Lichen planus actinicus
Published Web Location
https://doi.org/10.5070/D398k4v2zxMain Content
Lichen planus actinicus
Gene H Kim MD, Radha Mikkilineni MD
Dermatology Online Journal 13 (1): 13
New York University Department of DermatologyAbstract
A 53-year-old woman presented for evaluation and treatment of discrete, violaceous, annular plaques on the forehead and cheeks. The biopsy specimen and the clinical presentation were consistent with lichen planus actinicus. Lichen planus actinicus is a photosensitive variant of lichen planus that can present with annular, melasma-like, dyschromic, or violaceous plaques in sun-exposed areas. The clinical manifestations of lichen planus actinicus and treatments are discussed.
Clinical synopsis
A 53-year-old woman presented to the Charles C. Harris Skin and Cancer Pavilion for evaluation and treatment of several, discrete plaques on the forehead and cheeks. She first developed the plaques in the summer 3 years ago. She initially experienced pruritus that subsequently diminished. She was previously treated with chemical peels, hydroquinone, and 2.5 percent hydrocortisone cream with some improvement. She denied using any systemic medications prior to the onset of the eruption.
On the forehead and cheeks, there were annular plaques with a violaceous, minimally scaly rim and central hyperpigmentation. The wrists, mucous membranes, axillae, and nails were normal.
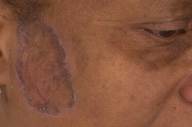 | 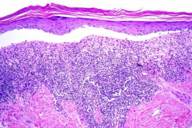 |
| Figure 1 | Figure 2 |
|---|---|
Histopathology reveals a dense band-like lymphocytic infiltrate in the superficial papillary dermis with scattered melanophages. In the epidermis, there is wedge-shaped hypergranulosis, compact orthokeratosis, and apoptotic keratinocytes along the basal layer. There is prominent clefting at the dermo-epidermal junction
Comment
Lichen planus (LP) is an idiopathic inflammatory disorder of the skin and mucous membranes that is typically characterized by pruritic, violaceous papules and plaques. Several clinical variants of lichen planus have been described, which include annular LP, linear LP, hypertrophic LP, atrophic LP, vesiculobullous LP, erosive LP, lichen planopilaris, lichen planus pigmentosus, and lichen planus actinicus [1].
Lichen planus actinicus is thought to be a photosensitive variant of lichen planus that occurs primarily on sun-exposed areas. It is also known as LP subtropicus, LP tropicus, lichenoid melanodermatitis, and summertime actinic lichenoid eruption. The majority of reported cases have occured in young adults of Middle Eastern descent [2].
Clinically, the presentation of lichen planus actinicus can be quite variable, with four morphologic patterns described: annular, dyschromic, classic plaque-like, and pigmented. The most common form is the annular type, which tends to have associated hyperpigmentation. In the dyschromic type, small, white angular papules coalesce into plaques on the neck and dorsa of the hands. The classic plaque-like form presents as violaceous papules in sun-exposed areas. The pigmented form has melasma-like patches on the face and neck. Unlike classic lichen planus, pruritus, the Koebner phenomenon, and mucous-membrane involvement are not common features of lichen planus actinicus [2, 3, 4].
The pathogenesis of lichen planus actinicus is not understood; however, ultraviolet radiation appears to be an important inciting factor. In some patients with lichen planus actinicus, lesions have been induced with ultraviolet provocation [2, 5, 6]. Ultraviolet radiation may be critical in the expression of altered self-antigens on basal keratinocytes that allows for the recruitment of cytotoxic T-cells and the characteristic histopathologic changes. Similar to classic lichen planus, on histopathologic examination, hyperkeratosis, wedge-shaped hypergranulosis, and necrotic keratinocytes are present, with a band-like lymphocytic infiltrate and pigment incontinence. Epidermal atrophy, however, may be more prominent in lichen planus actinicus [4].
The differential diagnosis of lichen planus actinicus includes discoid lupus erythematosus, polymorphous light eruption, granuloma annulare, sarcoidosis, melasma, and erythema dyschromicum perstans. A lichenoid drug eruption should be excluded by history.
Treatment strategies for lichen planus actinicus are based primarily on anecdotal reports but should include the use of sunscreens and sun avoidance. Hydroxychloroquine, intralesional glucocorticoids, and acitretin with topical glucocorticoids have been used successfully in patients with lichen planus actinicus [3, 7, 8]. Traditional therapies used for classic lichen planus such as cyclosporin and systemic glucocorticoids have not been reported.
References
1. Boyd A, Neldner K. Lichen planus. J Am Acad Dermatol 1991;25:5632. Isaacson, D, et al. Summertime actinic lichenoid eruption (lichen planus actinicus). J Am Acad Dermatol 1981;4:404
3. Jansen T, et al. Lichen planus actinicus treated with acitretin and topical corticosteroids. J Eur Acad Dermatol Venereol 2002;16:174
4. Meads SB, et al. Lichen planus actinicus. Cutis 2003;72:377
5. Van der Schroeff JG, et al. Induction of actinic lichen planus with artificial light sources. Arch Dermatol 1983;119:498
6. Katzenellenbogen I. Lichen planus actinicus (lichen planus in subtropical countries). Dermatologica 1962;124:10
7. Dilaimy M. Lichen planus subtropicus. Arch Dermatol 1976;112:1251
8. Zanca A, Zanca A. Lichen planus actinicus. Int J Dermatol 1978;17:506
© 2007 Dermatology Online Journal

