Linear atrophoderma of Moulin localized to the neck
Published Web Location
https://doi.org/10.5070/D31w2688c0Main Content
Linear atrophoderma of Moulin localized to the neck
Roberto Cecchi MD, Laura Bartoli MD, Luigi Brunetti MD, Mario Pavesi MD
Dermatology Online Journal 14 (6): 12
Department of Dermatology, Spedali Riuniti, Pistoia, Italy. r.cecchi@usl3.toscana.itAbstract
Linear atrophoderma of Moulin (LAM) is a rare and distinct skin condition characterized by unilateral, hyperpigmented and atrophic band-like skin lesions following the lines of Blaschko. Usually the disease begins in childhood or adolescence on the trunk or limbs, with no preceding inflammation or subsequent sclerodermatous changes. Approximately 25 cases have been reported in the English language literature. We describe a case of LAM occurring in a 9-year-old Peruvian boy with exclusive involvement of the neck. To our knowledge, this is the first report of LAM with this unusual localization.
Introduction
Linear atrophoderma of Moulin (LAM) was originally recognized as a distinct clinical condition by Moulin et al. in 1992 [1]. It is characterized by hyperpigmented and atrophic band-like skin lesions, that appear during childhood or adolescence on the trunk or the limbs, following the lines of Blaschko. Histopathology reveals a moderate basal layer hyperpigmentation with no epidermal or dermal pathologic findings. In general, the disease is self-limited. It appears without any preceding inflammation and there is no subsequent induration or sclerodermatous change. Including the original five cases, approximately 25 cases of LAM have been reported in the English language literature. We describe another patient with LAM, exclusively confined to the neck.
Clinical synopsis
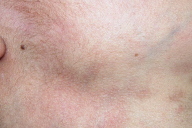
A 9-year-old boy immigrant from Peru was seen in April, 2006, with a 1-year history of asymptomatic, hyperpigmented plaques unilaterally distributed on the right aspect of his neck. The patient denied any local trauma, injection or drug intake. His past medical history was unremarkable, and there was no family history of pigmentary skin disorders. Physical examination revealed multiple, hyperpigmented, and slightly depressed plaques in a band-like arrangement on the right aspect of the neck, under the jaw-line (Fig. 1). These lesions were oval or linear shaped, light brown in color, and appeared to follow the lines of Blaschko. No area of induration was palpable. There had been no prededing inflammation and symptoms such as pruritus and pain were absent.
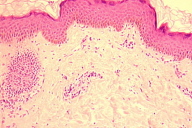
A skin biopsy showed a normal epidermis with moderate, diffuse hyperpigmentation of the basal layer. A perivascular lymphocytic infiltrate was noted in the dermis, without any other pathologic feature (Fig. 2). A diagnosis of LAM was established based on clinical and histopathologic findings.
During a 1-year follow-up the disease has remained fixed and unmodified.
Discussion
Since the original 1992 publication, the diagnosis of LAM has been extended to include cases displaying disparate clinical and histologic findings, including preceding inflammation, collagen sclerosis, teleangiectases, and psoriasiform changes. Browne et al. [2] reported a case with antecedent inflammation in a 16-year-old man and proposed that LAM may occasionally be preceded by an inflammatory stage that ultimately evolves into hyperpigmentation and atrophy. Therefore, they suggested that there are 2 variants of the same disease: an inflammatory and a non-inflammatory LAM [2].
Later, Utikal et al. [3] described 2 patients with prominent teleangiectatic erythema within lesions of linear atrophoderma and argued that these cases may represent a novel variety of LAM.
Danarti et al. [4] reported 4 new cases of LAM and reviewed another 15 published cases published, including 2 originally described as atrophoderma of Pasini and Pierini and morphea, respectively. The presence of a hyperpigmented atrophoderma, strictly following the lines of Blaschko was considered to be the key finding for the diagnosis of LAM [4].
Conversely, Ang et al. [5] in a recent letter believe that the diagnosis of LAM should exclusively be reserved to the cases that fulfil the criteria originally proposed by Moulin. In particular, they consider it unlikely that the cases involving alterations of the collagen fibers, such as thickening or sclerosis, represent a different stage of LAM. Therefore, the cases originally diagnosed as atrophoderma of Pasini and Pierini and morphea following Blaschko lines should remain as such [5].
