Spontaneous cutaneous umbilical endometriosis: Report of a new case with immunohistochemical study and literature review
Published Web Location
https://doi.org/10.5070/D33mj2444nMain Content
Spontaneous cutaneous umbilical endometriosis: Report of a new case with immunohistochemical study and literature review
Kyriakos Kyamidis MD, Viviana Lora MD, Jean Kanitakis MD
Dermatology Online Journal 17 (7): 5
Department of Dermatology, Edouard Herriot Hospital Group, Lyon, France. jean.kanitakis@univ-lyon1.frAbstract
Endometriosis (i.e., the presence of functional endometrial tissue outside the uterine cavity) may rarely affect the skin either spontaneously or secondary to abdomino-pelvic surgery. Spontaneous cutaneous endometriosis appears most commonly on the umbilicus (Villar nodule) and manifests with a red-brown nodule that characteristically shows cyclic variations (tenderness or bleeding) with the menstrual cycle. We present herein a new case of spontaneous cutaneous endometriosis of the umbilicus that was studied immunohistochemically and review the salient clinicopathologic features of this rare condition.
Introduction
The term “endometriosis” (EM) describes the presence of functional endometrial tissue outside the uterine cavity. The first description of this condition was made by the German physician, Daniel Schroen, in 1690 [1]. Endometriosis is a chronic, mostly benign condition affecting up to 15 percent of reproductive age women [2], but can occur also in women in menarche and in menopause [3, 4], and exceptionally also in men after long-term hormonal therapy for prostatic tumors [5]. The most common sites of EM are the ovaries, followed by the appendix, intestine, cervix, omentum, and the skin [6]. Cutaneous EM (CEM) is usually secondary, following abdomino-pelvic surgery, but can rarely appear spontaneously, in the absence of prior surgery; in the latter case it shows predilection for the umbilical region. We present herein a new case of spontaneous cutaneous umbilical endometriosis that was studied immunohistochemically and review the relevant literature in order to highlight the salient features of this uncommon condition.
Case report
 |  |
| Figure 1 | Figure 2 |
|---|
 |  |
| Figure 3 | Figure 4 |
|---|
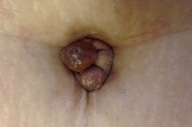
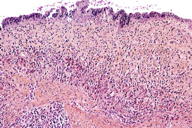
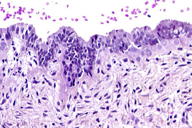
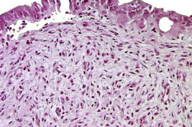
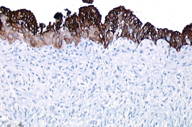
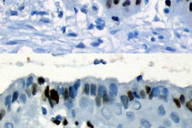
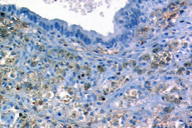
A 37-year-old woman presented with a multilobated, red-brownish nodule that had developed ten years earlier over her umbilicus (Figure 1), two years after the delivery of a single healthy baby. This lesion had slowly grown in size and was reportedly tender and exhibited occasional bleeding during the menses. The patient was otherwise healthy. A clinical diagnosis of EM was made and confirmed by a skin biopsy taken from the nodule. This showed, within the dermis, an epithelial lining made of 2-4 rows of cylindrical or polygonal cells with an eosinophilic cytoplasm and regular nuclei (Figures 2 and 3). The surrounding dermis contained a proliferation of capillary vessels and fibroblasts, as well as extravasated red-blood cells and a rather dense cell infiltrate made predominantly of macrophages containing a brown granular pigment that proved to be hemosiderin (Perls stain positive) (Figure 4). Immunohistochemically, the epithelial cells in the dermis expressed strong cytoplasmic reactivity for pan-keratin (AE1/AE3), keratin 7 (Figure 5), and nuclear reactivity for estrogen receptors (Figure 6a). A lower percentage of cells (about 20%) expressed nuclear reactivity for progesterone receptors (Figure 6b). No expression of keratin 20 or calretinin was seen. Dermal-stromal fibroblasts expressed the CD10 antigen (Figure 7).
 |  |
| Figure 5 | Figure 6 |
|---|
 |
| Figure 7 |
|---|
The nodule was excised under general anesthesia; it was found to be contiguous with the umbilical peritoneum. The post-operative course was uneventful.
