Kaposi varicelliform eruption (eczema herpeticum)
Published Web Location
https://doi.org/10.5070/D39dr4c02zMain Content
Kaposi varicelliform eruption (eczema herpeticum)
Jonathan Olson 1, David T Robles MD PhD2, Phil Kirby MD2, Roy Colven MD2
Dermatology Online Journal 14 (2): 18
1. Department of Medicine, University of Washington School of Medicine, Seattle, WA 981052. Department of Medicine, Division of Dermatology, University of Washington School of Medicine, Seattle, WA 98105
Abstract
A 35-year-old woman with a history of atopic diathesis presented to the emergency department with 2 weeks of widespread facial vesiculopustules and eroded vesicles. HSV-1 was found on viral culture and direct fluorescent antibody testing. She was diagnosed with eczema herpeticum, an uncommon and potentially life-threatening viral infection that arises in areas of pre-existing dermatosis. Antiviral treatment for eczema herpeticum is very effective, and should be instituted without delay to avoid significant morbidity and mortality.
Clinical synopsis
 |  |
| Figure 1 | Figure 2 |
|---|---|
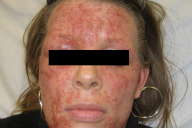
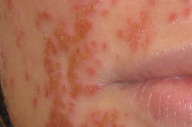
| Figure 1. Numerous umbilicated vesiculopustules and punched-out erosions Figure 2. Yellow crusting representing staphylococcal super-infection | |
A 35-year-old woman with a long history of severe atopic dermatitis, asthma, and allergic rhinitis presented at Harborview Medical Center Emergency for evaluation of a painful vesicular eruption on her face. Two weeks prior to presentation, she was vacationing in England when she developed some vesicles that initially started over the right brow and over the next several days developed some widespread vesicles on the face. She had significant facial swelling and pain and was diagnosed in England with eczema herpeticum 2 days prior to returning to the United States and given oral acyclovir, codeine and flucloxacillin. When she arrived in the US the following day, she went to an outside community emergency department (ED) and was diagnosed instead with a severe contact allergy and given morphine and prednisone and released. Her rash continued to worsen and she was complaining of general malaise when she presented to our ED. Dermatology was consulted to evaluate her skin condition.
On physical examination she had widespread clusters of umbilicated vesiculopustules and eroded vesicles across the face (Fig. 1). Yellow crusting, concerning for staphylococcal super-infection was also present (Fig. 2). Her trunk and extremities had areas of lichenification and erythema, predominantly on the flexural and extensor aspects of her extremities. She had scattered excoriations and although she had swelling of the right eyelid, the ophthalmologic exam was negative for involvement. Dermatology recommended admission with general labs including complete metabolic panel, blood count, and liver function studies to rule out systemic involvement (all of which were negative in this patient). A bacterial culture swab of the facial lesions identified 2+ Staphylococcus aureus and a Herpes group direct fluorescent antibody and culture of the vesicles was positive for Herpes simplex virus (HSV) Type-1. The patient responded well to IV acyclovir at 5 mg/kg per day administered every 8 hours and was discharged in good condition with valacyclovir 1 gram PO TID x 7 days and then switched to acyclovir 200 mg po BID for chronic suppression.
Comment
Eczema herpeticum (EH), or Kaposi varicelliform eruption, is a potentially life-threatening viral infection that arises in pre-existing skin conditions. In some cases, it may progress to fulminating, life-threatening infection and can have severe sequelae, including herpes keratitis, disseminated infection with visceral involvement, and death [1, 2]. Mortality ranges from 1 to 9 percent [3], with reported rates as high as 75 percent before the advent of effective antiviral drugs [4].
The true incidence of EH is not accurately known, because of its rarity and a lack of large studies. Eczema herpeticum was originally considered a disease of infants, and remains more common in children, but can occur at any age [5]. An Increasing incidence was reported in teenagers and young adults in the latter part of the 20th century, along with the increasing prevalence of atopic dermatitis [6], although this has been disputed by more recent studies [7].
As the name implies, the vast majority of EH cases are caused by herpes simplex viruses (HSV 1 and 2) and occur concomitantly with atopic dermatitis [1]. However, Cocksackie virus A16 and vaccinia virus have been implicated also in EH [5]. Multiple skin disorders have been associated with EH including, pemphigus foliaceous, Darier disease, pemphigus vulgaris, pityriasis rubra pilaris, Hailey-Hailey disease, irritant contact dermatitis, cutaneous T-cell lymphoma, seborrheic dermatitis, psoriasis, Wiskott-Aldrich syndrome, congenital icthyosiform erythroderma, and Sezary syndrome [2, 5, 8, 9]. Viral infection is believed to occur as a result of auto-inoculation in a host with a latent infection, or from an infected contact [1].
The most clearly delineated risk factor for EH is disruption of the epidermal barrier [1, 2]. In a retrospective review of 100 EH patients, Wollenberg et al. found that a high serum IgE level and early onset of atopic dermatitis were both risk factors [9]. Defective cytokine secretion and decreased cell-mediated immunity in skin affected by atopic dermatitis and other diseases also appear to play a role in the pathogenesis of EH [10]. An HSV-specific T-cell defect has been proposed [11], although some authors have found no evidence to support this theory [12]. Topical calcineurin inhibitors, which are commonly used to treat atopic dermatitis, have been associated with development of EH and are contraindicated during a herpetic outbreak [13]. Although corticosteroids have long been implicated in EH, recent evidence indicates they have no significant effect [9].
