Fluoroscopy-induced chronic radiation dermatitis: A report of three cases
Published Web Location
https://doi.org/10.5070/D39c24v99hMain Content
Fluoroscopy-induced chronic radiation dermatitis: A report of three cases
Michelle F Henry MD, Jennifer L Maender MD, Yang Shen MD, Jaime A Tschen MD, Paul Subrt MD, Jimmy D Schmidt MD, Sylvia Hsu
MD
Dermatology Online Journal 15 (1): 3
Department of Dermatology, Baylor College of Medicine, Houston, Texas. shsu@bcm.eduAbstract
We report these cases to emphasize the importance of recognizing fluoroscopy as a cause of radiation dermatitis. The diagnosis of fluoroscopy-induced chronic radiation dermatitis should be raised when patients present with morpheaform, telangiectatic, or ulcerative skin findings in the characteristic locations.
Case one
A 57-year-old Caucasian woman presented to her dermatologist with a 12-year history of a red, painful, pruritic patch of skin located on her right subscapular area. Her dermatologist's initial clinical impression was that of radiation dermatitis; however, the patient denied a history of cancer or radiation exposure. Two 4-mm punch biopsies were performed. With no past medical history of radiation exposure, the dermatopathologist interpreted the specimens as morphea. When the patient was informed of her diagnosis, she became upset fearing that she would develop scleroderma. Her dermatologist reassured her that that was not the case and referred her to the medical center.
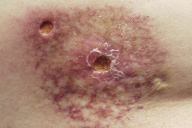
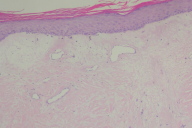
On examination, the patient had a well-demarcated angular reticulated erythematous atrophic plaque with overlying telangiectasia of the right subscapular back (Fig. 1). Suspecting fluoroscopy-induced radiation dermatitis, we specifically asked her if she had had any type of cardiac procedure. The patient then revealed that she had had a myocardial infarction 12 years earlier with subsequent cardiac catheterization that lasted 4-5 hours due to complications. Thinking it was unrelated, the patient had not provided this history to her previous dermatologist even though the lesion appeared shortly after her procedure. The evolution of the lesion was that one week after the procedure, the patient noted redness and pruritus. During the following weeks, the patch enlarged and blisters appeared. Over the years the area became more violaceous and atrophic; the patient experienced increasing pruritus and pain. She denied a history of ulceration. With this new history, the dermatopathologist interpreted the skin biopsy as chronic radiation dermatitis (Fig 2).
Case two
 |
| Figure 3 |
|---|
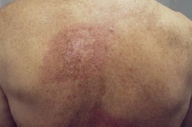
| Figure 3. A rectangular, erythematous, indurated plaque on the right side of his back immediately below the scapula |
A 73-year-old Caucasian man was sent to us from his cardiologist for a rash below his right scapula that had been present for almost 2 months. Two months earlier, the patient had undergone a fluoroscopy procedure in which he had 4 coronary artery stents placed. The procedure was supposed to last 1.5 hours, but due to complications, it lasted 4.5 hours. Since the rash appeared on only one side of his back, his cardiologist diagnosed the patient with shingles and prescribed valacyclovir. On examination, there was a rectangular erythematous indurated plaque on the right side of his back immediately below the scapula (Fig. 3).
Case three
A 69-year-old Caucasian male with a significant history of coronary artery disease underwent a cardiac catheterization with subsequent placement of 4 coronary artery stents in 1989. The duration of the procedure was approximately 4 hours, during which multiple fluoroscopy images were obtained. He experienced no immediate complications, but 3 days post-intervention the patient developed an intensely pruritic erythematous eruption on the left upper paramedial back. The lesion progressed into a large reticulated, erythematous, indurated plaque within one week. He was given topical steroid ointments with some relief of the pruritus and induration, but the reticulated discoloration remained unchanged. Physical examination over fifteen years later revealed a well demarcated reticulated 12 cm x 16 cm erythematous plaque on the left upper back with central atrophy consistent with radiation dermatitis.
