Parry-Romberg syndrome with coexistent morphea
Published Web Location
https://doi.org/10.5070/D38dk1b0fwMain Content
Parry-Romberg syndrome with coexistent morphea
Tameka K Lane MD, Jessie Cheung MD, Julie V Schaffer MD
Dermatology Online Journal 14 (10): 21
Department of Dermatology, New York UniversityAbstract
We present a 14-year-old girl with a nine-year history of progressive subcutaneous atrophy on the right side of the face, which is consistent with a diagnosis of Parry-Romberg syndrome. The onset of the atrophy was heralded by the development of a morpheaform plaque on the right temple. This case highlights the substantial of overlap of Parry-Romberg syndrome and morphea.
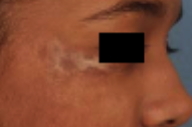 | 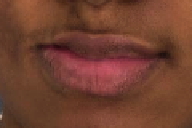 |
| Figure 1 | Figure 2 |
|---|
History
A 14-year-old girl presented to the Pediatric Dermatology Clinic at the Charles C. Harris Skin and Cancer Pavilion in July, 2006, for evaluation of facial asymmetry. At age five, a scar-like plaque appeared on her right temple. This was located lateral to a site of superficial abrasion by a tree branch several months earlier. Over the next eight years, the right side of her face developed progressive hyperpigmentation and subcutaneous atrophy that slowly extended from the upper part of the cheek to the lips to the chin and mandibular area. Associated dental malocclusion was corrected with orthodontic treatment. The patient had no history of seizures or other neurologic abnormalities and she was a good student. Treatment with oral methotrexate was initiated during the summer of 2007, but this medication was discontinued after two months because the disease had been stable for more than a year. Injections of a hyaluronic acid filler into the right side of the upper lip improved the cosmetic appearance and further treatment with autologous fat transfer is planned.
Physical Examination
The face was asymmetric in appearance, with hyperpigmentation and subcutaneous atrophy that extended from the right lower eyelid and temple to the ipsilateral cheek, lips, and chin. An ill-defined, shiny, firm, hypopigmented plaque was evident on the right temple.
Lab
A complete blood count, chemistry panel, erythrocyte sedimentation rate and C-reactive protein level were normal. Antinuclear antibodies were absent.
Histopathology
In a biopsy specimen obtained from the right temple there is a mild perivascular and perifollicular lymphocytic infiltrate and increased dermal thickness with broad collagen bundles in the reticular dermis. (This biopsy specimen was not reviewed by the NYU Dermatopathology Section.)
Comment
Parry-Romberg syndrome (progressive hemifacial atrophy) was initially described by Parry in 1825 and further characterized by Romberg in 1846. The relationship between this condition and the en coup de sabre subtype of linear morphea has been a subject of debate in the medical literature for more than 150 years [1, 2]. Parry-Romberg syndrome classically affects one-half of the face, while en coup de sabre presents as a linear streak that is most often located on the paramedian forehead and scalp. Atrophy of the subcutaneous fat represents the primary process in Parry-Romberg syndrome, whereas dermal sclerosis characterizes linear morphea. However, areas of morpheaform sclerosis (as observed in our patient) are evident in almost three-quarters of individuals with Parry-Romberg syndrome; one-half of Parry-Romberg syndrome patients have coexistent en coup de sabre morphea. Conversely, one-third of en coup de sabre morphea patients have coexistent Parry-Romberg syndrome (Figure) [1]. In addition, both conditions frequently involve the muscle, bone, and even meninges and brain underlying affected areas, with seizures and other neurologic manifestations occurring in 10 to 20 percent of patients with either disorder [1, 3]. Parry-Romberg syndrome and en coup de sabre also share a female-to-male ratio of 2:1 and a predilection for children, with a median age of onset of approximately 10 years [1].
Pharmacologic therapies for Parry-Romberg syndrome have largely been the same as regimens used for the treatment of morphea [4]. For individuals with active en coup de sabre morphea, methotrexate with or without monthly pulses of systemic glucocorticoids is commonly utilized. A variety of surgical interventions can help to correct facial atrophy in patients with Parry-Romberg syndrome (Table) [5].
References
1. Tollefson MM, Witman PM. En coup de sabre morphea and Parry-Romberg syndrome: a retrospective review of 54 patients. J Am Acad Dermatol 2007; 56: 257 PubMed2. Orozco-Covarrubias L, et al. Scleroderma Ôen coup de sabreÕ and progressive facial hemiatrophy: is it possible to differentiate them? J Eur Acad Dermatol Venereol 2002; 16: 361 PubMed
3. Holland KE, et al. Linear scleroderma en coup de sabre with associated neurologic abnormalities. Pediatrics 2006; 117: e132 PubMed
4. Korkmaz C, et al. Beneficial effect of immunosuppressive drugs on Parry-Romberg syndrome: a case report and review of the literature. South Med J 2005; 98: 940 PubMed
5. Guerrerosantos J, et al. Classification and treatment of facial tissue atrophy in Parry-Romberg disease. Aesthetic Plast Surg 2007; 31: 424 PubMed
© 2008 Dermatology Online Journal

