Systemic amyloidosis with an exceptional cutaneous presentation
Published Web Location
https://doi.org/10.5070/D33vv2r1j7Main Content
Systemic amyloidosis with an exceptional cutaneous presentation
Juan Barja1 MD, Francisca Piñeyro1 MD, Manuel Almagro1 MD, Felipe Sacristán2 MD, Romina Rodríguez-Lojo1 MD, Beatriz Fernández-Jorge1 MD, Sonia Ruanova3 MD, Jesus García-Silva1 MD
Dermatology Online Journal 19 (1): 11
1. Department of Dermatology2. Department of Pathology
3. Department of Internal Medicine
Complejo Hospitalario Universitario de A Coruña, Spain
Abstract
Alopecia and nail distrophy are rare signs of systemic amyloidosis. We present a case with both manifestations and give a brief review of the cutaneous signs of this disease. A biopsy of affected or unaffected skin may provide the diagnosis.
Case report
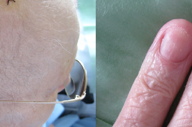
A 73-year-old woman presented with a 1-year history of dyspnea, weakness, dysphagia, dry eye and mouth, and pain in her legs. Physical examination revealed paleness, submandibular swelling, macroglossia, right basal hypophonesis on chest auscultation, and peripheral edema. There was a diffuse alopecia with thin hair and positive hair pull test without infiltration of the scalp (Figure 1A). Eyebrows and eyelashes were affected and axillary and genital hair was absent. Fingernails were thin and brittle, with longitudinal ridging and distal onychoschizia (Figure 1B). These nail changes had started two years before and they were initially attributed to propanolol therapy for hypertension.
Blood analysis showed mild anemia. A chest X-Ray showed right pleural effusion. A computed tomography showed an infiltration in the gastric wall. Protein electrophoresis was normal, but IgG 526, IgA 48, and IgM 16 were low. Immunofixation revealed monoclonal production of the immunoglobulin light chain lambda, which also appeared in a 24-hour urine sample. Electromyography proved sensitive and detected motor axonal polyneuropathy. A gastroscopy showed a thick and micronodular mucous membrane.
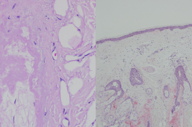
A scalp biopsy showed loss of follicular units related to the infiltration of an amorphous, eosinophilic material which was deposited around the hair follicles and vessels, and in some areas, inside the follicles. The material was stained with Congo red (Figure 2A) and did not vanish with potassium permanganate.
Immunohistochemistry was positive for P-substance and AL (Figure 2B).
A gastric biopsy showed amyloid infiltration of the mucous membrane.
A bone marrow aspiration and biopsy revealed 8 to 14 percent of atypical plasma cells. Serial X-Ray of the bones was normal and a diagnosis of systemic primary amyloidosis, without apparent myeloma, was made. Treatment with melphalan and prednisone was started, but the patient died four months later.
Discussion
Systemic amyloidosis (SA) is caused by extracellular tissue deposition of circulating immunoglobulin monoclonal light chains, which are produced by clonal proliferation of plasma cells [1]. Resulting from the amyloid infiltration of the involved organs, SA has multiple clinical manifestations, which may make it a diagnostic challenge. Clinical skin involvement occurs in 20 to 40 percent of the cases [2] and may be the first and only manifestation of the disease. A biopsy of affected or unaffected skin may provide the diagnosis [3].
Classical cutaneous signs are purpuric lesions and waxy, smooth, shiny, non tender, non pruritic papules, nodules or plaques, often with purpuric appearance, located on flexural areas, eyelids, anogenital region, and mouth [4]. Less common features are infiltrative lesions [4, 5], blisters [5], chronic paronychia [2], and Sjögren-like syndrome [3].
Alopecia has been reported in only a few cases. It is generally diffuse, with thin hair, without scarring and with positive hair pull test. It may affect all the hair-bearing areas of the body [6, 7]. Histopathologically there is perifollicular amyloid deposition. Hunt et al suggested that the amyloid infiltration could affect perifollicular blood vessels and lead to a failure in anagen restoration [7]. In our case with end-stage disease the amyloid also infiltrated the hair follicles and destroyed them.
Nail dystrophy is another uncommon presentation of SA. The changes are similar to those caused by lichen planus: brittleness, crumbling, longitudinal ridging, onychoschizia, subungual thickening, onycholisis and anonychia [5, 8, 9]. Histopathology reveals dermal amyloid deposition of matrix and nail bed [8, 9].
In conclusion, dermatologists must know this life-threatening systemic disease and keep it in mind when facing atypical cases of alopecia, nail dystrophy, paronychia, sicca syndrome or diffuse skin infiltration. Biopsies of any suspicious lesions and serum protein electrophoresis testing should reveal the plasma cell dyscrasia.
References
1. Daoud MS, Lust JA, Kyle RA, Pittelkow MR. Monoclonal gammopathies and associated skin disorders. J Am Acad Dermatol 1999; 40(4):507-35. [PubMed]2. Rajkumar V. Pathogenesis and clinical features of AL (primary) amyloidosis and light and heavy chain deposition diseases. In: UpToDate, Rose, BD (Ed), UpToDate, Waltham, MA, 2009
3. Ahmed I, Cronk JS, Crutchfield CE 3rd, Dahl MV. Myeloma-associated systemic amyloidosis presenting as chronic paronychia and palmodigital erythematous swelling and induration of the hands. J Am Acad Dermatol. 2000; 42; 339-42. [PubMed]
4. Wong CK. Mucocutaneous manifestations in systemic amyloidosis. Clin Dermatol. 1990; 8(2):7-12. [PubMed]
5. Breathnach SM. Amyloid and amyloidosis. J Am Acad Dermatol. 1988;18;1-16. [PubMed]
6. Fujita Y, Tsuji-Abe Y, Sato-Matsumura KC, Akiyama M, Shimizu H. Nail dystrophy and blisters as sole manifestations in myeloma-associated amyloidosis. J Am Acad Dermatol. 2006; 54(4): 712-4. [PubMed]
7. Lutz ME, Pittelkow MR. Progresive generalized alopecia due to systemic amyloidosis. JAAD. J Am Acad Dermatol. 2002; 46(3):434-6. [PubMed]
8. Hunt SJ, Caserio RJ, Abell E. Primary systemic amyloidosis causing diffuse alopecia by telogen arrest. Arch Dermatol. 1991; 127(7):1067-8. [PubMed]
9. Prat C, Moreno A, Viñas M, Jucglà A. Nail dystrophy in primary systemic amyloidosis. JEADV. J Eur Acad Dermatol Venereol. 2008; 22(1):107-9. [PubMed]
10. Mancuso G, Fanti PA, Berdondini RM. Nail changes as the only skin abnormality in myeloma-associated systemic amyloidosis. Br J Dermatol. 1997; 137(3):471-2. [PubMed]
© 2013 Dermatology Online Journal