Successful treatment of superficial pyoderma gangrenosum associated with hidradenitis suppurativa with adalimumab
Published Web Location
https://doi.org/10.5070/D34ph5r1m2Main Content
Letter: Successful treatment of superficial pyoderma gangrenosum associated with hidradenitis suppurativa with adalimumab
CL Reddick, MN Singh, RJG Chalmers
Dermatology Online Journal 16 (8): 15
The Dermatology Centre, University of Manchester, Salford Royal Foundation Hospital, Manchester, UKAbstract
Pyoderma gangrenosum (PG) and hidradenitis suppurativa (HS) are chronic inflammatory dermatoses that can be a challenge to treat. A role for TNF-alpha in their pathogenesis has been postulated in the literature. A therapeutic benefit of infliximab has been reported in recalcitrant cases of both conditions. To date, there is less evidence about the use of adalimumab for these conditions. We report a patient with severe superficial PG on a background of HS, which responded to adalumimab therapy after failure of infliximab therapy.
Introduction
Pyoderma gangrenosum (PG) and hidradenitis suppurativa (HS) are both chronic inflammatory dermatoses. Infliximab has been shown to be of therapeutic benefit in recalcitrant cases of both conditions and a role for TNF-alpha in their pathogenesis has thus been proposed [1, 2, 3, 4]. To date, there is less evidence for the use of adalimumab for these conditions. We report a patient with severe superficial PG on a background of HS, which responded to adalumimab therapy after failure of infliximab therapy.
Case presentation
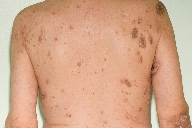 | 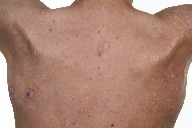 |
| Figure 1a | Figure 1b |
|---|---|
| Figure 1a. Vegetating plaques of superficial pyoderma gangrenosum Figure 1b. After eleven months of adalumimab, 40mg given subcutaneously, fortnightly. | |
A 54-year-old man presented to our service with an eighteen month history of painful, ulcerating and vegetating plaques on his trunk and limbs consistent clinically with a diagnosis of superficial PG (Figure 1a). He complained of boils in the axillae, groin, and buttocks since his teenage years resulting in quite marked scarring consistent with HS (Figure 2). Investigations for alternative causes of pyoderma gangrenosum included full blood count, liver function tests, immunoglobulins, autoantibodies, and chest x-ray, all of which were within normal limits. Culture of a skin swab yielded no significant growth of organisms. Endoscopic investigation for inflammatory bowel disease was negative. A skin biopsy was consistent with the clinical diagnosis and revealed a dense acute and chronic dermal inflammatory infiltrate with scattered small giant cell granulomata and areas of ulceration and abscess formation (Figure 3). Ziehl-Neelsen and PAS stains were negative.
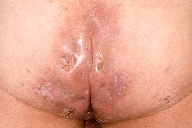 | 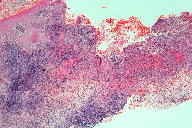 |
| Figure 2 | Figure 3 |
|---|---|
| Figure 2. Chronic scarring from hidradenitis suppurativa of the buttocks Figure 3. Skin biopsy (H+E) with a dense acute and chronic inflammatory infiltrate and small granulomata (x10) | |
Prior treatment included high dose oral corticosteroids, prednisolone (40 mg daily) and dapsone (100 mg daily), with the later addition of cyclosporine (2.5 - 4 mg/kg). Reduction in dose of these produced flares of his condition. Significant improvement was seen following acceptance into an open pilot study of infliximab (two infusions at 5 mg/kg) for PG. However, further funding was not available for continuation of treatment. A poor response to pulsed intravenous methylprednisolone followed by thalidomide (100 mg/200 mg) necessitated reintroduction of oral prednisolone. This was continued at 10 mg daily in conjunction with cyclosporine (2.5 mg/kg) and minocycline (100 mg bd).
The latter regimen was moderately effective for eighteen months until minocycline was discontinued because of marked skin dyspigmentation. The dose of cyclosporine was tapered gradually and withdrawn. Within three months his PG flared severely; extensive new vegetating plaques developed resulting in a major impact on his quality of life (Dermatology Life Quality Index [DLQI] score 20/30) [5]. A further trial of infliximab resulted in significant infusion reactions after two doses. Funding on compassionate grounds was successfully obtained for adalimumab (80mg week 1, 40 mg week 2, 40 mg fortnightly thereafter). Significant improvement was noted at three weeks and his skin was clear of active inflammation by twelve weeks; a dramatic improvement in DLQI score (4/30) was achieved. He remains on fortnightly injections of adalimumab with no adverse effects detected. The PG has remained quiescent on this therapy for eleven months (Figure 1b), although he has had a mild flare of his HS. Minocycline has been reinstituted with good effect.
Discussion
Superficial PG is an uncommon variant of classical PG that shows superficially ulcerated and vegetative plaques [8]. There is a characteristic, although not pathognomic, appearance of focal neutrophilic abcesses in the papillary dermis with peripheral palisaded histiocytes and giant cells. This variant is said to be relatively benign and more responsive to treatment than classical PG, but evidence for this assertion is not completely convincing [8], as illustrated by our patient.
