Blastomycosis-like pyoderma in association with recurrent vesicular hand eczema: Good response to acitretin
Published Web Location
https://doi.org/10.5070/D30ds6984nMain Content
Blastomycosis-like pyoderma in association with recurrent vesicular hand eczema: Good response to acitretin
Roberto Cecchi MD, Laura Bartoli MD, Luigi Brunetti MD, Mario Pavesi MD
Dermatology Online Journal 17 (3): 9
Department of Dermatology, Hospital of Pistoia, Pistoia, Italy. r.cecchi@usl3.toscana.itAbstract
Blastomycosis-like pyoderma, also known as pyoderma vegetans, is an uncommon disease characterized by vegetating skin lesions mimicking blastomycosis or warty tuberculosis, often associated with staphylococcal and streptococcal infections. It is more commonly observed in elderly patients with impaired immunological capacity, and is often unresponsive to various therapeutic modalities. We describe a case of BLP that occurred on the palmar aspect of the left hand in an elderly female, affected with recurrent vesicular hand eczema. The disease resolved completely following the administration of oral acitretin 25 mg/day for 10 weeks.
Introduction
Blastomycosis-like pyoderma (BLP), also known as pyoderma vegetans, is a rare cutaneous disease possibly related to bacterial infection and often occurring in patients with impaired immune status [1, 2, 3, 4]. It mostly arises on the extremities with single or multiple, vegetating nodules and plaques, similar to blastomycosis or warty tuberculosis. Necrosis, pustules, ulceration, fistulae, abscesses, and sinus tracts can variably be present. Histopathology shows pseudoepitheliomatous hyperplasia and multiple abscesses in the dermis [3, 4]. The disorder has a chronic course and is often refractory to antibiotic therapy, even when chosen on the basis of culture and sensitivities [3, 4, 5].
We describe a case of BLP in association with recurrent vesicular hand dermatitis, effectively treated with oral acitretin.
Case report
A 79-year-old female was referred to our department with a 3-month history of a rapidly growing nodule on her left hand. She was also affected by recurrent vesicular eczema of her hands for several years, which had been treated with topical steroids and emollients, until the nodule occurrence. Investigations to rule out allergic reactions or infectious agents, including a search for dermatophytes (direct and culture) from hands and feet, patch testing, and prick tests had given negative results.
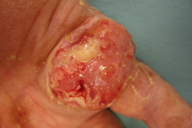
Clinical examination revealed an ulcerated, vegetating, reddish nodule with multiple pustules and sinus tracts located on the left palm (Figure 1). The formation was painful and measured 5 x 4 cm in diameter. In addition, ill-defined, scaly areas with small, itchy vesicles were also evident on both palmar and lateral aspects of the fingers. There was no axillary lymphadenopathy. The remaining physical examination was normal.
Laboratory tests, including blood cell count, serum glucose, electrolytes and creatinine, liver function tests, serum lipids, serum protein electrophoresis, HIV testing, and urinalysis revealed normal findings. In addition, the circulating CD4 and CD8 lymphocyte count was substantially normal.
The patient denied any improvement following treatments with oral antibiotics (doxycycline, clarithromycin) and local medications with gentamycin cream and hydro-gels given by her family physician.
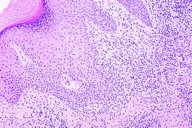 |
| Figure 2 |
|---|
| Pseudoepitheliomatous hyperplasia with a dense inflammatory infiltrate and neuthophilic microabscess formation in the dermis (H&E, x40) |
A biopsy specimen from the nodule showed a marked pseudoepitheliomatous hyperplasia with multiple neutrophilic abscesses in the dermis and subcutaneous tissue (Figure 2). Microbiological stains (Periodic acid-Schiff, Ziehl-Neelsen, and Wide-Fite) gave negative results. Direct and indirect immunofluorescence tests were negative. Bacteriological culture from a pus swab was positive for Staphylococcus aureus. A search for nocardia and actinomycetes was negative. Further serological and instrumental investigations excluded a search for concurrent hematologic or bowel diseases, which were negative. These findings suggested a diagnosis of BLP.
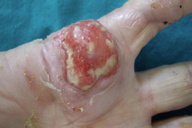
The patient was treated with oral acitretin 25 mg/day in combination with ciprofloxacin 500 mg/day, which was selected on the basis of antibiotic sensitivity tests. Moreover, local medications with clindamycin 1 percent gel were added. After 15 days of therapy, there was an improvement, but not resolution, of the clinical skin lesions that exhibited a marked reduction of the nodule size (Figure 3). Ciprofloxacin was stopped.
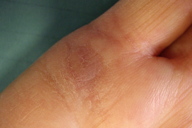
The patient continued with oral acitretin. After 10 weeks of treatment the lesion resolved completely with an atrophic scar (Figure 4). The treatment was stopped after 12 weeks and no recurrence was observed during the subsequent three-month follow-up.