Discussion
According to CDC reports in 2002, an estimated 657,000 percutaneous transluminal coronary angioplasty (PTCA) procedures were performed in adults in the United States. The rate of coronary artery stent insertion increased from 157 to 318 per 100,000 adults, aged 45-64, from 1996 to 2000. Fluoroscopy is a method of radiography in which the image is formed on a fluorescent screen such as a television monitor, instead of a traditional film [1]. This produces a continuous image which is of value when studying moving structures, such as the heart and vasculature. Interventional fluoroscopy uses this ionizing radiation to guide small instruments such as catheters through blood vessels or other pathways in the body [2]. Interventional fluoroscopy has experienced a significant increase in the number of diagnostic and therapeutic applications during the past few years and continued growth is expected. Consequentially, the complexity of the procedures has been increasing. This increase leads to lengthier procedures, allowing for higher radiation doses for patients, predisposing them to side effects of high dosage radiation exposure, including skin injuries. Such skin injuries, termed fluoroscopy-induced chronic radiation dermatitis (FICRD) usually appear within 7-14 days of exposure and may be acute or chronic. Chronic radiodermatitis is a non-stochastic reaction. Thus, a certain threshold attained at once or in cumulative doses of irradiation causes inflammation of the skin, presenting as erythema, pain, and pruritus that may later transform into ulceration, atrophy, telangiectasia, sclerosis, discoloration, and malignancy, such as invasive basal cell or squamous cell carcinoma [3]. Fluoroscopy-induced chronic radiation dermatitis has also been associated with breast cancer [4]. Mossman et al. report that the risk of radiation-induced cancer death approximates 10-4 per cGy (rad) [5]. In 2004, it was reported that 0.9 percent of cancers in the US could be caused by diagnostic X-rays, almost double the 1981 estimate of 0.5 percent of cancer mortality [6].
In 1994, the FDA provided information to physicians stating that severe skin radiation injuries had been reported as a result of fluoroscopic imaging during interventional radiologic procedures. Implicated procedures were PTCA, radiofrequency cardiac catheter ablation, vascular embolization, stent and filter placement, thrombolytic and fibrinolytic procedures, and percutaneous transhepatic cholangiography [7]. Physicians providing these procedures were alerted that FICRD should be considered in patients who complained of skin sequelae after exposure to ionizing radiation.
Fluoroscopy-induced chronic radiation dermatitis is an often misdiagnosed complication of fluoroscopic procedures. The onset of symptoms is not predictable and may develop months to years after radiation exposure. According to Miller et al., skin injury is a deterministic effect of radiation in that once a threshold has been exceeded through localized radiation exposure the severity of the injury at that point increases with increasing dose. The threshold for erythema is 2 Gy, whereas permanent hair loss, desquamation, and necrosis occur at doses of 3-10, 7-10, and 12-25 Gy respectively. The exposure necessary to cause FICRD is 10-12 Gy. The average cardiac catheterization exposes the patient to approximately 0.02 to 0.05 Gy/minute, but may range from 0.01 to 0.5 Gy/minute [8]. In our cases, it can be assumed that the radiation exposures were considerably higher because the standard procedure lasts for 1 to 2 hours compared to the 4- to 5-hour procedures for our patients.
It is important to note that, although the reported threshold for skin erythema is 2 Gy, this is often an arbitrary number because there are a number of factors that may cause the individual patient to be more or less sensitive to radiation exposure. Biologic factors, such as diabetes mellitus, systemic lupus erythematosus, scleroderma, or mixed connective tissue disease, and homozygosity for ataxia telangiectasia, have increased sensitivity and potential for severe skin reactions [8]. Closer monitoring in the field of radiology – by providing fluoroscopic devices that estimate the amount of radiation received by focal areas of skin – would generate helpful indices to stratify patient risk after undergoing these procedures. This technology is required by the European Union and is readily available in the United States. Universal adoption of such practices could promote minimization of radiation exposure, therefore decreasing the incidence of FICRD and increasing awareness of post-fluoroscopy adverse events.
