Necrobiotic xanthogranuloma treated with chlorambucil
Published Web Location
https://doi.org/10.5070/D39sd4d9z9Main Content
Necrobiotic xanthogranuloma treated with chlorambucil
Sima Z Torabian MD, Nasim Fazel MD DDS, Robin Knuttel MD
Dermatology Online Journal 12 (5): 11
University of California Davis Department of Dermatology. sima.torabian@ucdmc.ucdavis.eduAbstract
We report a case of necrobiotic xanthogranuloma that responded to treatment with chlorambucil. A 56-year-old man presented with a 5-year history of multiple, mildly pruritic, brown-to-violaceous plaques with central ulceration and atrophy involving the periorbital area, extremities, and trunk. Laboratory studies showed mild leukopenia and a monoclonal gammopathy of the IgG lambda type on serum protein immunoelectrophoresis. Histopathological evaluation revealed a dense histiocytic infiltrate with hyaline necrobiosis involving the dermis with extension to the subcutis. Multiple large multinucleated giant cells and scattered lymphocytes were seen. A diagnosis of necrobiotic xanthogranuloma was established. The patient was started on chlorambucil initially at 2 mg per day. The dose was later increased to 4 mg per day, which resulted in flattening and complete resolution of his skin lesions.
Clinical synopsis
A 56-year-old man presented to the UC Davis Dermatology Clinic with a 5-year history of multiple mildly pruritic reddish brown lesions around his eyes, extremities, and trunk. Initial biopsy at an outside facility showed palisading granuloma and he was given topical and intralesional steroids without any improvement. In fact, his lesions continued to grow in number and size and later became ulcerated. His review of systems revealed mild fatigue. Physical examination showed multiple indurated firm erythematous to violaceous plaques and nodules with faint yellow hue arrayed in an asymmetrical distribution involving the peri-orbital area, trunk, and extremities. Some lesions had telangiectases, central ulceration, and atrophy. There was no evidence of lymphadenopathy or hepatosplenomegaly.
 |  |
| Figure 1 | Figure 2 |
|---|---|
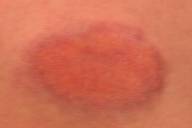
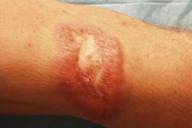
| Figure 1: Violaceous indurated plaque with xanthomatous hue Figure 2: Erythematous indurated plaque with central ulceration and atrophy | |
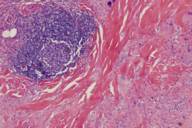
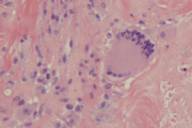
Laboratory evaluation was significant for mild leukopenia, elevated erythrocyte sedimentation rate, hyperlipidemia, and hypocomplementemia. Serum protein electrophoresis showed monoclonal gammopathy of the IgG-λ type. A punch biopsy revealed a dense histiocytic infiltrate with hyaline necrobiosis involving the dermis extending to subcutis. Many large multinucleated giant cells and scattered lymphocytes were seen. Bone marrow aspirate and biopsy showed approximately 2 percent atypical plasma cells. This finding was worrisome but not sufficient to make a diagnosis of multiple myeloma.
Based on the clinical picture, serum electrophoresis, and biopsy results, a diagnosis of necrobiotic xanthogranuloma was made. He was started on chlorambucil, initially at 2 mg per day. The dose was increased to 4 mg daily after 2 weeks. Treatment resulted in progressive flattening and disappearance of his skin lesions, however his paraproteinemia spike persisted throughout treatment and was still present at a 6-month-followup visit.
Comment
Necrobiotic xanthogranuloma (NXG) is a rare chronic progressive disease first described by Kossard and Winkelmann in 1980 [1]. It affects men and women equally with the average age of onset in the sixth decade [2]. Its pathogenesis remains unclear, however most patients are noted to have serum lipid abnormalities. It has been suggested that the monoclonal component may interfere with lipoprotein binding to HDL or LDL receptors, leading to elevation of serum lipids. Increased levels of serum immunoglobulins complexed with lipids may be deposited into skin inciting a foreign body granulomatous reaction [3].
