Cutis verticis gyrata
Published Web Location
https://doi.org/10.5070/D31dp6w6ksMain Content
Cutis verticis gyrata
Nathalie Q Nguyen MD
Dermatology Online Journal 9(4): 32
From the Ronald O. Perelman Department of Dermatology, New York University
Abstract
An 82-year-old man had deep, linear skin folds on the scalp. The patient did not have a history of neuropsychiatric disorders and was generally in good health except for diabetes mellitus, hypertension, and benign positional vertigo. Cutis verticis gyrata is a term used to describe the appearance of deep, linear skin folds in the scalp. Primary and secondary types of this condition exist. No treatment is typically needed, although surgical modalities may be beneficial for severely disfiguring types.
Clinical summary
History.—An 82-year-old man was noted to have scalp folds for many years. During a routine examination at the New York Harborview Health Care System, an patient with a history of squamous-cell carcinoma was found to have multiple folds on his scalp. When these particular folds were pointed out to the patient, he replied that his scalp had appeared unchanged to him for years. He denied having any family members with a similar condition. His medical history includes diabetes mellitus, hypertension, and benign positional vertigo. He denied psychiatric or neurologic illnesses.
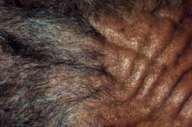
Physical examination.—Deep, linear folds in an antero-posterior direction were present on the scalp. The folds were more prominent over the right frontal scalp than they were over the left. There was no alopecia and no difference in the distribution of hair over the folds and in the ridges. The furrows did not extend onto the posterior neck. However, the horizontal skin folds on his forehead did appear more prominent. The patient did not have coarse facial features or clubbing of his fingers.
|
| Figure 1 |
|---|
Laboratory data.—The fasting serum glucose was 140 mg/dl, and the hemoglobin A1C was 8.1 percent. The complete blood count, kidney and liver panels, and cholesterol were normal.
Histopathology.—None.
Diagnosis.—Cutis verticis gyrata.
Comment
Cutis verticis gyrata (CVG) is a term that refers to a pattern of redundant skin on the scalp that exhibits deep furrows and convolutions [1]. The hypertrophy and folding of the skin produces a gyrate appearance. The deep lines in the scalp typically are in an anteroposterior direction but may also be in a horizontal direction.
Primary CVG occurs predominantly in men and has often been associated with mental retardation or neuropsychiatric disease, such as seizures and schizophrenia [1, 2]. The onset is typically after puberty, and the folds are usually symmetrical. The histopathology can be normal or contain thick connective tissue with some hypertrophy or hyperplasia of adnexal structures [1]. Secondary CVG has been linked to local inflammatory skin conditions, such as eczema and psoriasis and to systemic illnesses, such as amyloidosis, syphilis, myxedema, Ehlers-Danlos syndrome, acanthosis nigricans, and insulin-resistance syndrome [3]. The appearance of the skin folds in secondary CVG may be more asymmetrical and can appear at any age. Acromegaly and pachyodermoperiostosis (idioathic hypertrophic osteoarthorpathy) are two conditions that often present with secondary CVG [3]. Chromosomal abnormalities such as Turner syndrome, Klinefelter syndrome, and fragile X have also been associated with CVG. The only known familial form of CVG occurs in association with primary pachyodermoperiostosis.
Although CVG may be disfiguring, the process is essentially benign and no intervention is required. Surgical repair may be implemented if desired, and the type of surgery depends on the size and location of the lesions, the underlying disorder, and the wishes of the patient. Surgical modalities range from simple excisions to tissue expansion and skin grafts for those cases with more extensive scalp involvement [3].
References
1. Diven D, et al. Cutis verticis gyrata. Int J Dermatol 1991;30:710.2. Chang GY. Cutis verticis gyrata: Underrecognized neurocutaneous syndrome. Neurology 1996;47:573.
3. Synder MC, et al. Congenital primary cutis verticis gyrata. Plastic Reconstr Surg 2002;110:818.
© 2003 Dermatology Online Journal

