A case of chronic expanding hematoma in the tensor fascia lata.
Published Web Location
https://doi.org/10.5070/D36wg5260xMain Content
A case of chronic expanding hematoma in the tensor fascia lata
Mineo Nakano1, Tomoo Kondoh2, Jun Igarashi2, Atsushi Kadowaki2, and Eiichi Arai3
Dermatology Online Journal 7(2): 6
1. Division of Plastic and Reconstructive Surgery, 2. Department of Surgery, Organized Center of Clinical Medicine, International
University of Health and Welfare 3. Department of Pathology, Saitama Medical SchoolAbstract
We describe a patient in whom a chronic expanding hematoma was pathologically confirmed by examination of the resected specimen. It developed gradually in the left lateral thigh, which had been bruised 8 months before, but had produced no mass-related symptoms initially. Computed tomography (CT) showed the mass to be homogeneous with capsule formation, whereas ultrasonography showed it to resemble a multilocular cyst. The lesion was treated by complete excision of a perifascial mass. Grossly, a well-circumscribed, fusiform mass with a soft cystic center and a fibrous pseudocapsule was observed. Histologically, the mass was composed of necrotic debris, fibrin and blood clots. This was surrounded by a rim of hyalinized fibrous tissue with a chronic inflammatory infiltrate and granulation tissue with sprouting new capillaries. CT was unable to discriminate the chronic expanding hematoma from other soft tissue masses, ultrasonography being needed to reveal its characteristics in this case.
Introduction
Chronic expanding hematoma of soft tissue is a rare entity. It was defined by Reid et al. [1], and is characterized by its persistence and by its increasing size for more than a month after the initial hemorrhage. The diagnosis of this uncommon entity is often difficult, it being easily mistaken for one of the relatively more frequent malignant neoplasms. We report a patient in whom a chronic expanding hematoma developed in the tensor fascia lata, and we discuss both the difficulty in making a preoperative diagnosis and the clinicopathologic findings.
Case Report
 |
| Figure 1 |
|---|
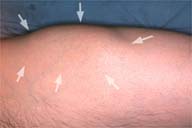
| Figure 1: Lesion in the left lateral thigh. |
A 54-year-old man presented with an 8-month history of a firm, painless mass (approximately 15 x 9 cm) upon examination. He reported that after the initial blunt trauma at the site a bruise had resulted, but no mass had been evident. During the subsequent eight month period he noted development of a mass at the site which gradually enlarged to the size noted upon presentation. The lesion was located in the lateral aspect of his left thigh (Figure 1). The skin was not involved. No left groin lymph nodes were palpable. He denied having a history of coagulopathy or of using any medical agents. Routine laboratory examinations, including coagulation profile and platelet counts, were all normal.
 |  |
| Figure 2 | Figure 3 |
|---|---|
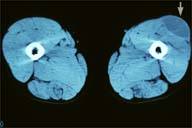
| Figure 2: CT: Soft tissue mass in tensor fascia lata; low-attenuation homogeneous mass and well-defined rim. | |
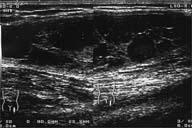
| Figure 3: Ultrasonography: tissue mass resembles a multilocular cyst. | |
CT showed a fusiform soft tissue mass within the deep subcutaneous and perifascial tissue of the tensor fascia lata. It showed up as a lowly-attenuated homogeneous mass with a well-defined rim. There was no enhancement of the lesion with intravenous contrast medium (Figure 2). Ultrasonography revealed that the mass resembled a multilocular cyst (Figure 3).
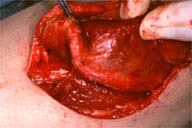
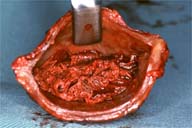
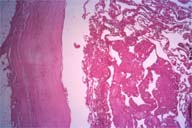
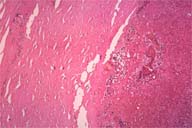
A complete excision of the mass contained in the tensor fascia lata was performed. A perforating vessel from the tensor fascia lata seemed to run into the mass (Figure 4). Grossly, the mass showed soft lobulation with chocolate-brown fluid and a dense fibrous pseudocapsule (Figure 5). Microscopically, the cavity of the mass could be seen to contain necrotic debris, fibrin and blood clots. The inner lining of the cyst wall consisted of hyalinized, hypocellular fibrous tissue with a chronic inflammatory infiltrate and granulation tissue with sprouting new capillaries (Figure 6,7).
The mass was pathologically diagnosed as a chronic expanding hematoma. There were no postoperative complications, and there was no sign of recurrence at the 6-month follow-up.
