Café au lait has hue of its own
Published Web Location
https://doi.org/10.5070/D38pq4j4ndMain Content
Café au lait has hue of its own
Edith Orion, MD1 Hagit Matz, MD1,2 Danny Wolf, MD3 Ronni Wolf MD1
Dermatology Online Journal 9 (5): 8
1. The Dermatology Unit, Kaplan Medical Center, Rechovot 2. Tel-Aviv Sourasky Medical Center, and the Sackler Faculty of Medicine,
Tel-Aviv University, Tel-Aviv 3. Pediatric Outpatient Clinic, Kupat Holim Clalit, Hasharon Region, Israel. wolf_r@netvision.net.il
Abstract
Segmental pigmentation disorder is a pigmentation disorder (hypo- or hyperpigmentation) first described some 20 years ago. It appears early in life, is segmental, and usually has a sharp border in the midline. It can be confused clinically and histologically with several pigmentary disorders, especially with giant or segmental café-au-lait macules. The purpose of this article is to promote, revive, and refresh this somewhat neglected entity, and to further subdivide it into two types: segmental pigmentation disorder simplex and segmental café-au-lait. We illustrate our contention with case reports.
Introduction
"The ill and unfit choice of words wonderfully obstructs the understanding" [Sir Francis Bacon Novum Organum, "Aphorisms, XLIII"]; whereas precision and clearness in language reflects precision in thought.
Clinical dermatology has always been and still is a descriptive and morphologic specialty. Therefore, more than any other discipline, dermatology needs to observe the highest standards of clarity and precision in the terms, classification and nomenclature it uses, integrating both morphology and etiology.
We applaud Metzker et al. for having introduced the term segmental pigmentation disorder (SPD) some 20 years ago to describe pigmentary changes, sometimes with a dermatomal distribution. Although it appeared to be a very practical and useful term for a rather common condition, it never took off and has not received the status it deserved. The purpose of the present article is to promote, revive, and refresh this somewhat neglected entity, and to further subdivide it into segmental pigmentation disorder simplex and segmental café-au-lait. We illustrate our contention in the following case reports.
Report of seven cases
Case 1
|
|
| Figure 1 | Figure 2 |
|---|---|
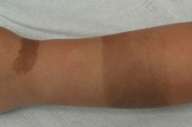
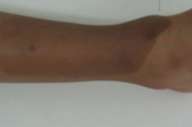
| Fig. 1.—Case 1. Two brown macules on the left arm and wrist. | |
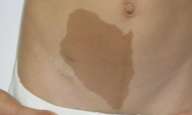
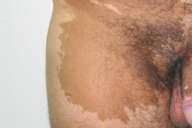
| Fig. 2.—Case 2. Brown macule to the right of the lower abdominal midline. | |
A 3-year-old girl presented from birth with two brown macules on her left arm and wrist (fig.1). The bigger macule on her arm had sharp demarcation lines, not consistent with the dermatomal lines or Blashko's lines. The pigmentation was of café-au-lait color but not completely homo genous, the proximal part being lighter in color. She had a smaller macule on her wrist. There were no other significant cutaneous findings.
Case 2
An 8-year-old boy presented from birth with a brown macule to the right of the lower abdominal midline (fig.2). The pigmentation was café-au-lait in color, and the border of the lesion was smooth, resembling the coast of California. A darker spot at the right lower pole of the macule was noted. The lesion was large enough to cover most of the lower right quadrant of the abdomen and was enlarging proportionately to the boy's growth. There were no other significant cutaneous findings.
Case 3
|

|
| Figure 3 | Figure 4 |
|---|---|
| Fig. 3.—Case 3. Brown macule over the anterior aspect of the right shin. | |
| Fig. 4.—Case 4. Two hyperpigmented, adjacent macules on the right buttock and upper right thigh. | |
A 5-year-old boy presented from birth with a brown macule over the anterior aspect of his right shIn, enlarging proportionately to his growth (fig.3). The macule had smooth borders like the coast of California, and was evenly café-au-lait-pigmented, except for two small darker spots. There was a smaller but similar lesion on the anterior aspect of the right ankle. There were no other significant skin lesions.
Case 4
A 9-year-old boy presented from birth with two hyperpigmented, adjacent macules on his right buttocks and upper right thigh in a dermatomal distribution (fig.4). The macules were café-au-lait in color and had borders like the coast of Maine. Other medical history was of no relevance. These were no other significant cutaneous findings.
