Treatment of molluscum contagiosum a brief review and discussion of a case successfully treated with adapelene
Published Web Location
https://doi.org/10.5070/D387v1z7htMain Content
Treatment of molluscum contagiosum: A brief review and discussion of a case successfully treated with adapelene
Noah Scheinfeld MD JD
Dermatology Online Journal 13 (3): 15
Columbia University Department of DermatologyAbstract
Molluscum contagiosum occur in 2-8 percent of children. This infection is among the most common viral skin infections in children. Although the lesions will resolve spontaneously when puberty, there are several reasons to treat them. The lesions can be cosmetically unappealing. About 10 percent of those with this infection develop a pruritic eczematous eruption. In about 4 percent of children with molluscum, the lesions are numerous and recurrent with no other coexisting immunological problem. Patients who have atopic dermatitis may develop widespread involvement with molluscum. Treatment options include destruction, topical therapy, and oral therapy. Destructive treatment modalities include curettage, cryotherapy, expression or pricking with a sterile needle, electrodesiccation, photodynamic therapy, and laser ablation. Destructive therapy is poorly tolerated in children. Topical medical therapy includes salicylic acid, glycolic acid, tretinoin, tazortene, 5 percent sodium nitrite co-applied daily with 5 percent salicylic acid topical preparations, podofilox, liquefied phenol, tretinoin, cantharidin, and potassium hydroxide. Oral treatment of molluscum includes cimetidine. No therapy is universally effective. I report herein a case of generalized numerous and recurrent molluscum treated with minimal irritation with adapelene.
The reported incidence of molluscum contagiosum (MC) among children ranges from 2 to 8 percent [1]. Most cases are limited in extent but MC can be extensive. Kakourou found in a series of 110 Greek children that 4 (3.8 %) had numerous and recurrent molluscum with no other coexisting immunological problem [2].
A variety of therapies exist for the treatment of molluscum. Destructive treatment modalities include: curettage, cryotherapy, expression or pricking with a sterile needle, electrodesiccation, photodynamic therapy and laser. These are poorly tolerated in children. Topical medical therapies include salicylic acid, glycolic acid, tretinoin, tazortene, 5 percent sodium nitrite co-applied daily with 5 percent salicylic acid topical preparations, podofilox, liquefied phenol, tretinoin, cantharidin, and potassium hydroxide. Oral treatment include of molluscum cimetidine. No therapy is universally effective.
Established treatments modalities have their specific drawbacks. Although curetting particularly in combination with cryotherapy is seen widely as an effective treatment of MC, poor tolerance by children of curetting has prompted the use of a variety of topical preparations. Although topical imiquimod has been advocated as a therapy for MC, it has drawbacks that include that it is expensive and no more effective than a mixture of salicylic acid and glycolic acid which is cheaper but more irritating [3]. Imiquimod is not indicated by the FDA for the treatment of MC despite undergoing clinical trials. There are two reports noting the effectiveness of tretinoin 0.05 percent cream for treating MC [4, 5].
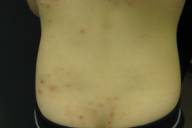 |
| Figure 1 |
|---|
I report a 4-year-old girl with atopic dermatitis who presented with over 200 MC, a problem that had been ongoing and worsening for almost 1 year, despite treatment with topical imiquimod, oral cimetidine (25 mg/kg in 3 divided doses daily), topical tazorotene, cantharidin, or cryotherapy of limited areas (limited by poor tolerance of pain associated with therapy. She used alcometasone dipropionate (0.05 % ointment) for her atopic dermatitis. She received adapelene 1 percent cream. Four weeks later she presented for reexamination and approximately 50 percent of her flank MC and 80 percent of her back and buttock MC (Fig. 1) had resolved (areas of macular erythema and macular pigmentation had been MC just 4 weeks previously).
The adapelene did not worsen her atopic dermatitis in any way. Adapelene has advantages over other anti-molluscum agents. Adapelene causes less irritation compared to topical tretinoin or tazorotene, and comes in a tube rather than the packets that contain imiquimod, which might increase the ease of use and compliance with adapelene. When adapelene loses patent protection in the near future, it may become a low-cost, effective treatment option for MC. Obviously, clinical trials would be needed to assess the place of treatment in the pediatric dermatologist's armamentarium, but this report makes it an interesting treatment option.
References
1. Gellis SE. Warts and molluscum contagiosum in children. Pediatr Ann 1987;16: 69-70, 72-73, 76. PubMed2. Kakourou T, Zachariades A, Anastasiou T, Architectonidou E, Georgala S, Theodoridou M. Molluscum contagiosum in Greek children: a case series. Int J Dermatol. 2005;44:221-3. PubMed
3. Hanna D, Hatami A, Powell J, Marcoux D, Maari C, Savard P, Thibeault H, McCuaig C. A prospective randomized trial comparing the efficacy and adverse effects of four recognized treatments of molluscum contagiosum in children. Pediatr Dermatol. 2006;23:574-9. PubMed
4. Papa CM, Berger RS. Venereal herpes-like molluscum contagiosum: treatment with tretinoin. Cutis. 1976;18:537-40. PubMed
5. Erdmann SM, Rubben A, Frank J, Poblete-Gutierrez P. Mollusca contagiosa in an infant with atopic eczema. A therapeutic challenge Hautarzt. 2004;55:991-4. PubMed
© 2007 Dermatology Online Journal

