Cutaneous metastasis of gastric adenocarcinoma: An exuberant and unusual clinical presentation
Published Web Location
https://doi.org/10.5070/D31xs1g51pMain Content
Cutaneous metastasis of gastric adenocarcinoma: An exuberant and unusual clinical presentation
Marcus Henrique de S B Xavier MD, Tadeu de Rezende Vergueiro MD, Enoi Guedes Vilar PhD, Jane Marcy N Pinto PhD, Maria Cláudia
A Issa MD, Gabriela Blatt Pereira MD, Ana Paula G Carocha MD
Dermatology Online Journal 14 (11): 8
Universidade Federal Fluminense, Hospital Universitário Antônio Pedro - Serviço de Dermatologia. Niterói, Rio de janeiro -
Brasil. marcus_hx@hotmail.comAbstract
There are different types of skin changes associated with internal malignancy. One type is the skin involvement as a result of cutaneous metastasis from an internal tumor. The skin is an uncommon site for distant metastasis; when it is present the most common sources are breast, lung, and colon. Metastasis generally occurs after an internal malignancy had been discovered and signifies disseminated disease with a poor prognosis. We report an exuberant and rare case of cutaneous metastasis from gastric adenocarcinoma as the first sign of this serious visceral cancer.
Clinical Synopsis
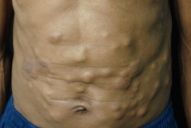
A 48-year-old male Brazilian rural worker presented with a 5-month history of development of asymptomatic cutaneous nodules on his lower abdomen. Progression of involvement to the thorax, left side, arms, and face occured. His medical history was unremarkable, except by a non-measured weight loss and a 30-year history of cigarette addiction (1 pack daily). He denied any familial cases of visceral cancer.
 |  |
| Figure 1 | Figure 2 |
|---|
 |  |
| Figure 3 | Figure 4 |
|---|
 |
| Figure 5 |
|---|
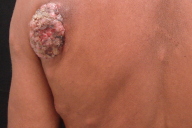
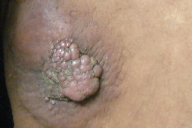
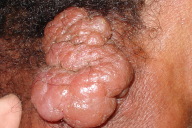
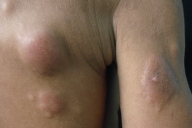
On physical examination, the patient appeared cachectic, and exhibited multiple firm to hard subcutaneous nodules located mainly on the lower abdomen (Fig. 1). Most nodules showed normal overlying skin, but some nodules appeared erythematous. On his left scapular area and left thigh there were vegetative tumors (Figs. 2 & 3). A tumor on the neck had infiltrated the underlying dermis (Fig. 4). There were red infiltrated plaques on the posterior aspect of the right arm (Fig. 5). There was an enlarged and firm mass in his left axillary region. Neither intra-abdominal masses nor organomegaly were palpated.
Laboratory tests revealed elevations in alkalin phosphates (364 U/L) and normocytic-normochromic anemia (Hg 12g/dL). A chest X-ray was normal.
 |  |
| Figure 6 | Figure 7 |
|---|
 |  |
| Figure 8 | Figure 9 |
|---|
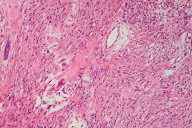
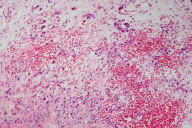
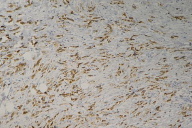
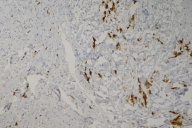
A skin biopsy revealed infiltrating neoplastic cells dispersed in a dense fibrous stroma (Fig. 6); in the dermis and subcutaneous tissue there was the appearance of some signet ring cell formations (Fig. 7). Immunohistochemical studies were positive for antibodies anti- epithelial membrane antigen (EMA), carcinoembryonic antigen (CEA), anti-cytokeratin antibodies (A1E and A3E), and thyroid transcription factor 1 (TTF-1) (Figs. 8, 9, 10, & 11). Other antigens, such as anti S-100, CK20, CK7, HHF-35, and AML, were negative. Metastatic adenocarcinoma was diagnosed and investigation for a primary tumor of the lungs or gastrointestinal systems was undertaken.
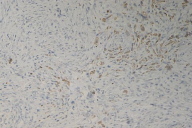 | 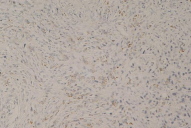 |
| Figure 10 | Figure 11 |
|---|
Thorax computed tomography showed pulmonary nodules. In the abdominal computed tomography scan there was pre-aortic ganglia enlargement and lytic lesions were noted in the lumbar spinal column. When the patient underwent a gastric endoscopy, a rough infiltrative ulcer, about 3 cm in diameter, originating from the angular notch was revealed. The ulcer biopsy showed a poorly differentiated gastric adenocarcinoma with signet ring cells.