Case 5
A 4-year-old boy presented from birth with a hyperpigmented macule over his entire left side of the abdomen, lower anterior chest, and left axilla (fig.5). The lesion had smooth borders, café-au-lait color and a sharp delineation at the midline. The lesion was enlarging proportionally to the boy's growth; yet, a recent lighter area was noted in the middle of the abdominal part of the macule. There were no other cutaneous findings.
Case 6
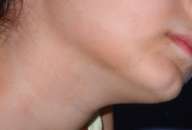
An 11-year-old girl presented with a hyperpigmented macule extending from the right side of the neck, over the clavicle, and down to the shoulder (fig.6); the lesion did not take the precise course of a dermatome or of Blaschko's lines. The macules were pale brown with yellowish tones, evenly pigmented and smooth bordered. The parents could not remember whether the lesion was present at birth. There were no other cutaneous findings.
Case 7
|
| Figure 7 |
|---|
| Fig. 7: Case 7. Hyperpigmented macule on the right lower abdomen, groin, and upper thigh. Note vitiligo macule on glans penis. |
A 40-year-old man presented with vitiligo on the glans penis. Physical examination revealed, apart of the hypopigmented typical lesion of vitiligo on the penis, a hyperpigmented dark macule extending over the right lower abdomen, right groin, and right upper thigh. The lesion was café-au-lait colored and had well-defined irregular borders, like the coast on Maine, with sharp delineation on the midline (fig.7). At the upper part of the macule a streak of normal-colored skin was apparent, and the borders were smoother, like the coast of California. According to the patient, the lesion was noted soon after birth and did not change over the years but did grow proportionally to the natural growth of his body. Apart from these cutaneous findings, he was otherwise healthy.
Medical history of all patients and their families was not significant. No other relevant findings were noted on physical examination in all cases.
In all the above cases, biopsies were taken from the pigmented lesions and, when necessary, from darker spots of the lesions as well. In case 7 the biopsy was performed some 20 years ago, and, although we did not examine the slides, the description was identical to the other biopsies.
All biopsies mentioned were similar and revealed epidermal hyperpigmentation only, with neither elongation of the rete ridges, nor with an excess of melanocytes. There was no evidence on nevus cells in any of the biopsies.
Discussion
In 1983 Metzker et al. described a disorder of pigmentation (hypo- and hyperpigmentation) in the young population of Israel, sometimes with a segmental distribution, and labeled it segmental pigmentation disorder (SPD) [1]. Although occasional case reports of this condition had appeared earlier, these authors were the first to recognize it as a distinct entity. They found it to be a rather common presentation in clinical practice, with an incidence of 0.35 percent, and, in contrast to various other segmental pigmentary disorders, one that was not associated with other lesions of the nervous system. Histologic examination usually reveals basal hyperpigmentation only. According to the authors, the condition tends to fade away spontaneously over time [1]. Because we have classic cases of segmental pigmentation disorders that did not fade over time, we believe that probably some cases do fade and others do not. It certainly needs more investigation and followup for further establishing whether this group is homogeneous or not.
In the literature one can find an array of disorders of pigmentation that are segmental, dermatomal, or running along the lines of Blaschko. They can be either hypo- or hyperpigmented, with or without concomitant disturbances, with no specific histologic features. For example, linear and whorled nevoid hypermelanosis is a descriptive name, given to a sporadic hyperpigmentation disorder that shares the same histologic features as SPD. It is distributed in streaks and whorls along Blaschko's lines and is believed to represent genetic mosaicism, rarely with associated abnormalities [2, 3, 4].
A decade ago, Happle, in his groundbreaking article [5], gave dermatologists a powerful tool to understand the pathological mechanism of various cutaneous findings, among which are pigmentary lesions. It appears that mosaicism, in its various forms, can explain many of the unique cutaneous lesion patterns; nevertheless, more genetic research is needed to further clarify and prove the theory. It is our concern, however, that the etiology of mosaicism has been attributed to too many entities, lacking the necessary scientific evidence for it. Happle has also classified five clinical pigmentary patterns, thus setting the ground for a better understanding of the genetic mechanism behind it [5]. SPD, however, cannot always be sorted clinically according to this classification.
An important disorder of pigmentation, which can be easily confused with SPD, is giant or segmental café-au-lait macules (CALMs). They can be segmental in distribution and may share the same histology as SPD [6]. Here, also, histologic findings may be an increase in melanin content in melanocytes and basal keratinocytes, without melanocytic proliferation. Melanin macroglobules, occasionally seen in café-au-lait macules, are not specific for CALMs and are found in other pigmentary skin lesions [6], so they do not contribute to the diagnosis. Segmental neurofibromatosis (neurofibromatosis type V), although limited to a segment of the body, by definition also exhibits other features of the disease, such as neurofibromas, axillary freckling and smaller, more numerous CALMs [7], and should not be confused with giant or segmental CALMs.