Discussion
Endometriosis (EM) occurs in the majority of cases in the pelvic genital organs, especially the ovaries (up to 88% of all cases) and the fallopian tubes, but may be found in almost every tissue or organ, such as the CNS [7], the extremities (bones or muscles) [8], the urinary system [9], the lungs, the pleura [10], the gallbladder [11], the pancreas, the nasal mucosa [12] and possibly also the spleen [13]. According to its site, a classification of EM in four classes has been proposed (I: intestinal tract, U: urinary tract, L: lung and thoracic cage, O: all other sites) [14].
Cutaneous EM (CEM) accounts for less than 5.5 percent of all EM cases [15, 16, 17]. In our dermatopathology laboratory, out of 44100 biopsies examined over the last ten years, we encountered five cases of CEM (0.01%), three of which were located on the umbilicus. Cutaneous endometriosis affects patients with a mean age of 35-38 years [15, 18] and appears most commonly (>70% of cases) on scars (scar or secondary EM) over the abdomen, the perineum, the inguinal area, and the vulva. The onset often follows various types of gynecologic surgery, such as cesarean section, laparoscopy/laparotomy, hysterectomy, metroplasty, myomectomy, episiotomy, appendicectomy, Bartholin gland cyst removal, amniocentesis, and intrauterine injections for abortions [17]. The alleged mechanism is iatrogenic implantation of endometrial tissue into the skin during the procedure. The relative risk of developing surgical scar EM following cesarean section delivery has been estimated to 27.37 [19]. Occasionally, secondary EM may develop in a site not directly related to the surgical scar [20].
Less than 30 percent of CEM cases appear in the absence of prior surgery and are then referred to as primary or spontaneous CEM [15-17]. In this case, the most common site is the umbilicus followed by the inguinal area and the abdominal wall [21]. The right inguinal area seems more often affected than the left one (allegedly because of the clockwise movement of the peritoneal fluid because of the peristaltic movement of the intestinal wall) [22, 23].
Cutaneous EM of the umbilicus is also known as Villar nodule, with reference to the physician who first described it in 1886. Cutaneous endometriosis can develop spontaneously during pregnancy, and is then most often located on the umbilicus [24, 25]; it may regress spontaneously after delivery [24]. Umbilical EM (UEM) accounts for up to 30-40 percent of all CEM cases [15, 16, 26]. It manifests as a rubbery or firm nodule ranging in size from some mm to 6-9 cm (mean 2-2.5 cm). Its color varies from red, blue to brown-black, depending on the amount of hemorrhage and the penetration depth of ectopic endometrial tissue. Occasionally, the nodule is flesh-colored [27, 28]. It is usually single and often multilobated, although multiple discrete nodules may be present [29]. Clinical symptoms include tenderness, pain, bleeding, swelling, and growth correlated with the menstrual cycle. However, not all symptoms are present in a given patient and some patients are totally asymptomatic (30). Ubilical EM may be associated with umbilical hernia [31]. When UEM is associated with pelvic EM, general symptoms such as dysmenorrhea and dyspareunia may be present.
