Pseudoverrucous papules and nodules: A case report
Published Web Location
https://doi.org/10.5070/D32p59p1xxMain Content
Letter: Pseudoverrucous papules and nodules: A case report
Thaer Douri, A Zahi Shawaf
Dermatology Online Journal 18 (4): 14
Department of Dermatology & Venereology, Ministry of Health, Hama, SyriaAbstract
Pseudoverrucous papules and nodules (PPN) is an uncommon complication, mainly reported in the diaper area. It is thought to be a manifestation of chronic irritant contact dermatitis that develops as a result of prolonged exposure to liquid stool and/or urine. We describe a case of a peristomal PPN in a patient who had a urostomy after treatment of bladder carcinoma with radical cystectomy.
Case report
A 55-year-old man presented with a 1-month history of an asymptomatic peristomal dermatitis, which was diagnosed as a skin infection and treated with a topical antifungal agent and antibiotic cream without improvement. The patient had a urostomy for three months after treatment of bladder carcinoma with radical cystectomy. He had no personal history of dermatitis or psoriasis.
 |  |
| Figure 1 | Figure 2 |
|---|
Skin examination showed several 3 mm to 5 mm flat gray-white warty papules and nodules with a peristomal distribution (Figure 1). The differential diagnosis included viral warts, neoplastic processes, halogenoderma, bacterial infections, candidiasis, and cutaneous Crohn disease.
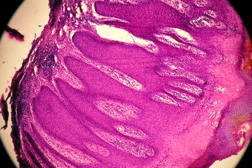
A skin biopsy revealed a marked psoriasiform epidermal hyperplasia with broad hyperparakeratosis (Figure 2). We suggested the diagnosis of pseudoverrucous papules and nodules (PPN) and we treated our patient with combination of zinc oxide and olive oil; resolution was noted in two weeks.
Discussion
Pseudoverrucous papules and nodules (PPN) is an uncommon complication, mainly reported in children in the diaper area and around ostomies after surgery for gastrointestinal or urologic diseases. It has been described after colectomy and coloanal anastomosis for Hirschsprung disease [1]. It has also been reported after radical cystectomy [2] as in our patient who had a bladder carcinoma treated with radical cystectomy and urostomy. In one case series, one fifth of patients with urostomies displayed pseudoverrucous skin lesions in a peristomal location. These lesions were described as wart-like papules or small, gray-white or reddish-brown erosive papules about 2 mm to 3 mm in size [3, 4]. Biopsy specimens of these pseudoverrucous lesions demonstrate a marked psoriasiform epidermal hyperplasia with broad hyperparakeratosis.
The condition is thought to be a manifestation of chronic irritant contact dermatitis that develops as a result of prolonged exposure to liquid stool and/or urine [2]. These lesions appear to be uncommon and sometimes can be misdiagnosed, even leading to surgical removal [5].
Jacquet erosive diaper dermatitis, perianal pseudoverrucous papules and nodules, and granuloma gluteale infantum/adultorum have been regarded as either separate entities or as part of the same clinical spectrum, representing the result of chronic severe irritant contact dermatitis [5, 6].
The differential diagnosis includes viral warts, condyloma lata, condyloma acuminata, neoplastic processes, halogenoderma, bacterial infections, candidiasis, cutaneous Crohn disease, and Langerhans cell histiocytosis [5, 7].
The treatment options include topical corticosteroid with zinc oxide as a barrier. We treated our patient topically with a combination of olive oil and zinc oxide twice daily. It did not make stoma adherence difficult and the PPN resolved after 2 weeks.
In my practice I usually use olive oil routinely for treatment of diaper dermatitis, alone or in combination with another topical antifungal or zinc oxide. It is safe and effective. Olive oil has been used since 4000 B.C.E. by the Mediterranean populations as a food, drug, and cosmetic [8]. Virgin oil's composition is like sebum, given its high content of squalene, β-sitosterol optimum fatty acid content (the presence of oleic acid, which acts as a skin softener), and antioxidant-rich substances. For these reasons it is particularly able to directly protect the skin. When applied to the skin after sun exposure, olive oil has an inhibitory effect on sun-induced cancer development. This is accomplished by the activation of enzyme p53, the substance that prevents and repairs skin damage caused by exposure to UVA [8, 9]. Topical use of olive oil alone or as an ingredient in dermo-cosmetology shows therapeutic effects (anti-inflammatory, anti-neoplastic, and anti-aging) [8].
References
1. Rodriguez-Poblador J, González-Castro U, Herranz-Martínez S, Luelmo-Aguilar J. Jacquet erosive diaper dermatitis after surgery for Hirschsprung disease. Pediatr Dermatol. 1998 Jan-Feb;15(1):46-7. [PubMed]2. Fernández IS, Moreno C, Vano-Galvan S, Olasolo PJ. Pseudoverrucous irritant peristomal dermatitis with an histological pattern of nutritional deficiency dermatitis. Dermatol Online J. 2010 Sep 15;16(9):16. [PubMed]
3. Robson KJ, Maughan JA, Purcell SD, Petersen MJ, Haefner HK, Lowe L. J Am Acad Dermatol. 2006 Nov;55(5 Suppl):S74-80. Epub 2006 Sep 1. [PubMed]
4. Bergman B, Knutson F, Lincoln K, Lowhagen GB, Mobacken H, Wahlen P. Chronic papillomatous dermatitis as a peristomal complication in conduit urinary diversion. Scand J Urol Nephrol 1979;13:201-4.
5. Coppo P, Salomone R. Pseudoverrucous papules: an aspect of incontinence in children. J Eur Acad Dermatol Venereol. 2002 Jul;16(4):409-10. [PubMed]
6. Van L, Harting M, Rosen T. Jacquet erosive diaper dermatitis: a complication of adult urinary incontinence. Cutis. 2008 Jul;82(1):72-4. [PubMed]
7. Amiry SA, Pride HB, Tyler WB. Perianal pseudoverrucose papules and nodules mimicking condylomata acuminata and child sexual abuse. Cutis 2001;67:335-8. [PubMed]
8. Viola P, Viola M. Virgin olive oil as a fundamental nutritional component and skin protector. Clin Dermatol. 2009 Mar-Apr;27(2):159-65. [PubMed]
9. Budiyanto A, Ahmed NU, Wu A, Bito T, Nikaido O, Osawa T, Ueda M, Ichihashi M. Protective effect of topically applied olive oil against photocarcinogenesis following UVB exposure of mice. Carcinogenesis. 2000 Nov;21(11):2085-90. [PubMed]
© 2012 Dermatology Online Journal

