Sudden onset of verrucous plaques to the face and trunk: A case of cutaneous histoplasmosis in the setting of HIV
Published Web Location
https://doi.org/10.5070/D38bj0v4qcMain Content
Sudden onset of verrucous plaques to the face and trunk: A case of cutaneous histoplasmosis in the setting of HIV
Adam Friedman MD1,2, Garron Solomon MD3, Sorana Segal-Maurer MD4,5, Fred Pereira MD1,6,7
Dermatology Online Journal 14 (2): 19
1. Department of Medicine, New York Hospital Queens, Queens, NY2. Division of Dermatology, Department of Medicine, Albert Einstein College of Medicine, Bronx, NY
3. Department of Pathology and Laboratory Medicine, New York-Presbyterian Hospital/Weill Medical College University , NY, NY
4. Division of Infectious Diseases, Department of Medicine, New York Hospital Queens, Queens, NY
5. Department of Medicine, Weil Medical College of Cornell University, NY, NY
6. Department of Dermatology, Mount Sinai School of Medicine, NY, NY
7. Department of Dermatology, New York Medical College, Westchester , NY
Abstract
A 66-year-old Columbian man presented with a 15-day history of generalized weakness, cough, fever, and verrucous, ulcerating plaques of the face, upper chest and back, and arms. The patient proved to be HIV positive. Histopathologic examination showed a diffuse lymphocytic infiltrate coupled with a striking number of yeast forms within macrophages. The clinical presentation and histopathologic alterations are consistent with the diagnosis disseminated Histoplasma capsulatum. This case emphasizes the importance of increasing awareness of histoplasmosis in nonendemic areas as a result of the large subgroup of immunocompromised patients at risk. Disseminated histoplasmosis can be a treatable HIV complication if recognized early, though is unfortunately a harbinger for an overall poor prognosis.
Clinical synopsis
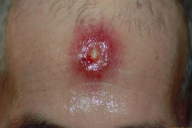 | 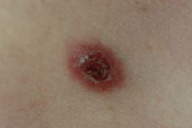 |
| Figure 1 | Figure 2 |
|---|
 |  |
| Figure 2 | Figure 4 |
|---|---|
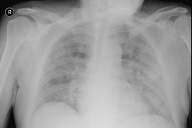
A 66-year-old Columbian man, who had moved to New York City in 1990, presented with a 15-day history of generalized weakness, cough, weight loss, low grade fever, and skin lesions of the face, upper chest and back, and arms. The lesions consisted of verrucous plaques (several ulcerated) varying in size from 1 to 3 cm (Figs. 1 and 2). Medical history was remarkable for treated hypothyroidism. There was no history of prior pulmonary disease; a recent PPD had been negative. On examination, the patient appeared chronically ill, although he was both afebrile and in no acute distress. White, easily-dislodged pseudomembranes were present on the buccal mucosa, palate, and posterior pharynx. Auscultation of the lungs revealed diminished bibasilar breath sounds associated with expiratory wheezing. Chest radiograph showed interstitial opacification of the superior segment of the left lower lobe (Fig. 3). The patient was anemic, but there was no leukocytosis. A biopsy was taken of the forehead plaque for culture and histopathological examination (Fig. 4).
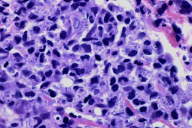
The biopsy specimen showed a diffuse lymphocytic infiltrate coupled with a striking number of yeast forms within macrophages, consistent with Histoplasma capsulatum (hematoxylin-eosin, original magnification X400). A quantitative urinary assay for histoplasma capsular polysaccharide antigen was strongly positive; culture of tissue grew a white, cottony colony on Sabouraud medium at 25° C. Direct microscopic examination of the white patches of the oral mucosa showed budding yeasts and pseudohyphae, consistent with candidiasis. The patient proved to be HIV positive, with a CD4 count of 30 cells/mm.
Comment
Histoplasma capsulatum is a thermally-sensitive, dimorphic fungus that exists in an infectious mycelial form in damp, acidic environments, but proliferates as a pathogenic yeast at mammalian body temperature. The organism is distributed worldwide but is endemic to the central United States, Latin America, and the Caribbean.
