Generalized lichen nitidus successfully treated with pimecrolimus 1 percent cream
Published Web Location
https://doi.org/10.5070/D365p7c1s7Main Content
Letter: Generalized lichen nitidus successfully treated with pimecrolimus 1 percent cream
Susan Farshi MD MPH, Parvin Mansouri MD
Dermatology Online Journal 17 (7): 11
Tehran University of Medical Sciences, Imam HospitalAbstract
An eight-year-old child presented with generalized popular eruptions of two years duration. The diagnosis was lichen nitidus with pathologic confirmation. The lesions were successfully reduced and flattened by pimecrolimus 1 percent cream for 8 weeks.
Introduction
Lichen nitidus (LN) is an uncommon, usually asymptomatic, chronic eruption characterized by the presence of multiple, tiny, discrete, shiny, flesh colored flat papules 2-3 mm in diameter that are predominantly observed on the chest, abdomen, glans penis, and upper extremities [1, 2, 3]. The etiology of LN is unknown and no laboratory abnormalities or associations with systemic disease have been established [4]. Multiple clinical variants of LN have been described, including keratodermic, vesicular, hemorrhagic, purpuric, perforating, palmoplantar and generalized forms [1-3, 5, 6]. The disorder is most often localized and only a few cases of generalized LN have been reported [2, 5-8]. We report a case of generalized LN that improved but did not completely clear with application of pimecrolimus 1 percent cream for eight weeks.
Case report
 |
| Figure 3 |
|---|
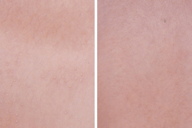
| Figure 3. The lesions on the trunk of the child before (A) and after (B) treatment with pimecrolimus 1 percent cream for 2 months. |
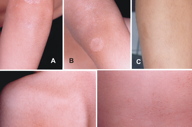
An eight-year-old child presented to the hospital for evaluation of a non-pruritic, generalized cutaneous eruption that had been present for two years. Physical examination revealed multiple flesh-colored and tan-brown papules, from 1 to 2 mm in diameter, on the child's torso, extremities, body, and face, as seen in Figure 1. There was no evidence of mucocutaneous or palmoplantar involvement. The child did not have any associated systemic complaints. The patient's medical history was unremarkable and he had not been taking any other medication over the previous 2 years. The laboratory tests also were normal. A skin biopsy was performed. The diagnosis was LN, which was confirmed by pathology.
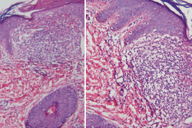
Sections of the skin biopsy showed slight hyperkeratosis, acanthosis, and foci with vacuolization of the basal layer; the epidermis was relatively thinned over the infiltrate. Rete ridges adjacent to dermal infiltrate were elongated and infolding. Discrete focus of inflammatory cells consisted of histiocytes, lymphocytes, and occasionally multinucleated giant cells that filled the papillary dermis. There was perifollicular fibrosis admixed with some lymphocytic infiltration in the mid dermis (Figure 2).
The lesions were improved with application of pimecrolimus 1 percent cream twice daily for 8 weeks. Figure 3 shows lesions on the body of the child before (Figure 3A) and after (Figure 3B) treatment with pimecrolimus 1 percent cream for 8 weeks. Any side effect of the drug was not seen in our patient.
Discussion
Lichen nitidus is a chronic popular eruption of the skin that most commonly affects children and young adults [2], but has been reported in the elderly. Generalized LN is a rare subtype of LN characterized by multiple, skin-colored, shiny, dome-shaped papules occurring over the entire body [9]. The differential diagnosis of LN includes keratosis pilaris, lichen planus, follicular eczema, verruca plana, pityriasis rubra pilaris, phrynoderma (vitamin A deficiency), lichen simplex chronicus, prurigo nodularis, psoriasis [4], and papular mucinosis [3]. Histopathological evaluation is helpful to confirm the diagnosis. Because LN is usually asymptomatic and resolves without any sequelae, no treatment is required in most cases. Although, LN tends to be asymptomatic and usually resolves spontaneously in a year, the clinical course of generalized LN is unpredictable and there is no effective or tolerable treatment for generalized LN in children [2, 8, 10]. Persistent lesions and those that are refractory to various treatments can pose therapeutic challenges [10]. Systemic and topical corticosteroids [10], dinitrochlorobenzene (DNCB), diphenylcyclopropenone immunotherapy, astemizole, itraconazole, isoniazid, enoxaparin, and psoralen and ultraviolet A (PUVA) phototherapy have all been tried [2, 11]. Sun exposure and narrow band UVB (NBUVB) therapy have been reported to be helpful in treating LN [8, 9, 12]. Successful treatment of LN with tacrolimus 0.1 percent ointment has been reported in one case in 2004 [13]. The topical calcineurin inhibitors tacrolimus and pimecrolimus have an effect on various cells of the cutaneous immune system, specifically on T cells, by inhibiting the phosphatase calcineurin and preventing the transcription of proinflammatory cytokines [14].