The coexistence of PG and HS has been reported [8, 9] but the frequency of association with the superficial subtype is unknown. There is a significant body of literature to support the use of infliximab in resistant cases of both conditions [1, 2, 3, 4]. Response for treatment periods up to twelve months has been reported with PG and up to six months with HS. This suggests a common pathogenetic factor with a significant role for the cytokine TNF-alpha in the development of these diseases. However clinical benefit has been limited by funding problems, infusion reactions or loss of efficacy. As a consequence, alternative biological agents have been used. In HS, a good response to adalimumab response (40 mg fortnightly) has been noted within one month and maintained up to a mean period of 21 months [9]. We are aware of six reports of benefit from adalimumab in patients with PG [6, 7, 12, 13, 14]. In four patients infliximab therapy had not sustained disease remission prior to initiating adalimumab. Three patients had co-existent inflammatory bowel disease. Significant improvement occurred within 8 to 12 weeks of commencing adalimumab (loading dose 80 mg, thereafter 40 - 80 mg/fortnightly). Therapy duration at time of publication ranged from four to six months. There were no adverse effects described in these reports or in our case. Our experience accords with published case reports and supports the consideration of adalimumab as an alternative to infliximab in the management of recalcitrant pyoderma gangrenosum. Our case also demonstrates that benefit from continued therapy may be maintained for longer than has been reported in previous cases. Further reports will help to establish the true value of adalimumab for this unpleasant disease.
References
1. Moschella SL. Is there a role for infliximab in the current therapy of hidradenitis suppurativa? A report of three treated cases. Int J Dermatol. 2007 Dec;46(12):1287-91 [PubMed]2. Poulin Y. Successful treatment of hidradenitis suppurativa with infliximab in a patient who failed to respond to etanercept. J Cutan Med Surg. 2009 Jul-Aug;13(4):221-5. [PubMed]
3. Akhras V, Sarkany R, Walsh S, Hyde N, Marsden RA. Superficial granulomatous pyoderma treated preoperatively with infliximab. Clin Exp Dermatol. 2009;34(5):183-5 [PubMed]
4. Brooklyn TN, Dunnill MG, Shetty A, Bowden JJ, Williams JD, Griffiths CE, Forbes A, Greenwood R, Probert CS. Infliximab for the treatment of pyoderma gangrenosum: a randomised, double blind, placebo controlled trial. Gut. 2006;55(4):505-9 [PubMed]
5. Finlay AY, Khan GK. Dermatology Life Quality Index (DLQI): A simple practical measure for routine clinical use. Clinical and Experimental Dermatology 1994; 19: 210-216 [PubMed]
6. Fonder MA, Cummins DL, Ehst BD, Anhalt GJ, Meyerle JH. Adalimumab therapy for recalcitrant pyoderma gangrenosum. J Burns Wounds. 2006;5:66-71 [PubMed]
7. Heffernan MP, Anadkat MJ, Smith DI. Adalimumab treatment for pyoderma gangrenosum. Arch Dermatol. 2007;143(3):306-308 [PubMed]
8. Wilson-Jones E and Winkelmann RK. Superficial granulomatous pyoderma: A localized vegetative form of pyoderma gangrenosum. J Am Acad Dermatol 1988;18(3):511-21 [PubMed]
9. Blanco R, Martínez-Taboada VM, Villa I, González-Vela MC, Fernández-Llaca H, Agudo M, González-López MA. Long-term successful adalimumab therapy in severe hidradenitis suppurativa. Arch Dermatol. 2009 May;145(5):580-4 [PubMed]
10. Ah-Weng A, Langtry JA, Velangi S, Evans CD, Douglas WS. Pyoderma gangrenosum associated with hidradenitis suppurativa. Clin Exp Dermatol. 2005 30(6):669-71. [PubMed]
11. Shenefelt PD. Pyoderma gangrenosum associated with cystic acne and hidradenitis suppurativa controlled by adding minocycline and sulfasalazine to the treatment regimen. Cutis. 1996;57(5):315-9. [PubMed]
12. Zold E, Nagy A, Devenyi K, Zeher M, Barta Z. Successful use of adalimumab for treating fistulating Crohn's disease with pyoderma gangrenosum: Two birds with one stone. World J Gastroenterol. 2009 14;15(18):2293-5. [PubMed]
13. Alkhouri N, Hupertz V, Mahajan L. Adalimumab treatment for peristomal pyoderma gangrenosum associated with Crohn's disease. Inflamm Bowel Dis. 2009 ;15(6):803-6.
14. Pomerantz RG, Husni ME, Mody E, Qureshi AA. Adalimumab for treatment of pyoderma gangrenosum. Br J Dermatol. 2007;157(6):1274-5. [PubMed]
14. Hubbard VG, Friedmann AC, Goldsmith P. Systemic pyoderma gangrenosum responding to infliximab and adalimumab. Br J Dermatol. 2005 ;152(5):1059-61. [PubMed]
© 2010 Dermatology Online Journal

