A case of male invasive breast carcinoma presenting as a non-healing wound
Main Content
A case of male invasive breast carcinoma presenting as a non-healing wound
Amanda Cooper1 MD, Adrienne Schupbach1 MD, Lawrence Chan1,2,3 MD
Dermatology Online Journal 19 (2): 5
University of Illinois at Chicago, Departments of Dermatology1 and Microbiology/Immunology2, and Jesse Brown VA Medical Center, Section of Dermatology3, Chicago, IllinoisAbstract
Breast cancer in male patients accounts for less than 1 percent of malignancies in men. When compared to women, men with breast cancer are, on average, older, diagnosed at a more advanced stage, more likely to be hormone-receptor positive, less likely to overexpress HER2/neu, and have a lower overall survival. Owing to the paucity of data, male breast cancer treatment is typically guided by trials from female breast cancer. We report a case of invasive ductal carcinoma in a male patient with the initial presenting morphology of a non-healing chest wound. Interestingly, immunostaining identified positivity for estrogen receptor, progesterone receptor, and HER2/neu in the patient’s tumor. Although rare, breast carcinoma is an important consideration in any male with a breast mass, retracted nipple, or ulceration, as was seen in our patient.
Clinical summary
A 40-year-old man presented to the emergency department with a painful chest wound. He reported a recent syncopal event with resultant trauma to his right chest wall; he subsequently developed a draining wound. His past medical history was significant for morbid obesity, pulmonary embolism, and a cerebrovascular accident. Upon further questioning, the patient admitted to a gradual hardening of his right breast as well as significant weight loss (The patient reported approximately 100 lbs in past 2 months). The patient reported taking only loratadine at time of presentation. His family history was largely unknown other than possible breast cancer in his grandmother.
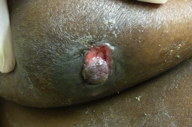
On physical examination, this morbidly obese male had diffuse induration (approximately 12 cm) of his right breast with a hyperpigmented, firm, tethered, tender plaque across the areola. The central 1.5 cm friable ulceration exhibited purulent drainage (Figure 1). Enlarged lymph nodes were palpated in the right axilla. Punch biopsy of the infiltrated plaque was performed.
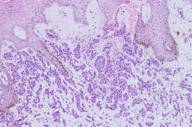
Histology of the right breast biopsy specimen revealed cords, strands and nests of atypical epithelial cells with ductal differentiation (Figure 2). The tumor was strongly positive for estrogen receptor, progesterone receptor, and HER-2/neu on immunohistochemistry.
Computed tomography (CT) of the chest, abdomen, and pelvis showed soft tissue infiltration in the right breast, but did not identify any additional lesions suggestive of metastases. However, the evaluation of the axilla was limited in this study. Total body bone scan did not reveal any bony abnormalities.
After evaluation by medical and surgical oncology, a treatment plan consisting of a modified radical mastectomy with lymph node dissection and subsequent chemotherapy, radiation therapy, and adjuvant hormonal therapy was proposed by the oncology team. Unfortunately, because of numerous social issues the patient missed several appointments with the medical and surgical oncology services and was lost to follow-up.
Discussion
Epidemiology
Male breast cancer (MBC) is exceedingly rare. Whereas breast cancer occurs in 1 in 8 women, only a small fraction of breast cancer cases occur in men. It is estimated that in 2011 there were only 2,140 new cases of MBC, compared to 230,480 new cases of female breast cancer (FBC) [1]. Men are, on average, diagnosed at a later age than women. In a large population-based study of breast cancer, the median age at diagnosis was 67 in men, compared to 62 in women [2]. Male breast cancer is slightly more prevalent in African American men compared to Caucasians [3]. Typically, men with breast cancer present with a mass, along with nipple discharge, nipple retraction, or skin ulceration, as was seen in our patient [4].
Risk factors
Hormone imbalance, occupational and environmental exposures and family history are risk factors for developing MBC. Alterations in the estrogen-testosterone balance (i.e., increase estrogen:testosterone ratio) incur risk in developing MBC. This risk is most strongly associated with Klinefelter syndrome (XXY) [4]. The absolute risk of MBC in Klinefelter syndrome reaches approximately 3 percent [5]. Decreased testosterone from testicular abnormalities such as cryptorchidism, orchitis, or orchidectomy are also associated with increased MBC, as are obesity and cirrhosis, which can lead to increased estrogen. Radiation, from environmental exposures or therapeutic intervention, has been associated with an increased risk of MBC. In addition, industrial workers who work in a hot environment have also been shown to have an increased risk of MBC, likely from reduced testosterone production related to heat-induced testicular failure [4]. Because the patient’s chest trauma occurred just days before he presented for his skin lesion, it is likely that this traumatic event was responsible for leading to the discovery of underlying tumor, rather than being an inciting factor for the tumor. The patient’s obesity is an identifiable risk factor for his development of MBC.
An estimated 10 percent of males with breast cancer have a genetic component [3]. BRCA1 and 2 are tumor-suppressor genes that act to regulate cell cycle checkpoints and DNA repair. BRCA2 mutation is the strongest genetic risk factor for breast cancer development in men, with a 7 percent lifetime risk in those carrying the mutation, a risk 80-100 times that of men without the mutation. Genetic testing is suggested in men and women who are diagnosed with breast cancer and have a family history of cancers seen with BRCA mutations (breast, ovarian, prostate, colorectal and pancreatic) [4].
