Old World eyelid cutaneous leishmaniasis: A case report
Published Web Location
https://doi.org/10.5070/D32pn8p44dMain Content
Old World eyelid cutaneous leishmaniasis: A case report
Enrique Mencía-Gutiérrez1 MD, Esperanza Gutiérrez-Díaz1 MD, José L. Rodríguez-Peralto2 MD PhD, Juan Monsalve-Córdova1 MD
Dermatology Online Journal 11 (3): 29
Departments of Ophthalmology1 and Pathology2, 12 de Octubre Hospital, Complutense University, Madrid, Spain. emencia.hdoc@salud.madrid.org
Abstract
Leishmania is a protozoa that may infect the skin, mucous, and viscera. The geographical distribution of cutaneous leishmaniasis (CL) is mainly determined by the sandfly vectors. The Old World type is mainly attributed to Leishmania major and Leishmania tropica, and in South of Europe only to Leishmania infantum. A 63-year-old woman, who noted a pimple on the external third of the left upper eyelid 6 months before. The lesion was nodular, well-defined and measured 1.1 cm in diameter and in height, simulating a basal cell carcinoma. It was surgically excised. CL diagnosis was made upon the histologic examination, which showed histiocytes with intracellular leishmania organisms. At 2 years followup, no evidence exists of cutaneous, mucous, or visceral involvement. Apart from carcinomas, nodular lesions with central ulceration are rare on the eyelid. A single cutaneous lesion of leishmania (oriental sore) has to be considered in the differential diagnosis, along with malignant eyelid neoplasms.
Introduction
Leishmaniasis is a disease attributed to any of a number of species of protozoa of the genus Leishmania. It is transmitted by the bite of an infected female sandfly. There are four major clinical types of this infection: cutaneous, diffuse cutaneous, mucocutaneous, and visceral. Cutaneous leishmaniasis (CL) is characterized by the development of single or multiple localized lesions on exposed areas of skin that typically ulcerate and generally heal spontaneously within 3-6 months. In 1980 Rioux et al. [1] first isolated L. infantum from cutaneous lesions; until then this organism was considered to be exclusively an agent of visceral leishmaniasis; this finding has since been confirmed in several countries of the Mediterranean basin. L. infantum is the only species endemic to Spain [2]. The face is the site of predilection of infection, although the eyelid is not often involved. Where leishmaniasis is endemic, the incidence is increasingly prevalent in urban areas.
Clinical synopsis
|
| Figure 1 |
|---|
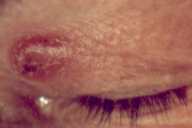
| Figure 1. A 1.1-cm well-defined nodule on the upper eyelid. |
A 63-year-old woman noted a small pimple on her left upper eyelid 6 months before presentation. The eyelid lesion enlarged slowly. It presented as a well-defined, firm, tender, subcutaneous skin-colored nodule with an erythematous halo; the edges were indurated and the center had a small ulcer that spontaneously bled. The lesion measured 1.1 cm in diameter and in height. The remaining ophthalmologic and systemic studies were normal. A medical history showed hypertension and insulin-treated diabetes.
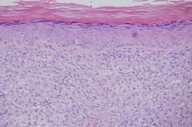
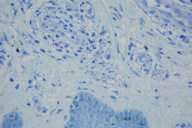
With a suspected diagnosis of a basal cell carcinoma, surgery was performed with 5-mm safety margins. The histopathologic examination of sections stained with hematoxylin and eosin showed a superficial reticular dermis occupied by large pale histiocytes with leishmania. With the Giemsa stain technique multiple leishmania were seen within large pale cytoplasm (Fig. 2), features consistent with the diagnosis of CL. HIV and leishmania serology tests were negative. A complete blood cell count and blood chemistries gave results within normal limits. No regional lymphadenopathy or clinical signs of visceral involvement were detected. After 2 years of followup, there have been no new lesions, cutaneous, mucous, or visceral.
Discussion
CL is caused by different species of the hemoflagellatic protozoan Leishmania and affects approximately 1.5 million individuals per year. Old World CL is separated into four distinct types: L. aethiopica, L. major, L. tropica and L. infantum. The geographical distribution of CL is mainly determined by the sandfly vectors Phlebotomus ariasi and Phlebotomus perniciosus in Spain [3]. This parasite is commonly seen on dogs; humans are considered an accidental host. L. infantum CL is a sporadic disease that has been described in most patients in foci where the visceral disease is endemic. L. infantum, in southwestern Europe, including Spain, is the only species that has long been identified in patients with authochthonous leishmaniasis [3], and includes 20 different zymodenes. Clinical forms of localized CL due to L. infantum are ulcerative, papular, infiltrative, and impetiginoid [1]. The face is the site of predilection in the CL. The low incidence on the eyelid is attributed to the frequent movements of the eyelid, which deter the sandfly from biting the skin in this region [4]. A dermotrophic species, they usually remain close to the inoculation site causing cutaneous disease, and they may produce satellite lesions, or affect lymphatic regional lymph nodes, as well. It is well known that infection by L. infantum can exist in a subclinical form in healthy individuals without a previous background of cutaneous or visceral leishmaniasis. These asymptomatic individuals could, therefore, act as reservoirs for parasites [5]. No documented case of L. infantum CL has been complicated by a visceral disease in an immunocompetent patient. Patients infected with HIV have a seroprevalence for L. infantum of 64 percent; thus HIV has emerged as a risk factor for CL [6].