Histologically, CEM is characterized by the presence of endometrial glands and stroma in the mid- or deep dermis. The endometrial glands are made of tall columnar epithelium with basophilic cytoplasm and basally located nuclei, forming irregular glandular lumina, sometimes with a marked mitotic activity, depending on the phase of the menstrual cycle. The high cellular and vascular stroma is composed of spindle cells and is usually edematous. Menstrual bleeding into the dermis leads to hemosiderin deposition (which is seen with the Perls stain), scarring and chronic inflammation [32, 33]. The pathologic appearance varies somewhat according to the phase of the cycle (proliferative, secretion, decidualization) [33]. Several metaplastic changes can be seen in the glandular epithelium (tubal, oxyphilic, hobnail, mucinous, and papillary syncytial) and the stroma (smooth muscle metaplasia, decidualization, stromal endometriosis, and elastosis) [34]. Atypical changes include reactive atypia and atypical mitoses. Differential diagnosis should be made with metastatic carcinoma or other malignancies, especially if hypertrophic or myxoid decidual changes occur during pregnancy [33]. Endometrial epithelial cells express keratin 7 [35], the Human Epithelial Antigen (BerEP4) [36], estrogen and progesterone receptors [35, 36, 37], and Ki-67 [37]. Neither keratin 20 nor calretinin are expressed [35, 36]. These findings are in accordance with the immunohistochemical properties of normal human endometrial epithelium (keratin 7+/keratin 20-) [38]. Our immunohistochemical findings are in accordance with those of the literature. CD10 has often been used as a marker of stromal cells in CEM [35, 36, 37, 39]. However, in our opinion the usefulness of this marker is limited because several fibroblastic cells of the normal dermis express this neutral endopeptidase [40]. Other less specific markers that are reportedly expressed by stromal cells of CEM include smooth-muscle actin (SMA), von Willebrand factor, caldesmon, desmin, VEGF, and COX-2 [38, 41]. Immunohistochemical examination, namely with antibodies to keratin polypeptides, are useful for the differentiation of EM from metastatic adenocarcinomas from the digestive tract that are typically keratin 7-/keratin 20+.
The diagnosis of CEM can be suspected clinically on the basis of the clinical appearance and a good history, but relies mainly on histopathological examination. Other diagnostically helpful imaging methods include dermatoscopy, MRI, and ultrasonography. Dermatoscopical findings of EM include a homogenous reddish pigmentation with small, well-defined, globular structures of a deeper hue, termed “red atolls” [42]. The findings in MRI include a low signal on T1 weighting and a low or high signal on T2 weighting, depending on the presence or lack thereof, respectively, of hemosiderin [30, 43]. Ultrasonography and computed tomography are more accessible than, but not as sensitive as, MRI. Fine needle aspiration cytology has been used, but its results may be inconclusive [17, 22, 44]. Serum CA-125 levels may be increased (up to 260 U/ml) [24, 37, 44], but this finding is not specific for EM.
The clinical differential diagnosis of UEM includes all tumors that may involve the umbilicus, namely Sister (Mary) Joseph nodule (umbilical metastasis of a visceral carcinoma), hemangioma, umbilical hernia, pyogenic or foreign body granuloma, primary carcinoma or sarcoma, (irritated) nevus or melanoma, keloids developing on previous scars, urachal duct cyst, and endosalpingiosis [31, 45]. Inguinal EM can be mimicked by (angio)lipomas and enlarged lymph nodes.
The accepted pathogenetic mechanism of secondary or scar EM is iatrogenic implantation of endometrial tissue into the skin during a surgical procedure. The pathogenesis of spontaneous EM is, however, still elusive. Several hypotheses have been proposed, such as the in situ theory, the transplantation theory, and the induction theory, a combination of the two former theories. The transplantation theory is the most widely accepted and postulates that implantation via retrograde menstruation or mechanical (iatrogenic) transplantation or hematogenous/lymphogenous metastasis occurs. The in situ theory suggests the presence of embryonic cell remnants. The induction theory is a combination of the former two theories [46]. Recent studies have shown that cadherins and integrins are important cell adhesion molecules of endometrial cells. An impaired immune response in both T-cell-mediated cytotoxicity and a decrease in natural killer (NK)-cell activity, could account for a decreased clearance of endometrial cells from the peritoneal cavity. Macrophages seem to also play an important role in the pathogenesis of EM through the induction of cytokines that stimulate the endometrial cell proliferation [46, 47].
