Partial lipodystrophy in a girl
Published Web Location
https://doi.org/10.5070/D3874271r2Main Content
Partial lipodystrophy in a girl
Dr Sadollah Shamsadini and Dr Akbar Ahmadi
Dermatology Online Journal 10 (2): 17
Abstract
A 9-year old girl presented with a 2-year history of severe loss of subcutaneous fat in her face. Her medical history included a self-limited episode of jaundice and mild fever 2 years prior. Laboratory examination revealed low serum C3 but normal serum C4. Renal function tests were normal. Low C3 can be a warning sign in patients partial lipodystrophy; it may be a harbinger of renal insufficiency. Patients with partial lipodystrophy may be predisposed to renal failure, especially after pregnancy or the use oral contraceptive pills.
Introduction
Partial lipodystrophy (PL) is a rare condition of unknown etiology, with onset in childhood. It is characterized by progressive loss of subcutaneous fat of the face and neck, and C3 hypocomplementemia [1]. Internationally and in United States of America localized lipodystrophy is extremely rare [2]. PL, also known as Barraquer-Simon disease, is a progressive benign condition described by Michael in 1988 [1, 3]. This disorder chiefly involves the face but can progress to neck, shoulders, and scalp [4, 5, 6].
Clinical synopsis
|
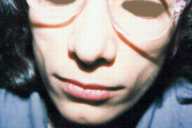
| Figure 1 |
|---|
A 9-year-old girl was referred to the dermatology clinic for severe thinning of face that began 2 years prior. According to the parents, her condition has been progressive. The onset of the disease began 1 year after an episode of fever and jaundice. Facial fat loss began on the cheek and extended to neck and upper trunk; there were no complaints of other areas of involvement, including the eyes and ears. She was the fifth child of the family; her siblings were normal with no family history of similar disease.
On physical examination, she had normal growth and was well nourished. Her face was thin, such that it appeared that her facial skin was adherent to the cheek bone. The cheeks were sunken, and there were bilateral crinkles when she smiled (Fig. 1). Head, face, and neck skin was so thin that underlying bone easily could be palpated. The appearance of the extremities and fat tissues were normal. No abnormality was found in the cardiovascular, respiratory, or renal systems.
Immunologic tests showed normal levels of IgA and IgM, but IgG was slightly higher than normal. Serum C3 level was 15mg/dl (much lower than normal); whereas, serum C4 level was normal. Blood count, blood culture, erythrocyte sedimentation rate, and glucose tolerance test were all normal. (see Table 1)
Discussion
W present a patient with severe thinning of skin beginning on the face of a 7-year-old girl after a prodromal episode of fever and jaundice. The onset symptoms of PL usually begins at age 5-15 years and may follow an acute specific fever, such as measles. PL was first reported by Mitchell in 1885. Females seem to be affected more often than males (4:1) [2].In our case IgG was slightly higher than normal but C3 serum level was 15 mg/dl, well below the normal range. C4 serum level was in normal range. Although PL is benign, C3 hypocomplementemia is present in 70 percent of patients, and is an index for C3 nephritic factor that can induce severe renal insufficiency [1, 4]. Her mother has been advised that her daughter must not become pregnant or use contraceptive pills, because C3 nephritic factor can be induced resulting in RI. If the kidneys become involved, the prognosis may be poor. Early death may result [2, 3, 4, 5].
Two major syndromes are included: Partial cephalothoracic lipodystrophy (so-called Barraqure Simons Disease) and partial face-sparing lipodystrophy (so-called Dunningon Kobberling syndrome) [5]. Although this entity has been long recognized, the etiology and pathogenesis is not well understood. PL is not only a cosmetic disability but may also be a generalized and potentially serious disorder. It is associated with immunologically related renal disease, systemic sclerosis and high titer of thyroid antibodies, all evidence for an underlying immunologic basis [5]. A neural basis involving the autonomic system has also been proposed because experimental studies have shown that the transplanted adipose tissue assumes the characteristics of the area into which it is placed [6]. Disorders that are usually in associated with PL such as diabetes mellitus, retinitis pigmentosa, chronic purpura, polyglossitis, and polyarthralgia, were not present in our patient.
Conclusion
Localized lipodystrophy is a rare disease that is associated with a decrease in C3 serum level with normal C4 level. This abnormality can be a warning sign for occurrence of severe renal damage and renal insufficiency.
References
1. Kumar R, Seema, Aneja S, Seth A, Taluja V. Partial lipodystrophy in a boy. Indian Pediatr. 2000 Jan;37(1):93-6. PubMed2. Garg A. Lipodystrophies. Am J Med. 2000 Feb;108(2):143-52. PubMed
3. Moore SJ, Auchterlonie IA, Cole GF, Gray ES, Dean JC. Partial lipodystrophy presenting with myopathy. Dev Med Child Neurol. 1999 Feb;41(2):127-31. PubMed
4. Burden RP. Partial lipodystrophy and glomerulonephritis. Br J Dermatol. 1978 Jul;99(Suppl 16):49-51. No abstract available. PubMed
5. Senior B, Gellis SS. The syndromes of total lipodystrophy and of partial lipodystrophy. Pediatrics. 1964 Apr;33:593-612. No abstract available. PubMed
6. Anold, Odom, James: Anderws; Diseases of the skin clinical Dermatology partial lipodystrophy. 8th ed pp 576-7 1990.
7. Sekhar RV, Jahoor F, White AC, Pownall HJ, Visnegarwala F, Rodriguez-Barradas MC, Sharma M, Reeds PJ, Balasubramanyam A. Metabolic basis of HIV-lipodystrophy syndrome. Am J Physiol Endocrinol Metab. 2002 Aug;283(2):E332-7. PubMed
8. Daniel W. Foster. The lipidodystrophies and other rare disorders of adipose tissue Harrison's Principles of Internal Medicine. Vol.2 12th edition pp 1883-5,1991.
9. Ljunghall S, Fjellstrom KE, Wibell L. Partial lipodystrophy and chronic hypocomplementemic glomerulonephritis. Acta Med Scand. 1974 Jun;195(6):493-7. No abstract available. PubMed
© 2004 Dermatology Online Journal

