Eruption of bullae within psoriatic plaques: A rare adverse effect of narrow-band ultraviolet B (NB-UVB) phototherapy
Published Web Location
https://doi.org/10.5070/D38w32p0wbMain Content
Eruption of bullae within psoriatic plaques: A rare adverse effect of narrow-band ultraviolet B (NB-UVB) phototherapy
Kristen Corey1 BS, Nikki A Levin1 MD PhD, Michelle Hure2 MD, April Deng2 MD PhD, Jeffrey Mailhot1 MD
Dermatology Online Journal 18 (6): 3
1. Division of Dermatology2. Division of Dermatopathology
University of Massachusetts Medical School, Worcester, Massachusetts
Abstract
The sudden eruption of bullae within psoriatic plaques is an uncommon adverse effect of narrow-band UVB phototherapy (TL-01 radiation). We report the case of a 49-year-old man who developed a bullous eruption after several NB-UVB treatments and will review important aspects of this unusual phototherapy complication.
Introduction
Narrow-band UVB phototherapy from TL-01 lamps is currently a first-line therapy for the treatment of moderate to severe plaque-type psoriasis [1]. Although it is more effective than broadband UVB, higher dosages of radiation are required and a steeper curve of phototoxicity has been observed when therapeutic doses are exceeded [2]. A rare phototoxic reaction unique to narrowband UVB phototherapy involves a blistering eruption strictly confined to psoriatic plaques. To our knowledge, only 11 cases of this distinct eruption have been described in the literature to date [3, 4]. We report a case of this eruption in order to reinforce the clinical, histopathologic, and pathogenetic features of this condition. In doing so, we aim to illustrate the fine threshold between the efficacy and toxicity of narrow-band UVB radiation.
Case report
A 49-year-old Vietnamese man who had a 4-month history of severe guttate and plaque-type psoriasis involving 40 percent of his body surface area was being treated with narrowband UVB phototherapy when he presented acutely to clinic with numerous pruritic blisters located within psoriatic plaques on his trunk and extremities. He developed the blistering eruption while he was at work near a 400-degree furnace in an airplane manufacturing facility one day after his 23rd phototherapy treatment. He had been experiencing significant improvement in his psoriasis on a biweekly (Tuesday and Thursday) phototherapy protocol for skin type IV at a dose of 2.7 joules/cm² (cumulative dose of 42.8 joules/cm²) when the blisters occurred. He was otherwise healthy and was taking neither photosensitizing agents nor any other oral medications; he was using only topical triamcinolone 0.1 percent cream as needed for pruritus.
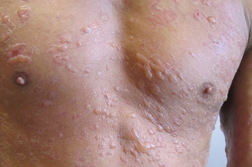
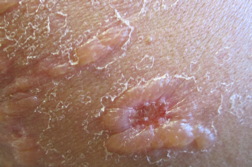
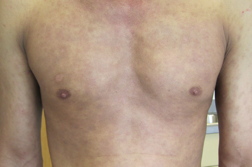
His physical examination revealed numerous thin, erythematous, scaly plaques of psoriasis distributed symmetrically over his trunk and upper and lower extremities. Located within many of these psoriatic plaques were serous fluid-filled, tense and flaccid bullae (Figure 1). Some of the bullae, particularly on his upper chest, were arranged in an annular configuration at the periphery of psoriatic plaques (Figure 2). The skin surrounding the psoriatic plaques was completely free of bullae, lacked erythema or desquamation, and otherwise appeared normal. His face, scalp, neck, palms, soles, and mucosa were spared.
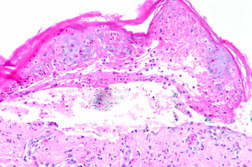
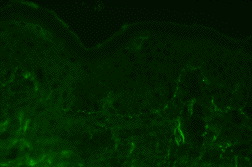
Laboratory tests including a complete blood count, comprehensive metabolic panel, and thyroid stimulating hormone were unremarkable except for a microcytic anemia. A punch biopsy of lesional skin revealed a subepidermal separation with epidermal necrosis and apoptotic keratinocytes, accompanied by a superficial mixed inflammatory infiltrate including eosinophils (Figure 3). There was underlying re-epithelialization. Direct immunofluorescence from a perilesional punch biopsy was negative except for faint granular C3 deposition along the basement membrane zone (Figure 4).
The differential diagnosis included immunobullous disorders, particularly bullous pemphigoid (related to the finding of C3 deposition along the basement membrane zone), linear IgA bullous disease, heat-induced bullae, phototherapy-induced burn, bullous erythema multiforme or drug eruption, and pseudoporphyria. None of these diagnoses, however, could explain why the bullae were confined to psoriatic plaques completely sparing surrounding normal skin. A subsequent literature search revealed that such bullae limited to psoriatic plaques can occur as a rare adverse effect of narrowband UVB phototherapy producing clinical and histopathologic features consistent with our patient’s picture [3, 4].