In areas where leishmaniasis is endemic such as in the Mediterranean region, even in the absence of an appropriate history of exposure to Leishmania, such a possibility may be kept in mind for any eyelid skin lesion. The definitive diagnosis depends on demonstrating either amastigotes in tissue or promastigotes in culture. Serology is rarely helpful excepted by Western blotting [3]. The polymerase chain reaction-enzyme-linked immunosorbent assay has been developed for the diagnosis of CL and visceral leishmaniasis caused by L. infantum. The diagnosis in our case was based on the presence of amastigotes in the stains with Giemsa technique and hematoxylin and eosin, which may quickly yield a diagnosis in some patients. However, the finding of parasites in the epidermis has been exceptionally reported [3], as it has been in our patient.
As most Old World lesions heal rapidly without treatment, a waiting approach may be appropriate, particularly for those patients living in endemic areas, because spontaneous healing is associated with the development of protective immunity. Lesions on cosmetically or functionally important sites (such as the face or hands), those with associated lymphangitis, and multiple or persistent lesions are best given active treatment. Local treatment is appropriate for those with early non-inflamed lesions, and systemic therapy for those with multiple or more complicated lesions [7]. The pentavalent antimony derivatives sodium stibogluconate and meglumine antimoniate, remain the mainstay treatment [8]. Actually, the prevention and control of leishmaniasis vectors depends on the availability of a suitable public health infrastructure, including adequate supplies of insecticide, spraying equipment, and trained personnel [9].
In our case local excision was an important and definitive option, particularly as the presumed clinical diagnosis was of a basal cell carcinoma. Differential diagnosis for CL includes secondarily infected insect bite, sporotrichosis, or more rarely cutaneous tuberculosis; early detection of the infection is necessary in order to start effective treatment and prevent more serious complications. This presentation is unusual, having only been described in one case [10]. The clinical presentation should be considered in the differential diagnosis of malignant eyelid neoplasms.
References
1. Rioux JA, Lanotte G, Maazoun R, Perello R, Pratlong F, Leishmania infantum Nicolle, 1908, the agent of the autochthonous oriental sore. Apropos of the biochemical identification of 2 strains isolated in the eastern Pyrenees, CR Seances Acad Sci D.291:701-703,1980.2. Martin-Sanchez J, Gramiccia M, Di Muccio T, Ludovisi A, Morillas-Marquez F, Isoenzymatic polymorphism of Leishmania infantum in southern Spain, Trans R Soc Trop Med Hyg.98:228-232,2004.
3. Aransay AM, Testa JM, Morillas-Marquez F, Lucientes J, Ready PD, Distribution of sandfly species in relation to canine leishmaniasis from the Ebro Valley to Valencia, northeastern Spain, Parasitol Res.94:416-420,2004.
4. Morgan G, Case of cutaneous leishmaniasis of the lid, Br J Ophthalmol.49:542-546,1965.
5. Pineda JA, Martin-Sanchez J, Macias J, Morillas F, Leishmania spp infection in injection drug users, Lancet.360:950-951,2002.
6. Garrote JI, Gutierrez MP, Izquierdo RL, et al, Seroepidemiologic study of Leishmania infantum infection in Castilla-Leon, Spain, Am J Trop Med Hyg.71: 403-406,2004.
7. Hepburn NC, Cutaneous leishmaniasis: an overview, J Postgrad Med.49:50-54, 2003.
8. Berman J, Recent developments in leishmaniasis: epidemiology, diagnosis, and treatment, Curr Infect Dis Resp.7:33-38,2005.
9. Maroli M, Khoury C, Prevention and control of leishmaniasis vectors: current approaches, Parassitologia.46:211-215,2004.
10. Charif Chefchaouni M, Lamrani R, Benjelloune A, El Lyacoubi M, Berraho A, Cutaneous leishmaniasis of the lid, J Fr Ophthalmol.25:522-526,2002.
© 2005 Dermatology Online Journal