The patient was diagnosed with gastric adenocarcinoma stage IV (T4N3M1). Although the patient has been receiving systemic chemotherapy with 5-Fluorouracil, Leucovorin and Etoposide, the cutaneous metastasis has not showed any improvement. In spite of the treatment new lesions have been appearing over 7 months of follow-up and his general health has deteriorated.
Discussion
The skin is an uncommon site for distant metastases (with a frequency ranging from 0.7% to 10.4%, depending on the series), which most commonly occur after the identification of a primary cancer [1, 2]. More than 60 percent of skin metastases are adenocarcinomas, usually arising in the breast, lung, or large intestine [3]. In males, primary solid tumors that most often metastasize to the skin are carcinomas of the lung (24%), carcinomas of the colon (19%), and melanomas (13%). In women, breast cancer is the most frequent (69%), followed by colon cancer (9%) and melanoma (5%) [3, 4]. Gastric cancer has been reported in only 6 percent of all skin metastases in males and 1 percent in females [2].
According to Schwartz et al. cutaneous metastatic disease as the presenting sign of internal cancer is most common with cancer of the lung, kidney, and ovary [3]. Nevertheless, in a recent review, cutaneous metastases have been seen as an initial sign of cancer in 20 of 92 cases (22%) [5].
Metastatic dissemination may take place through the lymphatics or the blood stream. In carcinomas of the breast and oral cavity, metastases reach the skin largely through lymphatic channels and are often located on the overlying skin. In contrast, cutaneous metastatic lesions from other carcinomas are often the result of hematogenous dissemination and may appear in any area of the skin [6]. Gastric cancer can spread locally to adjuvant structures and also develop distant metastatic deposits mainly by hematogenous spread. It usually metastasizes to the liver, peritoneal cavity, and regional lymph nodes more often than to the skin [7]. Although the most common location of cutaneous metastasis from gastric cancer is the abdominal wall, other skin sites such as head, neck, axillae, thorax, and limbs have been described [2, 8].
As with other visceral cancers, cutaneous metastasis from gastric adenocarcinoma usually occurs as solitary or multiple nonspecific, painless dermal or subcutaneous nodules with an intact overlying epidermis [9]. In clinical presentations, such as the famous Sister Mary Joseph nodules, umbilical metastases are most commonly found in advanced-stage adenocarcinomas of the upper digestive tract and ovary [10]. There are reports of cutaneous metastasis from gastric cancer appearing in a zosteriform pattern [11] or an erysipelas-like pattern called carcinoma erysipelatoides [12]. Other metastases can resemble alopecic areas [3], allergic contact dermatitis, photodermatoses [13], red plaques [14] and scars (en cuirasse) [5]. We have not found any other reports with vegetating tumors, as seen in our case. Moreover, generalized cutaneous metastases, as in this case presentation, are relatively infrequent [15, 16].
Once skin involvement presents, the site of primary tumor, if unknown, may be diagnosed by histopathologic study. Microscopic study usually shows the presence of adenocarcinomas with different degrees of differentiation. They can occasionally be difficult to differentiate from primary skin adenocarcinomas, such as mucinous eccrine adenocarcinoma or apocrine adenocarcinoma; diagnosis may require immunoperoxidase study [7].
The appearance of linear dissection of neoplastic cells in the collagen bundles in the skin is typical of breast metastases, but prostate, stomach, pancreas, and small cell carcinoma may also show this pattern. Signet-ring cells can be found in some metastases of mammary origin, but they are more usual in those of gastric origin [17]. Immunohistochemical studies are often included to help obtain the correct diagnosis [18].
Cutaneous metastasis is still a poor prognostic sign. The general survival after the diagnosis of skin metastasis drops below one year (average 11.4 weeks with a range of 2 to 34 weeks) and deteriorates further with multiple cutaneous metastases [6, 19].
The treatment of skin metastases depends on their size and location. Surgical excision followed by radiotherapy may occasionally control the disease leading to longer survival. Extensive lesions or successive recurrences are not usually amenable to curative resection; systemic chemotherapy is the most commonly used treatment [6, 20].
Acknowledgement: We would like to thank the language review by Lilian Bonilha Morais.
