Central centrifugal cicatricial alopecia: Superimposed tinea capitis as the etiology of chronic scalp pruritus
Published Web Location
https://doi.org/10.5070/D30vq7c5jmMain Content
Central centrifugal cicatricial alopecia: Superimposed tinea capitis as the etiology of chronic scalp pruritus
Charles Chiang MD1, Vera Price MD1, Paradi Mirmirani MD2
Dermatology Online Journal 14 (11): 3
1. Department of Dermatology, University of California San Francisco, San Francisco, CA. chiangc@derm.ucsf.edu2. Department of Dermatology, University of California San Francisco, San Francisco, CA. Department of Dermatology, Case Western Reserve University, Cleveland, OH. Department of Dermatology, The Permanente Medical Group, Vallejo, CA.
Abstract
We discuss a patient with central centrifugal cicatricial alopecia (CCCA) who developed severe scalp pruritus that was initially attributed to the cicatricial alopecia and ultimately diagnosed as tinea capitis. The rarity of severe pruritus in CCCA should prompt a search for a fungal infection in these patients.
Case description
A 63-year-old African American woman with a known, biopsy-proven diagnosis of CCCA (Fig. 1), presented with severe scalp itching of 2 months duration. In the past, her itching had been mild and easily controlled with antiseborrheic shampoos. Her past medical history included rheumatoid arthritis for which she was taking prednisone 5mg orally daily and methotrexate 15mg orally weekly. On physical examination, there was a 6cm patch of scarring alopecia at the scalp vertex which radiated centrifugally to the frontal and temporal scalp. Along the frontal scalp the patient also had decreased hair density and mild perifollicular scale (Fig. 2). The patient's symptoms and physical findings were attributed to a flare of CCCA. Her topical treatments included fluocinolone oil daily, clobetasol solution daily, and intralesional triamcinolone; her systemic medications were changed from hydroxychloroquine to minocycline 100mg daily. On a follow-up visit 6 weeks later, the appearance of her scalp was improved. However, her severe pruritus persisted.
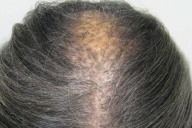 | 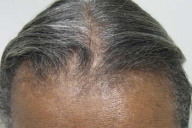 |
| Figure 1 | Figure 2 |
|---|
On examination of the body, an erythematous papule was present on the left forearm. A punch biopsy was performed and was positive for fungi (Fig. 3). A scalp fungal culture grew Trichophyton tonsurans.
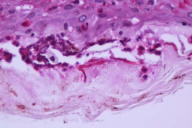 |
| Figure 3 |
|---|
The patient was treated with a six week course of griseofulvin 250mg by mouth twice daily and topical terbinafine twice daily on the scalp and arm. A repeat scalp fungal culture at the end of the six week course was negative and the patient's pruritus had resolved.
Discussion
Tinea capitis (TC) is a common infection in the United States with the predominant fungal organism being Trichophyton tonsurans [1, 2, 3, 4]. Although most common in children aged 3 to 7 years, TC can occur at any age from the neonate [5, 6] to the elderly [7, 8] and the increasing incidence in adults ranges from 2.7 percent to 11.4 percent of reported cases [3, 9, 10, 11, 12, 13]. However, low clinical suspicion combined with the varied clinical manifestations of tinea capitis caused by T. tonsurans can lead to under-recognition of the problem in adults. At times, pruritus and mild scaling may be the only clinical manifestation of disease, such as seen in this patient. Interestingly, it has been suggested that asymptomatic or minimally symptomatic carrier adults may act as a reservoir of disease in households of children with TC, underscoring the importance of a heightened awareness of TC in adults [14]. At-risk adults may be difficult to identify since there is a complex and changing relationship between the host and dermatophyte that ultimately determines susceptibility and infection [15, 16]. Host factors predisposing to infection include the presence of a broad-based immune dysregulation such HIV infection and a defective epidermal barrier [17, 18, 19, 20]. Whether chronic immunosuppression due to medications (chemotherapy, prednisone) increases the host's risk of infection is debatable [17, 18, 19, 20]. Patients with rheumatoid arthritis have been noted to have a higher likelihood of dermatophyte infection compared to a control group even after adjusting for immunosuppressive medications suggesting an inherent host susceptibility [21]. Increased rates of TC infection in black patients has also been documented, but to date, the reason for this observation is unclear as a case-controlled study showed that acquisition of TC was unrelated to specific hair care practices such as use of hair oils, frequency of washing, or tight braiding [22].