Discussion
Most hematomas subside without causing any serious clinical problems. However, some persist for long periods and appear clinically as slowly expanding lesions in soft tissues simulating neoplastic growth; these are called chronic expanding hematomas.[1] These lesions are essentially similar to chronic subdural hematomas, pseudotumors in hemophilia, hemorrhagic neuropathy and rectus sheath hematomas.
The precise mechanism responsible for chronic expanding hematomas remains unclear. Bradshaw et al.[2] speculated that the initial trauma results in displacement of skin and subcutaneous fatty tissue away from more deeply located, fixed fascia and underlying muscle, with the consequent formation of blood-filled cysts surrounded by dense fibrous tissue. The lesion's self-perpetuating, expanding nature appears to be due to the irritant effects of blood and its breakdown products leading to repeated exudation or bleeding from capillaries in the granulation tissue of the cyst wall.[3]
The macroscopic and microscopic features seen in the present case were consistent with the chronic organized hematoma being associated with reactive inflammation, and were similar to the findings reported in the existing literature on chronic expanding hematomas. This pathology would seem to support the theory mentioned above. Furthermore, the nutrient vessel we noted running into the mass may have been the origin of the initial hematoma. It may spontaneously have stopped bleeding, and thereafter new capillaries in the inner wall of the granulation tissue produced the retention fluid more gradually.
There have been sporadic reports from various medical fields of chronic expanding hematomas not only in soft tissues, but also in brain, lungs etc. However, to our knowledge, there has been no previous report of this condition in the dermatologic literature. In our review of the literature (in both Japanese and English) concerning chronic expanding hematomas in soft tissues, we found only 41 cases, including this one (Table).[4, 5, 6, 7, 8, 9, 10, 11, 12, 13, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25] In making this count, clinical conditions associated with natural or iatrogenic hemorrhagic diatheses, neoplasms, hemorrhagic neuropathy and rectus sheath hematoma were excluded, as were reports lacking a minute description.
Of the 41 cases found in our review, 29 were male and 12 were female. This condition is most frequently encountered in patients between the ages of 20 and 80 years, although ages outside this range have been reported. The lesions in 30 patients were predominantly located in the lower extremities, including the buttocks, with the other 11 patients having lesions in the neck, head, shoulder, scapula, breast, elbow, or nape. There is evidence to suggest that an antecedent episode of trauma or surgery plays a major role in producing this condition, although 13 cases had no history of trauma. The range of reported clinical latent periods is very wide from 1 month to 57 years. The treatment for these lesions was usually complete excision, with almost no place being found for aspiration or drainage treatment.
According to previous reports,[8, 9, 10, 11, 14, 15, 16, 20, 21, 24] the typical CT findings with respect to this lesion are of a heterogeneous or homogeneous lowly-attenuated mass with or without a partially calcified rim. Interestingly, our CT showed homogeneous fluid within a well-defined wall, although ultrasonography produced a different finding: a multilocular cyst-like appearance. To judge from the literature, the multicystic quality and attenuation values within the lesion appear to change as time goes by. Possibly, ours may represent an immature, early stage of the lesion without calcification, with the result that CT did not show irregularly mixed low-attenuation images. Magnetic resonance (MR) images were not obtained in our case, but it has been reported that MR is a more sensitive diagnostic tool than CT in chronic expanding hematoma because there is a mosaic of differing MR signal intensities from fresh and altered blood components.[24,26] Although various kinds of imaging modalities have been utilized for diagnosis, we should keep in mind that even CT, MR and ultrasonography may not give accurate preoperative data enabling the differentiation of chronic expanding hematomas from other soft tissue neoplasms. Furthermore, when a limited cytology or frozen section sample is viewed, large pleomorphic and mitotic fibrocytes may be found within the organizing clot which may further simulate a malignant neoplasm. In addition, aspiration of the material may not remove the clot contents fully and certainly will not remove the fibrous wall that produced the retention fluid. Therefore,
It seems that complete surgical excision, including the pseudocapsule, is the best treatment for chronic expanding hematoma, because aspiration of the fluid or incomplete excision could lead either to an unconfirmed diagnosis or recurrence.
References
1. Reid JD, Kommareddi S, Lankerani M, Park MC. Chronic expanding hematomas. A clinicopathologic entity. JAMA 1980;244(21):2441-2. PubMed2. Bradshaw JR, Davies GT, Edwards PW, Richards HJ. The radiological demonstration of traumatic cysts due to severe soft tissue trauma. Br J Radiol. 1972;45:905-910.
3. Labadie EL, Glover D. Physiopathogenesis of subdural hematomas: I. Histological and biochemical comparisons of subcutaneous hematoma in rats with subdural hematoma in man. J Neurosurg. 1976;45: 382-392.
4. Friedlander HL, Bump RG. Chronic expanding hematoma of the calf. A case report. J Bone Joint Surg. 1968;50A:1237-1241.
