Allergic Contact Dermatitis to Textile Dyes
Published Web Location
https://doi.org/10.5070/D34053p27cMain Content
Allergic Contact Dermatitis to Textile Dyes
Edwin K. Joe, M.D.
Dermatology Online Journal 7(1): 9
Department of Dermatology, New York UniversityPATIENT: A.L., 30-year-old woman
DURATION: Two and one-half years
DISTRIBUTION: Abdomen, lower back, upper and lower extremities, scalp, face
History
The patient has a two and one-half year history of a generalized, diffuse, pruritic, erythematous skin eruption that began suddenly. Prior evaluation elsewhere included six skin biopsies with a diagnosis of psoriasis. Patch tests were negative. Prior treatments have included ultraviolet B phototherapy, topical glucocorticoids, oral antibiotics, and oral antifungal preparations without improvement. He partially responded to oral glucocorticoids, with prompt recurrence of the eruption after discontinuation of the medication. He also has a history of a pustular eruption on both upper and both lower extremities that has been unresponsive to therapy. He denies a family history of psoriasis or atopy.
After patch tests were performed at our institution, he was advised to avoid dye sources (i.e., hair dyes and orange, red and blue clothing), pants with liners, elastic underwear, tight clothing, and neomycin. Loose-fitting clothing made of 100 percent natural-based fabrics (i.e., cotton, linen, silk, and wool) were recommended. It was suggested that all clothing be washed with an extra rinse cycle. Topical therapy includes fluocinolone acetonide ointment, mupirocin ointment, augmented betamethasone dipropionate scalp solution, P & S scalp solution, and T-gel shampoo.
Physical Examination
Multiple, well-demarcated, erythematous plaques with excoriations and a fine scale were present on the abdomen, lower back, buttocks, posterior thighs, calves, and scalp. A linear demarcation was noted superior to the umbilicus. Multiple, excoriated, erythematous papules with scale were also noted on her face and elbows.
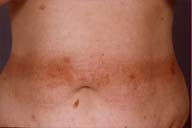 | 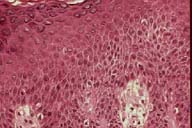 |
| Figure 1 | Figure 2 |
|---|
Laboratory Data
Positive patch test reactions were noted to paraphenylenediamine, neomycin sulfate, thiuram mix, nickel sulfate, cobalt chloride, disperse orange 3, and disperse red 17.
Histopathology
There is psoriasiform epidermal hyperplasia with spongiosis and mounds of parakeratosis. There is a superficial, perivascular infiltrate of lymphocytes and eosinophils with exocytosis. A periodic acid-Schiff stain is negative for fungi.
Diagnosis
Allergic contact dermatitis to textile dyes
Comment
Allergic contact dermatitis to textile dyes is not very common. Although the true incidence is unknown, incidence rates range from 0.05 to 15.9%. [1,2]
Textiles are made from synthetic or natural fibers, or both. Generally, the actual fibers are not allergenic; rather, the dyes used to color the fabrics or formalin finishing resins added to make them wrinkle-resistant, shrink-proof, or easily laundered, are the responsible contactants. Other possible allergens include rubber additives, metals (nickel and chrome), glues, biocides, and fire retardants.
The most common sensitizers belong to the disperse dye application class, which loosely hold onto the fibers and are easily rubbed off.[3,4] Disperse blue 106 and disperse blue 124 have been reported to cause an allergic contact dermatitis to a variety of garments, which include underwear, blouses, pants, swimming suits, pantyhose, shoulder pads, and the velvet material of leggings and body suits.
The distribution of the dermatitis is often widespread, usually corresponding to areas that come into contact with clothing. Often, the dermatitis is worse in areas with increased friction and sweating. In men, this is often the collar area on the neck. In women, this includes the axillary folds, vulva, and suprapubic area. In both sexes, the waistband area, upper thighs, popliteal fossae, and buttocks are commonly involved.
Allergens specific for textile dyes are frequently not included in patch testing. Although studies are limited, disperse blue 106 and 124 may serve as good screening allergens for textile allergy, with positive reactions in approximately 80% and 57 % of dye-related cases in two separate reports. [3,4] These data appear to be comparable, if not superior, to those of paraphenylenediamine as a screening allergen in cases of textile dermatitis.
Management of textile dye dermatitis includes use of topical and systemic glucocorticoids, avoidance of offending dye sources (avoidance of specific colors may not be sufficient), tight synthetic spandex or Lycra clothing, 100 percent polyester linings, and nylon stockings. Instead, patients should wear 100 percent natural-based fabrics (i.e., cotton, linen, silk, wool), 100 percent silk long-sleeved undershirts and slip pants, and loose-fitting clothing, all of which should be washed three times prior to wearing.
References
1. Hatch KL, Maibach HI. Textile dye dermatitis. J Am Acad Dermatol 1995;32(4):631-639. PubMed2. Lazarov A, Trattner A, David M, Ingber A. Symptoms and signs reported during patch testing. Am J Contact Dermat 2000;11(1):26-9. PubMed
3. Pratt M, Taraska V. Disperse blue dyes 106 and 124 are common causes of textile dermatitis and should serve as screening allergens for this condition. Am J Contact Dermat 2000;11(1):30-41. PubMed
4. Hatch KL, Maibach HI. Textile dye allergic contact dermatitis prevalence. Contact Dermatitis 2000;42(4):187-95. PubMed
© 2001 Dermatology OnlLine Journal