Discussion
Historically, BLP was firstly described in 1898 by Hallopeau under the title of “pyodermite végétante,” and five years later, in 1903 by Azua and Pons as “pseudo-epitheliomatous cutane” [6, 7]. Various other synonyms for BLP include pyodermitis chronica vegetans of Azua, pseudoepithelioma of Azua, mycosis-like pyoderma, hyperinflammatory proliferative pyoderma, and pyoderma vegetans [8].
BLP is believed to represent a vegetating inflammatory tissue reaction to a bacterial infection, generally occurring in patients with reduced immunological resistance. It has been reported in association with HIV infection/AIDS, hematologic and solid malignancies, malnutrition, alcoholism, diabetes mellitus, obesity, inflammatory bowel diseases, psoriatic arthritis, pulmonary granuloma, immunosuppressive therapies, X-radiation, and other conditions [3, 5, 8-12]. However, there are several cases of classic BLP in immunocompetent patients without any underlying factors [3, 5, 10, 14]. Minor trauma may favor the beginning of the lesions, probably creating a localized area of impaired resistance [8]. In Australia, a variant of BLP has been reported under the term of coral reef granuloma, which typically occurs on sun-damaged skin of elderly patients [15,16]. Although Staphylococcus aureus is the most common organism isolated from these lesions, several other organisms, including Gram-positive (ß-hemolytic streptococci), Gram-negative bacteria (Escherichia coli, Proteus, Pseudomonas aeruginosa) and anaerobes (Clostridium, Prevotella) have been isolated [3, 5, 8, 17, 18].
The diagnosis of BLP is based on clinical, pathological, and laboratory features. In 1979 Su et al proposed 6 diagnostic criteria for BLP: (1) large verrucous plaques with multiple pustules and raised border; (2) pseudoepitheliomatous hyperplasia with microabscesses; (3) isolation of a pathogenic bacterium; (4) negative culture for deep fungi, atypical mycobacteria, and mycobacterium tuberculosis; (5) negative fungal serology; and (6) normal bromide and iodide blood levels [3]. Our patient met four of these criteria. Fungal serology tests were not performed and halogen blood levels were not investigated. However, she denied using medications containing halogens. The differential diagnosis of BLP includes several diseases with clinical and pathological similarities, such as pemphigus vegetans, skin infections (tuberculosis and deep mycoses), halogenoderma, and pyoderma gangrenosum [3, 8, 13]. In addition, squamous cell carcinoma should be ruled out, mainly in the presence of marked pseudocarcinomatous hyperplasia.
Treatment of BLP is a challenge. The response to therapy is variable or poor and the course of the disease is often long and frustrating for both patient and physician. Because of the rare occurrence of BLP, there have been no clinically controlled trials examining the efficacy of different treatment regimens [5]. Some reports have described favorable responses to empirically chosen antibiotics, whereas others have reported recovery with culture-driven antibiotics in association with other therapies. Conversely, there are many cases unresponsive to sensitive antibiotics. In addition, several other treatment modalities, including surgical excision and other locally ablative measures (curettage, electrocoagulation, cryotherapy, and laser therapy), intralesional corticosteroids, topical disodium chromoglycate, oral dapsone, and PUVA have been employed with variable results [2, 3, 8, 17-21]. More recently, a good response to etanercept has been reported in a patient affected with severe psoriatic arthritis and pyoderma vegetans with extensive lesions on the lower extremities [13].
Our patient presented with a single BLP lesion on the left palmar area in association with recurrent vesicular hand eczema. To our knowledge, a similar combination has never been reported in the English literature. The pre-existing dermatitis, as well as topical steroid applications for its treatment, or minor trauma may have favored the BLP development, by a decrease of the local immune response.
Partial regression of the nodule was observed after two weeks of a combined therapy with oral ciprofloxacin and acitretin. We cannot exclude that ciprofloxacin alone may have cleared the infection after a longer administration period. However, the patient experienced a complete recovery of BLP within 10 weeks of treatment with acitretin and no recurrence or significant side effect was observed.
Similarly, good results had been reported in two case reports described by Nguyen and Beardmore in 2005 [18]. Acitretin was successfully administered at the dosage of 10 mg daily for 3-4 months in two elderly patients affected with multiple lesions on the face and extremities, and a solitary plaque on the calf, respectively. The excellent response might be related to the anti-inflammatory and anti-proliferative action of retinoid [18]. Subsequently, a young male patient affected with a single BLP lesion and decreased CD4+ T cells attained a good response to a combined treatment of acitretin and a sensitive antibiotic [22]. Again, another patient with metastatic carcinoma of the thyroid developed BLP lesions, refractory to several therapies. The skin disorder showed a significant improvement after acitretin administration [23].
In conclusion, previous reports and our observation suggest that acitretin may be a well-tolerated, efficacious therapy for BLP, mainly in localized forms. However, prospective studies on larger series are warranted to further support these promising results.