5. Brown CS, Wallace CT. Chronic hematoma: A complication of percutaneous catheterization of the internal jugular vein. Anesthesiology 1976; 45: 368-369.
6. Sterling A, Butterfield WC, Bonner R Jr, Quigley W, Marjani M. Post-traumatic cysts of soft tissue. J Trauma 1977;17(5):392-6. PubMed
7. Vecchione TR. Persistent post-traumatic pseudosheath formation secondary to a movable organized blood clot. J Trauma 1977;17: 480-481.
8. Momoi Y, Kawabata M, Takizawa H, Mikami Y. A case of chronic expanding hematoma in the thigh. Kanto Seikeisaigaigeka Gakkai Zasshi 1985;16: 518.
9. Palatinsky E, Liccardo G, DiLorenzo N. Chronic subperitoneal hematoma of the skull in an adult: a case report, Neurosurgery 1986;19:294-296.
10. Lewis VL, Johnson PE. Chronic expanding hematoma. Plast Reconstr Surg 1987;79: 465-467.
11. Lovern RE, Bosse DA, Hartshorne MF, Bauman JM, Billingsley JL, Byrd BF, Momii GD, Crooks LA. Organizing hematoma of the thigh. Multiple imaging techniques. Clin Nucl Med 1987;12(8):661-4. PubMed
12. Sato N, Tomioka K, Kobayashi K, Ishizaka H, Kurihara M, Mizuno H, Amanuma M, Heishiki A. Idiopathic giant hematomas in soft tissue: difficulty of in diagnosing malignant tumors. Nippon Iji Shinpou 1989;3376:79-82.
13. Sugita H, Morita S, Iwaki T, Inoue M, Hiasa H, Maekawa M, Sakayama K, Tao S, Kato M. A case of giant hematoma suspected to be a soft tissue tumor in the thigh. Ehime Igaku 1990 9:204.
14. Okada K, Sato K, Ohba M, Kataoka Y, Tsuboi J. Chronic expanding hematoma suspected of soft tissue tumor in the thigh and the buttock. Rinsho Seikeigeka 1992;27:1083-1089.
15. Ishiguro M, Ohtsuka T, Tsuji H, Nimura A, Matsui N. A case of chronic expanding hematoma in the right lower limb. Tyubu Nippon Seikeigeka Saigaigeka Gakkai Zasshi 1993;29:1162.
16. Tsuyama K, Hirokawa Y, Ishida M, Ueda S. Subcutaneous hematoma as a complication of the rib fracture, resembling soft tissue tumor; a case report. Rinsho Seikeigeka 1993;28:1083-1085.
17. Kitaura T, Shimizu T. A case of giant hematoma in the ankle joint suspected to be a malignant soft tumor. Shiga Igaku 1994;16:71.
18. Levy O, Ganel A, Givon U, Schindler A, Heim M. Expanding mass in the gluteal area of a 7-year-old child. Orthop Rev 1994;23: 826-831.
19. Daw JL, Lewis VL, Smith JW. Chronic expanding hematoma within a periprosthetic breast capsule, Plast Reconstr Surg. 97: 1469-1472, 1996.
20. Yamamoto N, Asato H, Takushima A, Aiba E. Chronic expanding hematoma: case report. Keiseigeka 1997;40:521-527.
21. Mentzel T, Goodlad JR, Smith MA, Fletcher CD. Ancient hematoma: a unifying concept for a post-traumatic lesion mimicking an aggressive soft tissue neoplasm. Mod Pathol 1997;10(4):334-40. PubMed
22. Mimoto H, Onituka A, Miyauti T, Katagiri Y, Hirose M, Shimamoto T. A case of chronic expanding hematoma in left elbow. Gifu Sekijujibyoin Igaku Zasshi 1999;11:13-17.
23. Kurokawa M, Muneuchi I, Fu Ichiryu, Tanaka K. Two cases of a chronic expanding hematoma in the head and neck of infant. Nippon Keiseigeka Gakkai Kaishi 1999;19:583-587.
24. Aoki T, Nakata H, Watanabe H, Maeda H, Toyonaga T, Hashimoto H, Nakamura T. The radiological findings in chronic expanding hematoma. Skeletal Radiol 1999;28:396-401.
25. Fukuda R, Ohyatsu Y, Miyoshi H, Uchinuma E. A case of chronic expanding hematoma. Nippon Keiseigeka Gakkai Kaishi 2000;20:277.
26. Akata S, Ohkubo Y, Jinho P, Saito K, Yamagishi T, Yoshimura M, Kotake F, Kakizaki D, Abe K MR. features of a case of chronic expanding hematoma, Clin Imaging 2000;24:44-46.
© 2001 Dermatology Online Journal