Auricular erythromelalgia: Report of a rare case
Main Content
Auricular erythromelalgia: Report of a rare case
Francesc Messeguer MD, Anna Agusti-Mejias MD, Juan José Vilata Corell MD, Celia Requena MD
Dermatology Online Journal 19 (2): 16
Department of Dermatology, Instituto Valenciano de Oncología, Valencia, SpainAbstract
Erythromelalgia is a rare disorder characterized by 3 major symptoms: warmth, redness, and burning pain. It involves the feet and, to a lesser extent, the hands, head, and ears. We report the case of a 27-year-old man presenting with a 15-year history of episodes with edema, local hyperthermia, and burning pain of both ears.
Case report
A 27-year-old man presented with a 15 year history of relapsing attacks that last from minutes to hours during which the ears become red, associated with edema, local hyperthermia, and burning pain of the two ears. The episodes were more frequent in winter, with 5-7 attacks per week, in contrast to one or no attacks in summer time. He related an improvement of the symptoms in the last years. Each episode presented with bilateral reddening, swelling, and burning of the ears. The symptoms were exacerbated by: touching the ears with the hands or clothes, the contact of the ears with the pillow in the night, high environmental temperature, and exercise.
Clinical exam
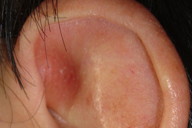 | 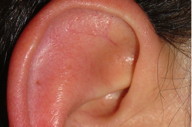 |
| Figure 1a | Figure 1b |
|---|
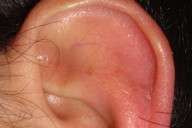 |
| Figure 1c |
|---|
On physical examination, the man was healthy and had no head, ear, nose, or throat abnormalities. He had no history of similar symptoms on feet or hands (Figure 1a). When touching the ears in the medical office to provoke an attack, the ears started reddening and swelling; the patient indicated the typical burning pain he suffered during the previous attacks (Figures 1b and 1c). Unlike the physiological flushing of the auricular regions, whose trigger are changes of environmental temperature and physical exercise, these episodes were also triggered by physical unspecific contact. Moreover, the ears were intensely painful and this pain lasted several hours, unlike the brief fluctuations of the flushing. Laboratory tests including blood cell count, rheumatoid factor, anti-nuclear antibodies, cold agglutinins, and viral serology were normal. The clinical diagnostic was “auricular erythromelalgia.” The patient declined any option of treatment when told that this condition was benign.
Discussion
Erythromelalgia is a rare disorder of uncertain cause. The incidence is 1.3 (0.8-1.7) per 100,000 people per year [1]. Erythromelalgia presents with marked heterogeneity of the affected population and is characterized by 3 major symptoms: warmth, redness, and burning pain, usually in the extremities [1, 2, 3].
The possible involvement of the ears with erythromelalgia has been reported since the early descriptions [3, 4]. Auricular erythromelalgia has almost identical features as the ones described for the Red Ear Syndrome (RES), particularly the idiopathic cases of RES described by Lance [5]. The idiopathic RES consists of relapsing attacks of redness, swelling, and burning sensations in one ear, with precipitation by heat, various movements, touching, and improvement by cooling, that usually is unilateral. Secondary RES is mainly related to neurological deficits [5, 6]. Erythromelalgia may extend to the face or the ears with bilateral involvement or may appear only in the ears [2, 4]. Brill et al consider that RES and auricular erythromelalgia are similar clinical conditions with almost identical diagnostic criteria [6]. A strong argument for continuing to differentiate between these diseases is that RES is limited to the ears and usually unilateral, whereas erythromelalgia involves mainly the feet and hands and more rarely the ears and is generally bilateral. However, some investigators describe a similar condition of the ears and it may therefore have a similar pathogenesis [3, 4, 5, 6].
Diagnosis of erythromelalgia is important because it is a chronic pain syndrome and proper counseling can enable the patient to minimize the severity and frequency of the painful episodes [2, 7]. Treatment options include: acetylsalicylic acid, calcium channel blockers, intravenous lidocaine, prostaglandin analogs, serotonin reuptake inhibitors, venlafaxine, opioids, mexiletine, gabapentin, and beta-adrenergic drugs; even sympathectomy may be considered in erythromelalgia of upper extremities [2, 4, 7]. However, further research is needed to develop more effective treatments.
References
1. Reed KB, Davis MD. Incidence of erythromelalgia: A population-based study in olmsted county, minnesota. J Eur Acad Dermatol Venereol 2009 Jan;23(1):13-5. [PubMed]2. Cook-Norris RH, Tollefson MM, Cruz-Inigo AE, Sandroni P, Davis MD, Davis DM. Pediatric erythromelalgia: A retrospective review of 32 cases evaluated at mayo clinic over a 37-year period. Journal of the American Academy of Dermatology 2012 Mar;66(3):416-23. [PubMed]
3. Davis MD, O'Fallon WM, Rogers RS, 3rd, Rooke TW. Natural history of erythromelalgia: Presentation and outcome in 168 patients. Archives of Dermatology 2000 Mar;136(3):330-6. [PubMed]
4. Vivas AC, Escandon J, Kirsner RS. Refractory erythromelalgia of the ears: Response to mexiletine. American Journal of Otolaryngology 2011 Mar-Apr;32(2):168-70. [PubMed]
5. Lance JW. The red ear syndrome. Neurology 1996 Sep;47(3):617-20. [PubMed]
6. Brill TJ, Funk B, Thaci D, Kaufmann R. Red ear syndrome and auricular erythromelalgia: The same condition? Clinical and Experimental Dermatology 2009 Dec;34(8):626-8. [PubMed]
7. Durosaro O, Davis MD, Hooten WM, Kerkvliet JL. Intervention for erythromelalgia, a chronic pain syndrome: Comprehensive pain rehabilitation center, mayo clinic. Archives of Dermatology 2008 Dec;144(12):1578-83. [PubMed]
© 2013 Dermatology Online Journal