Our patient’s phototherapy was discontinued at the time of his presentation and he was prescribed betamethasone diproprionate 0.05 percent cream to use twice daily. His bullae resolved within one week at which point he was restarted on phototherapy at 50 percent of his prior dose (1.3 joules/cm² with an increase of 75 mJ/cm² per treatment), because published reports indicate that blisters improve even on continued phototherapy [3, 4]. In follow-up at our clinic, the patient has shown complete clearing of his psoriasis without recurrence of bullae (Figure 5).
Discussion
The sudden eruption of blisters within psoriatic plaques represents an unusual adverse event observed only during narrow-band UVB phototherapy. As outlined in previous studies and highlighted by our case, bullae typically appear after a patient has completed several phototherapy treatments (23 in our patient’s case, 6-28 in the study by Calzavara-Pinton et al) and experienced significant overall improvement in psoriasis [4]. Only one out of ten patients in prior case reports had skin type IV like our patient; most had skin types I or II, suggesting that those with lighter skin types may be at higher risk of developing bullae or that the populations studied had predominantly lighter skin types [3, 4]. Routine laboratory tests are usually negative and skin biopsies show junctional blisters with epidermal necrosis and mild perivascular inflammation; direct immunofluoroscence studies are negative. Interestingly, our case showed keratinocytic necrosis and granular C3 deposition along the basement membrane zone, indicating complement-mediated epidermal damage. The course is benign and no treatment is required; blisters disappear within 5-7 days and phototherapy can be successfully resumed at lower doses.
Although the pathogenesis is unknown, previous reports have hypothesized that a combination of two factors is likely involved: 1) a change in the photoprotective properties of skin as psoriasis clears during the course of NB-UVB phototherapy and 2) the narrow therapeutic index or steep curve of phototoxicity associated with NB-UVB. This theory proposes that NB-UVB therapy leads to rapid desquamation and reduction of acanthosis without the concomitant development of photoprotective measures (thickened stratum corneum, increased pigmentation) within psoriatic plaques. Surrounding skin, however, has acquired such defensive measures thereby allowing increased, supra-therapeutic dosages of NB-UVB radiation to penetrate vulnerable psoriatic plaques [3, 4]. Thus at some critical point after a certain number of phototherapy treatments, psoriatic skin is exposed to a burning dose of NB-UVB radiation, resulting in blisters. This event is unique to NB-UVB radiation because of its higher risk of photo-damaging effects beyond therapeutic doses when compared to broadband UVB. Gentler irradiation protocols with less frequent treatments may reduce the risk of this blistering eruption but would also result in slower rates of psoriasis clearance.
Notably, all previous reported cases of blistering occurred in Europe under a minimal erythema dosing (MED), triweekly treatment protocol. To our knowledge, a bullous eruption occurring under a skin type protocol has not been reported, which is surprising given that skin type protocols are considered less precise than MED-based protocols [5]. Perhaps the actual incidence of this eruption is higher, but patients do not seek medical treatment given the benign course and rapid resolution of blisters. This phenomenon may also be more widely recognized in Europe where NB-UVB phototherapy has been used as a popular psoriasis therapy for longer than in the United States.
In conclusion, the eruption of bullae within psoriatic plaques is a rare side effect of narrowband-UVB phototherapy with characteristic clinical and histopathological features and a relatively benign course. Proposed pathogenetic mechanisms underlying blister formation demonstrate the qualities of NB-UVB radiation to be both highly effective and potentially phototoxic at increasing doses. Because narrow-band UVB phototherapy is widely used as a first-line therapy for extensive psoriasis based on its superior efficacy to broad-band UVB and better safety profile than PUVA, clinicians may easily overlook the capacity of this type of radiation to induce damage above therapeutic doses, a phenomenon which is emphasized by this case report.
References
1. Lapolla W, Yentzer BA, Bagel J, Halvorson CR, Feldman SR. A review of phototherapy protocols for psoriasis treatment. J Am Acad Dermatol. 2011 May;64(5):936-49. [PubMed]2. Coven TR, Burack LH, Gilleaudeau R, Keogh M, Ozawa M, Krueger JG. Narrowband UV-B produces superior clinical and histopathological resolution of moderate-to-severe psoriasis in patients compared with broadband UV-B. Arch Dermatol. 1997 Dec;133(12):1514-22. [PubMed]
3. George SA, Ferguson J. Lesional blistering following narrow-band (TL-01) UVB phototherapy for psoriasis: a report of four cases. Brit J Dermatol. 1992; 127: 445-46. [PubMed]
4. Calzavara-Pinton PG, Zane C, Candiago E, Facchetti F. Blisters on psoriatic lesions treated with TL-01 lamps. Dermatology. 2000; 200: 115-19. [PubMed]
5. Schneider LA, Hinrichs R, Scharffetter-Kochanek K. Phototherapy and photochemotherapy. Clin Dermatol. 2008 Sep-Oct;26(5):464-76. [PubMed]
© 2012 Dermatology Online Journal