Teaching Morphology on the World Wide Web: The Experience of "Language of Dermatology"
Published Web Location
https://doi.org/10.5070/D34x18v6rbMain Content
Teaching Morphology on the World Wide Web:
The Experience of "Language of Dermatology"
Gregory J. Raugi, MD, PhD
Sara Kim, MA
Peter B. Odland, MD
Dermatology Online Journal Volume2 Number 1: 3
Introduction
The growth of the World Wide Web (WWW) during the past few years has sparked an immense interest in its capability to store, connect, access, and represent information in hypertext and multimedia modes. This interest has been evident in medicine and medical informatics as manifested by a number of Web-based innovative projects. Some of these examples include on-line biomedical databases (1), a digital health sciences library to aid physicians' clinical decision making (2,3), and Internet-based teaching files that integrate basic and clinical science curricula (4). In dermatology, Web sites with a collection of digitized images of clinical skin diseases can be found at the University of Erlangen, Germany (Project Dermatology On-line Atlas) (5), Mie University, Japan (Anatomy of the Skin) (6), and the University of Iowa (Dermatology Department) (7). Few Web-based curricula are found that are specifically designed for medical education purposes. This is partly due to the novelty of Web technology and partly to the organizational complexity involved in shifting from conventional instructional practice to the untested territory of Internet-based curriculum design and implementation.
This paper describes the preliminary stage of the development and implementation of a Web-based dermatology curriculum, "The Language of Dermatology." The Web site was developed with the following two objectives:
- to provide an alternative instructional method to second year medical students in the HuBio 567 Skin System Course and the Introduction to Clinical Medicine II Course
- to make available an easily accessible review tool for the University of Washington medical students during their clinical clerkships.
Evolution of "Language of Dermatology"
Background
The University of Washington School of Medicine is a public institution with the mandate to train primary care physicians for a five state region (Washington, Alaska, Montana, Idaho, and Wyoming). About 100 students take their first year of basic science instruction at the University of Washington (Seattle); the other 65 take their first year at the University of Alaska (Fairbanks), Washington State University (Pullman), Idaho State University (Moscow), Montana State University (Bozeman), or the University of Wyoming (Laramie). Starting in September of the second year of instruction, students come together for the first time in the organ system curriculum. The Skin System course (HuBio 567) is one component of this curriculum and is offered in the fall concurrently with Introduction to Clinical Medicine (ICM) II. The curriculum consists of 19 hours of lectures and small group discussions regarding basic science topics related to the skin. Because of limited teaching faculty and clinical resources, fewer than 70 of these students will have a dermatology elective during their fourth year. Hence, the Skin System course serves as the only exposure to clinical dermatology for nearly 100 students, many of whom will end up in primary care careers. The course committee, therefore, considered the development of continuously available introductory clinical instructional materials to be of high priority.
Until the introduction of WWW-based teaching, the ICM II component of the skin biology course consisted of: 1) a short, 20-minute, lecture in which the terminology of clinical dermatology was introduced; 2) a faculty-led small group (about 15-20 students per group) in which students practiced examining each other and applying the newly learned clinical terminology; and 3) a live demonstration involving a panel of 15 patients. In this demonstration, students were expected to use the correct technique of skin examination and to select clinical descriptors appropriate to the patient's condition. Discussion and feedback was given in an adjacent room immediately after each patient encounter.
Rationale behind the Development of "Language of Dermatology"
Although the rich clinical materials presented in the lecture were welcomed by the students, four compelling reasons for curriculum reform emerged: 1) the content that could be presented in a 20 minute lecture was limited; 2) the lecture content, which had remained essentially unchanged for thirty years through a succession of lecturers, became stale for the lecturer; 3) students' performance in the follow-up "technique of skin examination" and "patient demonstration" sessions showed a poor assimilation and application of the lecture content in clinical settings; and 4) long-term follow-up of students showed poor retention of the course content. Instruction via the Web-based "Language of Dermatology" modules was designed to substitute for the lecture portion of the curriculum. Our effort to design an alternative instructional mode to enhance and replace the lecture format coincided with a rapid spread of the Web applications in medical education at the University of Washington.
