Tender nodules on the extremities
Published Web Location
https://doi.org/10.5070/D332k6213zMain Content
Tender nodules on the extremities
Alaina J James MD PhD1, Matthew M Bender MD1, Alice J Chen MD2, Ilene B Bayer-Garner MD1,2, and Sylvia Hsu MD1
Dermatology Online Journal 9(5): 20
From the Departments of Dermatology1 and Pathology2, Baylor College of Medicine, Houston. shsu@bcm.tmc.edu
Case presentation
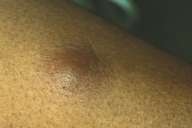
A 45-year-old West African man presented with a 5-day history of a red nodule on his left thigh (fig. 1) and a 3-week history of cough, fever, and night sweats. Although he had not been to West Africa in 2 years, his occupation involved selling West African art in the southeastern United States, including the Mississippi River Valley region.
Physical examination showed a 2-cm red, warm, tender nodule on his left leg and a 1-cm flesh-colored nodule on his right forearm. Lymphadenopathy was present in the left inguinal region. A chest radiograph revealed multilobar infiltrates. Bronchoscopic biopsy showed chronic inflammation with an intense eosinophilic response. Smears and cultures from the bronchoscopy were negative. HIV antibodies were also absent.
|

|
| Figure 1 | Figure 2 |
|---|
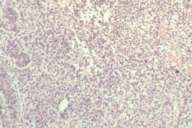
A punch biopsy from the left thigh was obtained for histology, special stains, and culture. The biopsy showed a mildly acanthotic epidermis covered by a layer of parakeratosis. A mixed inflammatory infiltrate was present in the deep dermis extending into the subcutis (fig. 2).
|

|
| Figure 3 | Figure 4 |
|---|
The inflammatory infiltrate, comprising histiocytes, lymphocytes, leukocytes, and scattered plasma cells, formed a dermal abscess (fig. 3). A silver stain shows the characteristic broad-based budding of Blastomycosis dermatitidis (fig. 4). A culture later confirmed the diagnosis.
The patient was started on amphotericin but rapidly developed acute renal insufficiency. He was switched to oral itraconazole with marked improvement in his cutaneous lesions and pulmonary symptoms.
Discussion
In 1894 T. C. Gilchrist described B. dermatitidis [5]. Also known as Gilchrist disease, Chicago disease, and North American blastomycosis, it typically occurs as a primary pulmonary infection with extrapulmonary involvement in 50 percent of cases.
B. dermatitidis is a broad-based, budding yeast, which is 8-20 µm in diameter, having a thick, refractile cell wall and multiple nuclei. It is a thermally dimorphic saprophyte endemic to the Mississippi River Valley (Kentucky, Mississippi, Arkansas, Tennessee, Illinois, Louisiana, and Wisconsin), southern Canada, and Central America. In these regions, B. dermatitidis exists as a mycelial form in warm, moist and richly organic soil, decomposed vegetation, and wood [1, 2]. On inhalation of airborne spores, the core body temperature induces the transformation of the blastomyces spores into thick-walled, budding yeasts [3]. The pulmonary system is initially seeded, but the fungus may be distributed hematogenously to the skin, bone, genitourinary tract, and central nervous system [4]. The clinical manifestations of blastomycosis are extremely variable and may render the initial diagnosis quite difficult.
The clinical presentation of blastomycosis is variable, ranging from an asymptomatic primary infection to disseminated primary infection or a fulminant infectious acute respiratory distress syndrome. The symptoms are often vague, including fever, malaise, fatigue, and weight loss. The most common extrapulmonary site of infection is the skin, including mucous membranes, the face, and other exposed areas. Dissemination of blastomycosis to the skin usually occurs during the early symptomatic phase but may occur from weeks to years after the primary infection. A delayed skin presentation may occur subsequent to resolution of the pulmonary pathology, thus complicating the diagnosis. The skin lesions are typically either a well-circumscribed ulcer surrounded by an inner margin of pustules and an outer margin of papules or a crusting, draining verrucous lesion with an irregular border associated with a subcutaneous abscess [5, 6]. Histologically, the lesions show papillomatosis and a dermal abscess with a neutrophilic infiltrate. The skin lesions of blastomycosis are often initially clinically misdiagnosed as keratoacanthoma, basal cell carcinoma, warts, squamous cell carcinoma, tuberculosis, other deep fungi, or pyoderma gangrenosum.
The other common extrapulmonary sites of infection include the pleura, bone, genitourinary tract, and central nervous system. Blastomycosis of the pleura usually presents with pleural effusions and is generally considered a poor prognostic factor. In the bone, the most common presentation is bone or joint pain secondary to osteomyelitis. It most often involves the spine, ribs, and skull. In males, blastomycosis may spread to the genitourinary system, causing prostatitis and epididymoorchitis. In the central nervous system, blastomycosis is associated with meningitis and cranial abscesses [7]. In extrapulmonary sites, other more common organisms are usually the causative agent, and without a history of camping or working in woody areas of the Mississippi River Valley, blastomycosis may not enter the clinical or pathologic differential diagnosis.
The diagnosis of B. dermatitidis is based on microscopic identification of a dimorphic, broad-based yeast in tissue samples or smears. Histopathologic identification of B. dermatitidis is enhanced by special stains including PAS, methenamine silver, and Papanicolaou stains. Cultures of B. dermatitidis demonstrate cotton-white to brown colonies at 25° C and broad-based yeast forms at 37° C.
The growth conditions and the mycologic characteristics of the broad-based budding yeast of B. dermatitidis is similar to H. duboisii. These two entities may be differentiated through serologic studies and the GenProbe test. Interestingly, our patient had a history of travel throughout the Mississippi River Valley region and contact with materials from Western Africa, thus the complicating the diagnosis.
In a large percentage of patients spontaneous resolution of blastomycosis occurs. Treatment is necessary, however, in cases of a progressive and unrelenting infection. The treatment of choice is amphotericin B or itraconazole [8]. Amphotericin B is recommended in rapidly progressive disease and in patients with multiple medical problems. In low-grade, nonemergent cases, oral itraconazole is an effective therapeutic agent.
References
1. Denton JF ME, Ajello L, et al. Isolation of Blastomyces dermatitidis from soil. Science 1961;133:1126-7.2. Bakerspigel A, Kane J, Schaus D. Isolation of Blastomyces dermatitidis from an earthen floor in southwestern Ontario, Canada. J Clin Microbiol 1986;24(5):890-1. PubMed
3. Medoff G, Painter A, Kobayashi GS. Mycelial- to yeast-phase transitions of the dimorphic fungi Blastomyces dermatitidis and Paracoccidioides brasiliensis. J Bacteriol. 1987 Sep;169(9):4055-60. PubMed
4. Bradsher RW. Clinical features of blastomycosis. Semin Respir Infect 1997;12(3):229-34. PubMed
5. Mercurio MG, Elewski BE. Cutaneous blastomycosis. Cutis 1992;50(6):422-4. PubMed
6. Leet NA, Parker CM. Multiple verrucous skin lesions. North American blastomycosis. Arch Dermatol 1991;127(5):723, 26. PubMed
7. Areno JP, Campbell GD, Jr., George RB. Diagnosis of blastomycosis. Semin Respir Infect 1997;12(3):252-62. PubMed
8. Chapman SW, Bradsher RW, Jr., Campbell GD, Jr., Pappas PG, Kauffman CA. Practice guidelines for the management of patients with blastomycosis. Infectious Diseases Society of America. Clin Infect Dis 2000;30(4):679-83. PubMed
© 2003 Dermatology Online Journal

