Genital primary herpetic infection in an infant: Clinical features, diagnosis and management
Published Web Location
https://doi.org/10.5070/D39102m0s1Main Content
Genital primary herpetic infection in an infant: Clinical features, diagnosis, and management
Rym Kort Khaddar1, Talal Badri2, Aoutef Ben Hassen1, Saadia Bouraoui3, Amel Souissi2, Naoufel Ben Tekaya2, Amel Ben Osmen Dhahri2
Dermatology Online Journal 11 (3): 22
1. Dermatology department, Ben Arous Hospital, Tunis, Tunisia. rymkort@yahoo.fr2. Dermatology department, Rabta Hospital,
1007 Tunis, Tunisia. 3. Dermatopathology department, Rabta Hospital 1007 Tunis, Tunisia.
Abstract
Genital herpes is a rare disease in infants and is mainly associated with herpes simplex virus (HSV) type 1. Asymptomatic carriers are frequently implicated as transmitters of the disease. Clinical manifestations are the main criteria for diagnosis, However, type-specific serologies and PCR are the most sensitive techniques for detecting HSV. Genital herpes is treated with local or systemic antiviral therapy depending on the severity of the infection. Reducing transmission relies on counseling patients. The disease prognosis is correlated with the underlying immunological status. We report a case of genital primary herpetic infection in an infant.
Introduction
Mucocutaneous herpes is a chronic and recurrent contagious disease associated with Herpes simplex virus (HSV) type 1 or 2. Typical progression is a primary infection followed by a latent phase and then by a reactivation phase that may or may not be symptomatic [1]. In its genital location, it is sexually transmitted and is mainly due to HSV-2 [2].
During childhood, HSV genital transmission results from auto-inoculation or from persons who are infected with HSV-1 rather than HSV-2 [3, 4].
We report a case of genital primary herpetic infection in an infant and discuss the epidemiology, clinical characteristics, and management of this condition.
Clinical synopsis
The patient is a 15-month-old rural female infant, with no personal history of atopy. She presents with a 7-day painful vesicular genital eruption containing a clear fluid, associated with fever and urinary discomfort.
The mother revealed suffering from recurrent labial herpes eruption. The last outbreak had occurred a few days before and resolved spontaneously.
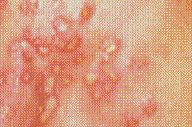
On cutaneous examination, we noted 1-5 mm vesicles, pustules, ulcers and crusts that were solitary or grouped in small bunches within an erythematous base (Fig. 1). These lesions were located in the groin, perineum, labia majora, and around the anus (Fig. 2). There were no similar cutaneous or oral lesions elsewhere. No satellite lymphadenopathy and no further anomalies on physical examination were observed.
|

|
| Figure 1 | Figure 2 |
|---|---|
| The findings suggested a diagnosis of genital herpes. | |
Tzanck cytodiagnosis showed many neutrophils and eosinophils with giant multinucleated cells, consistent with the cytopathogenic effect of herpes virus group. Serologic testing showed a rise in the titer of HSV-specific IgM antibodies over a 15-day period and negative IgG antibodies, confirming the diagnosis of primary herpetic infection. Cell culture and polymerase chain reaction were not available.
Treatment with topical acyclovir (five times daily for 5 days), daily applications of topical antiseptics, and systemic analgesics was followed by a rapid healing of the lesions. No recurrence was observed 6 months later. Topical acyclovir was prescribed to the mother as prevention.
Discussion
During childhood, primary herpetic infection is more commonly the result of HSV-1 than HSV-2 [5, 6]. It is asymptomatic in 88-99 percent of the cases [7]. The average age of disease onset ranges between 2 and 4 years, without any predominance by gender and without seasonal variation. However, as seen in our patient, infection seems to have been promoted by crowding and lack of hygiene.
In children transmission of both HSV-1 and HSV-2 may be inadvertent from someone with an oral infection. In fact, 8 percent of HSV asymptomatic carriers are found to excrete the virus in their saliva [1]. HSV-2 is less commonly involved in oral lesions [9]. Indirect transmission of HSV may occur from clothing, plastic materials, aerosols, towels, and toilet seats [1], but such transmission is probably rare because of the short survival of HSV outside human body. In our patient, contamination resulted from indirect contact with the mother who had a history of recurrent labial herpes. HSV venereal contamination in children raises forensic problems. This condition is more frequently observed in children between the ages of 6 and 12 [7, 10] and is mainly associated with HSV-2 rather than HSV-1 [7].
The diagnosis of genital primary herpetic infection is made clinically [3, 9, 11]. Following a 2-12 day incubation period, there is the sudden onset of a painful vesicular eruption that quickly evolves to ulcers and erosions within a swollen genital mucous membrane. The eruption is associated with fever and malaise and may involve the perineum [3]. Urinary disorders may occur [3]. At times HSV-1 genital primary infection is associated with herpetic gingivo-stomatitis or cutaneous herpes, suggesting auto-inoculation transmission [7].
