Acrokeratoelastoidosis
Published Web Location
https://doi.org/10.5070/D38c10f289Main Content
Acrokeratoelastoidosis
Mariame Meziane1, Karima Senouci1, Yasmina Ouidane1, Rim Chraïbi1, Tarik Marcil1, Fatima Mansouri2, Badreddine Hassam1
Dermatology Online Journal 14 (9): 11
1. Department of Dermatology, Ibn Sina Hospital, Rabat, Morocco. mariame_meziane@yahoo.fr2. Department of Histopathology, Ibn Sina Hospital, Rabat, Morocco
Abstract
Acrokeratoelastoidosis (AKE) is a rare skin disorder characterized by a papular eruption and fragmentation of elastic tissue that primarily involves the margins of the hands and feet. The most common histopathologic findings of AKE are hyperkeratosis and degeneration of elastic fibers. Various treatment options have been tried with little help or without success. We report the third case of acrokeratoelastoidosis in an Arabic woman localized exclusively to the feet.
Acrokeratoelastoidosis (AKE) is a rare skin disorder characterized by small, hyperkeratotic papules with an occasionally umbilicated surface that coalesce into larger plaques along the margins of the hands and feet. Familial occurrence is frequent as an autosomal dominant trait. The lesion result from decreased and abnormal elastic fibers in the dermis. The most common histopathologic findings of AKE are hyperkeratosis, mild acanthosis, and a decrease in the number (rarefaction) along with fragmentation of elastic fibers within the dermis.
In this report, we will present a patient with this rare condition and review the clinical and histopathologic features, cause, differential diagnosis, and treatments.
Case report
A 42-year-old Arabic women presented with multiple untreated and asymptomatic plaques on her feet. The lesions had first appeared ten years prior to presentation. First, one small papule on her right foot appeared. This increased in size and additional similar papules gradually formed and coalesced to form plaques over the years. The patient had no relevant personal history (no symptoms of hyperhidrosis, medication, excessive sun exposure or trauma) and no member of the family had a similar lesions.
 |
| Figure 1 |
|---|
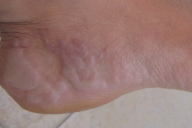
| Figure 1. Clinical photograph revealing violacious papular eruption that arose over lateral margins of soles |
Clinical examination showed multiple papules and plaques clustered symmetrically along the borders of both feet (Fig. 1). Some lesions had a violaceous hue and others were centrally depressed and showed a keratotic surface. There were no lesions on her hands and no hyperkeratosis on palms or soles.
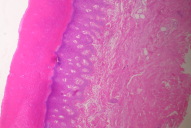
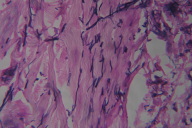
Histological examination of a skin-biopsy specimen taken from a papule on the patient's right foot revealed hyperkeratosis with epidermal acanthosis and hypergranulosis (Fig. 2). Acid orcein stain revealed coarse, fragmented, and rarefied elastic fibers (Fig. 3). These findings were consistent histologically with acrokeratoelastoidosis.
She was treated with topical tretinoin cream to the affected areas on the feet. We obtained partial regression of the disease after two months of treatment.
Discussion
Acrokeratoelastoidosis is a rare autosomal dominant condition first described by Oswaldo Costa in 1953 [1]; only scattered cases have been reported in the literature [2]. Two cases were reported in the north of Africa [3].
The condition exhibits marginal palmoplantar keratoderma characterized by a papular eruption and loss of elastic tissue. The onset of the disease is often in infancy or adolescence but can also begin in adulthood as for our patient [4]. There is no racial or sex predilection, but rapid progression has been reported during pregnancy [5]. The condition has been reported as sporadic and familial; a mode of autosomal dominant transmission is most common, but some recessive forms have been reported [6].
Clinically AKE is characterized by smooth, shiny, firm, and yellowish papules that can arise spontaneously over the dorsal hand and lateral margins of the palms and soles, the space between the thumb and forefinger, the anterior surface of the lower legs, and over the knuckles and nail folds [7]. Rarely the lesions may be violaceous as in our patient [5]. The distribution is generally bilateral, but unilateral forms have been described. An association between AKE and systemic scleroderma has been suggested [8].
Histopathology revealed a reduced number of elastic fibers in the dermis and a high proportion of fragmented fibers among those that were present. Electron microscopic studies have shown that fibroblasts within the reticular dermis are reduced in number and contain abnormal dense granules in or near the plasma membrane. These granules represent precursors of elastin fibers. Combined with sparse adjacent extracellular elastin fibers, this observation has led to the belief that the underlying pathologic process is one of elastorrhexis, not elastoidosis, as the name would imply. The end result would be an abnormal deposition or repair of connective tissue within the affected area [7].