The treatment of CEM is mainly surgical, preferably performed at the end of the menstrual cycle when the lesion is small in order to achieve a minimal excision [48]. The technique of removal varies depending on the size and extent of the lesion, from simple excision with wide margins under local anesthesia to laparoscopic excision en block of the umbilicus [28].A prolene mesh may be necessary to prevent the development of hernia, if the defect in the rectus sheath is large [17, 49]. Treatment with Gonadotropin-Releasing Hormone agonists, danazol, and contraceptive pills can be given in order to reduce tumor size before excision, or provide relief from the symptoms [17, 50]; these are insufficient as sole treatments [50] and may lead to incomplete excision [17]. Gynecologic examination and hormonal evaluation are recommended after excision of CEM in order to detect an associated pelvic EM. Abdominal and transvaginal ultrasonography or MRI scan should be performed in all asymptomatic patients, but whether laparoscopic examination should be systematically performed is still debated [17, 22, 28, 37, 50].
The prognosis of CEM is good. Recurrences are uncommon if excision is performed with clean and wide margins. However, malignant transformation has been reported in 0.3 percent to 1 percent of scar EM and should be suspected in the case of rapidly-growing or recurrent lesions [51, 52]. The commonest histological subtype is endometrioid carcinoma (69%) followed by clear-cell carcinoma (13.5%), (adeno)sarcomas (11.6%) and serous carcinoma [51, 52].
In some studies, a statistically significant association between EM and the development of melanoma has been found, with a relative risk of 1.62 [53]. It has been speculated that abnormal expression of some tumor suppressor genes (namely p16Ink4, p53, and PTEN) may favor the development of the two conditions. Long-term hormonal treatment given for EM could also favor the development of melanoma. However, other studies have failed to confirm this association [54, 55]. In any event, there are no precise data on a possible association of CEM with melanoma, because the studies performed so far did not examine specifically CEM.
In conclusion, physicians should consider CEM in the differential diagnosis of nodules appearing over the abdominal wall, especially the umbilicus [26, 29, 30, 48, 56-62], in reproductive-age women. The diagnosis can be suspected clinically based on history, but should be confirmed with histological examination. Treatment is surgical excision with wide margins. Gynecologic evaluation is recommended after excision, especially if the patient is symptomatic, for pelvic endometriosis. Malignant transformation, although very rare, should be suspected in recurrent or rapidly growing lesions.
References
1. Shroen D. Disputatio Inauguralis. Medica de Uleribus Uteri. Jena; Krebs: 1690, pp 6-172. Purvis RS, Tyring SK. Cutaneous and subcutaneous endometriosis: Surgical and hormonal therapy. J Dermatol Surg Oncol 1994;20(10):693-5 [PubMed]
3. Laufer MR. Premenarcheal endometriosis without an associated obstructive anomaly: Presentation, diagnosis and treatment. Fertil Steril 2000;74:S15
4. Choi SW Lee HN, Kang SJ, Kim HO. A case of cutaneous endometriosis in postmenopausal woman receiving hormonal replacement. J Am Acad Dermatol 1999;41(32):327-9 [PubMed]
5. Martin JD Jr, Hauck AE. Endometriosis in the male. Am Surg 1985;51(7):426-30 [PubMed]
6. Odobasic A, Pasic A, Iljazovic-Latifagic E, Arnautalic L, Odobasic Ad, Idrizovic E, Dervisefendic M, Dedic L. Perineal endometriosis: a case report and review of the literature. Tech Coloproctol 2010;14(S1):S25-7 [PubMed]
7. Ichida M, Gomi A, Hiranouchi N, Fujimoto K, Suzuki K, Yoshida M, Nokubi M, Masuzawa T. A case of cerebral endometriosis causing catamenial epilepsy. Neurology 1993 Dec;43(12):2708-9. [PubMed]
8. Giangarra C, Gallo G, Newman R, Dorfman H. Endometriosis in the biceps femoris. A case report and review of the literature. J Bone Joint Surg Am 1987;69:290-2. [PubMed]
