Klippel-Trenaunay syndrome
Published Web Location
https://doi.org/10.5070/D30sm631c3Main Content
Klippel-Trenaunay syndrome
Elizabeth K. Hale
Dermatology Online Journal 8(2): 13
From New York University Department of DermatologyHistory
This 55-year-old man has a problem since birth involving the left lower extremity. The patient presented to the Charles C. Harris Skin and Cancer Pavilion in December, 2000 for a routine skin examination. He was noted to have a vascular malformation on his left lower extremity, which had been present since birth. He had no cosmetic concerns regarding the lesion, but he did report occasional pain and mild swelling of his left lower extremity, especially after standing for long periods of time. The lesion was otherwise asymptomatic. He had not sought any previous medical advice or treatment of the lesion. His past medical history was otherwise unremarkable.
Physical Examination
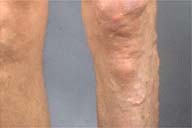 | 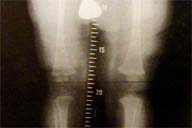 |
| Figure 1 | Figure 2 |
|---|
A large, irregular, deeply erythematous patch covered an extensive portion of his posterior left lower extremity. Multiple, large, venous varicosities were associated with the lesion, and there was mild, soft tissue hypertrophy. No other similar lesions were noted on the patient's skin. No bruit was appreciated.
Laboratory Data
Radiographs of the left femur, tibia, and fibula failed to show evidence of bony hypertrophy or other abnormalities. However, in the radiograph shown above, which was obtained from another patient with the same diagnosis, enlargement of the bones of the left leg, with associated soft tissue hypertrophy, can be visualized.
Comment
In 1900, Klippel and Trenaunay first described a syndrome consisting of a capillary-venous malformation in association with an early onset of varicosities and underlying soft tissue and bony hypertrophy. Years later, Frederick Parks Weber noted the occurrence of these findings in association with arteriovenous fistulas. The related Klippel-Trenaunay-Weber syndrome describes those individuals who have an arteriovenous malformation as a component of their syndrome.
Klippel-Trenaunay syndrome, also known as nevus vasculosus hypertrophicus, is characterized by a triad of extensive nevus flammeus, underlying venous varicosities, and underlying soft tissue and/or bony hypertrophy. The lower limb is the site of malformation in approximately 95 percent of patients. When found on the trunk, the malformation rarely crosses the midline. The hypertrophy involves the length as well as the circumference of the involved extremity and is caused by local hyperemia and venous stasis secondary to the vascular anomaly. Recent reviews demonstrate no specific sexual or ethnic predilection.
Patients with Klippel-Trenaunay syndrome frequently manifest additional vascular malformations, which include abnormalities of arteries and lymphatic vessels. Vascular abnormalities are congenital; therefore, they do not respond to agents used in the treatment of hemangiomas, such as prednisone and interferon alpha. Noninvasive imaging (plain radiographs, color duplex ultrasonography, magnetic resonance imaging, and lymphoscintigraphy) is used for diagnosis and ongoing evaluation in patients with Klippel-Trenaunay syndrome. These modalities are particularly useful when surgical intervention is required for arteriovenous malformation or limb length discrepancy. It is important to establish that the deep venous system is not compromised before attempting correction of other defects.
Most complications of Klippel-Trenaunay syndrome are related to the underlying vascular pathology, which includes stasis dermatitis, thrombophlebitis, cellulitis, limb disparity, and more serious sequelae as thrombosis, coagulopathy, bleeding, pulmonary embolism, and congestive heart failure. The most common problem is pain due to venous insufficiency or lymphedema, which can usually be managed by elevation, compression garments, and diuretics. Pulsed-dye laser treatments can lighten the nevus flammeus component. Patients with Klippel-Trenaunay syndrome are best served by a multidisciplinary approach to management. There are support groups to help patients and their families cope with the psychological impact of this condition. Klippel-Trenaunay Support Group website:www.k-t.org. Phone number is (952)-925-2596.
References
Kanterman RY, et al. Klippel-Trenaunay syndrome: imaging findings and percutaneous intervention. Am J Roentgenol 167:989, 1996al-Salman MM. Klippel-Trenaunay syndrome: clinical features, complications, and management. Surg Today 27:735, 1997
Berry SA, et al. Klippel-Trenaunay syndrome. Am J Med Genet 79:319, 1998
Gupta G, et al. A prospective study of the impact of laser treatment on vascular lesions. Br J Dermatol 143:356, 2000
Richards KA, et al. The pulsed-dye laser for cutaneous vascular and nonvascular lesions. Semin Cutan Med Surg 19:276, 2000
© 2002 Dermatology Online Journal