In primary cicatricial alopecia, there is an inflammatory assault directed primarily at the follicular unit. Although the antigentic trigger for this inflammation is unclear, there is eventually loss of the sebaceous glands and follicular stem cells leading to permanent hair loss. Aside from the cutaneous manifestations, there is no evidence of systemic immune dysregulation or increased susceptibility to infection. Central centrifugal cicatricial alopecia (CCCA) [23] is a subtype of primary cicatricial alopecia usually occurring in middle-aged African American females. Unlike other subtypes of cicatricial alopecia, patients seldom report pruritus. Furthermore, perifollicular scale is mild or absent in CCCA even when there is perifollicular inflammation on histology [24]. Although patients with cicatricial alopecia are not considered to have an increased risk of dermatophyte infection, this case highlights the fact that other host features, including immunosuppressive medications used for treatment of cicatricial alopecia or other co-existing disorders, may predispose to TC. Given the subtle or atypical manifestations of TC in adults and epidemic levels of TC in the United States, a fungal culture should be an integral part of the evaluation of CCCA, especially when there is the presence of localized scaling or pruritus. Furthermore, this case illustrates the importance of questioning working diagnoses when a patient fails to respond to therapy.
Tinea capitis requires systemic treatment [25]. Griseofulvin is most commonly utilized due to its cost-effectiveness although treatment failures have become more common and the dose required for effective treatment has been increasing [26, 27, 28, 29]. It is unclear whether there is emerging fungal resistance to griseofulvin or whether poor adherance to a 6-8 week course leads to failure of treatment. Newer antifungal agents including itraconazole, fluconazole, and terbinafine are similar in efficacy to griseofulvin, are safe, and may decrease the rate of recurrence [26, 27, 30]. Topical 2 percent ketoconazole and 1 percent selenium sulfide shampoos and topical antifungal creams can be considered as adjunctive treatment [31, 32, 33].
References
1. Aly R, Hay RJ, Del Palacio A, Galimberti R. Epidemiology of tinea capitis. Med Mycol. 2000;38 Suppl 1:183-188. PubMed.2. Elewski BE. Tinea capitis: a current perspective. J Am Acad Dermatol. Jan 2000;42(1 Pt 1):1-20; quiz 21-24. PubMed.
3. Frieden IJ, Howard R. Tinea capitis: epidemiology, diagnosis, treatment, and control. J Am Acad Dermatol. Sep 1994;31(3 Pt 2):S42-46. PubMed.
4. Kemna ME, Elewski BE. A U.S. epidemiologic survey of superficial fungal diseases. J Am Acad Dermatol. Oct 1996;35(4):539-542. PubMed.
5. Manglani PR, Ramanan C, Durairaj P, Ghorpade A. Trichophyton tonsurans infection in a 9-day-old infant. Int J Dermatol. Mar 1988;27(2):128. PubMed.
6. Weston WL, Morelli JG. Neonatal tinea capitis. Pediatr Infect Dis J. Mar 1998;17(3):257-258. PubMed.
7. Buckley DA, Fuller LC, Higgins EM, du Vivier AW. Lesson of the week. Tinea capitis in adults. BMJ. May 20 2000;320(7246):1389-1390. PubMed.
8. Conerly SL, Greer DL. Tinea capitis in adults over fifty years of age. Cutis. Apr 1988;41(4):251-252. PubMed.
9. Bronson DM, Desai DR, Barsky S, Foley SM. An epidemic of infection with Trichophyton tonsurans revealed in a 20-year survey of fungal infections in Chicago. J Am Acad Dermatol. Mar 1983;8(3):322-330. PubMed.
10. Lobato MN, Vugia DJ, Frieden IJ. Tinea capitis in California children: a population-based study of a growing epidemic. Pediatrics. Apr 1997;99(4):551-554. PubMed.
11. Suh DC, Friedlander SF, Raut M, et al. Tinea capitis in the United States: Diagnosis, treatment, and costs. J Am Acad Dermatol. Dec 2006;55(6):1111-1112. PubMed.
12. Williams JV, Honig PJ, McGinley KJ, Leyden JJ. Semiquantitative study of tinea capitis and the asymptomatic carrier state in inner-city school children. Pediatrics. Aug 1995;96(2 Pt 1):265-267. PubMed.
13. Sharma V, Hall JC, Knapp JF, Sarai S, Galloway D, Babel DE. Scalp colonization by Trichophyton tonsurans in an urban pediatric clinic. ?Asymptomatic carrier state. Arch Dermatol. Oct 1988;124(10):1511-1513. PubMed.
14. Bergson CL, Fernandes NC. Tinea capitis: study of asymptomatic carriers and sick adolescents, adults and elderly who live with children with the disease. Rev Inst Med Trop Sao Paulo. Mar-Apr 2001;43(2):87-91. PubMed.
15. Woodfolk JA, Platts-Mills TA. The immune response to dermatophytes. Res Immunol. May-Jun 1998;149(4-5):436-445; discussion 522-433. PubMed.