9. Calderón-Andrade HF, Murillo-Olivas M. Ureteral endometriosis: A case report. Rev Mex Urol 2010;70(2):123-6.
10. Baram A, Bagan P, Danel C, Badia A, Riquet M. Pleural endometriosis: An unusual presentation. Rev Mal Respir 2005;22(4):677-80. [PubMed]
11. Saadat-Gilani K, Bechmann L, Frilling A, Gerken G, Canbay A. Gallbladder endometriosis as a cause of occult bleeding. World J Gastroenterol 2007 Sep 7;13(33):4517-9. [PubMed]
12. Laghzaoui O, Laghzaoui M. Nasal endometriosis: a propos of one case. J Gynecol Obstet Biol Reprod 2001;30(8):786-8. [PubMed]
13. Sinder C, Dochat GR, Wentsler NE. Splenoendometriosis. Am J Obstet Gynecol 1965;15(92):883-4 [PubMed]
14. Markham S, Carpenter S, Rock J. Extrapelvic endometriosis. Obstet Gynecol Clin North Am 1989;16(1):193-219. [PubMed]
15. Fernández-Aceñero MJ, Córdova S. Cutaneous endometriosis: review of 15 cases diagnosed at a single institution. Arch Gynecol Obstet 2010 Apr 27 [Epub ahead of print] [PubMed]
16. Douglas C, Rotimi O. Extragenital endometriosis – A clinicopathological review of Glasgow hospital experience with case illustrations. J Obstet Gynecol 2004;24(7):804-8 [PubMed]
17. Agarwal A, Fong YF. Cutaneous endometriosis. Singapore Med J 2008;49(9):704-9 [PubMed]
18. Victory R, Diamond D, Johns A. Villar’s nodule: A case report and systematic literature review of endometriosis externa of the umbilicus. J Minimal Invas Gynecol 2007;14:23-32. [PubMed]
19. Leite GKC, Garvalho LFP, Korkes H, Guazelli TF, Kenj G, Viana AT. Scar endometrioma following obstetric surgical inscicions: Retrospective study on 33 cases and review of the literature. Sao Paulo Med J 2009; 127(5):270-7 [PubMed]
20. Esteves T, Cabrita J, Coelho R, Vale E. Endometriose cutânea. Dermatol Online J 2010;16(5):9 [PubMed]
21. Steck MWD, Helwig EB. Cutaneous endometriosis. Clin Obstet Gynecol. 1966;9(2):373-83. [PubMed]
22. Wong W, Lim C, Luo X. Inguinal endometriosis: An uncommon differential diagnosis as an inguinal tumor. ISRN Obstet Gynecol. Article ID 272159 doi:10.5402/2011/272159
23. Apostolidis S, Michalopoulos A, Papavramidis TS, Papadopoulos VN, Paramythiotis D, Harlaftis N. Inguinal endometriosis: three cases and literature review. South Med J. 2009;102(2):206-7. [PubMed]
24. Razzi S, Rubegni P, Sartini A, De Simone S, Fava A, Cobellis L, Fimiani M, Petraglia F. Umbilical endometriosis in pregnancy: a case report. Gynecol Endocrinol 2004;18(2):114-6. [PubMed]
25. Wiegratz I, Kissler S, Engels K, Strey C, Kaufmann M. Umbilical endometriosis in pregnancy without a previous surgery. Fertil Steril 2008;90(1):199. [PubMed]
26. Dadhwal V, Gupta B, Dasgupta C, Shende U, Deka D. Primary umbilical endometriosis: a rare entity. Arch Gynecol Obstet. 2010 Dec 18. [Epub ahead of print] [PubMed]
27. Skidmore RA, Woosley JT, Katz VL. Decidualized umbilical endometriosis. Int J Gynecol Obstet 1996:52(3):269-73 Int J Surg 2010;8(2):109-11. [PubMed]
28. Fedele L, Frontino G, Biachi S, Borruto F, Ciappina N. Umbilical endometriosis: A radical excision with laparoscopic assistance. Int J Surg 2010;8(2):109-11. [PubMed]
29. Weller CV. Endometriosis of the umbilicus. Am J Pathol 1935;11(2): 281-6. [PubMed]
30. Hartigan CM, Holloway BJ. MR imaging features of endometriosis at the umbilicus. Brit J Radiol 2005;78(932):755-7. [PubMed]
31. Ramsanahie A, Giri SK, Velusamy S, Nessim GT. Endometriosis in a scarless abdominal wall with underlying umbilical hernia. Ir J Med Sci 2000;169(1):67. [PubMed]
32. Weedon D. Endometriosis. In: Weedon D (ed). Skin Pathology (2nd edition). Churchill Livingstone, Edinburgh, 2002, p. 514.
