Epidermodysplasia verruciformis after cutaneous T-cell lymphoma: Periungual presentation
Published Web Location
https://doi.org/10.5070/D35bt0c996Main Content
Letter: Epidermodysplasia verruciformis after cutaneous T-cell lymphoma: Periungual presentation
Jonathan E Cutlan MD, Rashid M Rashid MD PhD, Carlos Torres-Cabala MD, Stephen K Tyring, Valencia Thomas MD
Dermatology Online Journal 16 (8): 12
University of Texas M.D. Anderson Cancer Center, Department of Pathology and Dermatology. rrashid@mdanderson.orgAbstract
Epidermodysplasia verruciformis (EV) has several clinical presentations and has been reported in various states of immune deregulation. We report the unique presentation of this disease as a pigmented periungual macule in a patient with a previous history of immune deregulation related to cutaneous lymphoma. A literature review did not reveal any previous reports of EV in patients with cutaneous T-cell lymphoma.
Case
 |
| Figure 1 |
|---|
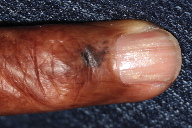
| Figure 1. Periungual pigmented macule |
A 77-year-old woman with a history presented to us with a new 5 mm, atypical black macule that was concerning for dysplastic nevus versus melanoma (Figure 1). Laboratory evaluation including CBC and T-cell counts were unremarkable. She had a history of cutaneous T-cell lymphoma treated with total body skin electron beam radiation, R-CHOP chemotherapy, nitrogen mustard, isotretinoin, and interferon. She was being maintained at the time of presentation with intermittent topical steroids and had been in clinical remission for over 2 years.
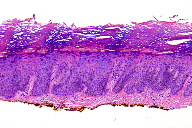
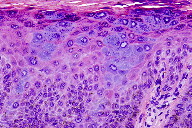
On physical examination, the patient was noted to have an ink black periungual macule. On dermoscopy, a reticular network was noted only on the peripheral margins. Melanoma was suspected and the macule was excised by ellipse. Histologic sections showed a hyperkeratotic and acanthotic epidermis with the characteristic cellular changes of EV. The keratinocytes appear to have swollen cytoplasm that is bluish-gray on hematoxylin and eosin staining. Otherwise, the keratinocytes failed to exhibit nuclear pleomorphism, atypia, or atypical mitotic figures, which excluded squamous cell carcinoma in situ. To rule out a melanocytic process, paraffin embedded tissue was stained with a pan-melanocytic cocktail (tyrosinase and HMB-45), which showed no increase in melanocytes. High and low risk HPV immunohistochemistry studies were negative. However, more specific studies of HPV typing by PCR showed HPV 8.
Discussion
Epidermodysplasia verruciformis has a polymorphic clinical presentation. However, dark black changes are not frequent in the literature. Recently, a case of subungunal Bowens disease with EV that presented as longitudinal melanonychia has been reported [1].
Epidermodysplasia verruciformis can be inherited or acquired. The inherited type is characterized by a genetic defect in the immunity against EV associated human papillomavirus types, primarily HPV 5 and 8. This defect caused by mutations in the EVER1 and EVER2 genes on chromosome 17. The inherited form commonly presents in infancy or early childhood as pink-brown patches and plaques involving the hands, forehead, limbs, neck, and trunk. The acquired form may be secondary to immune dysregulation, such as in HIV infected individuals [2]. Epidermodysplasia verruciformis and EV-like changes have also been reported as acquired conditions in patients with leukemia, transplant patients, and HIV positive patients. Characteristic findings may also be incidental changes without PCR confirmation (named EV acanthoma) [3]. Some authors believe the EV phenotype is histological evidence of a clonal proliferation of mutated keratinocytes susceptible to EV HPV infection, which may represent a direct sign of neoplastic genetic damage to focal keratinocytes [4]. In this patient, exposure to multiple mutagens, such as electron beam radiation, chemotherapy, and topical nitrogen mustard may have played a role in alteration of immune status. These exposures and the patient’s previous state of immune deregulation from the lymphoma, may account for the genetic damage of keratinocytes, enabling EV HPV infection.
Furthermore, patients with inherited EV are predisposed to cutaneous malignancies. It is not yet clear if similar risks exist in the acquired form of EV. However, immune dysregulation plays a well-established role in predisposition to both EV and cutaneous malignancies and physicians must always be particularly vigilant in monitoring these patients. This report also reminds us that the periungual region always warrants careful clinical evaluation [5].
In conclusion, to our knowledge, this is the first reported case of EV presenting as a periungual pigmented macule in a patient with cutaneous T-cell lymphoma; EV should be considered in the differential of pigmented lesions of the nail bed or periungual region.
References
1. Stetsenko GY, Chien AJ, Fleckman P, Swanson P, George E, Argenyi ZB.: Subungunal bowen disease in a patient with epidermodysplasia verruciformis presenting clinically as longitudinal melanonychia. Am J Dermatopathol 2008, 30:582-585. [PubMed]2. Gormley RH: Dermatologic manifestations of HPV in HIV-infected individuals. Curr HIV/AIDS Rep 2009, 3:130-138. [PubMed]
3. Ko CJ, Barr RJ, Binder SW: Changes of epidermodysplasia verruciformis in benign skin lesions: the EV acanthoma. J Cutan Pathol 2007, 34:44-48. [PubMed]
4. Rohwedder A, Tyring SK, Rady P, Carlson JA. : Incidental epidermodysplasia verruciformis human papillomavirus infection (EV acanthoma): evidence for "field cancerization" and a putative cofactor in seborrheic keratosis. J Cutan Pathol 2008, 35:1151-1155. [PubMed]
5. Serratos BD, Rashid RM. Nail disease in pemphigus vulgaris. Dermatol Online J. 2009 Jul 15;15(7):2. [PubMed]
© 2010 Dermatology Online Journal