Most infected individuals with normal immune function are either asymptomatic or suffer from a self-limited, flu-like illness associated with fever, cough, arthralgias, and erythema nodosum. In immunocompromised patients, however, the disease can disseminate widely causing meningitis, adrenal insufficiency, hepatosplenomegaly, skin ulcers and plaques, lung infiltrates, and pancytopenia secondary to bone marrow involvement [1]. Symptomatic infection with H. capsulatum is an AIDS-defining illness occurring in approximately 2-5 percent of patients with AIDS [2, 3]. Histoplasmosis in the setting of AIDS generally represents reactivation of prior infection and is considered a sign of profound immunosuppression; low CD4 counts are observed. Skin lesions occur in about 50 percent of AIDS patients with disseminated histoplasmosis (DH). These patients are typically men who have resided in endemic areas [4]. The skin lesions of DH are nonspecific and consist of papules, nodules, plaques, ulcers, and erythema multiforme-like macules [5]. Although DH skin lesions resemble those of other disseminated fungal infections, they have a distinct tendency to localize on the face, upper chest, and arms [1, 4, 5]. Mucosal lesions, particularly ulcers, are seen in approximately 40 percent of patients with DH [4].
Detection of H. capsulatum polysaccharide antigen in the urine is a rapid, highly accurate diagnostic test in AIDS patients. Urinary antigen levels can also be used to assess treatment response and to detect relapse [6]. Skin biopsy for histologic evaluation and culture is another simple, rapid diagnostic procedure.
Initial treatment of patients with severe disease consists of amphotericin B. Long-term itraconazole is recommended following resolution. Antiretroviral therapy is usually deferred until there is a reduction in fungal burden, to avoid precipitating immune reconstitution inflammatory syndrome (IRIS). This IRIS is characterized by a paradoxical worsening of infection because of reversal of immunosuppression in the setting of depressed CD4 cell counts and disseminated opportunistic infection [7, 8]. However, AIDS patients with DH who ultimately receive antiretroviral treatment have better outcomes than those who never receive such treatment [4].
References
1. Corti ME, Cendoya CA, Soto I, et al. Disseminated histoplasmosis and AIDS: clinical aspects and diagnostic methods for early detection. AIDS Patient Care STDS. 2000 Mar;14(3):149-154. PubMed2. Casotti JA, Motta TQ, Ferreira Junior CU, et al. Disseminated histoplasmosis in HIV positive patients in Espirito Santo state, Brazil: a clinical-laboratory study of 12 cases (1999-2001). Braz J Infect Dis. 2006 Oct;10(5):327-330. PubMed
3. Calza L, Manfredi R, Donzelli C, et al. Disseminated histoplasmosis with atypical cutaneous lesions in an Italian HIV-infected patient: another autochtonous case. HIV Med. 2003 Apr;4(2):145-148. PubMed
4. Tobon AM, Agudelo CA, Rosero DS, et al. Disseminated histoplasmosis: a comparative study between patients with acquired immunodeficiency syndrome and non-human immunodeficiency virus-infected individuals. Am J Trop Med Hyg. 2005 Sep;73(3):576-582. PubMed
5. K Ramdial P, Mosam A, Dlova NC, et al. Disseminated cutaneous histoplasmosis in patients infected with human immunodeficiency virus. J Cutan Pathol. 2002 Apr;29(4):215-225. PubMed
6. Wheat LJ, Kohler RB, Tewari RP. Diagnosis of disseminated histoplasmosis by detection of Histoplasma capsulatum antigen in serum and urine specimens. N Engl J Med. 1986 Jan 9;314(2):83-88 PubMed
7. Breton G, Adle-Biassette H, Therby A, et al. Immune reconstitution inflammatory syndrome in HIV-infected patients with disseminated histoplasmosis. AIDS. 2006 Jan 2;20(1):119-121. PubMed
8. Schiffer JT, Sterling TR. Timing of antiretroviral therapy initiation in tuberculosis patients with AIDS: a decision analysis. J Acquir Immune Defic Syndr. 2007 Feb 1;44(2):229-234. PubMed
© 2008 Dermatology Online Journal