33. Elder D, Elenitsas R, Ragsdale B. Cutaneous endometriosis. In: Elder D, Elenitsas R, Jaworsky C, Johnson B (eds). Lever’s Histopathology of the Skin (8th edition). Lippincott Raven, Philadelphia, 1997, p. 796.
34. Kazakov D, Ondic O, Zamecnik M, Shelekhova KV, Mukensnabl P, Hes O, Dvorak V, Michal M. Morphological variations of scar-related and spontaneous endometriosis of the skin and superficial soft tissue: a study of 71 cases with emphasis on atypical features and types of müllerian differentiations. J Am Acad Dermatol. 2007;57(1):134-46. [PubMed]
35. Lee H, Kim KR. Intestinal Endometriosis: Clinicopathologic analysis of 15 cases including a case of endometrioid adenocarcinoma. Korean J Pathol 2009;43(2):120-5.
36. Baram A, Bagan P, Danel C, Badia A, Riquet M. Pleural endometriosis: An unusual presentation. Rev Mal Respir 2005;22(4):677-80. [PubMed]
37. Mechsner S, Bartley J, Infanger M, Loddenkemper C, Herbel J, Ebert AD. Clinical management and Immunohistochemical analysis of umbilical endometriosis. Arch Gynecol Obstet 2009;280(2):235-42. [PubMed]
38. Campbell F, Herrington C. Application of cytokeratin 7 and 20 immunohistochemistry to diagnostic pathology. Current Diagnostic Pathology 2001;7(2):113-22
39. Fukuda H, Mukai H. Cutaneous endometriosis in the umbilical region: the usefulness of CD10 in identifying the interstitium of ectopic endometriosis. J Dermatol 2010;37(6):545-9. [PubMed]
40. Kanitakis J, Bourchany D, Claudy A. Expresion of the CD10 antigen by mesenchymal tumors of the skin. Anticancer Res 2000;20(5B): 3539-44. [PubMed]
41. Terada S, Miyata Y, Nakazawa H, Higashimori T, Arai T, Kikuchi Y, Nozaki M. Immunohistochemical analysis of an ectopic endometriosis in the uterine round ligament. Diagn Pathol 2006;9(1):27. [PubMed]
42. Di Giorgi V, Massi D, Mannone F, Stante M, Carli P. Cutaneous endometriosis: Non-invasive analysis by epiluminescence microscopy. Clin Exp Dermatol 2003;28(3):315-7. [PubMed]
43. Yu C, Perez-Reyes M. MR appereance of umbilical endometriosis. J Comput Assist Tomogr 1994;18(2):269-71. [PubMed]
44. Zhao X, Lang J, Leng J, Liu Z, Sun D, Zhu L. Abdominal wall endometriomas. Int J Gynecol Obst 2005;90(3):218-22 [PubMed]
45. Papavramidis TS, Sapalidis K, Michalopoulos N, Karayannopoulou G, Cheva A, Papavramidis ST. Umbilical endosalpingiosis : A case report. J Med Case Reports 2010;4;(4):287 [PubMed]
46. Van der Linden P. Theories on the pathogenesis of endometriosis. Hum Reprod 1996;11(S3):53-65 [PubMed]
47. Guarnaccia M, Silverberg K, Olive DA. Endometriosis and adenomyosis. In: Copeland LJ, Jarrel JF, McGregor JA (eds). Textbook of Gynecology. 2nd edition Philadelphia, Saunders, 2000.