The educational goals that shaped the instructional content of the "Language of Dermatology" included: 1) to provide a common language in which basic skin biology could be taught in the context of an organ systems curriculum; 2) to lay the foundation for interpretation of clinical observations and clinical decision-making; 3) to provide a linguistic framework for communication with other physicians regarding physical findings related to the skin; and 4) to develop the student's skill in interpreting textbooks and journal articles.
Structure of "Language of Dermatology"
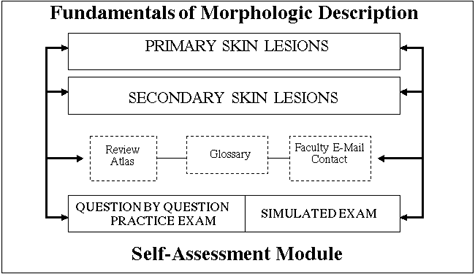
The design of the "Language of Dermatology" structure was carried out by the Integrated Advanced Information Management System (IAIMS) group, a branch of the medical informatics program in the Health Sciences Center at the University of Washington. Figure 1 illustrates the overall structure of the "Language of Dermatology."
|
Figure 1: Overall Structure of the Language of Dermatology. The Language of Dermatology is consisted of two main modules: Fundamentals of Morphologic Description Module that includes a total of 16 primary and secondary skin lesions; Self-Assessment Module that contains a practice exam with question by question feedback and a simulated exam. Students could assess Review Atlas, Glossary, and Faculty E-mail boxes from the two modules. |
Fundamentals of Morphologic Description
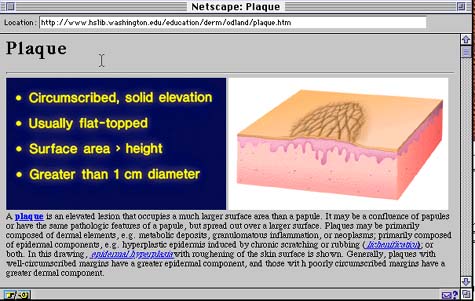
The "Fundamentals" module presented a total of 16 morphologic descriptors for primary and secondary skin lesions. A typical screen layout included the name of the primary or secondary lesion, a bullet summary of the key teaching points related to that term, a line-drawing illustration highlighting the critical features of the particular lesion, and several clinical images illustrating the morphological detail (Figures 2 and 3). Critical descriptors in the text were highlighted and connected via hyperlinks to detailed definitions in the glossary section. Students were free to browse through all 16 primary or secondary lesions in any order.
|
Figure 2: Screen Layout in the Fundamentals Module: Plaque. A typical screen layout included the name of the primary or secondary lesion, a bullet summary of the key teaching points related to that term, and a line-drawing illustration highlighting the critical features of the particular lesion. |
|
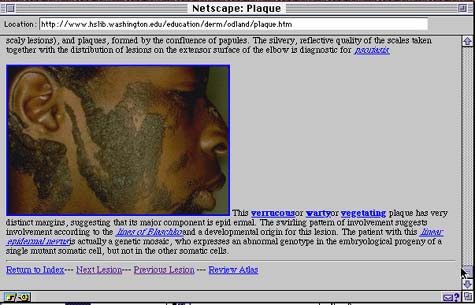
Figure 3: Screen Layout in the Fundamental Module: Plaque. Each skin lesion screen included several clinical images illustrating the morphological detail. Images can be zoomed with a mouse click to facilitate detailed study of the clinical cases. Students have the options of returning to the index of skin lesions, advancing to the next lesion, going back to the previous lesion or choosing Self-Assessment Module by clicking on the hypertext that appears on the bottom of the screen. |
Review Atlas
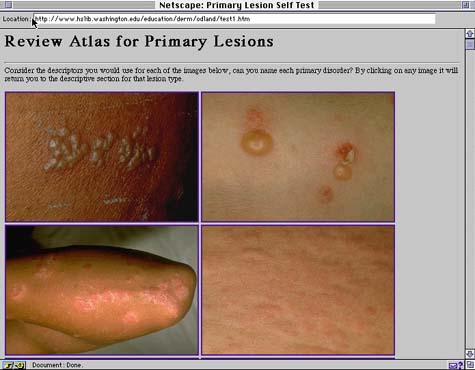
A "Review Atlas" module, accessible from the "Fundamentals" module, included a collection of clinical images (Figure 4). The purpose of the "Review" module was to have students view the clinical images that had already been presented in the "Fundamentals" module and monitor their learning in terms of the number of correct descriptors they recalled. Beyond employing a "think-aloud" strategy, students could click on each image in the "Review" module and automatically link to the screen of the corresponding primary or secondary lesion for further review purposes.
