Exogenous insulin-derived acanthosis nigricans: Could it be a cause of increased insulin requirement?
Published Web Location
https://doi.org/10.5070/D31w06w6rgMain Content
Exogenous insulin-derived acanthosis nigricans: Could it be a cause of increased insulin requirement?
Mandeep Dhingra MD, Geeta Garg, Monica Gupta, Ujjwal Khurana, Gurvinder Pal Thami
Dermatology Online Journal 19 (1): 9
Government Medical College and Hospital, Chandigarh, IndiaAbstract
Acanthosis nigricans is a cutaneous manifestation of insulin resistance. We herein present a case of localized acanthosis nigricans over the abdomen in a 14-year-old boy with type 1 diabetes mellitus. The acanthosis nigricans appeared secondary to repeated insulin injection over same site. After advising the patient about rotating the injection site there was better disease control along with drop in insulin requirement and a significant reduction in the size of the lesion.
Case report
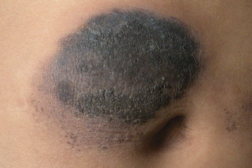
A 14-year-old male having a 4-year history of type 1 diabetes mellitus presented to the outpatient department for control of his raised blood sugar levels. He was receiving insulin (human biphasic isophane insulin 30/70, 30 percent human regular insulin, 70 percent human isophane insulin, recombinant DNA origin) in doses of 55-30 IU before meals. His fasting and postprandial blood sugars were 290 mg/dl and 390 mg/dl respectively. HbA1c value was 11.5 percent. Urinary ketones were negative. On physical examination a single well-defined, elevated, non-tender plaque approximately 6 × 4.5 cm over the right side of the abdomen just above the umbilicus was noticed. The surface of the plaque was hyperpigmented and hypertrophic with a verrucous texture (Figure 1). The neck, axillae, and groin were unremarkable. The patient recalled that the lesion had started as a raised pigmented area 3-years prior. It gradually increased in size and thickness and acquired a velvety texture with hyperpigmentation over its surface. Although the patient had been advised to rotate his injection site, he had been injecting insulin exclusively into this site for the last four years. He continued to inject into the thickened skin despite repeated advice because he felt less pain over the hypertrophied site.
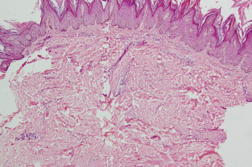
The histopathologic evaluation revealed marked basket-weave hyperkeratosis, papillomatosis, and acanthosis. The dermis was thickened with increased collagenization along with a mild superficial and deep perivascular lymphocytic infiltrate (Figure 2). Our patient was diagnosed as having exogenous insulin-derived acanthosis nigricans and advised to stop injecting insulin into the area of his plaque and start rotating his injection site regularly. Two weeks later, diabetic control had improved with amelioration of the symptoms of polyuria and polydipsia. The insulin requirement had come down to 30-25 IU (human biphasic isophane insulin). At a 3 month follow up the HbA1c levels came down to 8.5 percent. The plaque had also resolved slightly from the edges along with decreased pigmentation and thickness.
Acanthosis nigricans presents as asymptomatic tan to dark brown symmetrical, velvety, poorly marginated plaques with accentuation of skin markings, usually on the posterior neck and intertriginous areas. It is often a cutaneous manifestation of insulin resistance [1]. Localized acanthosis nigricans at the site of repeated insulin injections has been reported previously in the literature [2-6]. It has been suggested that it develops through similar mechanisms that are widely held true for acanthosis nigricans, namely the abnormal proliferation of keratinocytes and fibroblasts caused by stimulation of insulin-like growth factor (IGF) receptors by a localized and sustained high tissue concentration of insulin. This produces keratinocyte and fibroblast proliferation resulting in thickened and hyperkeratotic skin. Also the regression of the plaque on changing the injection site was compatible with this hypothesis. Histopathologically, these lesions demonstrate hyperkeratosis, papillomatosis, acanthosis, and a thickened dermis.
In our case there was a drop in insulin requirement after educating the patient about rotating the injection sites regularly. Similar findings have been reported recently and the authors proposed that this may relate to improper absorption from the acanthotic skin region [6]. Hence, patient education about rotating injection sites is of great importance to avoid such complications.
References
1. Hermanns-Lê T, Scheen A, Piérard GE. Acanthosis nigricans associated with insulin resistance: pathophysiology and management. Am J Clin Dermatol. 2004;5(3):199-203. [PubMed]2. Erickson L, Lipschutz DE, Wrigley W, et al. A peculiar cutaneous reaction to repeated injections of insulin. JAMA 1969 Aug 11;209(6):934-5. [PubMed]
3. Fleming MG, Simon SI. Cutaneous insulin reaction resembling acanthosis nigricans. Arch Dermatol 1986;122:1054-6.
4. Mailler-Savage EA, Adams BB. Exogenous insulin-derived Acanthosis nigricans. Arch Dermatol. 1986 Sep;122(9):1054-6. [PubMed]
5. Pachón Burgos A, Chan Aguilar MP. Visual vignette. Hyperpigmented hyperkeratotic cutaneous insulin reaction that resembles acanthosis nigricans with lipohypertrophy. Endocr Pract. 2008 May-Jun;14(4):514. [PubMed]
6. Buzási K, Sápi Z, Jermendy G. Acanthosis nigricans as a local cutaneous side effect of repeated human insulin injections. Diabetes Res Clin Pract. 2011 Nov;94(2):e34-6. Epub 2011 Aug 11. [PubMed]
© 2013 Dermatology Online Journal