Case report: Fluocinonide-induced perioral dermatitis in a patient with psoriasis
Published Web Location
https://doi.org/10.5070/D30731q371Main Content
Case report: Fluocinonide-induced perioral dermatitis in a patient with psoriasis
Payman Kosari1, Steven R Feldman MD PhD1,2
Dermatology Online Journal 15 (3): 15
1. Department of Dermatology2. Departments of Dermatology and Pathology
Center for Dermatology Research, Wake Forest University School of Medicine; Winston-Salem, North Carolina. sfeldman@wfubmc.edu
Abstract
Topical corticosteroids are the primary treatment for psoriasis. A patient with psoriasis being treated with topical fluocinonide for lesions on the extremities developed an erythematous facial eruption consistent with perioral dermatitis. When topical agents are applied, they often end up in unintended areas. The potential for drug-induced perioral dermatitis should be considered in psoriasis patients treated with potent topical corticosteroids.
Introduction
Topical corticosteroids are a mainstay of psoriasis treatment. They are used as the primary treatment for patients with localized disease and are often used as adjunct treatment for the worst spots in patients receiving phototherapy or systemic therapy for severe psoriasis. Potent corticosteroid agents, primarily clobetasol, are often used and effectively treat psoriatic lesions with few side effects. However, local reactions can occur in areas of the body where their use is not intended [1]. We present a patient who developed perioral dermatitis during the course of topical fluocinonide treatment for psoriasis lesions of the scalp and elbows.
Case Presentation
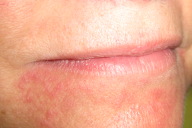 |
| Figure 1 |
|---|
| Figure 1. Clinical picture of perioral-dermatitis in a patient using high-potency corticosteroids for psoriasis |
A 57-year-old woman with psoriasis presented with a new, erythematous eruption around the mouth and nares (Fig. 1). She had been prescribed topical fluocinonide 0.05 percent ointment 9 months earlier as a treatment for psoriasis of the scalp and elbows. The scalp and elbow lesions had responded well. When she began to develop the perioral eruption, she applied the topical fluocinonide to her face with temporary relief and subsequent worsening.
She was diagnosed with perioral dermatitis, probably initiated and exacerbated by the topical fluocinonide. She was prescribed tetracycline to take by mouth twice daily and was told to taper off the antibiotics. No topical medications were used. For her psoriasis, she was instructed to continue the fluocinonide as needed and to thoroughly wash her hands with soap after each application, avoiding contact with her face.
The patient completed her seven-day course of antibiotics and began routinely washing her hands after each topical application of fluocinonide. She has since cleared of her perioral dermatitis with no recurrences and has not required any further treatment. Her psoriasis continues to be controlled with topical steroids.
Discussion
Our patient presented with perioral dermatitis in the setting of having used a potent topical corticosteroid to psoriasis lesions on the extremities. Prior to development of the facial eruption, she reported that she had not applied the fluocinonide to her face. Adherence to topical treatment recommendations is poor, and it is possible that she had used the medication on the face, despite warnings to the contrary. More likely, however, the fluocinonide may have been applied to the face unknowingly.
Topical preparations do not stay confined to the sites to which they are applied. The spread of topical tetracycline hydrochloride to areas of the body other than the site of original application was studied using a Wood's lamp, taking advantage of the fluorescence of tetracycline. When initial site of application was the dominant hand, there was an increased tendency towards transferring the topical preparation to the face. The vehicle used for delivery of the topical preparation also affected the extent of transfer, with ointments and creams exhibiting greater transfer than lotions or tinctures. Importantly, no areas of the body, including initial site of application, fluoresced with a Wood's lamp when washed with soap [2].
Inadvertent spread of topical agents from the hand to the face raises the potential for development of perioral dermatitis in patients receiving topical corticosteroids for psoriasis or other inflammatory skin diseases. To reduce the risk of perioral dermatitis, patients can be cautioned to wash their hands after applying the medication. However, when educating about hand washing after use of topical steroids, it is important to present the matter in such a way so as not to cause excessive fear and or to decrease compliance. Psoriasis patients are often noncompliant with their medications and one of the most important reasons for poor adherence is a fear of potential side effects [3, 4, 5].
References
1. Fritz KA, Weston WL. Topical glucocorticosteroids. Ann Allergy 1983;50:68-76. [PubMed]2. Johnson R, Nusbaum BP, Horwitz SN, Frost P. Transfer of topically applied tetracycline in various vehicles. Arch Dermatol 1983;119:660-3. [PubMed]
3. Brown KK, Rehmus WE, Kimball AB. Determining the relative importance of patient motivations for nonadherence to topical corticosteroid therapy in psoriasis. J Am Acad Dermatol 2006;55:607-13. [PubMed]
4. Ali SM, Brodell RT, Balkrishnan R, Feldman SR. Poor adherence to treatments: a fundamental principle of dermatology. Arch Dermatol 2007;143:912-5. [PubMed]
5. Storm A, Andersen SE, Benfeldt E, Serup J. One in 3 prescriptions are never redeemed: primary nonadherence in an outpatient clinic. J Am Acad Dermatol 2008;59:27-33. [PubMed]
© 2009 Dermatology Online Journal

