Extensive cerebriform nevus sebaceus: An unusual presentation
Published Web Location
https://doi.org/10.5070/D344z5h2hmMain Content
Extensive cerebriform nevus sebaceus: An unusual presentation
Rahul Mahajan1 MD, Sunil Dogra1 MD, Amrinder Jit Kanwar1 MD, Uma Nahar Saikia2 MD, Saurabh Agrawal1 MBBS
Dermatology Online Journal 18 (5): 9
Department of Dermatology, Venereology, and Leprology1 and Histopathology2, Postgraduate Institute of Medical Education and Research, Chandigarh, IndiaAbstract
Nevus sebaceus is an epidermal nevi composed of sebaceous glands, which usually presents as single yellowish plaque over the head and neck. A rare morphological variant, namely cerebriform nevus sebaceus was first reported in 1998. As with other nevi, the occurrence of nevus sebaceous is related to genetic mosaicism and the shape and distribution of the nevus is determined by the stage at which mosaicism has arisen. We report a patient with cerebriform nevus sebaceus having an unusually widespread distribution over the head, face, and trunk, but without any other organ system involvement.
Introduction
Nevi are hamartomatous growths of skin or mucosa which usually present at the time of birth or soon after. Nevus sebaceus (NS) is an epidermal nevus comprised predominantly of sebaceous glands. Clinically, it presents as a single or, less commonly, multiple yellowish colored plaques with overlying alopecia, usually confined to the head and neck region. In cases in which it is associated with other developmental defects, the condition is termed as epidermal nevus syndrome [1]. We report an unusual presentation of NS as multiple patterned cerebriform plaques in a young male.
Case report
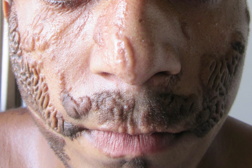 | 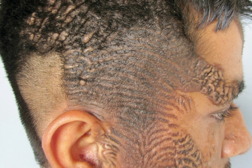 |
| Figure 1a | Figure 1b |
|---|---|
| Figures 1a and 1b. Multiple cerebriform yellowish colored plaques are present over the scalp, forehead, cheeks, chin, and temporo-parietal region. | |
 |
| Figure 2 |
|---|
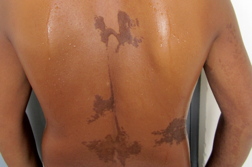
| Figure 2. Velvety yellowish plaques on the trunk along the Blaschko lines. |
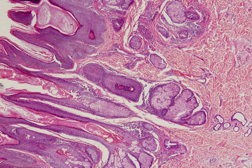
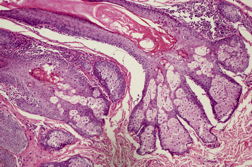
A 17-year-old male presented with abnormal growths on the scalp, face, and trunk, which were present since the time of his birth. The lesions were non-progressive, both in size and extent, except for proportionate increase with body size. There were no associated systemic abnormalities like seizures, impairment of vision or hearing, or skeletal deformities. The disease did not interfere with his daily activities. It had a significant negative impact, however, on his quality of life related to the cosmetic disfigurement. On examination, there were multiple circumscribed yellowish colored plaques present over the scalp, forehead, cheeks, chin, neck, and trunk (Figures 1a and 1b). The plaques on either side of the scalp were symmetrical, covering the parieto-temporal region, and were in continuity with those on the forehead. The surface of plaques was thrown into numerous sulci and gyri, giving them a cerebriform appearance. Similar lesions were also present on the forehead, cheeks, moustache region, and chin. However, the plaques on trunk were more velvety in appearance and followed the Blaschko lines (Figure 2). There was no involvement of oral and genital mucosa. A detailed systemic examination revealed no significant abnormality. Radiographs of the skull, chest, and long bones were normal. A skin biopsy was taken from the plaques on scalp and upper chest. Histopathologic examination from both the sites revealed hyperkeratosis, focal acanthosis, papillomatosis, and follicular plugging in the epidermis. The upper dermis showed underdeveloped hair follicles with mature sebaceus glands surrounding them, consistent with nevus sebaceus (Figures 3 and 4).
