An adult case of severe hand-foot-mouth disease accompanying persistent fever and systemic arthritis
Published Web Location
https://doi.org/10.5070/D35pt6g8x8Main Content
Letter: An adult case of severe hand-foot-mouth disease accompanying persistent fever and systemic arthritis
Masami Toya, Yuichiro Endo, Hideaki Tanizaki, Akihiro Fujisawa, Miki Tanioka, Yoshiki Miyachi
Dermatology Online Journal 18 (8): 14
Department of Dermatology, Kyoto University, Sakyo, Kyoto, JapanAbstract
This paper reports a case of adult HFMD with vesicles scattered on the whole body and severe oral lesions. In addition, a long-lasting elevated level of C-reactive protein (CRP) was a feature of this case. Our case is unusual for HFMD with long-lasting joint pain and high fever.
Introduction
Hand-foot-mouth disease (HFMD) is an acute viral infection that occurs usually among children in summer. HFMD is named after clinical manifestations of oval vesicles on the hands and feet and painful oral mucosa ulcerations. Symptoms usually resolve spontaneously in several days. Herein, we present an immunocompetent adult case of HFMD showing subsequent persistent fever and arthritis.
Case report
 |  |
| Figure 1 | Figure 2 |
|---|---|
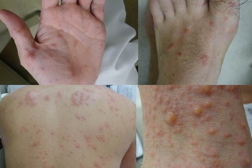
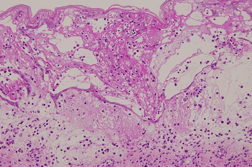
| Figure 1. Round vesicles on the hands and feet and numerous vesicles with erythema on the trunk Figure 2. An intraepidermal bulla containing degenerated keratinocytes | |
A 35-year-old male was referred to our department because of expanding rash, fever, joint pain, and general malaise. One day before the consultation, he noticed round vesicles on the hands and feet. HFMD was diagnosed by a pediatrician. Physical examination revealed numerous vesicles with erythema on the trunk, extremities, and oral mucosa (Figure 1). The grouped vesicles mimicked herpes zoster infection. Oral lesions were too severe and painful for him to eat. The patient complained of joint pain of the wrists and fingers. The body temperature was 39 degrees Celsius. C-reactive protein was 21.1 mg/L. Rheumatoid factor and anti-cyclic citrullinated peptide antibody were within normal levels.
Histopathological examination of a vesicle on the arm showed an intraepidermal bulla including degenerated keratinocytes (Figure 2). No multinuclear cells or inclusion bodies were found. Direct immunofluorescent examination of a vesicle on the arm was negative.
Antibodies against desmoglein 1 or 3, herpes simplex, and HIV were all negative. Antibodies against varicella virus showed a pattern suggesting previous infection and IgG antibodies were not elevated. However, the neutralization test for coxsackie virus type 16 using paired serum samples showed a sixty-four times increase in serum titer; serology was negative for enterovirus type 71. Cerebrospinal fluid examination and a CT scan did not suggest viral meningitis or encephalitis.
Considering these results, the skin lesions were diagnosed as severe HFMD. They resolved without complications in 14 days, although a high fever lasted for 22 days and joint pain and elevated CRP for 60 days. After that, the patient recovered uneventfully.
Conclusion
In adult cases of HFMD, more severe skin symptoms than is seen in children are common. However, admission is usually not necessary [1]. In the present case, vesicles scattered on the whole body and severe oral lesions lead us to suspect first varicella or autoimmune bullous diseases. To the best of our knowledge, no cases of HFMD with such long-lasting joint pain and high fever have been reported.
In 2011, an outbreak of HFMD occurred in Japan for the first time in the past 10 years. The characteristic features of HFMD in 2011 in Japan were adult cases with severe systemic symptoms, larger skin eruptions, and wider distributions on the face and buttocks besides the hands and feet. In 2011, we also experienced immunocompetent adult cases of HFMD with severe oral lesions [2]. One possible explanation for severe clinical symptoms may be a gene alternation of coxsackie virus type 16. In the previous outbreak in Singapore in 2008, mutations of coxsackie A strains and enterovirus type 71 were suspected for the cause [3]. Moreover, genetic variations of coxsackie virus B5 has been reported to be associated with aseptic meningitis in Greece [4]. Another explanation is that the type of coxsackie virus could be different. The neutralization test for coxsackie virus type 16 has a cross-reactivity with type 6. Actually, coxsackie virus type 6 is reported to induce a more severe and broader spectrum of skin symptoms [5, 6]. Therefore, it may be that the current case was caused by coxsackie virus type 6.
HFMD is usually a self-healing disease. However, sometimes it shows severe manifestations. Dermatologists should be aware of the atypical manifestations of HFMD.
References
1. Shin JU, Oh SH, Lee JH. A Case of Hand-foot-mouth Disease in an Immunocompetent Adult. Ann Dermatol; 22: 216-8. [PubMed]2. Shikuma E, Fujisawa A, Tanioka M et al. Letter: an adult case of hand-foot-mouth disease showing severe mucous involvement. Dermatol Online J; 17: 15. [PubMed]
3. Wu Y, Yeo A, Phoon MC et al. The largest outbreak of hand; foot and mouth disease in Singapore in 2008: the role of enterovirus 71 and coxsackievirus A strains. Int J Infect Dis; 14: e1076-81. [PubMed]
4. Papa A, Dumaidi K, Franzidou F et al. Genetic variation of coxsackie virus B5 strains associated with aseptic meningitis in Greece. Clin Microbiol Infect 2006; 12: 688-91. [PubMed]
5. Wei SH, Huang YP, Liu MC et al. An outbreak of coxsackievirus A6 hand, foot, and mouth disease associated with onychomadesis in Taiwan, 2010. BMC Infect Dis; 11: 346. [PubMed]
6. Lo SH, Huang YC, Huang CG et al. Clinical and epidemiologic features of Coxsackievirus A6 infection in children in northern Taiwan between 2004 and 2009. J Microbiol Immunol Infect; 44: 252-7. [PubMed]
© 2012 Dermatology Online Journal