Histopathology
The male breast contains primarily adipose tissue and stroma with ductal elements, but typically lacks the lobular tissue that allows for lactation in women [4]. This composition is reflected in the distribution of histological types of MBC, with ductal carcinoma by far the most prevalent MBC. A larger study classified 93.7 percent of MBC as ductal or unclassified carcinomas, compared to 83.6 percent in women. Lobular carcinomas are rare in men, comprising only 1.5 percent of MBC, compared to 11.8 percent of FBC. The remaining minority of MBC cases show papillary, medullary, or mucinous histology [2].
Hormone status
Alterations in hormone receptors and HER2/neu signaling pathways allow cancer cell proliferation and survival [6]. Men have been shown to have a significantly higher incidence of hormone receptor positivity with 91 percent estrogen receptor positive and 81 percent progesterone receptor positive, compared to 76 percent and 67 percent, respectively, in women in one study [2]. Unlike hormone status, Her-2/neu is less likely to be overexpressed in cases of MBC than in FBC [7]. In one study of 58 MBC and 202 FBC, 1.7 percent of MBC had overexpression of Her-2, compared to 27 percent of FBC [8].
Prognosis
Although the studies of MBC are limited, the overall survival in males with breast cancer appears to be lower than in their female counterparts. This is attributed to an older age and later stage at diagnosis. In a database including 2,537 cases of MBC and 383,146 FMB, cases of MBC were, on average, diagnosed at a more advanced stage with regional lymph node involvement in 37.7 percent of men compared to 29.2 percent in women. Distant metastases were present in 6.9 percent of men compared to 5.6 percent of women [2]. Other reports show an even higher percentage; approximately 50 percent of male patients with breast cancer have nodal involvement at diagnosis [3, 4]. Women are diagnosed with smaller lesions and at earlier stages likely because of screening mammography [2].
Although men have a high rate of hormone receptor positivity, unfortunately, the more favorable prognosis seen with hormone receptor positivity in women has not been shown in men [2, 9]. This poorer prognosis despite higher hormone receptor positivity and low histologic grade, is again attributed to the more advanced stage at presentation [10]. Unfortunately, our patient was lost to follow-up and therefore was not able to provide us the data on his prognosis.
Management
Treatment of early-stage disease is similar in men and women [7]. Modified radical or simple mastectomy have replaced radical mastectomy as the treatment of choice for MBC. Lumpectomy has been show to have poorer outcomes. In addition to mastectomy, axillary lymph node dissection is a surgical choice and was planned in our patient. Sentinel lymph node biopsy is another possible option with lower complication rate compared to axillary dissection [4]. Because of the rarity of this disease, there is limited data on treatment; therefore, following treatment guidelines for FBC is commonly recommended [7]. Although the effect on survival is not known, radiation therapy is often used because it has been shown to prevent local recurrence [4]. Radiation following mastectomy is more common in men compared to women, possibly owing to the fact that men are more likely to have cutaneous involvement. Similar to treatment of women, men with a higher risk of recurrence and mortality are treated with an adjuvant chemotherapy regimen. The use of adjuvant chemotherapy is well-established in female breast cancer and the benefit is suggested in smaller studies in men, so similar guidelines are followed in MBC. Because hormone-receptor positivity is high in men, the estrogen receptor antagonist, tamoxifen, is an important treatment consideration. Case series have shown a reduced risk of recurrence and death in men treated with tamoxifen [7].
References
1. Siegel R, Ward E, Brawley O, Jemal A. Cancer statistics, 2011: the impact of eliminating socioeconomic and racial disparities on premature cancer deaths. CA Cancer J Clin. 2011; 61(4): 212-236. [PubMed]2. Giordano SH, Cohen DS, Buzdar AU, Perkins G, Hortobagyi GN. Breast carcinoma in men: a population-based study. Cancer. 2004; 101(1): 51-57. [PubMed]
3. Korde LA, Zujewski JA, Kamin L, Giordano S, Domchek S, Anderson WF, Bartlett JM, Gelmon K, Nahleh Z, Bergh J, Cutuli B, Prudery G, McCaskill-Stevens W, Gralow J, Hortobagyi G, Cardoso F. Multidisciplinary meeting on male breast cancer: summary and research recommendations. J Clin Oncol. 2010; 28(12): 2114-2122. [PubMed]
4. Johansen Taber KA, Morisy LR, Osbahr AJ 3rd, Dickinson BD. Male breast cancer: risk factors, diagnosis, and management. Oncol Rep. 2010; 24(5): 1115-1120. [PubMed]
5. Niewoehner CB, Schorer AE. Gynaecomastia and breast cancer in men. BMJ. 2008; 336(7646): 709-713. [PubMed]
6. Gutierrez C, Schiff R. HER2: biology, detection, and clinical implications. Arch Pathol Lab Med. 2011; 135(1): 55-62. [PubMed]
7. Giordano SH. A review of the diagnosis and management of male breast cancer. Oncologist. 2005; 10(7): 471-479. [PubMed]
8. Bloom KJ, Govil H, Gattuso P, Reddy V, Francescatti D. Status of HER-2 in male and female breast carcinoma. Am J Surg. 2001; 182(4): 389-392. [PubMed]
9. Muir D, Kanthan R, Kanthan SC. Male versus female breast cancers. A population-based comparative immunohistochemical analysis. Arch Pathol Lab Med. 2003; 127(1): 36-41. [PubMed]
10. Joshi MG, Lee AK, Loda M, Camus MG, Pedersen C, Heatley GJ, Hughes KS. Male breast carcinoma: an evaluation of prognostic factors contributing to a poorer outcome. Cancer. 1996; 77(3): 490-498. [PubMed]
© 2013 Dermatology Online Journal