Dermatomyositis
Published Web Location
https://doi.org/10.5070/D38ds380m6Main Content
Dermatomyositis
Lisa M Gruson MD, and David E Cohen MD MPH
Dermatology Online Journal 10 (3): 7
From the Ronald O. Perelman Department of Dermatology, New York University
Abstract
A 51-year-old woman presented with weakness in her arms and legs and an eruption on the dorsal aspects of the hands, upper back, and face. Histopathologic features showed vacuolar alteration of the basal layer, a thick basement membrane, and deposits of connective-tissue mucin in the papillary dermis and the upper reticular dermis. Dermatomyositis is an idiopathic disease that is characterized by specific cutaneous manifestations and myopathy, which may be associated with occult malignancy. Treatment options include corticosteroids and other immunosuppressive agents such as methotrexate, cyclosporine, mycophenolate mofetil, and azathioprine.
Clinical synopsis
History.—A 51-year-old woman noticed an eruption on her face and back, which prompted her to seek an appointment with her dermatologist. She was told she had eczema and was treated with topical glucocorticoids and antihistamines. The eruption did not improve, and she was referred to an allergist for patch tests, which did not yield pertinent findings. She was then referred to New York University Dermatology Associates for further evaluation. At that time she had new lesions on the backs of her hands and weakness in her arms and legs.
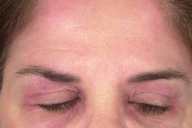
Physical examination.—On the face, diffuse erythema and edema were noted. The eyelids were violaceous and edematous with scattered telangiectases. On the back and shoulders, erythematous plaques with scale were observed. On the hands, the cuticles were frayed and telangiectases were present. There were also flat, violaceous papules on the knuckles of the hands. Muscle strength was 4/5 in all extremities.
|
|
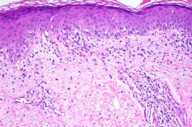
| Figure 1 | Figure 2 |
|---|
Laboratory data.—A complete blood count, chemistry panel, creatine kinase, liver function tests, aldolase, antinuclear antibody, rheumatoid factor, anti-SM antibody, anti-Scl-70 antibody, erythrocyte sedimentation rate, anti-Ro, anti-La and Jo-1 antibodies were normal or negative. A skeletal muscle biopsy specimen of the right calf showed minor changes with probable neurogenic atrophy. Computed-tomography scans of the chest, abdomen, and pelvis; mammograms; and a colonoscopy were normal.
Histopathology.—There is a superficial and mid-perivascular infiltrate predominantly of lymphocytes. The lymphocytes extend to the epidermis where there are vacuolar alterations of the basal cell layer. The basement membrane is thickened, and there is increased amounts of connective-tissue mucin.
Diagnosis.—Dermatomyositis.
Comment:
Dermatomyositis is an idiopathic disease that is characterized by cutaneous manifestations and myopathy. Classic dermatologic findings include Gottron papules, Gottron sign, heliotrope erythema with or without associated edema of the eyelids, the shawl sign, and facial erythema. [1] A study has shown that nailfold capillary diameter in dermatomyositis exceeds that observed in other connective-tissue diseases and in controls.[2] Histologically, an interface dermatitis and a thickened basement membrane are noted with dermal pallor secondary to edema and mucin.[3] The evaluation of muscle disease includes laboratory tests for creatine kinase, aldolase, and lactate dehydrogenase. If these tests are inconclusive electromyography and a muscle biopsy are indicated. [1] Dermatomyositis is also characterized by the production of autoantibodies that include antibodies to 155 KDa and Se antigens, Jo-1, Mi-2, SRP, Pl-12, anti-nuclear antibody, and anti-Ro antibody. [3]
An evaluation for occult malignant conditions is suggested as the incidence of dermatomyositis-associated malignant conditions is estimated to be between 7 and 34 percent. Factors thought to increase the probability of occult malignant conditions include age, refractory disease, female sex, and normal creatine kinase levels. The investigation includes a chest radiograph, colonoscopy, prostate-specific antigen in men, mammography in women, CA-125 levels, and imaging studies of the abdomen and pelvis.[4] Evaluation for occult malignant conditions should be ongoing as reports have shown that there may be a delay of up to five years before cancer develops.[5] Glucocorticoids are the first line therapy for dermatomyositis. Other agents such as methotrexate, cyclosporine, mycophenolate mofetil, and azathioprine may also be used. [1,6]
References
1. Callen JP. Dermatomyositis. Lancet 2000;355:53.2. Sontheimer RD. Cutaneous features of classic dermatomyositis and amyopathic dermatomyositis. Curr Opin Rheumatol 1999;11: 475.
3. Sontheimer RD, Costner MI. Dermatomyositis. In Freedberg IM et al, eds. Dermatology in General Medicine. 6th edition. New York: McGraw-Hill; 2003. PP. 1694-1708 4. Till SH, Jones AC. Dermatomyositis - how far to go! Ann Rheum Dis 1998;57: 198.
5. Zantos D, et al. The overall temporal relationship association of cancer with polymyositis and dermatomyositis. J Rheumatol 1994;21:1855.
6. Oddis, CV. Current approach to the treatment of polymyositis and dermatomyositis. Curr Opin Rheum 2000;12: 492 [18]Back to October 21, 2003 Cases.
© 2004 Dermatology Online Journal