References
1. Yaffee HS. Localized blastomycosis-like pyoderma occurring in a tattoo. Arch Dermatol. 1960 Jul; 82: 99-100. [PubMed]2. Williams HM Jr, Stone OJ. Blastomycosis-like pyoderma. Case report of unusual entity with response to curettage. Arch Dermatol. 1966 Feb; 93(2): 226-8. [PubMed]
3. Su WP, Duncan SC, Perry HO. Blastomycosis-like pyoderma. Arch Dermatol. 1979 Feb; 115(2): 170-3. [PubMed]
4. Stone OJ. Hyperinflammatory proliferative (blastomycosis-like) pyodermas: review, mechanisms, and therapy. J Dermatol Surg Oncol. 1986 Mar; 12(3): 271-3. [PubMed]
5. Cerullo L, Zussman J, Young L. An unusual presentation of blastomycosislike pyoderma (pyoderma vegetans) and a review of the literature. Cutis. 2009 Oct;84(4):201-4. [PubMed]
6. Hallopeau H. Pyodermite vegetante, ihre Beziehungen zur dermatitis herpetiformis und dem pemphigus vegetans. Arch Dermatol Syph (Wien). 1898; 43: 289-306.
7. Azua J, Pons DS. Pseudo-épithéliomas cutanés, abstracted. Ann Dermatol Syphilol. 1903; 4:745-6.
8. Sawalka SS. Phiske MM, Jerajani HR. Blastomycosis-like pyoderma. Indian J Dermatol Venereol Leprol. 2007 Mar-Apr; 73(2): 117-9. [PubMed]
9. Crowley JJ, Kim YH. Blastomycosis-like pyoderma in a man with AIDS. J Am Acad Dermatol. 1997Apr; 36(4): 633-4. [PubMed]
10. Dutta TK, James J, Baruah MC, Ratnakar C. Blastomycosis-like pyoderma in a case of chronic myeloid leukaemia. Postgrad Med J. 1992 May; 68(799): 363-5. [PubMed]
11. Harish K, Varghese T, Najeeba R, Harikumar R. Pyoderma vegetans and ulcerative colitis. J Postgrad Med J. 2006 Oct-Dec; 52(4): 302-3. [PubMed]
12. Bianchi L, Carrozzo AM, Orlandi A, Campione E, Hagman JH, Chimenti S. Pyoderma vegetans and ulcerative colitis. Br J Dermatol. Jun; 144(6): 1224-7. [PubMed]
13. Carrera C, Mascaró JM Jr, Moreno-Romero JA, Iranzo P, Palou J, Zamora E, Herrero C. Pyoderma vegetans associated with severe psoriatic arthritis: good response to etanercept. Dermatology. 2007; 214(1); 77-81. [PubMed]
14. Papadopoulos AJ, Schwartz RA, Kapila R, Samady JA, Ruszczak Z, Rao BK, Lambert WC. Pyoderma vegetans. J Cut Med Surg. 2001 May-Jun; 5(3): 223-7. [PubMed]
15. Georgouras K. Coral reef granuloma. Cutis. 1967; 3: 37-9.
16. Weedon D. Actinic comedonal plaque. J Am Acad Dermatol. 1981 Nov; 5(5): 611-3. [PubMed]
17. Trygg KJ, Madison KC. Blastomycosis-like pyoderma caused by Pseudomonas aeruginosa: report of a case responsive to ciprofloxacin. J Am Acad Dermatol. 1990 Oct; 23(4 Pt 1): 750-2. [PubMed]
18. Nguyen RT, Beardmore GL. Blastomycosis-like pyoderma: successful treatment with low-dose acitretin. Australas J Dermatol. 2005 May; 46(2): 97-100. [PubMed]
19. Su O, Demirkesen C, Onsun N. Localized blastomycosis-like pyoderma with good response to cotrimoxazol and cryotherapy. Int J Dermatol. 2004 May; 43(5): 388-90. [PubMed]
20. Rongioletti F, Semino M, Drago F, Blangetti MG, Rebora A. Blastomycosis-like pyoderma (Pyoderma vegetans) responding to antibiotics and topical disodium chromoglycate. Int J Dermatol. 1996 Nov; 35(11): 828-30. [PubMed]
21. Sawchuk WS, Heald PW. Blastomycosis-like pyoderma- report of a case responsive to combination therapy utilizing minocycline and carbon dioxide laser debridement. J Dermatol Surg Oncol. 1986 Mar; 12(3): 271-3. [PubMed]
22. Lu XL, Zhao W, Xia YK, Chen J, Wang L, Zhou XW, Liu WD. Good response of a combined treatment of acitretin and antibiotics in blastomycosis-like pyoderma. Eur J Dermatol. 2009; May-Jun; 19(3): 261-2. [PubMed]
23. Kobraei KB, Wesson SK. Blastomycosis-like pyoderma: response to systemic retinoid therapy. Int J Dermatol. 2010 Nov; 49(11): 1336-8. [PubMed]
© 2011 Dermatology Online Journal