Laboratory investigations are justified in infants because of the rarity of this condition at this age [7]. Tzanck cytodiagnosis is a nonspecific test that provides evidence favoring the presumptive diagnosis [8]. Serologic tests for Herpes simplex confirms the primary herpetic infection, showing a rise in the titer of HSV-specific IgM antibodies over a 15-day period [2, 3, 11]. This immunologic test is not commonly used because of the delay in diagnosis (15-20 days). More specific evaluation of cell smears, such as direct and indirect immunofluorescence, ELISA, and polymerase chain reaction allow rapid detection and distinguish between HSV-1 and HSV-2 [9]. The detection of HSV in mucocutaneous lesions using specific monoclonal antibodies is the reference method and it allows the virus type determination [2, 3, 9, 11]. However, the samples have to be transferred quickly to the laboratory because HSV is fragile.
The differential diagnoses of our patient included staphylococcal impetigo, fungal infection, herpes-zoster eruption, and post-traumatic lesions. Our diagnosis from the clinical presentation was confirmed by serology.
Primary herpetic infection is usually a mild disease of short duration and with favorable outcome [3, 9]. In children the disease prognosis does not depend on the HSV type but only on the underlying immunological status [7, 12]. In a child with atopic dermatitis, the primary herpetic infection occurs earlier (average age 18 months), the lesions are more widespread (cutaneous, ocular) and may have necrotic and hemorrhagic aspects (so called Kaposi-Juliusberg syndrome [7]).
Early treatment with acyclovir is efficient in HSV infections [9, 13]. Intravenous treatment is not indicated in the absence of local complications or systemic involvement. Long-term followup and preventive treatment of asymptomatic carriers are recommended because of the risk of recurrence. Until now, vaccination for preventing herpetic infections is not available (8, 14).
Conclusion
Primary herpes infection in infancy is rare and is mainly associated with HSV-1 that is usually transmitted by autoinoculation or indirectly. In case of genital location, the diagnosis may be unrecognized and specific or non-specific laboratory examinations may be warranted. Prognosis depends on the underlying immunological status. Treatment should be accompanied by family counseling.
References
1. Moran P. Histoire naturelle de l'infection a herpes simplex de type 1 et 2. Excretion virale asymptomatique. Transmission mere-enfant. Transmission indirecte. Ann Dermatol Venereol 2002;129: 577-85. PubMed2. Berland M. Herpes genital et accouchement. Rev Fr Gynecol Obstet 1991;86(11):639-43. PubMed
3. Jaber K, Zeglaoui F, Goucha S, Fazaa B, Kamoun MR. Infections genitales a herpes simplex. Maghreb Med 1999 Apr;19(335):44-6.
4. Smith JS, Robinson NJ. Age-specific prevalence of infection with herpes simplex virus types 2 and 1: a global review. J Infect Dis 2002 Oct;186(suppl 1):S3-28. PubMed
5. Mertz GJ. Epidemiology of genital herpes infections. Infect Dis Clin North Am 1993 Dec;7(4):825-39. PubMed
6. Enright AM, Prober CG. Neonatal herpes Infection: diagnosis, treatment and prevention. Semin Neonatol 2002 Aug;7(4):283-91. PubMed
7. Taieb A, Body S, Astar I, DuPasquier P, Maleville J. Clinical epidemiology of symptomatic primary herpetic infection in children. A study of 50 cases. Acta Paediatr Scand 1987;76:128-32. PubMed
8. Henrot A. Transmission materno-foetale et indirecte de l'infection HSV, traitement et prevention. Ann Dermatol Venereol 2002;129:533-49. PubMed
9. Thouvenot D, Najioullah F. Herpes simplex de types 1 et 2 (HSV-1 et HSV-2). Rev Prat 1999;49:2203-7. PubMed
10. Anderson C. Childhood sexually transmitted diseases: one consequence of sexual abuse. Public Health Nurs 1995 feb;12(1):41-6. PubMed
11. Straus SE, Rooney JF, Sever JL, Seidlin M, Nusinoff-Lehrman S, Cremer K. NIH conference. Herpes simplex virus infection : Biology, treatment and prevention. Ann Intern Med 1985;103:404-19. PubMed
12. Whitley RJ. Herpes simplex virus infection. Semin Pediatr Infect Dis 2002 Jan;13(1):6-11. PubMed
13. Nikkels AF, Pierard GE. Treatment of mucocutaneous presentations of herpes simplex virus infections. Am J Clin Dermatol 2002;3(7):475-87. PubMed
14. Stanberry LR. Herpes. Vaccine for HSV. Dermatol Clin 1998 Oct;16(4):811-6. PubMed
© 2005 Dermatology Online Journal