|
Figure 4: Screen Layout in the Review Atlas Module. A "Review Atlas" module, accessible from the "Fundamentals" module, included a collection of clinical images. Students viewed the clinical images that had already been presented in the "Fundamentals" module and monitor their learning in terms of the number of correct descriptors they recalled. Students could click on each image in the "Review" module and automatically link to the screen of the corresponding primary or seconday lesion for further review purposes. |
Self-Assessment Module.
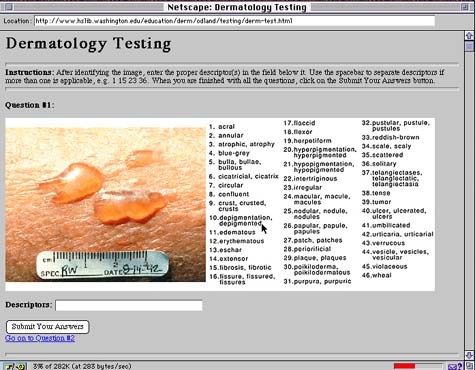
The "Self-Assessment" module was intended to assess a student's ability in a complex task of morphologic description beyond the memorization and application of 16 primary and secondary lesions (See Figure 5). Twelve questions were presented. Each contained an image of a case study accompanied by a list of 46 descriptors all of which had been introduced in the text or images of the "Fundamentals" module and defined in the "Glossary" section. Students were asked to select up to six descriptors that described the most critical morphologic features in each of the 12 case studies. After completing each case study, students submitted their answers and received a numerical score from the Web server.
|
Figure 5: Screen Layout in the Self Assessment Module. Twelve questions were presented in the Self-Assessment Module. Each question contained an image of a case study accompanied by a list of 46 descriptors all of which had been introduced in the text or images of the "Fundamentals" module and defined in the "Glossary" section. Students were asked to select up to six descriptors that described the most critical morphologic features in each of the 12 case studies. |
Implementation of "The Language of Dermatology"
Orientation. The Skin System course included 19 hours of lecture, small group discussions, and patient demonstrations plus a two-hour final examination, all given within the span of 15 calendar days. An orientation on the use of the "Language of Dermatology" was conducted during the first hour of instruction. A portable computer was connected by ethernet link to the UW server and to a projection system. After providing students with a handout detailing the location of hardware resources, the log-on procedure, and the navigation tools, one faculty member (GJR) explained the rationale behind the new instructional format. He then demonstrated all modules in the Web page, the key buttons, commands, and the e-mail links with the course director and a faculty member. Students were encouraged to take a self-assessment test at least once during the 15 day period. Students were told that six of the final examination questions would be comparable to the test format in the "Self-Assessment" module.