References
1. Rosen T. Cutaneous metastases. Med Clin North Am. 1980 Sep;64(5):885-900. [PubMed]2. Lookingbill DP, Spangler N, Helm KF. Cutaneous metastases in patients with metastatic carcinoma: a retrospective study of 4020 patients. J Am Acad Dermatol. 1993; 29(2 Pt 1):228-36. [PubMed]
3. Brownstein MH, Helwig EB. Patterns of cutaneous metastasis. Arch Dermatol. 1972 Jun;105(6):862-8. [PubMed]
4. Schwartz RA. Cutaneous metastatic disease. J Am Acad Dermatol. 1995; 33(2 Pt 1):161-82. [PubMed]
5. Nashan D, Müller ML, Braun-Falco M, Reichenberger S, Szeimies RM, Bruckner-Tuderman L. Cutaneous metastases of visceral tumours: a review. J Cancer Res Clin Oncol. 2008 Jun 17. [PubMed]
6. Johnson WC. Metastatic carcinoma of the skin: incidence and dissemination. In: Elder DE, Elenitsas R, Johnson BL, Murphy GF, editors. Lever's Histopathology of the skin. 9th ed. Lippincott Williams & Wilkins; 2005. p1149-1157.
7. Esaki Y, Hirayama R, Hirokawa K. A comparison of patterns of metastasis in gastric cancer by histologic type and age. Cancer. 1990 May 1;65(9):2086-90. [PubMed]
8. López-Tarruella Cobo S, Moreno Antón F, Sastre J, López García-Asenjo JA, Torres A, Díaz-Rubio E. Cuirasse skin metastases secondary to gastric adenocarcinoma. Clin Transl Oncol. 2005 Jun;7(5):213-5. [PubMed]
9. Barreto G, Shrikhande S, Shukla P. Cutaneous metastasis of gastric signet ring cell carcinoma masquerading as allergic contact dermatitis. J Eur Acad Dermatol Venereol. 2007 Jan;21(1):123-4. [PubMed]
10. Fill S, Taran A, Schulz HU, Kahl S, Kalinski T, Smith B, Costa SD. Sister Mary Joseph's nodule as the first sign of pregnancy-associated gastric cancer: a case report. World J Gastroenterol. 2008;14(6):951-3. [PubMed]
11. Kikuchi Y, Matsuyama A, Nomura K. Zosteriform metastatic skin cancer: report of three cases and review of the literature. Dermatology. 2001;202(4):336-8. [PubMed]
12. Acikalin MF, Vardareli E, Tel N, Saricam T, Urer S. Erysipelas-like cutaneous metastasis from gastric signet ring cell carcinoma. J Eur Acad Dermatol Venereol. 2005 Sep;19(5):642-3. [PubMed]
13. Ahn SJ, Oh SH, Chang SE, Jeung YI, Lee MW, Choi JH, Moon KC, Koh JK. Cutaneous metastasis of gastric signet ring cell carcinoma masquerading as allergic contact dermatitis. J Eur Acad Dermatol Venereol. 2007 Jan;21(1):123-4. [PubMed]
14. Lifshitz OH, Berlin JM, Taylor JS, Bergfeld WF. Metastatic gastric adenocarcinoma presenting as an enlarging plaque on the scalp. Cutis. 2005 Sep;76(3):194-6. [PubMed]
15. Sood A, Midha V, Sekhon JS, Sidhu SS. Generalized cutaneous metastases from carcinoma stomach. Am J Gastroenterol. 1998 Sep;93(9):1601. [PubMed]
16. Ozakyol AH, Sariçam T, Paşaoğlu O. A rare entity: cutaneous metastasis from gastric adenocarcinoma. Am J Gastroenterol. 1999 Apr;94(4):1118-9. [PubMed]
17. Inoue Y, Johno M, Kayashima K, Kako H, Ogawa M, Ono T. Metastatic skin cancer; a case with signet ring cell histology. Br J Dermatol. 1996 Oct;135(4):634-7. [PubMed]
18. Lee MJ, Lee HS, Kim WH, Choi Y, Yang M. Expression of mucins and cytokeratins in primary carcinomas of the digestive system. Mod Pathol. 2003 May;16(5):403-10. [PubMed]
19. Bordin GM, Weitzner S. Cutaneous metastases as a manifestation of internal carcinoma: diagnostic and prognostic significance. Am Surg. 1972 Nov;38(11):629-34. [PubMed]
20. Michiwa Y, Earashi M, Kobayashi H, Matsuki N. Cutaneous metastases from gastric adenocarcinoma treated with combination chemotherapy producing complete response with long survival. J Exp Clin Cancer Res. 2001 Jun;20(2):297-9. [PubMed]
© 2008 Dermatology Online Journal