Because of the great difficulties differentiating giant or segmental CALMs from SPD, it may sometimes mistakenly be considered a variant of the latter, especially in the dermatologist's office but also in the literature. It is worth noting that some articles describe SPD but present images of segmental café-au-lait (because SPD is difficult to reproduce photographically; a fact that can be used as an additional tool for diagnosis).
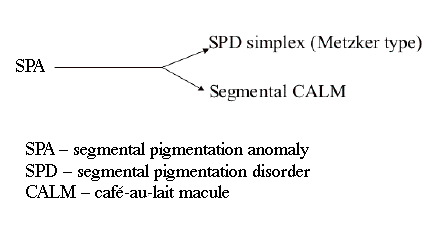
Because the entity of SPD is still a descriptive one, based solely on morphology, it should reflect the true clinical picture and adhere faithfully and authentically to morphology. In other words, we suggest that we call a spade a spade and not a garden implement: a café-au-lait spot is just that, and not a pigmentation disorder. Thus, for sake of morphologic simplicity and accuracy, we suggest that the catch-all term segmental pigmentation disorder be changed to segmental pigmentation anomaly (SPA). The new term can be used as a family name for an array of pigmentation disorders, with or without associated features. The old term SPD should be changed into segmental pigmentation disorder simplex" (Metzker type) and be included under the umbrella of segmental pigmentation anomaly. Segmental café-au-lait is another entity that can reside under this umbrella (fig. 8).
|
| Figure 8 |
|---|
| Fig. 8.—SPA-segmental pigmentation anomaly, CALM-café-au-lait macule. |
Other pigmentation disorders with similar histologic features should be subdivided under this umbrella as well. Further subdivision may include anomalies that do not share the same histology, but form a distinct clinical entity (e.g., nevus depigmentosus).
Finally, we need to ask ourselves whether our patients will gain any benefit from the suggested change in terminology. The answer to this question is not as straightforward as it may appear. At present, neither condition is treatable, nor do they have any known associated defects or known patterns of inheritance. This situation may change, however, if and when we find the underlying specific genetic mutation(s) responsible for these diseases. But a prerequisite for detecting the genetic defects of a disease is the exact description, definition, and classification of it, so as to ensure a homogeneous series of cases with identical genetic predisposition as a basis for further research. "The study of the causes of things must be preceded by the study of things caused" (Hughlings Jackson, a famous English neurologist, who described also Jacksonian epilepsy).
It is our hope that this new classification (terminology) will serve as an effective steppingstone for further genetic and molecular investigations and that the seeds we sow today that will take root and flourish in the future.
We presented six cases illustrating the segmental café-au-lait subdivision and one case of the segmental pigmentation disorder simplex subdivision of SPA to demonstrate the differences.
The time has come to set the record straight.
Acknowledgment: We would like to thank Dr. Bernice R. Krafchik for her important contribution to this article and Esther Eshkol for editorial assistance.
References
1. Metzker A, Morag H, Weitz R. Segmental pigmentation disorder. Acta Dermatol Venereol (Stockh) 1983; 63: 167-169.2. Alvarez J, Peteiro C, Toribio J.Linear and whorled nevoid hypermelanosis. Pediatr Dermatol. 1993 Jun;10(2):156-8. PubMed
3. Mendiratta V, Sharma RC, Arya L, Sardana K. Linear and whorled nevoid hypermelanosis. J Dermatol. 2001 Jan;28(1):58-9. PubMed.
4. Hofmann U, Wagner N, Grimm T, Brocker EB, Hamm H. Linear and whorled nevoid hypermelanosis. Case report and review of the literature. Hautarzt 1998; 49[5]: 408-412. PubMed
5. Happle R. Mosaicism in human skin. Understanding the patterns and mechanisms. Arch Dermatol. 1993 Nov;129(11):1460-70. PubMed.
6. Landau M, Krafchik BR. The diagnostic value of cafe-au-lait macules. J Am Acad Dermatol. 1999 Jun;40(6 Pt 1):877-90. PubMed
7. Hager CM, Cohen PR, Tschen JA. Segmental neurofibromatosis: case reports and review. J Am Acad Dermatol 1997; 37: 864-869. PubMed
© 2003 Dermatology Online Journal