Diffuse plexiform neurofibroma in a 13-year-old girl
Published Web Location
https://doi.org/10.5070/D30ct715bmMain Content
Diffuse plexiform neurofibroma in a 13-year-old girl
Amor Khachemoune MD CWS1, Khalid Al Aboud MD2, Khalid Al Hawsawi MD2
Dermatology Online Journal 9 (5): 23
1. Georgetown University Medical Center 2. Dermatology unit, Department of Medicine, King Faisal hospital, Taif, Saudi Arabia.
amoa65@hotmail.com
Plexiform neurofibroma is an uncommon skin tumor. We present a case of 13-year-old girl with neurofibromatosis type 1 who presented with a large, diffuse, plexiform neurofibroma.
Case report
A 13-year-old girl presented with a slightly painful swelling over the left thigh of 2 years' duration. The swelling developed within a café-au-lait patch that has been present since birth. The uncle of the patient's father has neurofibromatosis type 1 (NF1).
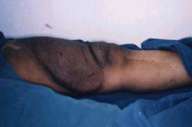
The patient has a total of 23 café-au-lait patches, each measuring more than 1.5 cm in diameter. She also has both axillary and inguinal freckling. On the left thigh is a large, soft, compressible, hyperpigmented and hypertrichotic plaque measuring 24 cm in diameter (fig. 1). Overlying this plaque and extending from the groin to the proximal leg, is a 42 × 5-cm café-au-lait patch with a smooth border, with marked hyperpigmentation over the plaque component.
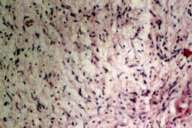
Skin biopsy from the plaque shows a circumscribed, lobular proliferation of spindle cells in a loose fibular background that distorts much of the dermis and subcutaneous fat (fig. 2). The lobule is lined with a compressed rim of thin, delicate collagen bundles and perineurial cells. Pleomorphic nuclei and mitotic figures are not seen. Except for a deeply pigmented basal layer, the epidermis is normal. This histological presentation is consistent with a plexiform neurofibroma.
Given the constellation of cutaneous findings and a positive family history, this patient is diagnosed as having NF1.
Discussion
NF1 is a common, autosomal-dominant disorder, with an incidence of about 1 in 2,500-3,300. It accounts for up to 90 percent of the cases of NF. The cardinal clinical features are multiple neurofibromas and pigmentary changes [1]. These include café-au-lait spots, freckles, and hyperpigmentation overlying plexiform neurofibromas. The complete list of criteria for the diagnosis of NF1 are summarized in table 1, developed by the National Institute of Health Consensus Development Conference on neurofibromatosis (1987) [2].
|
|
|
| Source.—The National Institute of Health Consensus Development Conference on neurofibromatosis (1987). |
|
|
Plexiform neurofibromas are diffuse, elongated fibromas coursing along the nerves. These lesions frequently involve the trigeminal or upper cervical nerves. Plexiform neurofibromas often appear within the first 2 years of life [1]. There are two types of plexiform neurofibromas, nodular and diffuse [3]. Diffuse plexiform neurofibroma, also known as elephantiasis neurofibromatosa [1], has an overgrowth of epidermal and subcutaneous tissue associated with a wrinkled and pendulous appearance. Plexiform neurofibroma occurs in only 5 percent of patients with NF1 [3].
Recently, Happle proposed that large plexiform neurofibromas might be explained as type 2 segmental manifestations of NF1 [4]. Accordingly, such tumors would originate from loss of heterozygosity occurring at an early developmental stage[3].
Plexiform neurofibromas need to be monitored frequently because 5 percent develop into malignant peripheral nerve sheath tumors [3]. Other complications include bleeding from trauma, neurological deficits, limited limb, and psychological disturbance because of abnormal anatomy. In each of the above complications surgery might be helpful. However, one should keep in mind that in plexiform neurofibromas, dangerous bleeding may complicate surgical procedures, and therefore, extreme caution should be exercised during surgery [5].
Our case indicates the importance of following a child with multiple large café-au-lait spots as they may precede the onset of an underlying plexiform neurofibroma. Our patient was referred to a surgeon.
References
1. Harper JI. Genetics and genodermatoses. In: Champion RH, Burton JL, Burns DA, Breathnach SM editors Rook/Wilkinson/Ebling. Text book of Dermatology. 6th ed. Oxford: Blackwell Science; 1998. P.378-84.2. National Institutes of Health Consensus Development Conference Statement: neurofibromatosis. Bethesda, Md., USA, July 13-15, 1987. Neurofibromatosis. 1988;1(3):172-8.
3. Pivnick EK, Riccardi: VM. The Neurofibromatoses. In : Freedberg IM, Eisen AZ,Wolff K, Austen KF, Goldsmith LA, Kartz SI, Fitzpatrick TB. Fitzpatrick's Dermatology in General Medicine. New York: Mc graw Hill ; 1999. p.2152-58.
4. Happle R: large plexiform neurofibromas may be explained as a type 2 segmental manifestation of neurofibromatosis 1. Am J Med Genet 2001;98:363-364.
5. Littlewood AH, Stilwell JH:The vascular features of plexiform neurofibroma with some observations on the importance of pre-operative angiography and the value of pre-operative intra-arterial embolization. Br J Plast Surg 1983;36:501-506.
© 2003 Dermatology Online Journal