Histopathologic findings from skin biopsy are variable depending on the elapsed time since exposure to the ionizing radiation. However, common findings of chronic radiation dermatitis include thickened, sclerotic collagen bundles with sparse proliferation of hyperchromatic fibroblasts, loss of adnexal structures, and reduction or shrinkage of adipose tissue. Dilated superficial vessels may be present when telangiectasia is seen clinically. These findings can be confused with other processes such as morphea or graft versus host disease.
Stone et al. report that neither routine histopathology nor immunohistochemistry can reliably distinguish subacute radiation dermatitis and other conditions, again highlighting the importance of thorough history taking [9]. Erythema ab igne due to use of heating pads can also be considered in the clinical differential diagnosis of reticulated patches. In addition to the patient's past medical history, there are a number of features that are highly suggestive of FICRD. The characteristic location involves the right or left scapular or subscapular region, the right midaxillary trunk, midback, or the right anterolateral chest [5]. The shape is often geometric or angulated. The complaints patients most commonly report are pain, pruritus, ulceration, and discoloration.
Treatment of FICRD is tailored to the severity of the skin findings. First-line therapies include topical and intralesional corticosteroid administration, whereas ulcerated or sclerotic lesions limiting mobility may require surgical excision with musculoskeletal skin flap repair.
The diagnosis of some dermatological disorders is not always straightforward. The histological findings of FICRD are sometimes misleading. Taking a good dermatological history is crucial and may be the only way to determine causation. Raising the level of suspicion for a diagnosis of FICRD is indicated when patients present with morpheaform, telangiectatic, or ulcerative skin findings in the characteristic locations for fluoroscopy-related exposure to ionizing radiation. We report these cases to emphasize the importance of recognizing fluoroscopy as a cause of radiodermatitis and to stress that early diagnosis of FICRD helps to avoid unnecessary treatment and ensures proper surveillance for malignant transformation.
References
1. Simon G, Wightman A, editors. Clinical Radiology. 4th ed. UK: Butterworth & Co Ltd, 1983.2. National Cancer Institute. Avail from: http://www.cancer.gov/cancertopics/interventionalfluoroscopy /allpages. (2008 Jan 15).
3. Aerts A, Decraene T, van den Oord JJ, et al. Chronic radiodermatitis following percutaneous coronary interventions: a report of two cases. J Eur Acad Dermatol Venereol 2003; 17(3): 340-3. [PubMed]
4. Schwartz RA, Burgess GH, Milgrom H. Breast carcinoma and basal cell epithelioma after x-ray therapy for hirsutism. Cancer 1979; 44(5): 1601-5. [PubMed]
5. Mossman K. Analysis of risk in computerized tomography and other diagnostic radiology procedures. Comput Radiol 1982; 6(5): 251-6. [PubMed]
6. Berrington de González A, Darby S. Risk of cancer from diagnostic X-rays: estimates for the UK and 14 other countries. Lancet 2004; 363(9406): 345-51. [PubMed]
7. Food and Drug Administration. Public health advisory: avoidance of serious x-ray-induced skin injuries to patients during fluoroscopically-guided procedures. Rockville, Md: Center for Devices and Radiological Health, 1994.
8. Miller DL, Balter S, Noonan PT, Georgia JD. Minimizing radiation-induced skin injury in interventional radiology procedures. Radiology 2002; 225(2): 329-36. [PubMed]
9. Stone MS, Robson KJ, LeBoit PE. Subacute radiation dermatitis from fluoroscopy during coronary artery stenting: evidence for cytotoxic lymphocyte mediated apoptosis. J Am Acad Dermatol 1998; 38(2 Pt 2): 333-6. [PubMed]
10. Frazier TH, Richardson JB, Fabre VC, Callen JP. Fluoroscopy-induced chronic radiation skin injury: a disease perhaps often overlooked. Arch Dermatol 2007; 143(5): 637-40. [PubMed]
© 2009 Dermatology Online Journal