Although the exact mechanism of pimecrolimus in the treatment of LN is unknown, anti-inflammatory and immunumodulatory effects have been suggested. Our patient responded to a short course of topical pimecrolimus cream but more controlled studies are needed.
Acknowledgement: The authors indebted to thank Dr. Zahra Safaie-Naraghi for her help in preparing of the pathologic pictures.
References
1. Vijaya B, Manjunath GV. Perforating lichen nitidus. Indian J Pathol Microbiol. 2010 Jan-Mar;53(1):162-3. [PubMed]2. Mehta V, Balachandran C. Generalized lichen nitidus in childhood. Indian J Dermatol. 2008;53(4):221-2. [PubMed]
3. Park SH, Kim SW, Noh TW, Hong KC, Kang YS, Lee UH, et al. A case of palmar lichen nitidus presenting as a clinical feature of pompholyx. Ann Dermatol. 2010 May;22(2):235-7. [PubMed]
4. Pielop JA, Hsu S. Tiny. skin-colored papules on the arms and hands. Am Fam Physician. 2005 Jan 15;71(2):343-4. [PubMed]
5. Soroush V, Gurevitch AW, Peng SK. Generalized lichen nitidus: case report and literature review. Cutis. 1999 Aug;64(2):135-6. [PubMed]
6. Rallis E, Verros C, Moussatou V, Sambaziotis D, Papadakis P. Generalized purpuric lichen nitidus. Report of a case and review of the literature. Dermatol Online J. 2007;13(2):5. [PubMed]
7. Al-Mutairi N, Hassanein A, Nour-Eldin O, Arun J. Generalized lichen nitidus. Pediatr Dermatol. 2005 Mar-Apr;22(2):158-60. [PubMed]
8. Do MO, Kim MJ, Kim SH, Myung KB, Choi YW. Generalized lichen nitidus successfully treated with narrow-band UVB phototherapy: two cases report. J Korean Med Sci. 2007 Feb;22(1):163-6. [PubMed]
9. Park JH, Choi YL, Kim WS, Lee DY, Yang JM, Lee ES, et al. Treatment of generalized lichen nitidus with narrowband ultraviolet B. J Am Acad Dermatol. 2006 Mar;54(3):545-6. [PubMed]
10. Chen W, Schramm M, Zouboulis CC. Generalized lichen nitidus. J Am Acad Dermatol. 1997 Apr;36(4):630-1. [PubMed]
11. Cholongitas E, Kokolakis G, Giannikaki E, Ioannidou D. Persistent generalized lichen nitidus successfully treated with enoxaparin sodium. Am J Clin Dermatol. 2008;9(5):349-50. [PubMed]
12. Kim YC, Shim SD. Two cases of generalized lichen nitidus treated successfully with narrow-band UV-B phototherapy. Int J Dermatol. 2006 May;45(5):615-7. [PubMed]
13. Dobbs CR, Murphy SJ. Lichen nitidus treated with topical tacrolimus. J Drugs Dermatol. 2004 Nov-Dec;3(6):683-4. [PubMed]
14. Breuer K, Werfel T, Kapp A. Safety and efficacy of topical calcineurin inhibitors in the treatment of childhood atopic dermatitis. Am J Clin Dermatol. 2005;6(2):65-77. [PubMed]
© 2011 Dermatology Online Journal