Discussion
Nevus sebaceus is seen in about 0.3 percent of all neonates [2]. Classically, it presents at the time of birth as a single bald patch over the scalp. It generally remains unchanged until puberty after which the patch becomes more thickened and protuberant and at times verrucous or nodular, with a smooth velvety surface. The most common sites of involvement are scalp, temples, forehead, periauricular, and centrofacial regions. However, at times, there may be deviation from this classic description. Less commonly, NS may present at multiple sites, at sites other than head and neck [3], or have an atypical morphology. One such rare morphologic variant is cerebriform NS. It was first reported by Ramesh et al in 1998 when they described a 20-year-old man with a large cerebriform plaque over the right parieto-occipital region, which on histopathologic examination was confirmed to be NS [4]. Bomztyk et al described a similar presentation in a 6-month-old child in the postauricular region [5]. Correale et al reported 5 cases of this unusual presentation of NS, describing it as large, papillomatous, and pedunculated NS [6]. All of their patients presented at birth with large exophytic lesions; all but one were confined to the scalp and the face. Only one patient had extensive NS extending from scalp to the elbow. None of the patients showed any associated abnormalities. They concluded that whereas the patients presenting with large cerebriform and papillomatous NS over the scalp should be evaluated for neurologic and ophthalmic abnormalities, they do not usually reveal any underlying abnormality.
What causes an organoid nevus to assume a cerebriform appearance is not known. Similarly the factors that determine the pattern of distribution in nevoid skin diseases is still a matter of debate. The various nevoid patterns include a blaschkoid pattern, a predominant lateralization pattern, and quadrant, patchy, and checkerboard patterns. Lines of Blaschko represent the developmental growth patterns of skin and it is along these lines that linear dermatoses appear. These were described and drawn in 1901 by Alfred Blaschko [7]. These lines represent a form of human mosaicism that may occur related to lyonization (random inactivation of one of the two X chromosomes in all cells in females), post-zygotic somatic mutations during early embryogenesis, or gametic half chromatid mutation occurring before fertilization. It has been suggested that all nevi occur because of genetic mosaicism and the shape of nevi is determined by the stage at which they arise [8]. If the mutation occurs early in embryonic life, they follow the Blaschko lines. However, they tend to be more fixed if mutation occurs later. Recently, Gilmore proposed an attractive hypothesis to explain the patterns in nevoid skin disease [9]. According to him, mosaicism does not imply that any particular cell carrying an abnormal genotype is responsible for dermatosis; conversely, skin disease may occur caused by the effect of a few functionally abnormal clones. He defined two patterns in nevi – anatomical and functional. In the former, abnormal clone of cells are limited to pathologic skin as in NS, whereas the two are spatially unrelated in the latter and hence may not follow Blaschko lines.
The present case was peculiar because of the multiplicity of lesions, their pattern of distribution, as well as their atypical morphology. That the lesions of NS were so extensive and following Blaschko lines would imply that the genetic mutation leading to mosaicism in this patient occurred very early in the embryonic development. The patient was referred to the department of plastic surgery where he underwent serial excision of plaques under general anesthesia with skin grafting; he achieved a significant improvement in general appearance. Hence, cerebriform NS represents a rare morphologic variant of NS, although the factors that govern the morphology of a nevus are not yet known. At the same time, it should be emphasized that the presence of a large and extensive cerebriform NS on the scalp should call for a detailed systemic evaluation to rule out involvement of other organ systems.
References
1. Rogers M. Epidermal nevi and the epidermal nevus syndromes: a review of 233 cases. Pediatr Dermatol 2000;9:342-44. [PubMed]2. Apler J, Holmes LB, Mihm MC Jr. Birthmarks with serious medical significance: naevocellular naevi, sebaceoud naevi amd multiple café-au-lait spots. J Pediatr 1979;95:696-700. [PubMed]
3. Coskey RJ: An unusual organoid naevus. Cutis 1979;24:181-3. [PubMed]
4. Ramesh A, Murugusundaram S, Kumar KV et al. Cerebriform sebaceous nevus. Int J Dermatol 1997; 37:220. [PubMed]
5. Bomsztyk ED, Garzon MC, Ascherman JA. Postauricular cerebriform sebaceous nevus- case report and literature review. Ann Plast Surg 2008;61: 637-39. [PubMed]
6. Correale D, Ringpfeil F, Rogers M. Large, papillomatous, pedunculated nevus sebaceus: a new phenotype. Pediatric Dermatology 2008;25:355-358. [PubMed]
7. Blaschko A: Die Nervenverteilung in der Haut in ihrer Beziehung zu den Erkrankungen der Haut. Beilage zu den Verhandlungen der Deutschen Dermatologischen Gesellschaft VII Congress. Breslau. Wien: Braumuller, 1901.
8. Happle R. What is a naevus: A proposed definition of a common medical term. Dermatology 1995;191:1-5. [PubMed]
9. Gilmore SJ: Patterns in naevoid skin disease: development, disease and modeling: Exp Dermatol 2010; 19:240-45. [PubMed]
© 2012 Dermatology Online Journal