Acquired reactive perforating collagenosis
Published Web Location
https://doi.org/10.5070/D38bn2p6zxMain Content
Acquired reactive perforating collagenosis
Chrysalyne A. Schmults
Dermatology Online Journal 8(2): 8
From New York University Department of DermatologyHistory
This 68-year-old man has a three month history of a rash on the extremities. In June, 2000, the patient developed a pruritic eruption on the lower extremities which resolved. In December, 2000, the patient presented with an erythematous, pruritic eruption over his legs. He was treated with hydroxyzine, loratadine, triamcinolone ointment, Lidex ointment, and Temovate ointment without resolution. He had been on simvastatin for many years and lisinopril since the summer of 2000. These medications were discontinued early in January 2001, but the pruritus persisted and spread to the arms as well as the legs. He began to develop papules with a central hyperkeratotic scale. A biopsy was performed. Medical history includes diabetes mellitus with retinopathy, hypertension, and hyperlipidemia.
Current medications include insulin and aspirin.
Physical Examination
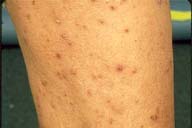 | 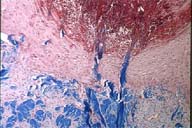 |
| Figure 1 | Figure 2 |
|---|
Multiple, 3-to-8-mm, violaceous-to-hyperpigmented papules with central keratotic scale and excoriations were present over the arms and legs.
Laboratory Data
A complete blood count, blood chemistry profile, and hemoglobin A1C were normal.
Histopathology
Within the epidermis, there is a cup-shaped channel containing degenerated collagen bundles admixed with neutrophils and nuclear debris.
Comment
The perforating disorders are a group of pathologic abnormalities in which there is transepidermal elimination of collagen and/or elastin. This group of disorders includes Kyrle's disease, perforating folliculitis, elastosis perforans serpiginosum, reactive perforating collagenosis, and perforating disorder secondary to chronic renal disease and/or diabetes. There may be overlap cases, and diagnostic criteria are not well-defined for all entities. The term acquired perforating dermatosis has been suggested.
Reactive perforating collagenosis is a rare genodermatosis with lesions appearing early in life after trauma, arthropod bites, folliculitis, or cold exposure. Acquired reactive perforating collagenosis occurs in adults and was first described in association with the renal disease of diabetic nephropathy. All forms of reactive perforating collagenosis share severe pruritus as a feature, and it is possible that the transepidermal elimination of collagen is simply a reaction pattern due to chronic rubbing or scratching in a subset of pruritic patients. Lesions have resolved when the pruritus was controlled.
Acquired reactive perforating collagenosis has been seen in association with multiple disorders, which include diabetes mellitus, renal failure, hyperparathyroidism, liver disease, neurodermatitis, IgA nephropathy, periampullary carcinoma with jaundice, adenocarcinoma, and liver neoplasms. It is unclear whether acquired reactive perforating collagenosis is primary in these cases or is a reaction to scratching. Transepidermal elimination of collagen also has been reported in granuloma annulare, pseudoxanthoma elasticum, and chondrodermatitis nodularis helicis.
Our patient is interesting in that he had a pruritic, erythematous eruption that predated the development of lesions consistent with acquired reactive perforating collagenosis, and there were numerous eosinophils in the biopsy specimen. His current medications are unlikely culprits. The pruritus and scratching may have lead to the acquired reactive perforating collagenosis. Also of note is the fact that his diabetes was controlled with a normal glycosylated hemoglobin at the time of onset of acquired reactive perforating collagenosis.
Treatment of acquired reactive perforating collagenosis is often difficult, and control of pruritus is central. Topical glucocorticoids, antihistamines, keratolytics, PUVA photochemotherapy, UVB phototherapy, liquid nitrogen cryotherapy, electrical nerve stimulation, allopurinol, and retinoids have all been tried with various degrees of success.
References
Rapini RP, et al. Acquired perforating dermatosis. Arch Dermatol 125:1074, 1989Faver IR, et al. Acquired reactive perforating collagenosis: report of six cases and review of the literature. J Am Acad Dermatol 30:575, 1994
Briggs PL, et al. Reactive perforating collagenosis of diabetes mellitus. J Am Acad Dermatol 32:521, 1995
Yanagihara M, et al. The pathogenesis of the transepithelial elimination of the collagen bundles in acquired reactive perforating collagenosis: a light and electron microscopical study. J Cutan Pathol 23:398, 1996
Kawakami T, et al. Acquired reactive perforating collagenosis associated with diabetes mellitus: eight cases that met Faver's criteria. Br J Dermatol 140:521, 1999
© 2002 Dermatology Online Journal

