Juvenile rheumatoid arthritis (Juvenile chronic arthritis)
Published Web Location
https://doi.org/10.5070/D32cz320kfMain Content
Juvenile rheumatoid arthritis (Juvenile chronic arthritis)
Macrene Alexiades-Armenakas
Dermatology Online Journal 7(2): 19
History
This 31 year old woman presented with a five month history of a rash involving her medial upper arms. The patient presented to the Charles C. Harris Skin and Cancer Pavilion in October, 2000, with asymptomatic lesions on her arms of five months duration. She had been evaluated by a rheumatologist and a dermatologist who performed skin biopsies and laboratory studies. On review of systems, she reported morning stiffness in her hands, elbows, and knees, with improvement after 30 minutes. She also reported a ten pound weight loss since the birth of her son in April, 2000. She denied fever, malaise, headaches, visual difficulties, or other problems.
She was treated with plaquenil 200 mg. twice daily. At a one-month follow-up examination, the lesions resolved although her joint symptoms persisted.
Juvenile rheumatoid arthritis, which responded to hydroxychlorine, previously had been present at age 16.
Physical Examination
Flesh-colored, subcutaneous nodules ranging from 0.2 to 1.0-cm in diameter were distributed linearly along the biceps and tendons of the medial aspects of the upper arms. There was generalized fat wasting with zygomatic, temporal, and blood vessel prominence. There was also buccal fat pad atrophy. There were no mucosal lesions or pain on ocular movement.
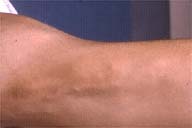 |  |
| Figure 1 | Figure 2 |
|---|
Laboratory Data
White-cell count 6.4 x 109/L, with 51% neutrophils, 27% lymphs, 8% monos, 12% eosinophils, and 1% basophils, erythrocyte sedimentation rate 11 mm/hr, rheumatoid factor <20 IU/ml, angiotensin converting enzyme 36.8 U/L, HLA-B27 negative, urinalysis normal, serum protein electrophoresis with a total protein 6.3 g/dl, albumin 3.27 g/dl, and normal globulin indices, antinuclear antibody negative, C- and P-ANCAs negative, anti-DNA Ab negative, and calcium 8.5 mg/dl.
Histopathology
There are palisades of histiocytes surrounding a central area of eosinophilic fibrinoid degeneration. The surrounding fat lobules are atrophic.
Diagnosis
Juvenile rheumatoid arthritis (Juvenile chronic arthritis)
Comment
Juvenile rheumatoid arthritis, known as juvenile chronic arthritis in Europe, is the most common rheumatic disease in children. Criteria for diagnosis include age of onset less than 16 years, disease duration greater than six weeks, arthritis, and exclusion of other forms of juvenile arthritis. Juvenile rheumatoid arthritis is subdivided into pauciarticular (less than five joints involved), polyarticular (five or greater joints involved), and systemic (arthritis, fever and rash) forms.
Skin manifestations of juvenile rheumatoid arthritis include amyloiosis which occurs in one to ten percent of all subtypes. Ninety percent of systemic-onset juvenile rheumatoid arthritis is characterized by an evanescent salmon-covered eruption that occurs on the trunk and thighs and which is concurrent with fever. The eruption may be elicited by scratching, ie, the Koebner phenomenon. A variant of juvenile rheumatoid arthritis with onset in young adulthood is adult Still's disease, which occurs at ages 16 to 35, is characterized by multi-system involvement and an evanescent, salmon-pink, macular and papular eruption, and is accompanied by fever. The eruption occurs on the trunk and proximal extremities and may be elicited by the Koebner phenomenon.
The skin manifestations of rheumatoid arthritis include rheumatoid nodules, rheumatoid papules, rheumatoid neutrophilic dermatitis, and vasculitis. Rheumatoid nodules are subcutaneous nodules that occur in 20 percent of rheumatoid patients with positive rheumatoid factors, and rarely in seronegative patients. The nodules generally correlate with disease activity. Rheumatoid nodulosis (multiple, widespread nodules) is a separate entity that occurs mostly in men with a low-grade fever and mild synovitis. Nodules develop most commonly on pressure areas, such as the elbows, joints, ischial and sacral prominences, along tendons, and the occiput. In general, nodules regress with treatment as the rheumatoid arthritis improves. Rheumatoid nodules in rheumatoid factor-negative patients have been reported but appear to be rare.
References
Kaye BR, et al. Rheumatoid nodules: review of the spectrum of associated conditions and proposal of a new classification, with a report of four seronegative cases. Am J Med 76:279, 1984Yamamoto T, et al. Skin manifestations associated with rheumatoid arthritis. J Dermatol 22:324, 1995
Nelson JL, Ostensen M. Pregnancy and rheumatoid arthritis. Rheum Dis Clin North Am 23:195, 1997
White PH. Juvenile chronic arthritis: clinical features. In: Klippel JH, Dieppe PA, eds. Rheumatology, 2nd Ed. Mosby, London, 1998
© 2001 Dermatology Online Journal

