Mastocytosis with urticaria pigmentosa and osteoporosis
Published Web Location
https://doi.org/10.5070/D360f3r72dMain Content
Mastocytosis with urticaria pigmentosa and osteoporosis
Jennifer A Stein MD PhD, Hideko Kamino MD, Ruth F Walters MD, Miriam K Pomeranz MD
Dermatology Online Journal 14 (10): 2
Department of Dermatology, New York UniversityAbstract
A 76-year-old man with a 52-year history of urticaria pigmentosa was found to have an elevated serum tryptase level as well as osteoporosis. Histopathologic alterations of one his skin lesions showed an infiltrate of mast cells. Urticaria pigmentosa patients are at risk for osteoporosis because of elevated heparin and stem-cell factor levels. These patients should be screened with serum tryptase levels and bone density studies to detect osteoporosis, regardless of their age.
History
A 76-year-old physician with a 52-year history of asymptomatic, erythematous-to-brown macules and papules on the trunk, neck, buttocks, and extremities had sought no medical care for his condition until his daughter brought it to his attention. The patient's mother first noted the lesions when he was 24 years old. His lesions intermittently flare, and new lesions continue to develop. He had a syncopal episode in 2001, the etiology of which was never pursued. Upon his daughter's insistence at age 74, he had his serum tryptase measured and had a bone density scan performed one year later. His only medical problems are seasonal allergies and a history of an inguinal hernia repair. His medications at the time of diagnosis were aspirin 81 mg every other day and three unknown pills taken as part of the Harvard Physician Health Study. He is an internist and has been a runner for over 30 years. He has run marathons and is still an active runner. Review of systems was non-contributory. A biopsy was performed which confirmed the diagnosis. The patient is now treated with alendronate 70 mg weekly, calcium 1500 mg daily, and vitamin D 400 IU daily.
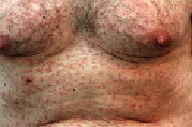 | 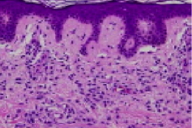 |
| Figure 1 | Figure 2 |
|---|
Physical Examination
Scattered, two-to-five mm, erythematous, edematous papules and orange-brown macules were present on the neck, chest, abdomen, back, extremities, and buttocks. The face, palms, soles, and genitals were spared.
Lab
A complete blood count, basic metabolic profile, and hepatic and lipid panels were normal. Serum tryptase was 193 ng/mL (normal are 2-10 ng/mL). A bone density study showed osteoporosis of the lumbar spine and osteopenia of the hip and forearm bones.
Histopathology
In the papillary and superficial reticular dermis, there is a perivascular and interstitial infiltrate of mast cells with oval nuclei and abundant cytoplasm with basophilic granules. The overlying epidermis shows mild basal layer hyperpigmentation. Giemsa and chloracetate esterase (Leder) stains highlight the mast cell infiltrate.
Comment
Urticaria pigmentosa (UP) is a form of mastocytosis characterized by diffusely scattered, yellow, erythematous-to-brown macules and papules. Patients may have extracutaneous mast-cell involvement in the bone marrow, gastrointestinal tract, liver, spleen, or lymph nodes, or may have disease limited to the skin [1, 2]. Within the spectrum between skin-limited UP and systemic disease, there may be patients with systemic effects of mast cell mediators unrelated to the presence of extracutaneous mast cells. These mediators include heparin and stem-cell factor, which have been proposed to induce osteoporosis [3, 4].
Mast cells produce mediators pre-formed in granules, such as histamine, serine proteases (e.g., tryptase), acid hydrolases, and proteoglycans (e.g., heparin). They also release newly-generated membrane-derived mediators such as glandin prosta and leukotrienes as well as multiple cytokines including IL-6 and stem-cell factor [5].
Mast cell mediators can induce acute symptoms such as pruritus, whealing, flushing, palpitations, tachycardia, headache, diarrhea, dizziness, and syncope. These attacks are more common in patients with systemic mastocytosis than they are in patients with skin-limited UP, but they may be in observed in both groups. Severity of symptoms cannot be predicted by total number of mast cells [2].
Serum tryptase can be a surrogate marker for disease extent. Baseline tryptase levels greater than 20 ng/mL suggests systemic mastocytosis. Normal patients or those with only cutaneous mastocytosis usually have levels below 14 ng/mL [2].
Long-term exposure to heparin and stem-cell factor are believed to put patients at increased risk for osteoporosis. Heparin is thought to mediate osteoporosis by upregulating osteoclast activity [3]. Additionally, patents with mastocytosis often have an activating mutation in the tyrosine kinase growth factor receptor, KIT. Osteoclasts express KIT on their surface and are upregulated by stem cell factor, the KIT ligand and a mast cell mediator [6].
Patients with UP should have a serum tryptase level measured as well as a bone density study to detect osteoporosis. If osteoporosis is found, patients can be managed with calcium, vitamin D, and bisphosphonates. Estrogen replacement in post-menopausal women and testosterone in men with low testosterone levels may be considered [2].
There is no cure for urticaria pigmentosa. Patients with systemic flares are advised to avoid potential mast cell stimuli such as nonsteroidal anti-inflammatory agents, narcotics, and systemic anesthetics. Topical glucocorticoids can provide localized symptomatic relief. Systemic therapy such as antihistamines, cromolyn sodium, systemic glucocorticoids, and PUVA photochemotherapy can be useful in patients with more widespread disease [7]. More aggressive cases have been managed with interferon alpha 2b [8] and cladribine, a chemotherapeutic agent [2]. Cosmetic improvement of UP lesions has been demonstrated with the ND:Yag laser at 532 nm [9].
Imatinib is a small molecule protein kinase inhibitor which acts on KIT. Preliminary studies have not shown a benefit in mastocytosis; however, targeted molecules may represent potential therapeutic agents in the future [10].
References
1. Brockow K, Metcalfe DD. Mastocytosis. Curr Opin Allergy Clin Immunol 2001; 1: 449 PubMed2. Brockow K. Urticara pigmentosa. Immunol Allergy Clin N Am 2004; 24: 287 PubMed
3. Fuller K, et al. Heparin augments osteoclast resorption - stimulating activity in serum. J Cell Physiol 1991; 147: 208 PubMed
4. Brumsen C, et al. A potential role for the mast cell in the pathogenesis of idiopathic osteoporosis in men. Bone 2002; 31: 556 PubMed
5. Church MK, Levy-Schaffer F. The human mast cell. J Allergy Clin Immunol 1997; 99: 155. PubMed
6. Chiappetta N, Gruber B. The role of mast cells in osteoporosis. Semin Arthritis Rheum 2006; 36:32 PubMed
7. Tharp MD. Mastocytosis. In: Bolognia J, et al, eds. Dermatology. London: Mosby; 2003: 1455
8. Casassus P, et al. Treatment of adult systemic mastocytosis with interferon alpha: results of a multicentre phase II trial on 20 patients. Br J Haematol 2002; 119: 1090 PubMed
9. Resh B, et al. The cosmetic treatment of urticaria pigmentosa with Nd:YAG laser at 532 nanometers. J Cosmet Dermatol 2005; 4: 78 PubMed
10. Levitski A. Tyrosine kinases as targets for cancer therapy. Eur J Cancer 2002; 38: S11
© 2008 Dermatology Online Journal

