complete excision of the tumor is considered curative. Other modalities such as electrodesiccation and curettage or Mohs micrographic surgery may be considered.
References
1. Pinkus H. Premalignant fibroepithelial tumors of skin. AMA Arch Derm Syphilol 1953. 67: 598-615.2. Bowen AR, LeBoit, PE. Fibroepithelioma of pinkus is a fenestrated trichoblastoma. Am J Dermatopathol. 2005 Apr;27(2):149-54. PubMed
3. McNiff JM, Eisen RN, Glusac EJ. Immunohistochemical comparison of cutaneous lymphadenoma, trichoblastoma, and basal cell carcinoma: support for classification of lymphadenoma as a variant of trichoblastoma. J Cutan Pathol. 1999 Mar;26(3):119-24. PubMed
4. Schulz T, Hartschuh W. Merkel cells are absent in basal cell carcinomas but frequently found in trichoblastomas. An immunohistochemical study. J Cutan Pathol. 1997 Jan;24(1):14-24. PubMed
5. Ackerman AB, Gottlieb GJ. Fibroepithelial tumor of pinkus is trichoblastic (Basal-cell) carcinoma. Am J Dermatopathol. 2005 Apr;27(2):155-9. No abstract available. PubMed
6. Cohen PR, Tschen JA. Fibroepithelioma of Pinkus presenting as a sessile thigh nodule. Skinmed. 2003 Nov-Dec;2(6):385-7. No abstract available. PubMed
7. Betti R, Inselvini E, Carducci M, Crosti C. Age and site prevalence of histologic subtypes of basal cell carcinomas. Int J Dermatol. 1995 Mar;34(3): 174-6. PubMed
8. Aszterbaum M, Epstein J, Oro A, Douglas V, LeBoit PE, Scott MP, Epstein EH Jr. Ultraviolet and ionizing radiation enhance the growth of BCCs and trichoblastomas in patched heterozygous knockout mice. Nat Med. 1999 Nov;5(11):1285-91. PubMed
9. Mehregan D, Pegouske D. Premalignant Fibroepithelial Tumor (Pinkus Tumor). eMedicine 2005.
© 2006 Dermatology Online Journal