Revision of "Language of Dermatology". Within the first three days of the course, several acute problems associated with the "Self-Assessment Module" became apparent and were addressed with programming changes. Students' enthusiastic e-mail reports of problems, suggestions, and complaints alerted the faculty and technical team and the necessary revisions were promptly carried out. Some of these problems and follow-up actions are discussed in this section. First, inadequate image display in terms of their resolution and size emerged as the most hindering factor in student learning. Students complained that the fixed sizes of images in the "Self-Assessment" module limited their ability to detect subtle clinical details. The attachment of the list of 46 descriptors to each clinical image prohibited us from offering the students the option of "zooming" the image. The amount of programming time and manpower required to correct this problem was beyond our resources during the course. However, the second version of the "Language of Dermatology" will provide "zoomable" images in the "Self-Assessment" module to facilitate detailed study of the clinical cases.
Second, the length of time to download the 12 images in the "Self-Assessment" module was too long. Students reported that downloading time took about 40 seconds on library workstations and much longer if students worked via modem connection from their personal computers at home. To address this problem, the "Self-Assessment" module was redesigned so that students had a choice of either studying each problem individually with a marked reduction in the downloading time, or taking the whole test as a simulated examination.
Third, students cited insufficient feedback in the "Self-Assessment" module as another problem. The only feedback to students was their score on the correctly identified descriptors out of the total possible score. Students were dismayed by not knowing what the correct answers were and why their own responses were considered inaccurate. This led them to engage in protracted and frustrating efforts to maximize their score with repeated access to the module. For example, several students reported that they took one exam item at a time, downloaded the score, and repeated the process until they found a set of descriptors that maximized their score. Currently, the development team is designing a new feedback module. It will provide not only numerical scores of student performance but also elaborated feedback tailored to students' answers. In addition, student performance will be tracked throughout the entire "Self-Assessment" module and summarized at the end of the test.
Student Feedback Student feedback on the overall usefulness of the "Language of Dermatology" was indispensable in understanding the learner's perspectives on a Web-based curriculum. Feedback was collected from three sources: e-mail contacts from within the "Language of Dermatology," an on-line feedback form, and a supplemental course evaluation.
The table summarizes student feedback collected via 66 on-line survey forms:
Table :
| Summary of On-Line Student Feedback | ||
|---|---|---|
| 1. Compared to viewing slides in the Library, class, and in a discussion session, how do you compare this computer based learning method? | Better About the Same Worse |
64% 29% 7% |
| 2. How would you rate the visual quality of the images? | Good Acceptable Poor Unacceptable |
64% 29% 6% 1% |
| 3. How much time did you spend working with these materials? | 30 min or less 30 min to 1 hour 1 to 2 hours Over 2 hours |
17% 24% 32% 27% |
| 4. By placing this material on the World Wide Web and accessible from any Internet connection we hope to make it more easily available. Does this seem like a good method to you? | Yes Not ever Not until I have my own computer |
91% 1% 8% |
| 5. How would you improve this instructional material? | More Examples More links Case examples No improvement |
49% 21% 15% 15% |
| 6. Was this learning experience effective in teaching you to accurately describe skin lesions? | Yes Somewhat No |
55% 44% 1% |
| 7. Is this material something you would look at again in preparation for or on a clinical rotation? | Yes No |
86% 14% |
The overall student response to the "Language of Dermatology" as a learning tool was positive. The majority of the students used the Web at least 30 minutes during the 15 day course period. In spite of some difficulties that students experienced with "unzoomable" clinical images, more than 80% of the students rated the visual quality of the teaching materials acceptable and good. Students' interest in re-visiting the Web site during their clinical rotation confirmed that the "Language of Dermatology" could be used as a valuable reference tool for the third and fourth year students.