Our case matches the clinical-pathologic findings of typical LAM, without antecedent inflammation or subsequent induration or scleroderma. Remarkably, the plaques were unilaterally distributed on the right side of the neck and this localization has never been reported. On the lateral aspect of the neck the lines of Blaschko run in parallel downward from the cranial-lateral areas to the anterior midline [6].
Linear atrophoderma of Moulin should be distinguished from other pigmentary dermatoses that follow the lines of Blaschko, such as incontinentia pigmenti or focal dermal hypoplasia [4]. Linear and whorled nevoid hypermelanosis shows hyperpigmented streaks and whorls that follow the Blaschko lines [7]. However, there is no associated atrophy [2]. Finally, atrophoderma of Pasini and Pierini and morphea should also be considered in the differential diagnosis. Atrophoderma of Pasini and Pierini exhibits hyperpigmented and atrophic plaques, which do not follow the lines of Blaschko; linear scleroderma can be excluded by the presence of sclerosis [4].
No satisfactory treatment modalities for LAM are currently available. High dose penicillin G and topical corticosteroids did not prove to be effective in a few cases [4, 8], but potassium aminobenzoate was claimed to induce an early stabilization of the skin lesions in another case [9]. However, the disease is self-limited and the prognosis is favorable. Camouflage cosmetics may be useful to reduce the cosmetic abnormality [8, 10].
The etiology of LAM remains unknown. It has been hypothesized that the disorder may reflect the mosaicism of a predisposing gene. A post-zygotic mutation may result in an aberrant cell clone, which becomes manifest along the Blaschko lines later in life, giving rise to LAM [4].
References
1. Moulin G, Hill MP, Guillaud V, Barrut D, Chevallier J, Thomas L. [Acquired atrophic pigmented band-like lesions following Blaschko's lines] Ann Dermatol Venereol. 1992; 119 (10): 729-36. Review. French. PubMed.2. Browne C, Fisher BK. Atrophoderma of Moulin with preceding inflammation. Int J Dermatol. 2000 Nov; 39(11): 850-2. PubMed.
3. Utikal J, Keil D, Klemke CD, Bayerl C, Goerdt S. Predominant teleangiectatic erythema in linear atrophoderma of Moulin: novel variant or separate entity? Dermatology. 2003;207(3): 310-5. Review. PubMed.
4. Danarti R, Bittar M, Happle R, Konig A. Linear atrophoderma of Moulin: postulation of mosaicism of a predisposing gene. J Am Acad Dermatol. 2003 Sep; 49(3): 492-8. Review. PubMed.
5. Ang GC, Lee JB. Linear atrophoderma of Moulin: is it a single disease? J Am Acad Dermatol. 2005 May; 52(5): 923-4. PubMed.
6. Happle R, Assim A. The lines of Blaschko on the head and neck. J Am Acad Dermatol. 2001 Apr; 44(4): 612-5. PubMed.
7. Kalter DC, Griffiths WA, Atherton DJ. Linear and whorled nevoid hypermelanosis. J Am Acad Dermatol. 1988 Dec; 19(6): 1037-44. PubMed.
8. Baumann L, Happle R, Plewig G, Schirren CG. [Atrophodermia linearis Moulin. A new disease picture, following the Blaschko lines] Hautarzt. 1994 Apr; 45(4): 231-6. German. PubMed.
9. Artola Igarza JL, Sanchez Conejo-Mir J, Corbi Llopis MR, Linares Barrios M, Casals Andreu M, Navarrete Ortega M. Linear atrophoderma of Moulin: treatment with Potaba. Dermatology. 1996; 193(4): 345-7. Review. PubMed.
10. Wollenberg A, Baumann L, Plewig G. Linear atrophoderma of Moulin: a disease which follows Blaschko's lines. Br J Dermatol. 1996 Aug; 135(2): 277-9. Review. PubMed
© 2008 Dermatology Online Journal