Cutaneous lesions consist of multiple firm violaceous to erythematous papules and nodules with a faint yellow hue and telangiectases. Lesions tend to enlarge and later undergo central ulceration followed by atrophy. They most commonly occur in the periorbital area but may involve the face, trunk and extremities [4]. Ocular findings account for the most severe associated extracutaneous complications and include ulcerations of the palpebral fissure, scleritis, iritis, conjunctivitis, anterior uveitis, keratitis, and blindness [5]. Other reported organ involvement includes granulomatous infiltration of the larynx (presenting with hoarseness), lung, heart, liver, kidney, skeletal muscle, and central nervous system [6, 7, 8, 9, 10].
The most prominent laboratory finding is paraproteinemia, most commonly of the IgG-κ light-chain type, that can be present in up to 80 percent of patients. These patients have a 9-11 percent risk of developing multiple myeloma or other malignant lymphoproliferative diseases [1, 4]. Therefore, repeated hematological evaluation is necessary. Other reported laboratory abnormalities are leukopenia, anemia, elevated erythrocyte sedimentation rate, hyperlipidemia, hypergammaglobulinemia, hypocomplementemia, and cryoglobulinemia [11].
Histopathological evaluation shows a palisading histiocytic granulomatous infiltrate with alternating foci of hyaline necrobiosis invading the dermis and extending to the subcutis. Multiple Touton giant cells, bizarre-shaped foreign body giant cells, lymphoid nodules, foci of plasma cells and occasional cholesterol clefts may be seen [12].
NXG has a chronic slowly progressive course leading to tissue destruction. Unfortunately, owing to its rarity, no controlled therapeutic trials have been conducted. Surgical excision of the lesions has been associated with recurrence and or worsening of disease activity [13]. Various outcomes have been reported with other treatment modalities such as intralesional steroids [14], high dose systemic corticosteroid [15], plasmapheresis [16], interferon-α-2b [17], radiation [18], and cytotoxic agents such as melphalan [1, 19], cyclophosphamide [20], and methotrexate [1].
Chlorambucil is a low-dose alkylating agent that was first used by Finan and Winkelmann in 9 out of 22 patients with NXG. Three had total clearing, 4 had partial response and 2 had a halt in the progression of their disease [11]. Machado et al. reported complete resolution of skin lesions and paraproteinemia after 7 months of treatment with chlorambucil at 2 mg per day [21]. Our case is the third report of successful treatment of NXG with chlorambucil.
In conclusion, although NXG is a rare condition, its recognition is important not only because it is locally destructive but also because it can be associated with systemic diseases such as multiple myeloma, lymphoproliferative disorders or granulomatous involvement of various internal organs. A thorough physical examination looking for lymphadenopathy and hepatosplenomegaly, protein immunoelectrophoresis, and bone marrow biopsy are mandatory.
Acknowledgment: The author would like to acknowledge Dr. Rafael Rodriguez for his assistance in preparing the photomicrographs.