16. Mirmirani P WA, Chamlin A, Frieden IJ, Price VH. Tinea Capitis Mimicking Cicatricial Alopecia: What Host and Dermatophyte Factors Lead to this Unusual Clinical Presentation? Journal of the American Academy of Dermatology. 2008;In Press.
17. Mirmirani P, Hessol NA, Maurer TA, Berger TG, Nguyen P, Khalsa A, Gurtman A, Micci S, Young M, Holman S, Gange SJ, Greenblatt RM. Prevalence and predictors of skin disease in the Women's Interagency HIV Study (WIHS). J Am Acad Dermatol. May 2001;44(5):785-788. PubMed.
18. Stiller MJ, Rosenthal SA, Weinstein AS. Tinea capitis caused by Trichophyton rubrum in a 67-year-old woman with systemic lupus erythematosus. J Am Acad Dermatol. Aug 1993;29(2 Pt 1):257-258. PubMed.
19. Smith KJ, Welsh M, Skelton H. Trichophyton rubrum showing deep dermal invasion directly from the epidermis in immunosuppressed patients. Br J Dermatol. Aug 2001;145(2):344-348. PubMed.
20. Hay RJ. Chronic dermatophyte infections. I. Clinical and mycological features. Br J Dermatol. Jan 1982;106(1):1-7. PubMed.
21. Bicer A, Tursen U, Cimen OB, Kaya TI, Ozisik S, Ikizoglu G, Erdogan C. Prevalence of dermatophytosis in patients with rheumatoid arthritis. Rheumatol Int. Jan 2003;23(1):37-40. PubMed.
22. Sharma V, Silverberg NB, Howard R, Tran CT, Laude TA, Frieden IJ. Do hair care practices affect the acquisition of tinea capitis? A case-control study. Arch Pediatr Adolesc Med. Jul 2001;155(7):818-821. PubMed.
23. Olsen E, Bergfeld W, Cotsarelis G, Price VH, Shapiro J, Sinclair R, Soloman A, Sperling L, Stenn K, Whiting DA, Bernardo O, Bettencourt M, Bolduc C, Callendar V, Elston D, Hickman J, Ioffreda M, King L, Linzon C, McMichael A, Miller J, Mulinari F, Trancik R, Workshop on Cicatricial Alopeica. Summary of North American Hair Research Society (NAHRS)-sponsored Workshop on Cicatricial Alopecia, Duke University Medical Center, February 10 and 11, 2001. J Am Acad Dermatol. 2003;48(1):103-110. PubMed.
24. Whiting D, Olsen E. Central centrifugal cicatricial alopecia. Dermaol Ther. 2008;21(4):268-278. PubMed.
25. Fuller L, Child F, Midgley G, Higgins E. Diagnosis and management of scalp ringworm. BMJ. 2003;326(7388):539-541. PubMed.
26. Elewski BE, Caceres HW, Deleon L, El Shimy S, Hunter JA, Korotkiy N, Rachesky IJ, Sanchez-Bal V, Todd G, Wraith L, Cai B, Tavakkol A, Bakshi R, Nyirady J, Friedlander SF. Terbinafine hydrochloride oral granules versus oral griseofulvin suspension in children with tinea capitis: Results of two randomized, investigator-blinded, multicenter, international, controlled trials. J Am Acad Dermatol. Mar 29 2008. PubMed.
27. Gonzalez U, Seaton T, Bergus G, Jacobson J, Martinez-Monzon C. Systemic antifungal therapy for tinea capitis in children. Cochrane Database Syst Rev. 2007(4):CD004685. PubMed.
28. Gupta AK, Cooper EA, Bowen JE. Meta-analysis: griseofulvin efficacy in the treatment of tinea capitis. J Drugs Dermatol. Apr 2008;7(4):369-372. PubMed.
29. Roberts BJ, Friedlander SF. Tinea capitis: a treatment update. Pediatr Ann. Mar 2005;34(3):191-200. PubMed.
30. Cáceres-Ríos H, Rueda M, Ballona R, Bustamante B. Comparison of terbinafine and griseofulvin in the treatment of tinea capitis. J Am Acad Dermatol. 2000;42(1 Pt 1):80-84. PubMed.
31. Greer DL. Successful treatment of tinea capitis with 2% ketoconazole shampoo. Int J Dermatol. Apr 2000;39(4):302-304. PubMed.
32. Allen HB, Honig PJ, Leyden JJ, McGinley KJ. Selenium sulfide: adjunctive therapy for tinea capitis. Pediatrics. Jan 1982;69(1):81-83. PubMed.
33. Redondo-Mateo J, Esquivias-Gomez JI, Carrero-Gonzalez P. Tinea capitis and topical Terbinafine cream. Int J Dermatol. May 2004;43(5):395-396. PubMed.
© 2008 Dermatology Online Journal