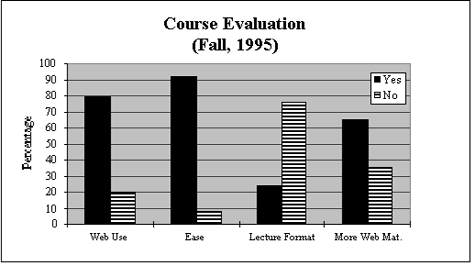
In addition to the on-line feedback form, a supplemental course evaluation was received from 122 students (77% response rate) at the end of the course and is summarized in Figures 6a and 6b.
|
Figure 6a: Supplemental Course Evaluation. The evaluation results showed that the majority of the students used the Web site (79%), found the Web site easy to use (92%), preferred not to have the material presented in lecture format (76%), and would be interested in having more course material on the Web site (65%). |

|
Figure 6b: Supplemental Course Evaluation--Continued. Students' rating of the Web site as a teaching tool is as follows: very poor (3%), poor (4%), fair (12%), good (34%), very good (19%), and excellent (25%). Overall, 78% of the students found the Web site to be of high quality. |
Based on students' feedback, we feel that our objective to provide a common language of basic skin biology within the context of an organ systems curriculum has been met. The survey content will be modified in the future to better assess the targeted learning objectives as well as the effectiveness of newly incorporated technical features. As discussed previously, direct access by students to faculty e-mail boxes from within the instructional material contributed to the rapid identification of problems arising during the use of the "Language of Dermatology." A more transparent e-mail module has been designed for the second version of "The Language of Dermatology" in order to further encourage students to provide informal and immediate notice of problems.
Future Direction: "Language of Dermatology"
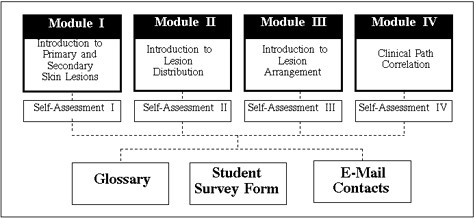
A proposal for the enhancement and revision of "The Language of Dermatology" has already been approved by the School of Medicine. A new version based on student feedback and faculty experience will be available in the fall of 1996. Figure 7 illustrates new modules to be developed and added to the current version.
|
Figure 7: Structure of the Future "Language" Series. Three additional modules will be developed and added to the future "Language" series. In addition to the current Fundamental of Morphologic Description Module, new modules will include Introduction to Lesion Distribution, Introduction to Lesion Arrangement, and Clinical Path Correlation. Each teaching unit will contain separate self-assessment modules. Students will have access to glossary section, on-line survey form, and faculty e-mail boxes from within each unit. |
Future enhancements of the "Language" series will include an expanded list of basic vocabulary and greater opportunities for students to attempt an accurate clinical description. A number of factors will continue to play crucial roles in the future development of the "Language" series and are briefly discussed in this section. The design of an effective on-line self-assessment module is by no means an easy task as experienced by other projects (8,9). Our efforts in assessing a student' ability to employ linguistically sophisticated descriptors in describing a skin condition on the Web also proved to be a challenging task. The initial design of the self-assessment module that asked students to choose from 46 descriptors taught in the "Fundamentals" module had to be revised due to several reasons: a) clinical images attached to the descriptor list could not be zoomed; b) faculty expectations for students to observe and describe beyond the most basic features of a complex skin lesion were unrealistic; and c) the original goal of teaching students to identify 16 primary and secondary lesions was not adequately reflected in the course materials. Based on this experience, the new self assessment module will be broken down into smaller components and will present a more limited spectrum of descriptive terminology for a student to apply in a given situation. In the new version of the "Language" series, the self assessment module will appear as the "Interactive Teaching Module," to reflect the emphasis on interactive technology.
Another future challenge lies in refining the "Language" series as a clinically relevant tool especially in light of students' interest in using the "Language of Dermatology" during their clinical rotations. In the past, faculty found that students retained little morphologic knowledge and showed insufficient skills in applying and articulating their knowledge in clinical settings. A follow-up study on the current second year students who used the "Language of Dermatology" may yield insightful information on how the Web-based instruction improved the retention of knowledge and their clinical performance throughout the remainder of their medical school experience. While there is no clear consensus on the essential components of an effective educational intervention in dermatology,(10,11) a Web-based approach to teaching morphology presents exciting educational opportunities in furthering our understanding of student learning and effective pedagogy of dermatology.