Conditions in the differential diagnosis of AKE include focal acral hyperkeratosis, degenerative collagenous plaques of the hands, keratoelastoidosis marginalis of the hands, acrokeratosis verruciformis of Hopf, and palmoplantar keratoderma of the punctate type [7].
The cause of AKE is not fully elucidated. It appears to be a genodermatosis with an autosomal dominant inheritance pattern and a possible linkage to chromosome 2. The keratotic papules seen clinically may result from an overproduction of filaggrin, which accumulates as a dense band above the granular layer before being incorporated into the protein matrix of mature epidermal keratin [9]. A report has been published in which elastorrhexis was found to be a feature of lesional skin as well as apparently normal skin in a patient with AKE, suggesting that the disorder could be regarded as a generalized defect of elastic tissue that is somehow limited in location [10]. If this is the case, it is not known why the lesions are predisposed to erupt on the margins of acral sites.
No treatment is usually required for acrokeratoelastoidosis because lesions are asymptomatic with no adverse effects [7]. Nevertheless, the condition may be cosmetically unappealing to patients, but no curative treatment has been reported for AKE to date [4, 5, 6]. Various treatments reported include topical medications (corticosteroids, salicylic acid, tretinoin), systemic immunosuppressive treatments using prednisone or methotrexate, antibiotic therapy, and destructive treatment with cryosurgery. All have been of little or no benefit [4, 5]. Retinoic acid (50 mg/d) has reportedly shown some response, although results were still unsatisfactory [11]. Erbil suggested recently that Er:YAG laser surgery may be considered as possible therapy. However, patients should be informed of the limited clinical improvement obtained with this treatment [12].
Conclusion
Acrokeratoelastoidosis is a rare condition characterized by grouped, small, firm, papules distributed on the margins of the hands and feet. Many studies and reviews have attempted to clarify and classify the different clinical and histologic changes. Multiple topical medications and treatments have been used to treat acrokeratoelastoidosis without much success.
References
1. Costa OG. Akrokerato-elastoidosis (a hitherto undescribed skin disease). Dermatologica 1953;107:164-8. PubMed2. Lewis KG, Bercovitch L, Dill SW, L. Robinson-Bostom. Acquired disorders of elastic tissue: Part II. Decreased elastic tissue. J Am Acad Dermatol 2004;51:165-85. PubMed
3. Boudghène-Stambouli O, Merad-Boudia A, Benkalfat MR, Khedim A. Costa acro-kerato-elastoidosis. Ann Dermatol Venereol 1993;120(8):539-41. PubMed
4. Fond L, Parent S, Franck F, Ulianov L, Mansard S, Souteyrand P, Cambazard F. Papules des bords latéraux des mains et des pieds. Ann Dermatol Venereol 2004;131:81-3. UI : 15041854
5. Tsai S, Kageyama N, Warthan M, Cockerell J. Acrokeratoelastoidosis. Int J Dermatol 2005; 44: 406-7. PubMed
6. Lee E, Kim C. Focal acral hyperkeratosis. Clin Exp Dermatol 2007; 32: 608-10. PubMed
7. Bogle A, Hwang Y, Tschen A. Acrokeratoelastoidosis. J Am Acad Dermatol 2002;47: 448-51. PubMed
8. Tajima S, Tanaka N, Ishibashi A, Suzuki K. A variant of acrokeratoelastoidosis in systemic scleroderma: Report of 7 cases. J Am Acad Dermatol 2002;46:767-70. PubMed
9. Greiner J, Krüger J, Palden L, Jung EG, Vogel F. A linkage study of acrokeratoelastoidosis: possible mapping to chromosome 2. Hum Genet 1983;63:222-7. PubMed
10. Fiallo P, Pesce C, Brusasco A, Nunzi E. Acrokeratoelastoidosis of Costa: a primary disease of the elastic tissue. J Cutan Pathol 1998;25:580-2. PubMed
11. Anderson B, Bierring F. Acrokerato-elastoidosis: a case report. Acta Derm Venereol 1981;61:79-82. PubMed
12. Erbil H, Sezer E, Koc E, Tunca M, Tastan HB, Demiriz M. Acrokeratoelastoidosis treated with the erbium:YAG laser Clinical and Experimental Dermatology 2007; 33: 30-31. PubMed
© 2008 Dermatology Online Journal