Eosinophilic fasciitis
Published Web Location
https://doi.org/10.5070/D34z06k5m8Main Content
Eosinophilic fasciitis
Timothy J Cardozo MD PhD
Dermatology Online Journal 9(4): 33
From the Ronald O. Perelman Department of Dermatology, New York University
Abstract
The case of a 76-year-old woman with eosinophilic fasciitis is presented. Reported etiologic associations and treatment options are discussed.
Clinical summary
History.—A 76-year-old woman had stiffening of the arms and legs for 8 months. The patient presented to the Charles C. Harris Skin & Cancer Pavilion in June 2002, with a 4-month history of progressive stiffening of the skin of her arms and legs associated with localized dull pain. Raynaud phenomena, fever, shortness of breath, mucosal and gastrointestinal symptoms, and night sweats were absent. The patient was started on methotrexate (2.5 mg per week and increased to 5 mg per week) in October 2002, with improvement.
Past medical history included syphilis 35 years ago and non-insulin-dependent diabetes.
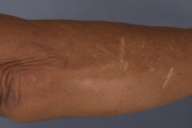
Physical examination.—Symmetric, thick, sclerotic skin with a subtle yellow-orange hue, was present on the forearms, the upper arms, and thighs. A groove sign was visible between the triceps and biceps of the medial upper arm. No prayer sign was evident.
|
|
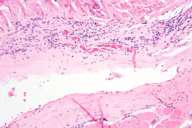
| Figure 1 | Figure 2 |
|---|
Laboratory data.—A complete blood count and comprehensive metabolic profile were normal. Anti-nuclear antibody, anti-Smith antigen, and anti-MP, anti-double stranded DNA, anti-J0-1, and anti-SCL-70 antibodies were negative.
Histopathology.—There is an inflammatory process characterized by foci of sclerosis at the dermosubcutaneous junction, thick subcutaneous septa and fascia, and a perivascular and interstitial infiltrate of lymphocytes and plasma cells. The inflammatory infiltrate extends into the fascia and skeletal muscle. The epidermis shows no pathologic changes.
Diagnosis.—Eosinophilic fasciitis.
Comment
Eosinophilic fasciitis is characterized by the acute or subacute development of induration of the skin and subcutaneous tissues of the forearms, flank, and upper legs. The hands and face are usually spared, and Raynaud phenomenon is usually absent. Autoimmune anemia, eosinophilia and hypergammaglobulinemia are variably present. Considered by some to be a variant of scleroderma or morphea, the predominantly subcutaneous and muscular involvement produces a less smooth and taut appearance to the skin than does scleroderma. The groove sign or vertically linear depressions following the course of vessels occurs between muscle groups.
The original description of eosinophilic fasciitis involved a cohort who experienced the onset of the cutaneous condition with premonitory weakness, swelling, and pain that developed after strenuous physical activity. A similar dermatologic presentation was found as part of the eosinophilia-myalgia syndrome after ingestion of large amounts of contaminated L-tryptophan [1] and in the toxic oil syndrome associated with the ingestion of adulterated rapeseed oil [2]. Recently, eosinophilic fasciitis was associated with the use of simvastatin [3]. Eosinophilic fasciitis has in common with morphea several reports of associated Borrelia burgdorferi infection [4].
The response to immunosuppressive regimens such as systemic glucocorticoids and methotrexate may be excellent with responders achieving a complete recovery within 12-36 months.
References
1. Blauvelt A, et al. Idiopathic and L-tryptophan associated eosinophilic fasciitis. Arch Dermatol 1991;126:1159.2. Alonso-Ruiz A, et al. Toxic oil syndrome: A syndrome with features overlapping those of various forms of scleroderma. Semin Arthritis Rheum 1986;15:200.
3. Choquet-Kastylevsky G, et al. Eosinophilic fasciitis and simvastatin. Arch Intern Med. 2001;161:1456.
4. Granter SR, et al. Borrelia fasciitis. Am J Dermatopatol 1996;18:465.
5. Pouplin S, et al. Treatment of eosinophilic fasciitis with methotrexate. J Rheumatol. 1998;25:606.
© 2003 Dermatology Online Journal