In conclusion, a number of critical ingredients in the successful design and implementation of the "Language of Dermatology" are noted: faculty initiatives; organizational support; a close collaboration with the Integrated Advanced Information Management System group on campus; student feedback collected via e-mail and on-line survey forms; and prompt revision of the system based on student feedback. New developments in Web technology offer a number of alternatives for presenting and integrating learning materials on-line. The challenge lies in how to transform, and not merely transfer, instructional content into a format that optimizes various interactive features of the Web including the manipulation of image sizes, instantaneous feedback, and nonlinear presentation of content. Our efforts in developing innovative dermatology instructional materials will continue as we enrich our experience from other similar initiatives and in turn, serve as a model example for newly emerging endeavors on the Internet.
References
(1) Lowe, HJ, Lomax, EC, Polonkey, SE. The World Wide Web: A Review of an Emerging Internet-based Technology for the Distribution of Biomedical Information. JAMIA 1996;3(1): 1-14.
(2) Galvin, JR, D'Alessandro, MP, Erkonen, WE, Smith, WL, El-Khoury, GY, Weinstein, JN. The Virtual Hospital: Providing Multimedia Decision Support Tools via the Internet. SPINE 1995;20(15): 1735-1738. (http://vh.radiology.uiowa.edu)
(3) Schnell, EH. The anatomy of a World Wide Web library service: the BONES demonstration project. Bull Med Libr Assoc 1995;83(4): 440-445.
(4) Wallis, JW, Miller, MM, Miller, TR, Vreeland, TH. An Internet-based Nuclear Medicine Teaching File. The Journal of Nuclear Medicine 1995;36(8): 1520-1527.
(5) Erlangen Atlas
(6) Mie Deparmtnet of Dermatology
(7) Dermatology, University of Iowa
(8) McEnery, KW, Roth, SM, Kelly, LK, Hirsch, KR, Mention, DN, Kelly, EA. A method for interactive medical instruction utilizing the World Wide Web. Proceedings of the Symposium on Computer Applications in Medical Care, October 28-November 1, 1995.
(9) Williams, TW, Giuse, NB, Huber, JT, Janco, RL. Cross-platform Hypermedia Examinations on the Web. Proceedings of the Symposium on Computer Applications in Medical Care, October 28-November 1, 1995.
(10) Ashton, RE. Teaching non-dermatologists to examine the skin: a review of the literature and some recommendations. British Journal of Dermatology 1995;132:221-225.
(11) Ashton, RE. Teaching non-dermatologists to examine the skin: a review of the literature and some recommendations. British Journal of Dermatology 1995;132: 221-225.
(11) Norman, JR, Rosenthal, D The Development of Expertise in Dermatology. Arch Dermatology 1989;125:1063-1068.
* http://www.hslib.washington.edu/education/derm/odland/
Acknowledgments: This research was supported in part by the Seattle Institute for Biomedical and Clinical Research and the Research Service of the VA Puget Sound Health Care System. The authors would like to acknowledge Dr. Jim Barrett, Director of the Integrated Advanced Information Management System, School of Medicine, for his technical support; and Dr. Douglas C. Schaad, lecturer, Department of Medical Education, School of Medicine, for his critical reading of this manuscript.
Correspondence to: Dr. Gregory J. Raugi at skin@u.washington.edu or Medical Service 111D VA Puget Sound Health Care System 1660 Columbian Way South Seattle WA 98108 phone: 206-764-2305; fax: 206-764-2689 Sara Kim at sarakim@u.washington.edu or Center for Medical Education Research School of Medicine, Box 355305 University of Washington phone: 206-543-4427 Dr. Peter Odland at odland@u.washington.edu Division of Dermatology School of Medicine University of Washington Seattle WA 98195 phone: 206-548-2112