48. Chatzikokkinou P, Thorfin J, Angelidis IK, Papa G, Trevisan G. Spontaneous endometriosis in an umbilical skin lesion. Acta Dermatovenerol Alp Panonica Adriat 2009;18(3):126-30 [PubMed]
49. Sidiropoulou Z, Souza AC, Gameiro P, Madureira R. Spontaneous abdominal wall endometriosis, a case report and a literature review. J Clin Diagn Res 2009;3(6):1931-4
50. Bagade PV, Guirguis MM. Menstruating from the umbilicus as a rare case of primary umbilical endometriosis: a case report. J Med Case Reports. 2009 Dec 10;3:9326. [PubMed]
51. Chene G, Darcha C, Dechelotte P, Mage G, Canis M. Malignant denegeration of perineal endometriosis in episiotomy scar, case report and review of the literature. Int J Gynecol Cancer 2007;175(3):709-14. [PubMed]
52. Heaps JM, Nieberg RK, Berek JS. Malignant neoplasms arising in endometriosis. Obstet Gynecol 1990;75(6):1023-8. [PubMed]
53. Kvaskoff M, Mesrine S, Clavel-Chapelon F, Boutron-Ruault MC. Endometriosis risk in relation to naevi, freckles and skin sensitivity to sun exposure: the French E3N cohort. Int J Epidemiol. 2009;38(4):1143-53 [PubMed]
54. Brinton LA, Gridley G, Persson I, Baron J, Bergqvist A. Cancer risk after a hospital discharge diagnosis of endometriosis. Am J Obstet Gynecol 1997;176 (3):572-579. [PubMed]
55. Olson JE, Cerhan JR, Janney CA, Anderson KE, Vachon CM, Sellers TA. Postmenopausal cancer risk after self-reported endometriosis diagnosis in the Iowa Women’s Health Study. Cancer 2002;94(5):1612-8. [PubMed]
56. Rai R, Sathyamoorthy A, D’Souza C. Umbilical endometriosis. J Clinic Diagn Res 2008;2(6):1203-1206
57. Panicker R, Pillai N, Nagarserkar U. Villar’s nodule: A rare presentation of external endometriosis. Med J Armed Forces India 2010;66(1):70-1
58. Chiang DT, The WT. Cutaneous endometriosis. Surgical presentations of a gynecological condition. Austral Fam Physician 2006;35(11): 887-8 [PubMed]
59. Lee A, Tran HT, Walters RF, Yee H, Rosenman K, Sanchez MR. Cutaneous umbilical endometriosis. Dermatol Online J 2008;14(10):23 [PubMed]
60. Friedman PM, Rico MJ. Cutaneous endometriosis. Dermatol Online J 2000;6(1):8 [PubMed]
61. Muñoz H, Waxtein L, Vega ME, Cortes R, Hojyo MT, Dominguez-Soto L. An ulcerated umbilical nodule. Arch Dermatol 1999;135(9):1113-8 [PubMed]
62. Al-Saad S, Al-Shinawi HM, Kumar MA, Brair AFI. Extra-gonadal endometriosis: unusual presentation. Bahrain Med Bull 2007; 29(1): 1-11
© 2011 Dermatology Online Journal

