Genital primary herpes simplex infection in a 5-month-old infant
Published Web Location
https://doi.org/10.5070/D36wg6f02hMain Content
Genital primary herpes simplex infection in a 5-month-old infant
Ana Batalla MD1, Ángeles Flórez MD PhD1, Paula Dávila MD1, Vanesa Ojea MD2, Teresa Abalde MD1, Carlos de la Torre MD PhD1
Dermatology Online Journal 17 (8): 8
1. Dermatology Service2. Pediatric Service
Complejo Hospitalario de Pontevedra, Pontevedra, Spain. anacebey@yahoo.es
Abstract
Genital primary herpes simplex infection is very uncommon in infants. Asymptomatic and oral primary infections are the most frequent presentations in this age group. We report a case of genital primary herpetic infection in a 5-month-old male, exclusively breastfed, whose mother suffered from active labial herpes.
Introduction
Primary herpes simplex infection in children is usually asymptomatic, but if symptomatic, it generally presents with gingivostomatitis. Genital primary infection is infrequent in this age group [1, 2, 3, 4]. We report a case of genital primary herpetic infection in a 5-month-old male, exclusively breastfed, whose mother suffered from active labial herpes. We briefly review the characteristics of this entity and discuss the peculiarities of this case.
Case report
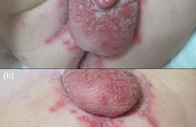
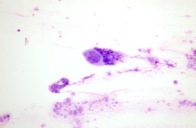
A 5-month-old male presented with a 4-day eruption of genital lesions associated with fever. The infant was exclusively breastfed and his mother suffered from active labial herpes at that moment. On physical examination vesicle-pustules over an erythematous-edematous area, affecting penis, scrotum, perineum, groin, and perianal areas, were observed (Figure 1). Other mucosal membranes or skin surfaces were not affected. Tzanck cytodiagnosis showed giant multinucleated cells with inclusion bodies (Figure 2). Direct fluorescent antibody testing detected herpes simplex virus (HSV)-1 antigen. Polimerase chain reaction (PCR) and cell culture also revealed the presence of HSV-1. Treatment with intravenous acyclovir (20 mg/kg/6 hours/5 days) and topical antiseptics lead to a rapid clinical improvement.
Discussion
Primary infection with HSV-1 or HSV-2 in childhood is asymptomatic in 88 to 99 percent of patients. When symptomatic, patients generally present with gingivostomatitis. A genital primary herpetic infection (PHI) is very uncommon, with few cases reported in the literature [1, 2, 3, 4]. The age of onset ranges between 6 months and 4 years. This characteristic age of onset may be explained by the presence of maternal antibodies during the first six months of life [1]. Nevertheless, approximately 1 percent of adults are seronegative for HSV. The lack of passively transmitted maternal antibodies in these patients might increase the risk of infants for early primary herpetic infection [2, 3].
Genital herpetic infection in adulthood is generally sexually transmitted and mainly caused by HSV-2. On the contrary, genital PHI in childhood is more frequently caused by HSV-1 and most commonly transmitted via asymptomatic carriers.
Auto-inoculation from concomitant oral PHI or carriers with active herpetic infection are other possible avenues [2, 3, 4]. Sexual abuse should be considered in children over 5-years-old when genital lesions alone occur or when HSV-2 is isolated [4, 5].
Clinically, genital PHI is characterized by sudden onset of bilateral clusters of vesicles over erythematous-edematous skin of the genitalia. Lesions may spread to the groin and perianal areas. Fever and malaise may be associated [3].
The definitive diagnosis relies on isolation of HSV directly from the genital tract. Direct methods are viral culture, cytologic diagnosis (Tzanck smear), antigen detection (direct fluorescent antibody testing), and viral DNA detection by PCR. Indirect (serological) methods are by western blot and enzyme immunoassay. It must be pointed out that the Tzanck smear test only gives a presumptive diagnosis because cytological features are identical in the whole of herpesvirus family [3, 4].
As in the case herein reported, the main differential diagnoses are fungal infection and superinfected irritant dermatitis. Other possibilities such as superinfected psoriasis or seborrheic dermatitis, impetigo, or post-traumatic lesions, may also be considered [3].
The prognosis of PHI in childhood depends on the underlying immunological status [3]. Early treatment with acyclovir is effective in PHI. Intravenous therapy is indicated in case of local complications or systemic involvement. Follow-up is recommended because of the risk of recurrences, which tend to decrease in both frequency and severity [3, 4].
In conclusion, we highlight the peculiarities of this case: the very unusual clinical presentation as genital PHI, and the early primary HSV-1 infection in an infant less than 6 months of age whose mother had active labial herpes.
References
1. Kasubi MJ, Nilsen A, Marsden HS, Bergström T, Langeland N, Haarr L. Prevalence of antibodies against herpes simplex virus types 1 and 2 in children and young people in an urban region in Tanzania. J Clin Microbiol. 2006 Aug;44(8):2801-7. [PubMed]2. Taieb A, Body S, Astar I, du Pasquier P, Maleville J. Clinical epidemiology of symptomatic primary herpetic infection in children. A study of 50 cases. Acta Paediatr Scand. 1987 Jan;76(1):128-32. [PubMed]
3. Khaddar RK, Badri T, Ben Hassen A, Bouraoui S, Souissi A, Ben Tekaya N, Dhahri AB. Genital primary herpetic infection in an infant: clinical features, diagnosis and management. Dermatol Online J. 2005 Dec 1;11(3):22. [PubMed]
4. Waggoner-Fountain LA, Grossman LB. Herpes simplex virus. Pediatr Rev. 2004 Mar;25(3):86-93. [PubMed]
5. Reading R, Rannan-Eliya Y. Evidence for sexual transmission of genital herpes in children. Arch Dis Child. 2007 Jul;92(7):608-13. [PubMed]
© 2011 Dermatology Online Journal