References
1. Kossard S, Winkelmann RK. Necrobiotic xanthogranuloma. Australas J Dermatol. 1980 Aug;21(2):85-8. PubMed2. Barzilai A, Trau H, Shpiro D, Yorav S. Necrobiotic xanthogranuloma with paraproteinemia. Cutis. 1996 May;57(5):320-2. UI 8726711
3. Bullock JD, Bartley GB, Campbell RJ, Yanes B, Connelly PJ, Funkhouser JW. Necrobiotic xanthogranuloma with paraproteinemia: case report and a pathogenetic theory. Trans Am Ophthalmol Soc. 1986;84:342-54. PubMed
4. Mehregan DA, Winkelmann RK. Necrobiotic xanthogranuloma. Arch Dermatol. 1992 Jan;128(1):94-100. Erratum in: Arch Dermatol 1992 May;128(5):632. PubMed
5. Robertson DM, Winkelmann RK. Ophthalmic features of necrobiotic xanthogranuloma with paraproteinemia. Am J Ophthalmol. 1984 Feb;97(2):173-83. PubMed
6. Hunter L, Burry AF. Necrobiotic xanthogranuloma: a systemic disease with paraproteinemia. Pathology. 1985 Jul;17(3):533-6. PubMed
7. Fortson JS, Schroeter AL. Necrobiotic xanthogranuloma with IgA paraproteinemia and extracutaneous involvement. Am J Dermatopathol. 1990 Dec;12(6): 579-84. PubMed
8. Winkelmann RK, Litzow MR, Umbert IJ, Lie JT. Giant cell granulomatous pulmonary and myocardial lesions in necrobiotic xanthogranuloma with paraproteinemia. Mayo Clin Proc. 1997 Nov;72(11):1028-33. PubMed
9. Yasukawa K, Kato N, Hamasaka A, Hata H. Necrobiotic xanthogranuloma: isolated skeletal muscle involvement and unusual changes. J Am Acad Dermatol. 2005 Apr;52(4):729-31. PubMed
10. Shah KC, Poonnoose SI, George R, Jacob M, Rajshekhar V. Necrobiotic xanthogranuloma with cutaneous and cerebral manifestations. Case report and review of the literature. J Neurosurg. 2004 Jun;100(6):1111-4. PubMed
11. Finan MC, Winkelmann RK. Necrobiotic xanthogranuloma with paraproteinemia: a review of 22 cases. Medicine (Baltimore). 1986 Nov;65(6): 376-88. PubMed
12. Finan MC, Winkelmann RK. Histopathology of necrobiotic xanthogranuloma with paraproteinemia. J Cutan Pathol. 1987 Apr;14(2):92-9. PubMed
13. Ugurlu S, Bartley GB, Gibson LE. Necrobiotic xanthogranuloma: long-term outcome of ocular and systemic involvement. Am J Ophthalmol 2000 May;129(5):651-7. PubMed
14. Codere F, Lee RD, Anderson RL. Necrobiotic xanthogranuloma of the eyelid. Arch Ophthalmol. 1983 Jan;101(1):60-3. PubMed
15. Plotnick H, Taniguchi Y, Hashimoto K, Negendank W, Tranchida L. Periorbital necrobiotic xanthogranuloma and stage I multiple myeloma. Ultrastructure and response to pulsed dexamethasone documented by magnetic resonance imaging. J Am Acad Dermatol. 1991 Aug;25(2 Pt 2):373-7. PubMed
16. Finelli LG, Ratz JL. Plasmapheresis, a treatment modality for necrobiotic xanthogranuloma. J Am Acad Dermatol. 1987 Aug;17(2 Pt 2):351-4. PubMed
17. Venencie PY, Le Bras P, Toan ND, Tchernia G, Delfraissy JF. Recombinant interferon alfa-2b treatment of necrobiotic xanthogranuloma with paraproteinemia. J Am Acad Dermatol. 1995 Apr;32 (4):666-7. No abstract available. PubMed.
18. Char DH, LeBoit PE, Ljung BM, Wara W. Radiation therapy for ocular necrobiotic xanthogranuloma. Arch Ophthalmol. 1987 Feb;105 (2):174-5. No abstract available. PubMed.
19. MacFarlane AW, Verbov JL. Necrobiotic xanthogranuloma with paraproteinemia. Br J Dermatol. 1985 Sep;113 (3):339-43. PubMed
20. Meyer S, Szeimies RM, Landthaler M, Hohenleutner S. Cyclophosphamide-dexamethasone pulsed therapy for treatment of recalcitrant necrobiotic xanthogranuloma with paraproteinemia and ocular involvement. Br J Dermatol. 2005 Aug;153(2):443-5. No abstract available. PubMed
21. Machado S, Alves R, Lima M, Leal I, Massa A. Cutaneous necrobiotic xanthogranuloma (NXG)-- successfully treated with low dose chlorambucil. Eur J Dermatol. 2001 Sep-Oct;11(5):458-62. PubMedS
© 2006 Dermatology Online Journal