Paramedian forehead flap thinning using a flexible razor blade
Published Web Location
https://doi.org/10.5070/D38945418rMain Content
Paramedian forehead flap thinning using a flexible razor blade
Hilda Justiniano MD1, Julia Edwards LVN2, Daniel B Eisen MD3
Dermatology Online Journal 15 (3): 12
1. Procedural Dermatology Fellow2. Department of Dermatology
3. Assistant Professor of Dermatology, Director Procedural Dermatology Fellowship and Aesthetic Dermatology
University of California, Davis, School of Medicine, Department of Dermatology, Sacramento, California
Abstract
Paramedian forehead flaps are sometimes required to resurface large or deep nasal defects. The flap often needs to be thinned to match the contour of the surrounding skin at the recipient site. We describe a technique to thin the distal potion of the paramedian forehead flap using a flexible razor blade, the Dermablade. Once familiar with it, this same technique may be applied to thin other interpolation flaps.
Introduction
Paramedian forehead flaps are sometimes required to resurface large or deep nasal defects. The flap often needs to be thinned to match the contour of the surrounding skin at the recipient site [1]. This is typically done with serrated iris scissors [1]. However, the thick fibrous skin of the forehead can be difficult to thin and the process of thinning the flap can take considerable time to accomplish. The use of a flexible razor blade for use in curettage of benign lesions has been described in the past [2]. We have found that this flexible blade works effectively and quickly for the purpose of thinning forehead flaps as well.
Methods
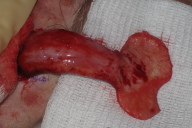
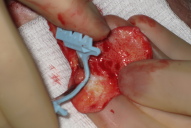
The flap is designed and elevated in the usual manner, where the paddle is dissected in the subcutaneous plane and the pedicle portion of the flap is dissected in the subgaleal plane to the level of the orbital rim. The flap is then stabilized with the non-dominant hand and positioned so that it is extended to its maximal length. The flexible razor blade (Personna Dermablade, American Safety Razor Company, Cedar Knolls, NJ) is then grasped with the other hand and the sharp side is used to scrape away the subcutaneous tissue until the desired flap thickness is reached (Figs. 1 & 2). A sterile gauze pad can be used to more easily grasp the flap and prevent slipping during the thinning procedure. Effort should be made to avoid "scooping" the tissue as opposed to the advocated scraping motion, as this could result in inadvertent divots and vascular compromise.
Conclusions
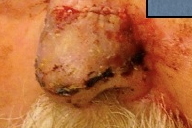
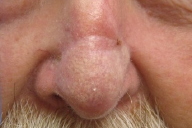
Part of the good cosmetic outcome of the paramedian forehead flap requires matching the thickness of the flap to the variable thicknesses of the different areas of the nose. Although thinning of the flap can be done at time of flap takedown or even as an additional procedure at an intermediate or later time, it is much more efficient to do it at the time of the initial procedure when access to the bottom of the flap is much easier [3]. The facial and thick fibrous forehead tissue is, at times, quite laborious to thin out and the process may consume considerable amount of time. The use of a flexible razor blade makes this process easier and less time consuming.
The use of a flexible razor blade has been described for many purposes in the Dermatology literature. Biopsies, shave excisions, curetting lesions, and most recently, harvesting skin grafts have been advocated [2, 4]. However, its use to thin skin flaps has not been reported to our knowledge.
Even though this technique is easy to perform, care must be taken when using the flexible razor blade to thin skin flaps. The most important issue is not to injure oneself through inadvertent lacerations resulting from flap slippage. This can be minimized by securely grasping the flap with a gauze pad. Menick advocates delaying thinning of the flap in high risk patients, such as smokers, and proposes adding a third stage to this traditional two stage procedure to ensure flap viability [3]. We prefer to perform the thinning during the initial procedure, since this will be the time when it is easiest to accomplish.
In conclusion, we have described an easy technique to thin the paddle portion of a paramedian forehead flap. This technique is efficient and may be performed in a short period of time. With adequate care, this same technique may be applied to other interpolation flaps as well.
References
1. Mellette, J.R. and D.Q. Ho, Interpolation flaps. Dermatol Clin, 2005. 23(1): p. 87-112, vi. [PubMed]2. Peterson, A.J., S.R. Peterson, and K.J. Jensen, Surgical pearl: The DermaBlade as curette. J Am Acad Dermatol, 2006. 54(3): p. 518-9. [PubMed]
3. Menick, F.J., A 10-year experience in nasal reconstruction with the three-stage forehead flap. Plast Reconstr Surg, 2002. 109(6): p. 1839-55; discussion 1856-61. [PubMed]
4. Kontos, A.P., et al., The use of a flexible razor blade in skin graft harvesting. Dermatol Surg, 2009. 35(1): p. 120-3. [PubMed]
© 2009 Dermatology Online Journal