Eruptive xanthomas
Published Web Location
https://doi.org/10.5070/D37vt3m2bdMain Content
Eruptive xanthomas
Narayan S. Naik
Dermatology Online Journal 7(2): 11
New York University Departent of DermatologyHistory
A 38 year-old man presented with a one year history of an eruption on the neck, extremities, back, and buttocks. For one year lesions have appeared in crops over the extremities and torso. He denies pruritus but occasionally notes tenderness over the lesions after slight trauma. He had recently been evaluated in a medical clinic for abdominal complaints, which have resolved with the administration of H2 antihistamines. He has been otherwise healthy. There is no history of a similar skin disorder during his childhood or in any of his family members. He also denies a family history of premature cardiovascular events. Treatment with gemfibrozil was initiated for his lipid abnormalities.
Physical Examination
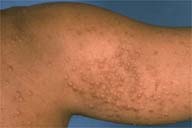 | 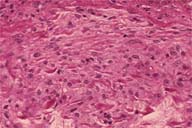 |
| Figure 1 | Figure 2 |
|---|
Yellow papules with an erythematous hue at their bases were noted over the extensor aspects of the arms, posterior portion of the neck, back, and buttocks. Yellow, confluent, nodular plaques were present over both elbows. No lesions were noted over the cornea, eyelids, mucous membranes, palms, or achilles tendons.
Comment
Eruptive xanthomas are yellow-orange-to-red-brown papules that are often surrounded by an erythematous halo. They appear in crops on the buttocks, extensor surfaces of the extremities, and flexural creases. Acutely, variable amounts of pruritus and pain occur. A Koebner reaction may be present. Lesions usually resolve spontaneously over weeks and may result in hypertrophic scars. Histologically, foamy macrophages are present in the dermis with an inflammatory infiltrate of lymphocytes and neutrophils.
Eruptive xanthomas occur in the setting of chylomicronemia and hypertriglyceridemia. This may be due to a primary hyperlipoproteinemia resulting from a genetic deficiency of lipoprotein lipase (Type 1 hyperlipoproteinemia) or familial hyperlipoproteinemia (Type V). Eruptive xanthomas often also occur secondarily in individuals unresponsive to insulin. Insulin is required for the normal triglyceride clearing function of lipoprotein lipase. Whenever insulin deficiency is present, an acquired liproprotein lipase deficiency exists, which results in impaired clearance of chylomicrons and very-low-density lipoproteins causing the resultant hypertriglyceridemia. Rarely, eruptive xanthomas have been reported with hypothyroidism, nephrotic syndrome, and von Gierke's glycogen storage disease. They have been noted also after ingestion of alcohol, glucocorticoids, estrogens, and retinoids.
Other features of hyperlipidemia often noted in patients with eruptive xanthomas include lipemia retinalis, hepatosplenomegaly, and abdominal pain. The abdominal pain may be secondary to intestinal ischemia from increased blood viscosity, stretching of organ capsules by lipid deposition in the liver or spleen, or chronic episodes of pancreatitis.
Adequate treatment involves controlling the underlying hyperlipidemia with strict dietary therapy. Weight reduction and carbohydrate intake restriction are helpful in cases associated with insulin resistance.
References
Haber C, Kwiterobich PO Jr. Dyslipoproteinemia and xanthomatosis. Pediatr Dermatol 1:261, 1984Parker F. Xanthomas and hyperlipidemias. J Am Acad Dermatol 13:1, 1985
Cruz PD, et al. Dermal, subcutaneous, and tendon xanthomas: diagnostic markers for specific lipoprotein disorders. J Am Acad Dermatol 19:95, 1988
Russo GG. Hyperlipidemias. Clin Dermatol 14:367, 1996
© 2001 Dermatology Online Journal