Eczema herpeticum usually begins as clusters of umbilicated vesiculopustules on skin affected by a pre-existing dermatitis and may be accompanied by a flu-like syndrome of fever, chills, and malaise. The vesiculopustules progress to painful hemorrhagic, crusted, punched-out erosions that coalesce to form denuded areas that are prone to secondary bacterial colonization [1]. The upper body is the most common site of infection, with a predilection for the head and neck [2]. Involvement of the eye is considered an ophthalmic emergency and if this is suspected an ophthalmology consult should be obtained. EH usually remains confined to the areas of dermatosis, a patients are infectious as long as active lesions are present [5].
The diagnosis of EH is mainly clinical, although several laboratory tests can be useful. A Tzanck smear is the fastest test but is neither sensitive nor specific for HSV infection [8]. Direct fluorescent antibody staining allows rapid and accurate diagnosis, with results often available in a few hours [1]. Viral culture is both sensitive and specific for HSV infection, but takes at least 48 hours [1]. Both biopsy and serology are of little diagnostic value, and are not recommended on a routine basis [6].
Early use of both antiviral drugs and antibiotics is extremely important; their use should not be delayed pending laboratory tests. The most commonly used antiviral drugs are the nucleoside analogs, which inhibit viral DNA polymerase. Initial treatment is generally with high-dose IV acyclovir, the most widely studied and used drug in EH [8]. Valacyclovir is also very effective, with better oral bioavailability and a more convenient dosing schedule for patients [14].. Antibiotic therapy is tailored to the organism found in culture, most commonly Staphylococcus species [15]. When a bacterial infection is not present, patients should be given a topical antibiotic cream like silver sulfadiazine for prevention [8]. Patients with recurrent HSV infections and a chronic skin disease predisposing to EH should be offered prophylaxis with either valacylovir or acyclovir [15].
Eczema herpeticum can be life threatening. This case illustrates the need for both timely treatment and the use of appropriate lab tests to confirm the diagnosis. Primary care physicians and emergency physicians should recognize the presentation; they are most likely to see these patients. Effective treatment is available in the form of antiviral drugs and should never be delayed.
References
1. Braun-Falco, O., Plewig, G., Wolff, H.H., & Burgdorf, W.H.C. (2000). Dermatology (2nd ed.). Berlin: Springer.2. Fitzpatrick JE, Aeling JL. (2001) Dermatology Secrets in Color (2nd ed.). Philadelphia: Hanley & Belfus.
3. Atherton DJ, Marshall WC. Eczema herpeticum. Practitioner 1982; 226:971-973. PubMed
4. Wollenberg A, Wetzel S, Burgdorf W, Haas J. Viral infections in atopic dermatitis: Pathogenic aspects and clinical management. J Allergy Clin Immunol 2003; 112:667-674. PubMed
5. Kaposi varicelliform eruption. McKenna J, Krusinski P. [Cited on July 2007 5] 2002. Available from: www.emedicine.com/derm/topic204.htm. Cited on 7/5/07.
6. Bork K, Brauninger W. Increasing evidence of eczema herpeticum: analysis of seventy-five cases. J Am Acad Dermatol 1988; 19:1024-1029. PubMed
7. Taieb A, Diris N, Boralevi F, Labreze C. Herpes simplex in children. Clinical manifestations, diagnositci value of clinical signs, clinical course [in French]. Ann Dermatol Venereol 2002; 129:603-608. PubMed
8. Mackley CL, Adams DR, Anderson B, Miller JJ. Eczema herpeticum: a dermatologic emergency. Dermatol Nurs. 2002 Oct; 14(5):307-10, 323; quiz 313. PubMed
9. Wollenberg A, Zoch C, Wetzel S, Plewig G, Przybilla B. Predisposing factors and clinical features of eczema herpeticum-a retrospective analysis of 100 cases. J Amer Acad Dermatol 2003; 49:198-205. PubMed
10. Schmid DS, Rouse BT: The role of T cell immunity in control of herpes simplex virus. Curr Top Microbiol Immunol 1992; 179: 57-74. PubMed
11. Goodyear HM, McLeish P, Randall S, et al: Immunological studies of herpes simplex virus infection in children with atopic eczema. Br J Dermatol 1996 Jan; 134(1): 85-93. PubMed
12. Goodyear HM, et al. Growth of herpes simplex type 1 on skin explants of atopic eczema. Clin Exp Dermatol 1996; 21:185-189. PubMed
13. Wahn U, Bos JD, Goodfield M, Caputo R, Papp K, Manjra A, Dobozy A, Paul C, Molloy S, Hultsch T, Graeber M, Cherill R, de Prost Y; Flare Reduction in Eczema with Elidel (Children) Multicenter Investigator Study Group. Efficacy and safety of pimecrolimus cream in the long-term management of atopic dermatitis in children. Pediatrics. 2002 Jul; 110(1 Pt 1):e2. PubMed
14. Buccolo LS. Severe rash after dermatitis. J Fam Pract. 2004 Aug; 53(8):613-5. PubMed
15. Brook I, Frazier EH, Yeager JK. Microbiology of infected eczema herpeticum.J Am Acad Dermatol. 1998 Apr; 38(4):627-9. PubMed
© 2008 Dermatology Online Journal

